Advertisement
Over Half Of Patients And Families Hesitate To Raise ICU Safety Concerns, Study Finds
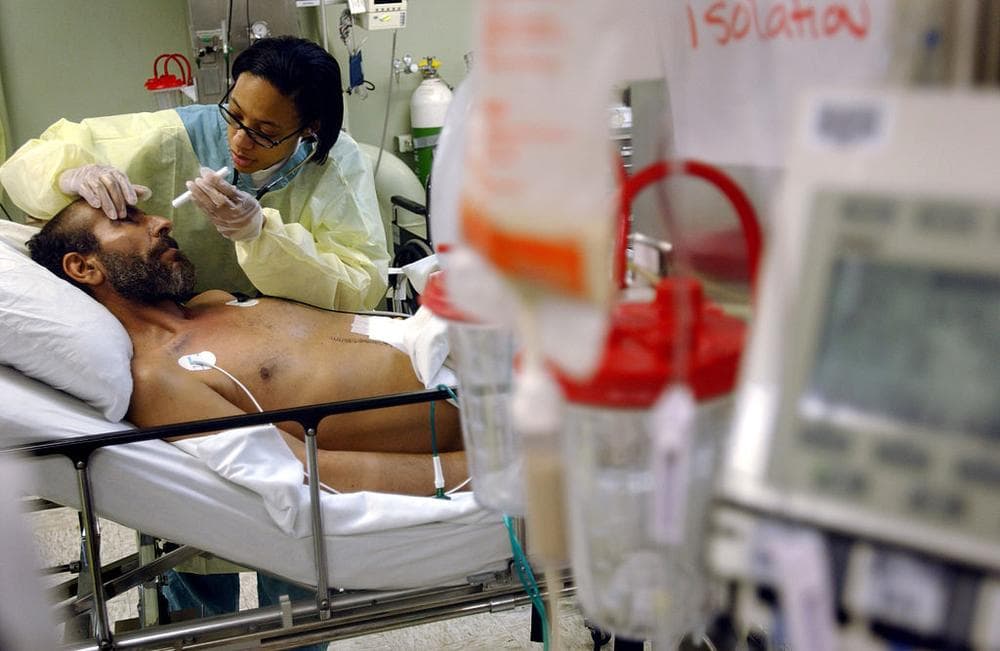
Imagine you're in the intensive care unit at the bedside of your loved one, and you think you see a medical mistake — a wrong pill, an unwashed hand. Do you speak up? Even if you're afraid that might annoy or alienate the medical team?
It's a delicate question, and a new study out of Beth Israel Deaconess Medical Center — the first ICU study of its kind — documents just how delicate. The researchers surveyed more than 100 family members in the ICU and more than 1,000 online about whether they'd feel comfortable speaking up about various concerns.
"One of the key take-home messages was that among patients and families currently experiencing an ICU stay, over half expressed some hesitancy to speak up about common ICU concerns, including a mistake in care," says lead author Dr. Sigall Bell of Beth Israel and Harvard Medical School.
About a third of those patients and families cited, "I don't want to be labeled as a troublemaker" as a reason. Another third said, "The team is too busy." And yet another third chose, "I don't know how to raise my concern, or who to talk to."
About one-fifth of respondents cited, "I'm afraid of seeming like I don't understand medical concepts," and another fifth chose, "I don't want to harm my relationship with the members of the medical team."
Of course, it makes plenty of sense to think twice before you interrupt a medical team in the midst of your loved one's health crisis. But the study comes amid a broader context: Medical errors are a huge problem nationwide, and over the last few years, increasing efforts have focused on empowering medical staffers to fight mistakes — to speak up when they see something that looks wrong, even if that means defying the hierarchy.
This new study helps expand that focus to empowering family members and patients to speak up more as well.
Exactly how families can speak up most helpfully remains to be studied, Bell said, but it's clear that a patient's loved ones — often present at the ICU bedside 24/7 — can be a tremendous asset.
"They know the patient best," she said. "They can detect those early signs when something is going wrong; they're present at transitions of care between different clinicians or different care teams. So they really have a vast amount of knowledge and experience that can contribute to the best care for the patient."
If you're at a loved one's bedside and see something you're concerned about, Bell advises, at least let somebody on the care team know so they can decide whether to pursue it.
"On the flip side is that patients and families who don't speak up when there's a possible problem often end up carrying a lot of guilt if something does go wrong," Bell said. "And sadly, it's not uncommon to hear amongst family members that they knew something wasn't quite right, or that they had this concern but didn't speak up."
Mistakes happen more often in medicine than most people think, said Barbara Fain, executive director of the Betsy Lehman Center, the state agency that aims to advance the safety and quality of health care.
"When patients end up being harmed, it's usually after a whole series of missed opportunities to catch the mistake," she said. "That's exactly where patients and families can play a key role. There are some really interesting studies that show that patients and family members are often better than doctors and nurses at detecting errors, and they're usually right about the errors that they report."
"On the flip side is that patients and families who don't speak up when there's a possible problem often end up carrying a lot of guilt if something does go wrong."
Dr. Sigall Bell of Beth Israel Deaconess Medical Center
Patients and family members "should trust their instincts much more than we know they do from all of this research," she added. "By speaking up about a change in medication they aren't aware the doctor ordered, or a sudden unexpected change in the patient's mental state or level of discomfort, they really can make a difference."
So what's the best way to speak up? What's the language?
Even though she works on patient safety, Fain said even she can struggle with finding just the right words.
"Most people do best framing their concern as a question," she said. "So something like, 'That seems like a different dose or a different drug than I've been getting. Could you double-check to make sure that's right?
"It might help to remind yourself that you do have a right to have your questions and concerns answered respectfully and thoroughly."
Research is needed on what is the most effective language, Bell said. But for now, "I would say things like: 'I'm really concerned about X,' or 'I know this family member very well, and this is different than what I've seen before.' Maybe even just a very direct statement for help: 'I need help to ensure that the patient is on the right track.' "
If your concerns aren't being addressed, Fain said, you should reach out beyond your care team: Most hospitals have staff whose job is to meet confidentially with patients or families on such concerns. They may be called "patient relations" or "customer service" — and, she said, that's what they're there for.
Of course, speaking up can only work if medical staffers are receptive. Both Bell and Fain said this is very much a question of hospital culture. Though the study looks at what patients and families can do, it's actually up to hospital leaders to foster a culture where people are encouraged to speak up.
Fain said one strategy would be to put up posters in patient rooms, or distribute flyers to let families and patients know how to initiate conversations about their concerns, and that they are encouraged.
Bell suggests patient education programs that would help patients and family members develop the language of speaking up, and assure them that they hold unique knowledge — knowledge the medical team does want them to share.
Readers, have you experienced this ICU hesitancy? What happened?
