Advertisement
Lazarus Effect: Witnessing A Life Saved By Narcan, Opioid Antidote
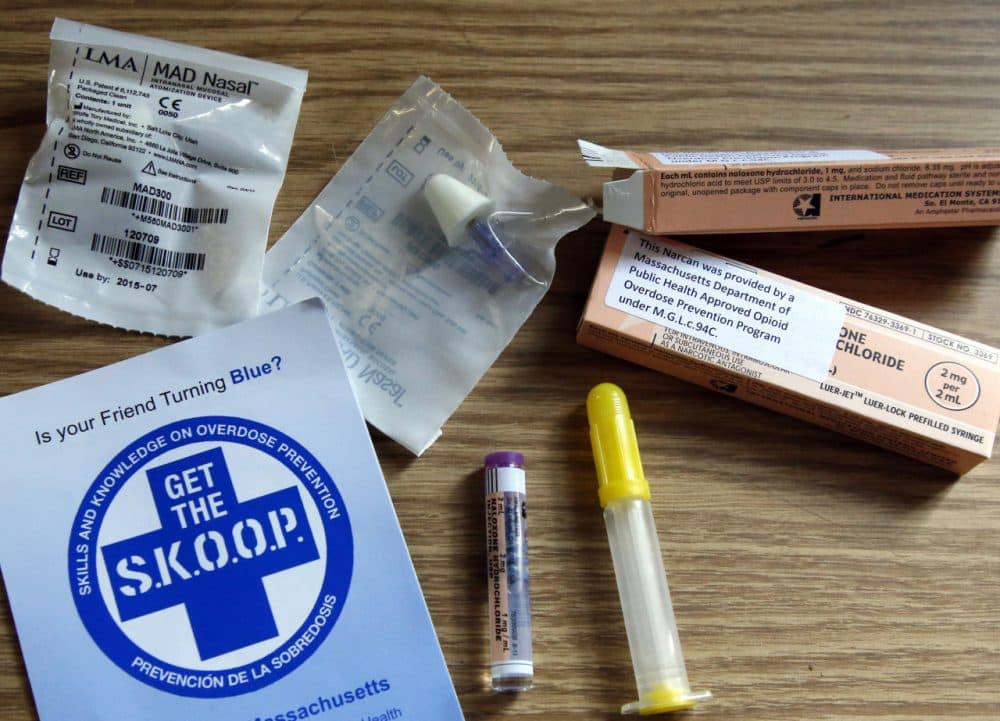
More than two and a half times as many people die from opioid overdoses as from car accidents in Massachusetts, Gov. Charlie Baker said last week. He has appointed a task force to address the problem and held community discussions around the state.
Among measures under discussion: expanding still further the access to Narcan, a drug that, when given promptly, can counteract the effects of an overdose. Its use to reverse heroin overdoses is already up 250 percent in the first quarter of this year compared to a year ago, WBUR's Martha Bebinger reports today. Here, a report from a medical staffer who recently saw Narcan work for the first time.
By Harold du Four
Guest contributor
"Help! Someone please help! Stay with us, Matthew, stay with us!"
The cries were coming from the parking area. In response, the charge nurse and I charged out the front doors of the Dimock Center in Roxbury, the community health center where I oversee the detox unit.
It didn't take long to recognize the source of that distress call: a mother who had just driven from south of the city with her son, who was now slumped over in the back of their gray, two-door convertible. He was in the throes of an overdose, barely breathing, his lips so blue they were almost black.
I knew what had likely happened: The mother had been seeking to check Matthew (not his real name) in to our detox unit. While she had focused on driving into the city to seek help, her son had focused on one last hit. A half-used hypodermic needle lay on the seat next to him, having fallen from his now limp forearm, marked by the vein track scarring that bespeaks a personal history of chronic use.
While my colleague attempted to help him by loosening his winter clothing, trying to wake him, goading his sternum for signs of life, I rushed back into the detox unit to grab a Narcan kit — a naloxone nasal spray that reverses the effects of heroin and some opiate-based prescription drugs.
After quickly assembling the device, I handed it over to my colleague, a nurse with more than 25 years of experience working in the field. She then reached in to carefully – yet confidently – apply a single spray to each nostril of the young man’s nose. Mucus drained slowly down her hand. I punched in 911 on my cell phone.
The mother’s pleas to save her son became more pronounced now; my heart ached for her as she begged, "Stay with us, Matt." We were doing all we could — but would it be enough?
Some have called Naloxone a miracle drug. I can now attest to the accuracy of that description. Along with the cadre of staffers, including recovery assistants and admissions personnel, who had gathered around, we witnessed something akin to a Lazarus effect on the young man's lifeless body. He regained his color, though he still looked pallid and wan. He opened his eyes, looking dazed and confused.
The mother’s tears now transformed into cries of joy.
Our grateful detox staff happily moved to the sidelines as the EMTs arrived to transport yet another young person who had survived a heroin overdose to hospital for further treatment.
Opioid addiction has become a public health crisis rising to epidemic proportions throughout the Northeast. It has made inroads into communities large and small, urban and suburban, including some that previously seemed immune to the havoc it causes.
State police report more than 200 suspected heroin overdose deaths already during the first three months of this year, with 72 suspected heroin overdose deaths in March alone.
As with so many other addictive disorders that begin imperceptibly and quickly take root and take over one's life, the handmaiden to opioid addiction is denial. It’s only after repeated relapses that the reality of one's condition kicks in: Substance use disorder is a chronic condition that requires ongoing treatment and community support.
For many, I've seen the Dimock Center detox act as a first step in that path towards recovery. But a detox is not treatment; it’s palliative care, medical monitoring and goal setting. And the road to sobriety is never simple — or direct. Because substance use disorders have so many dimensions, treatment invariably involves twists and turns along the way.
It is at those junctures in the path to recovery that Narcan can serve as a life saver.
At the Dimock Detox, we’ve seen how effectively Narcan can turn an overdose around. It should continue to be one prong in the multi-prong approach to the epidemic now under discussion at both the state and the federal level. It is a resource that should be available to families — or anyone — aware of someone struggling with an opioid dependence.
Narcan is a kind of a “safety net” for a people like the young man outside of the Dimock Detox, working through personal ambivalence toward a sustained recovery. It acts as a form of harm reduction, sparing a life until further treatment arrives in the form of first responders and later, a more structured approach to treatment.
Of course, there are those with opposing views, who argue that the use of Narcan only provides a pretext for continued use. In my view, that is a jaundiced opinion. Narcan’s role in treatment is essential, serving as a temporary intervention while clearing a path to the possibilities of a life of recovery and an expectation of hope.
Harold du Four is the clinical supervisor of the Acute Treatment Services Unit at The Dimock Center.