Advertisement
For Hives, A New Study Suggests Many Can Skip The Steroids
Mosquito bites? Chiggers? Maybe — please, no! — bed bugs?
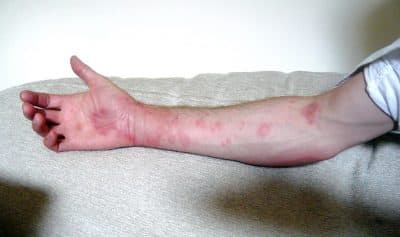
The baffling, itchy red welts began in early fall, cropping up in odd places: on my torso (why would a mosquito bite a spot that wasn't exposed?) and hip (why would a bed bug bite on a fat pad instead of near a vein?). Every day or two, a new one would appear; some in clusters and others alone; some as small as pimples, but one swelling almost to the size of a ping pong ball.
Finally, I went to urgent care. It took a seasoned doctor about 10 seconds to diagnose me with hives: the often-mysterious allergic reaction that affects about one-fifth of us at some time in our lives.
He prescribed an over-the-counter antihistamine, Benadryl, and a steroid, prednisone. I knew vaguely that steroids were not-to-be-taken-lightly drugs. They carry the potential for significant side effects: 'roid rage, blood sugar spikes, long-term risk of infection and bone loss. But this was a "Make it stop!" moment.
The treatment worked beautifully, ending the itch and beating down the swelling within a day or two. I never did figure out what triggered the hives.
But you can understand why I was struck by this recent headline from the American College of Emergency Physicians: "Got Hives? Hold The Steroids."
The press release about the Annals Of Emergency Medicine study included this:
"Prednisone is a strong and great drug for certain problems, but it is no better than antihistamine treatment for patients who are itching with hives," said lead study author Dr. Caroline Barniol of the Centre Hospitalier Universitaire in Toulouse, France. “The antihistamine levocetirizine alone achieved full itching relief within two days for 76 percent of patients. With the addition of prednisone, the relief scores were actually worse."
(Levocetirizine — better known by the brand name Xyzal — is a non-sedating antihistamine that lasts 24 hours. It got federal approval earlier this year to be sold over the counter.)
So maybe, I wondered, I didn't need to take those slightly scary steroids after all? The French study was small -- just 100 patients with basic hives, no puffiness of face or feet — but high quality: patients were randomly assigned to steroids or placebo, and "blind" to which they got.
On the other hand, hives can be a little scary too: They can — rarely — progress to a potentially life-threatening anaphylactic reaction. So couldn't steroids help prevent that? What does this study mean for the next time you or I see those nasty itchy red bumps breaking out?
First, as always, ask your doctor if you're in any doubt: Is this hives? Should I be seen? Editorializing here, but if you can't send a smartphone photo to your primary care office, something's wrong.
Second, I spoke with two specialists: Brigham and Women's Hospital allergist Dr. Karen Hsu Blatman and American College of Emergency Physicians spokesman Dr. Rade Vukmir.
Both say the study is unlikely to shift the current standard practice of offering both an antihistamine and a steroid — and often a Pepcid or Zantac as well, which block an additional kind of histamine, Vukmir said, for a "1-2-3 punch." It takes more evidence than a single study, even a good one, to shift practice.
But each found value in it nonetheless. Dr. Hsu Blatman says that for patients with relatively mild cases of hives, the study underscores the option of simply taking antihistamines at home.
"That's the nice thing about these options being over the counter," she said. "If you see something that looks like a mosquito bite, you can try the antihistamine first, and if it disappears, then you don't have to seek additional care. But if you continue to have symptoms or it doesn't seem like it's turning around, then you should be seeking medical advice."
She called the study "nicely done," and further evidence that histamine is a key element in the hives allergic reaction, "so it makes sense that if you take an antihistamine, that that would help with blocking the histamine, which is what's really driving that itch."
But, I asked her, doesn't it make sense that if an allergic reaction like hives is an overreaction of the immune system, and steroids ratchet down the immune system, they should be helpful against hives?
"Prednisone is never going to help immediately," she explained, and it doesn't really help with the itching, which was the focus of the study.
The steroid "is trying to help decrease that inflammation kind of slowly," she said. "A lot of times, when people are given it in the emergency room, it's to help keep the inflammation down, and hopefully keep the symptoms from coming back. So for patients who may have a bigger presentation, the steroids can be helpful in that way."
Dr. Vukmir said the study offers more fodder for a discussion between doctors and patients as they consider the options. In the wake of the study, he said, his script might sound like this:
You know, normally we would prescribe steroids in this situation. It's been done for years. There's a good track record. Some people get a little concerned about steroids. So there is this other alternative: There's a new study that said maybe we don't need to give steroids, in that you don't get better that much more quickly. And we can try that approach, and I might use a higher dose of the antihistamine.
He might also suggest that the patient call him if there's a problem, and that he could still phone the steroid prescription in to the pharmacy.
"We often involve the patient in the decision-making," he said. And medicine is always trying to improve, in part by reexamining current medical dogma, as this French study did.
Conclusions? I'm leaning toward skipping the steroid, at least at first, if I get another hives attack. But one lingering concern: The study did find that in one patient among the 50 who got a placebo rather than a steroid, the hives progressed to an anaphylactic allergic reaction.
Vukmir said he wasn't sure the report was a full-fledged anaphylactic reaction, and in any case, there's usually good warning: The classic anaphylactic reaction, he said, typically occurs within 20 minutes, and involves a blood pressure drop or significant breathing problems.
So if you're prone to hives, would you try skipping the steroid yourself? The good news is that hives usually pass on their own anyway — they're "self-limiting," in medical parlance. The better news is that whether you take steroids or not, the risks they'll turn life-threatening are exceedingly low.
And maybe the best news is that in current medical culture, you're likely to have a choice. "We'd like the patients to be partners in their care," Vukmir said.
