Advertisement
Report Shows Stark Care Disparities, More Amputations Among Black Diabetics
Consider this alarming statistic: The rate of diabetes-related amputations is nearly three times higher among blacks compared to other Medicare beneficiaries.
This, according to a new report from the Dartmouth Atlas Project, located at the Dartmouth Institute of Health Care Policy and Clinical Practice. This is the influential consortium that issues eye-popping reports detailing often painfully unfair regional and ethnic variations in medical care. Here are some of the findings from the report, “Variation in the Care of Surgical Conditions: Diabetes and Peripheral Arterial Disease” released today:
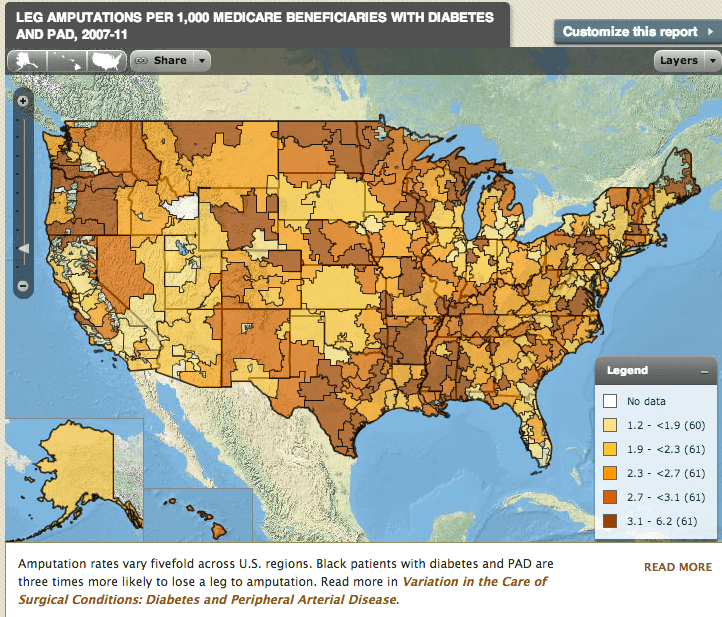
•Amputation rates vary fivefold across U.S. regions among all Medicare patients with diabetes and peripheral artery disease.
•Amputation rates in the rural Southeast, particularly among black patients, are significantly higher than other regions of the country. (Think Mississippi.)
•The amputation rate for black patients is seven times higher in some regions than others
•There is an eightfold difference across regions among blacks in the likelihood that they undergo invasive surgery to increase circulation in the lower legs. In a news conference announcing the report, Marshall Chin, MD, a leading expert on racial and ethnic disparities in health care and a professor at the University of Chicago called these types of diabetes-related amputations "entirely preventable." "In some ways," Chin said, "these disparities are hidden unless we look for them." And here's more from the Dartmouth news release:
There are significant racial and regional disparities in the care of patients with diabetes. According to a new report from the Dartmouth Atlas Project, blacks are less likely to get routine preventive care than other patients and three times more likely to lose a leg to amputation, a devastating complication of diabetes and circulatory problems...
Amputation rates vary fivefold across U.S. regions among all Medicare patients with diabetes and peripheral artery disease (PAD), the report found. Amputation rates in the rural Southeast, particularly among black patients, are significantly higher than other regions of the country. Furthermore, the amputation rate for black patients is seven times higher in some regions than others and there is an eightfold difference across regions among blacks in the likelihood that they undergo invasive surgery to increase circulation in the lower legs.
“This report leaves little doubt where the focus of amputation prevention needs to be directed,” said Philip Goodney, M.D., M.S., director of the Center for the Evaluation of Surgical Care at Dartmouth Hitchcock Medical Center who co-authored the report along with David Goodman, M.D., M.S. principal investigator of the Dartmouth Atlas, and other colleagues. “While a comprehensive approach is necessary, focusing on black patients in poor, rural regions of the United States is likely to be the best place to start. We must look for opportunities to expand education and preventative care for all patients at risk for amputation. However, initiating broader efforts in these high-risk communities will be essential to have the greatest impact...”
The report draws on Medicare claims from 2007-2011 and divides the country into 306 regional markets defined by hospital use. The Medicare data sort patients as either black or non-black (including white, Hispanic, Asian, and others), limiting additional ethnic or racial analysis.
Caring for individuals with diabetes and PAD can be extremely complex and multi-faceted.
Amputation in patients with severe diabetes and PAD is often caused by wounds on the feet and poor circulation, so preventive measures and surgical remedies focus on issues such as foot exams, cholesterol levels and blood sugar control. Tests for blood sugar control and cholesterol levels are inexpensive and universally available. However, the report found that use of these preventative measures varied regionally and racially – for example, only 75.2 percent of black diabetic patients received a blood lipids test in 2010, compared to 81.5 percent of non-black patients.
After the preventive strategies have been optimized, patients with diabetes, PAD, and wounds or ulcerations generally improve most rapidly if blood flow to their feet is restored. Surgery to improve circulation includes endovascular treatments such as balloons or stents and open surgical procedures such as bypass surgery.
The rate of endovascular treatments varied more than sixfold across regions, from fewer than 4.8 procedures per 1,000 patients in Columbus, Georgia to 33.5 in Petoskey, Michigan.
The national average rate among black patients (19.7 per 1,000) was nearly 50 percent higher than the rate among non-black patients (13.3). Rates among black patients also varied dramatically, from 4.8 procedures per 1,000 in Columbus, Georgia to 41.7 in Amarillo, Texas and Hattiesburg, Mississippi.
Amputation is a treatment of last resort. In almost all cases, when comparing black and non- black patients, the lowest risk black patients have a higher risk of amputation than nearly all non- black patients.
The national average rate of leg amputation from 2007-2011 was 2.4 per 1,000 Medicare beneficiaries with diabetes and PAD. The rate varied more than fivefold across regions, from 1.2 per 1,000 patients in Royal Oak, Michigan and Sarasota, Florida to 6.2 per 1,000 patients in Tupelo, Mississippi.
The amputation rate among black patients — 5.6 per 1,000 — was nearly three times higher than the rate among other beneficiaries (2.0). The amputation rate varied by a factor of more than seven among black patients, from 2.1 per 1,000 in San Diego to 16.1 in Tupelo, Mississippi. Among non-black patients, the amputation rate was less than 1 per 1,000 in Takoma Park, Maryland.
Some of the widest racial disparities were seen in Mississippi. There were 14.2 amputations per 1,000 beneficiaries for black patients in Meridian and 16.1 in Tupelo, compared to 3.8 and 4.7 respectively for non-black patients.
