Advertisement
Commentary
Does Cancer Screening Save More Lives Overall? Not Necessarily
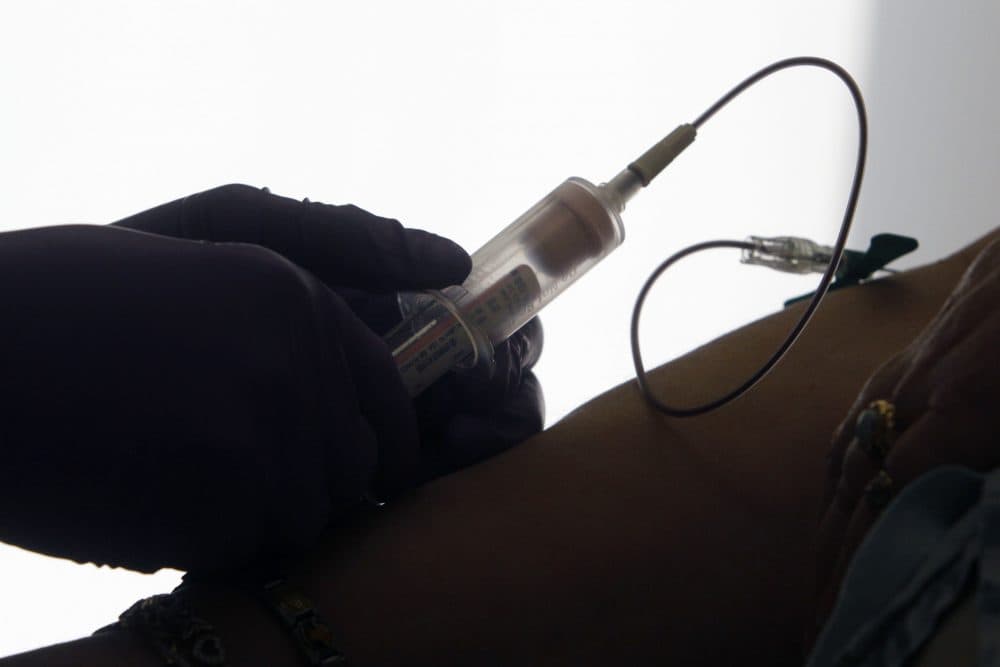
The American Cancer Society, biomedical giant Genentech and the governors of states including Texas, Pennsylvania and Florida have all declared December 4 through 8, 2017 “Cancer Screen Week.” This initiative has noble intentions: to catch cancer at its earliest stages and prevent unnecessary death. Who could have a problem with such a goal?
The problem is that while some individuals will have their lives saved by early cancer detection, if every person were to undergo screening, there would likely be no lives saved overall. It’s counterintuitive — but it’s what the evidence says.
You wouldn’t know this from the Cancer Screen Week promotions. The Cancer Screen Week website does not mention the risks and limitations of screening — only benefits. It declares simply, “Get screened now.” It asks patients to sign a “screening pledge card” as if this were a public television fundraiser and not an intimate medical decision that could result in life-altering surgery, chemotherapy or even death.
As doctors, we have seen patients harmed from screening. People should know exactly what they’re signing up for. They should be made aware of the patient who suffered a stroke while holding a blood thinner for her screening colonoscopy; the man who now wears a diaper after prostate cancer surgery or the woman who died of a complication of chemotherapy for a slow-growing breast cancer. Individual anecdotes never reveal the whole truth, but the scientific evidence against widespread cancer screening may surprise you.
Fear and hope are the dual emotions driving irrational messaging about cancer screening.
Three researchers from Stanford culled all the medical literature on medical screening—19 diseases, 39 screening tests and nearly 50 studies—and found that reductions in “all-cause mortality,” that is, living a longer life, “are very rare or non-existent.” Simply put: despite the dozens of screening tests widely promoted as “life saving,” very few, if any, have been shown to actually lower your chance of dying.
Writing in a prominent medical journal, cancer researcher Dr. Vinay Prasad and his co-authors explained how this could be so: a screening test, they write, may reduce your chance of dying from that type of cancer, but it does not reduce your chance of death overall — because there are many ways a person can die, from heart disease to a car accident to a complication from the very cancer treatment meant to help you. This is why blanket recommendations for everyone to get screened are doing more harm than good.
Another snag with cancer screening is the problem of “overdiagnosis.” Many people who receive cancer screening will undergo unnecessary treatment, because instead of detecting a life-threatening cancer, screening detected a slow-growing cancer that would not have harmed that person in his or her lifetime.
Even Dr. Otis Brawley, chief medical officer for the American Cancer Society, has publicly acknowledged these tradeoffs, declaring that “two decades of [prostate cancer] mass screening are estimated to have caused more than one million American men to receive unnecessary treatment.”
We are not suggesting that cancer screening is useless. Our critique aims to show that screening tests are like any other medical intervention: there are benefits and harms. And it’s why we support informed decision-making. In our view, a “Don’t get screened week” would be as inappropriate as Cancer Screen Week. Events like these make a mockery of the nuanced discussions about risks and benefits that the medical profession now recognizes as a cornerstone of good healthcare. If we presented such one-sided information to our own patients, we would be doing them a dangerous disservice, as well as breaking our ethical duties. Public health campaigns should be held to the same standard.
What we really need is a balanced conversation about cancer screening. The fact we haven’t had one yet is hardly a surprise. Cancer screening in the U.S. is a big business. In fact, the more false positives a screening test delivers, the more hospitals and doctors stand to profit from downstream testing. Ironic, too, is that patients accept false positives and unnecessary treatments because they either feel relieved if further testing was negative or thankful that a slow-growing cancer was detected early. Fear and hope are the dual emotions driving irrational messaging about cancer screening.
We know cancer remains a terrifying and stigmatized illness. But public health campaigns should be more realistic, more humble. We want people to see information like the graphics designed by the Harding Center for Risk Literacy, which display absolute risks and benefits rather than misleading, but commonly used, “relative risk” statistics. Relative risk differences make benefits appear larger than they actually are. For instance, a treatment that lowers the risk of cancer from 2 percent to 1 percent can be expressed as a 50 percent relative risk reduction. So when screening promotions promise large "relative risk" reductions in cancer death, they often fail to mention that the risk of developing that cancer is low to begin with – meaning most people could never be helped by screening.
Why can’t the “overdiagnosis epidemic” be discussed alongside the cancer epidemic? Some scientists estimate, for example, that more than half of the small breast cancers diagnosed by screening mammography represent “overdiagnosis,” and those women would never have been harmed by these tumors in the first place.
Someday there may be a screening test that delivers more benefit than harm. One that definitively saves lives. We will be for it. Until then, we favor honesty and balance rather than bullying and fear.

