Advertisement
What If We Really Knew Where To Get The Best Cancer Care: The Prostate As Case Study
Resume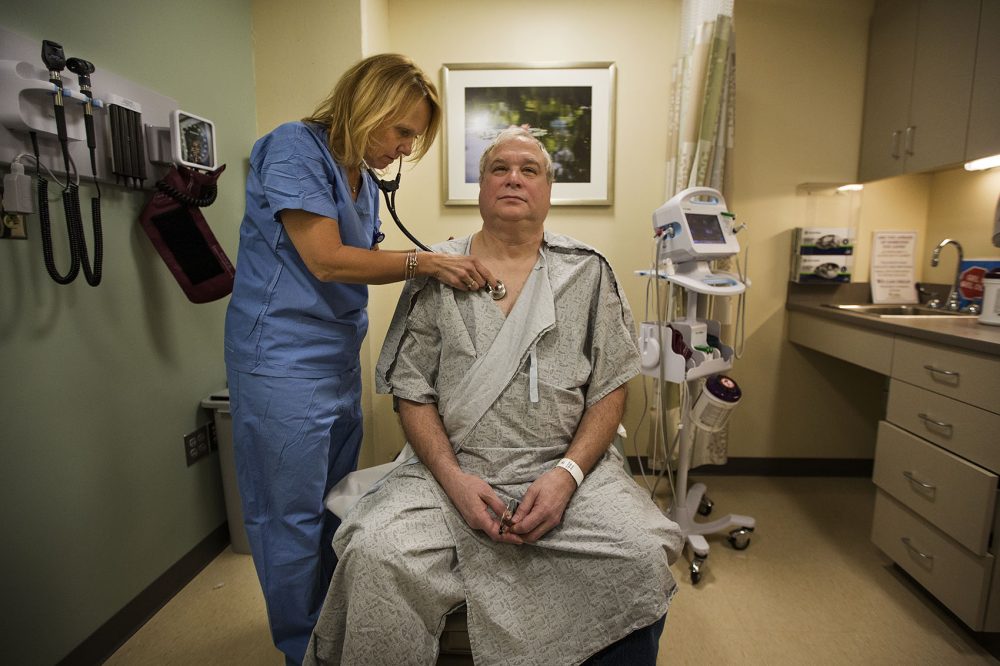
This story is part of our "This Moment In Cancer" series.
Sometime in his early 50s, Ron Dombrowski started getting a PSA test, as recommended, during the annual blood workup his doctor would order. A PSA test measures the level of a prostate-based protein that may be produced by cancerous cells. Dombrowski's PSA level was stable for many years. But this past August, when it started to rise, Dombrowski's doctor suggested an MRI.
The software developer, who's now 65, wasn't sure where to go for the test and a followup meeting with a urologist. So Dombrowski asked around.
"I have lots of friends who have other friends who work in the medical business," Dombrowski said. "The consensus of all these people was, just pick up the phone and call Dana-Farber 'cause you're not gonna get any better than that."
Dombrowski liked what he knew of the hospital's reputation. And he'd read that doctors who specialize and perform the same treatments over and over again tend to have the best results.
"If you have someone who can do the surgery with his eyes closed, in his sleep, because he's done so many of them, that's the guy you want," Dombrowski said.
At the Dana-Farber/Brigham and Women's Cancer Center, the MRI showed cancer in his prostate and possibly a lymph node. He meets Dr. Neil Martin, a radiation oncologist, for the first time.
Martin tells Dombrowski he probably has stage 3 cancer, although if it has spread to that lymph node, that would indicate the most advanced phase of cancer, stage 4.
"This is a cancer we can’t do nothing about," Martin says, leaning forward. Dombrowski nods, clenching and releasing hands clasped in his lap.
Martin describes the pros and cons of two treatment options: surgery to remove the prostate, or radiation to kill cancer cells in the gland. Martin compares surgery to radiation in the top three areas of concern for most men with prostate cancer: Which treatment gives me the best chance of survival? Will I be able to have an erection after either or both types of treatment? And, will I be able to control when I pee?
Dombrowski says he's inclined to choose surgery.
"If we go inside and take out the prostate, we'll be able to biopsy it, look at the lymph nodes and everything else," Dombrowski says, looking to Martin for confirmation. Martin nods and Dombrowski continues: "I want to know what the problem is, and how to fix it."
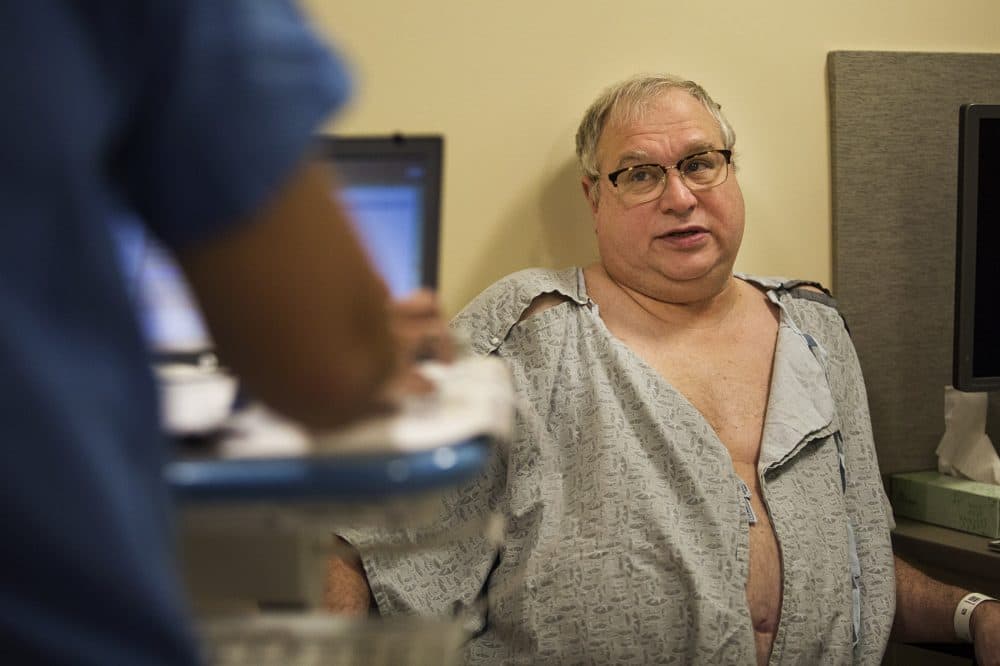
But as Dombrowski weighs this decision here, in the heart of Boston's medical mecca, he's missing some facts. Martin has outlined the different results patients can expect for surgery versus radiation, but not the differences between doctors who perform these treatments, or the differences between hospitals.
Dombrowski is not told, for example, that some doctors do a better job of preserving bladder control for their patients. He doesn't know how much difference there is between doctors. And he doesn't know if the Dana-Farber/Brigham and Women's Cancer Center delivers better care, overall, than other cancer centers across the country.
Dombrowski says he'd like to have some data that shows the this hospital is as good as or better than other hospitals.
"If you want to be recognized as being the best, you have to do this," Dombrowski tells Martin.
But what Dombrowski really wants is more information about individual doctors. How does the surgeon he expects to use compare to colleagues when it comes to patients with incontinence or sexual dysfunction after surgery?
"He's the one who's doing [the surgery]," Dombrowski says, referring to his surgeon. "It's not the brick and mortar building or a hospital administrator who's working on me. His outcomes are very important to me."
"Right," says Martin, "that's exactly what you want to know. And we're not where we owe you to be. You deserve that information. We're committed to getting it."
'Wherever We've Looked, There's Been Variation'
That commitment is more than Dombrowski would likely hear at the vast majority of hospitals across the U.S. Only a handful post their survival, incontinence and erection problem rates in an easily accessible form for patients. And in this age of Big Data, there is no standard way to compare the quality of doctors and hospitals that specialize in cancer care.
"It's shocking," says Doris Peter, who runs Consumer Reports Health Ratings Center, "especially when you think about how much money we're spending on cancer care."
Peter says the federal government should require cancer hospitals to start reporting on measures that patients can use to compare providers.
Peter says patients need this information because "wherever we've looked, there's been variation." That, says Peter, means that "there's clearly cases where people are getting care at facilities and would have done better at other facilities."
But patients have no way of knowing which hospital is which.
As new, often more expensive treatments come online, patients and others who pay for their health care are joining Dombrowski in asking: Where can patients find the best value in health care?
Experts who study cancer care don't know when patients will be able to answer that question. The quest to define quality or value in cancer care, and show patients who delivers the best care, is underway. Researchers started with the most common types of cancer: lung, prostate, breast and colorectal. But it's very early in the process. There's no agreement on what data hospitals should collect or requirement that they do so. In fact, there's still tension about whether sharing an individual physician's patient survival rate and other quality data would improve or harm care.
To illustrate the progress and challenges of measuring quality in cancer care, we'll focus on what's happening with prostate cancer. The walnut-sized gland, lodged precariously below a man's bladder in front of the rectum, hosts nerves that help control urine and also blood flow during an erection.
Doctors say treatment almost always leaves some damage. So which doctors or hospitals have the best record for minimizing damage? Before prostate cancer experts can answer that question, they have to figure out which results matter most to patients.
One Group's 11 Quality Measures
About 1 in 7 men will be diagnosed with prostate cancer during their lifetime. The average age of diagnosis is 66. Patients like Dombrowski have been sitting in exam rooms for decades asking questions about survival, incontinence, erections and more. How often, after treatment, does prostate cancer return? Will I have trouble with bowel movements? How long will I be out of work?
In March 2015, a group of 30 doctors from nine countries published a list of ways to assess whether localized prostate cancer treatment had improved or harmed the lives of patients. The group proposed that all doctors who treat prostate cancer patients begin collecting this uniform set of data for all patients. Collecting and sharing results, the authors wrote, would help doctors learn from each other and help patients make informed decisions about where to seek care.
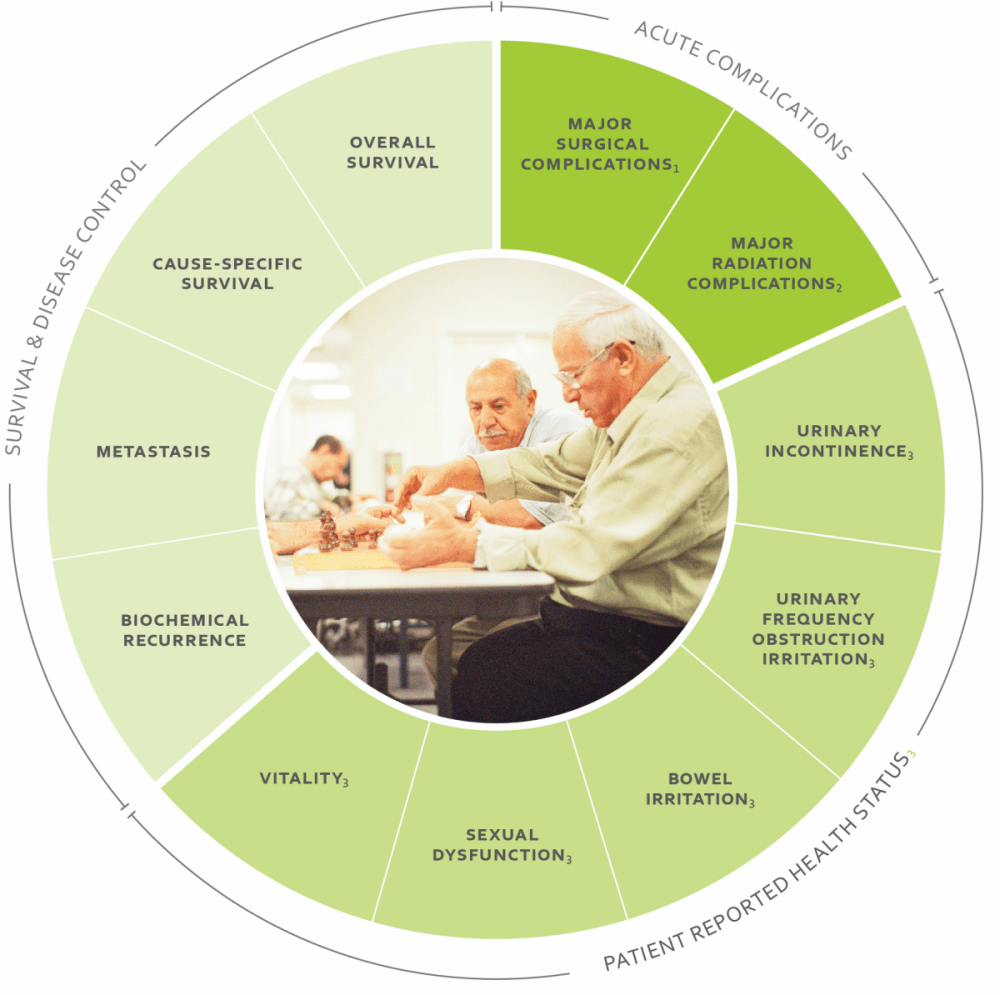
The work on prostate cancer quality measures was organized by a small Cambridge-based nonprofit with a weighty name. The International Consortium for Health Outcomes Measurement (ICHOM) was co-founded by Harvard Business School professor Michael Porter. The organization is developing what it hopes will become standard ways to measure the quality of care around the world for dozens of medical conditions. Prostate cancer was one of the first standard sets completed.
"We're trying to make competition work in health care," said Caleb Stowell, ICHOM's vice president for business development. For patients, that might mean easy online comparisons between doctors or teams of providers. For physicians, the idea is that sharing results will drive doctors to improve their surgical techniques or use of radiation.
The 11 ICHOM measures seen in the graphic above can be applied to all types of prostate cancer treatment. But some patients say some important parts of prostate cancer care are missing from this list.
When Quality Means No Treatment At All
With prostate cancer, sometimes the wise man does nothing. That's because about 30 percent of men who are diagnosed have a low risk that their cancer will grow or spread quickly. These men are candidates for active surveillance. During this period, many doctors will ask for the PSA blood test and a rectal exam every three to four months. Every year or two, a urologist will take samples from the man's prostate for a biopsy.
"It’s uncomfortable," says Len Ulbricht, as he lowers slowly onto a couch at Beth Israel Deaconess Medical Center (BIDMC) after a biopsy, "like sitting on a lump right now, 'cause I’m all stuffed with gauze."
Ulbricht was diagnosed as a low risk patient three years ago. He says the continuous testing and poking makes him anxious, but is still better than dealing with incontinence, bowel or sexual dysfunction after surgery or radiation.
"Every treatment has side effects," Ulbricht says. "I’m sticking as far along as I can with active surveillance to avoid the side effects."
Increased anxiety is common among cancer patients. Some doctors ask patients to track their anxiety levels and consider the effect on their quality of life, decisions and treatment. There are a half dozen other measures that some quality experts say are important, including the rate of patients who have extreme nausea and vomiting during chemotherapy, and the time patients must take off work for cancer care.
Anxiety affects cancer patients in many different ways. Ulbricht says he knows men who are low risk who go ahead with surgery or radiation because they can't tolerate the waiting. Ulbricht, a retired electrical engineer, says he’s managing.
"I try not to act impulsively, to think about the problem," he says. "I guess it’s the engineer in me."
Ulbricht’s urologist, Andrew Wagner, says all low risk prostate cancer patients at Beth Israel Deaconess are told that active surveillance is an option. But that's not the case at other hospitals. Wagner says research shows that the range of low risk patients on active surveillance varies from 20 percent among some doctors to 80 percent among others.
"So you can go to a urologist in one town and be offered surgery, but if you happen to live one town over and go to a different practice, you’ll be offered active surveillance," says Wagner, the director of minimally invasive urologic surgery at BIDMC.
Wagner says patients might want to ask doctors what percentage of their low risk patients are in active surveillance. No one has determined what the percentage should be, but asking the question would help patients find out if the doctor is comfortable monitoring a patient who prefers to wait.
Some patients say making sure doctors explain the option of active surveillance should be a quality measure because too many men have surgery or radiation, and suffer the side effects, without realizing that they had a choice.
"Remember, there is no treatment like no treatment," says Stan Klein, repeating a phrase that has become his mantra, of sorts.
Klein runs the Boston Prostate Cancer Support Group. He hosts about 90 men once a month and has spoken to thousands of prostate cancer patients since his own surgery in 1994. Klein's 89-year-old brain and the spreadsheet on his home computer may be the best repositories of quality information in Boston, especially when it comes to active surveillance.
"There are some very good urologists and radiation oncologists in Boston," Klein says, "but there are some doctors who never met a prostate they didn't want to remove." Klein points a finger at his chest during an interview in his Somerville home. "I know because patients tell me."
Klein is skeptical about the value of quality information collected by hospitals or physicians.
"No doctor is going to answer those questions correctly," Klein says, looking at a printout of the 11 ICHOM measures. "They're not going to tell you, '10 percent of my patients died.' Maybe he couldn't save that [patient] because they were too far gone in the beginning. It don't think that's a fair question."
About half of the prostate quality measures a few hospitals are beginning to collect and analyze comes from patient surveys. Other measures, like the survival or cancer recurrence or complications rates, would be collected by the hospital.
On Klein's last point, are the numbers fair? That's a question many doctors are asking too and is a reason many object to public posting of their data.
Collecting Numbers, But Who Gets To See Them?
When Dr. Martin told Ron Dombrowski that Dana-Farber was committed to collecting information about the performance of each doctor, he could have said it's already happening and that he's part of the reason why. Martin helped draft ICHOM's 11 measures. The Dana-Farber/Brigham and Women's Cancer Center has been collecting the measures for most prostate cancer patients since late 2014.
ICHOM's goal is to have all cancer hospitals gather and share the same data. Doing so could help expensive cancer centers prove that the care they provide is worth the cost. But some are pushing back, for several reasons.
Hospitals may be worried they won't look good, that they'll have lower survival or higher complication rates than their competitors. But there are practical and technical challenges too. Some hospitals have years of data from their own patient surveys that they might have to toss out if they switch to a new standard. Or they may have invested in software that doesn't fit the new data requirements.
The National Comprehensive Cancer Network (NCCN), which includes the 27 major cancer centers in the U.S., has not endorsed any quality measures.
"The need is great and this is difficult to do," says Dr. James Mohler, a urologist who chairs the NCCN's prostate cancer guidelines panel. "Hopefully we’re going to arrive at some type of consensus about how to do this to help our patients that are afflicted by cancer."
Mohler, who chairs the urology department at Roswell Park Cancer Institute in Buffalo, says a number of groups are developing prostate cancer quality metrics. Roswell Park is one of the handful of hospitals that publish survival rates for all major types of cancer. (Prostate cancer patients can also find results for incontinence after surgery (page 21) and the number of patients in active surveillance (page 22). Roswell Park does not list the results for each doctor.)
In Boston, BIDMC publishes its rate for complications and incontinence after surgery in a flier available to patients. Its Dr. Wagner says not all hospitals will have the resources to do the same, but, he says, "I'd foresee a future where practices are mandated to collect simple data that is easy to collect and display. We're not quite there yet."
But until all hospitals are defining incontinence or bowel irritation, complications and other prostate cancer measures the same way, it won't be possible to compare one facility to the next or the doctors who practice at each hospital.
Martin says he isn't sure when the Dana-Farber/Brigham and Women's Cancer Center will show patients some of the data he's helping collect. It might not happen, he says, without outside pressure.
"We’re perceived as being great," he says. "If you leave it to proud institutions like ours, we’ll never do it because there’s no upside. This sounds a little crass, but like, we can only lose with this, right?"
While Martin says patients deserve to see how each doctor compares on survival rates, some of his colleagues disagree.
Dr. Neil Wagle, the assistant director of quality at Partners HealthCare, says showing the data to patients may not be a good idea if one of the goals is for physicians to learn from colleagues who are doing a better job.
"If you’re forcing them to compete among each other by showing individual surgeon data, it doesn’t necessarily foster that cooperative learning environment," says Wagle, whose job includes measuring prostate cancer quality at Partners hospitals.
There is also concern that doctors whose individual ratings are public will cherry-pick, and decline to take on sicker, more complicated patients.
Wagle is just beginning to show doctors who treat prostate cancer patients at Massachusetts General Hospital, Brigham and Women's and Dana Farber their individual numbers. They are not yet adjusted so that doctors with sicker patients have fair scores. But preliminary findings show that even within these world class hospitals, some doctors perform better than others.
"It’s safe to say there are likely significant differences among surgeons," Wagle says.
'Would You Trade Incontinence For A Longer Life?'
Paul Drouilhet had radiation treatment for prostate cancer 10 years ago. He was stable for a few years, but then his cancer came back. Drouilhet says he'd be better off today if his first doctor had explained all the treatment options and shared his performance record.
“I haven’t run into doctors who proffered that,” Drouilhet says, but “no one likes to be graded.”
Drouilhet spent his career working on safety and quality systems -- for airlines. At MIT, he helped develop the collision avoidance system used in the airline industry today and the use of radar to detect severe weather.
Medicine, he’s learned, is much more complicated. With air traffic safety, he says, "the inputs are simpler. There are less variables that go into what it is you're trying to measure and accomplish."
Drouilhet would like to know more about how doctors and hospitals compare. But he has a caution. Having more information may make a patient's choices more complicated, not less. What if one physician had a much lower rate of cancer recurrence after 10 years, but a much higher rate of patients left incontinent after surgery. Some doctors say that might be a common dilemma for patients in the future because doctors who take out extra tissue during surgery are more likely to get stray cancer cells, but also more likely to damage urinary function.
"Would you trade incontinence for a longer life?" Drouilhet asks. "What if it was a 5 percent higher incontinence rate and a 80 percent probability of nonrecurrence?"
Drouilhet, who's 83, does not expect to have to make that choice. He switched doctors several years ago, based on a friend's recommendation, and started hormone therapy to help slow the growth of his cancer. He had another period of stability, but now his PSA number is doubling every six weeks. Drouilhet will have bone and CT scans in the coming week and an appointment with his doctor after that.
"It’s a matter of time," Drouilhet says. "I have a fatal disease, it’s going to kill me, and the issue is to keep it at bay as long as I can."
While they wait for accurate quality information, prostate cancer patients can do little more than hope for the best.
Do you have a question about cancer research, treatment or care that'd you like us to investigate? Ask it here.
This segment aired on February 3, 2017.
