Advertisement
Not Just Nausea And Vomiting: Cancer Docs Now Worry About 'Financial Toxicity'
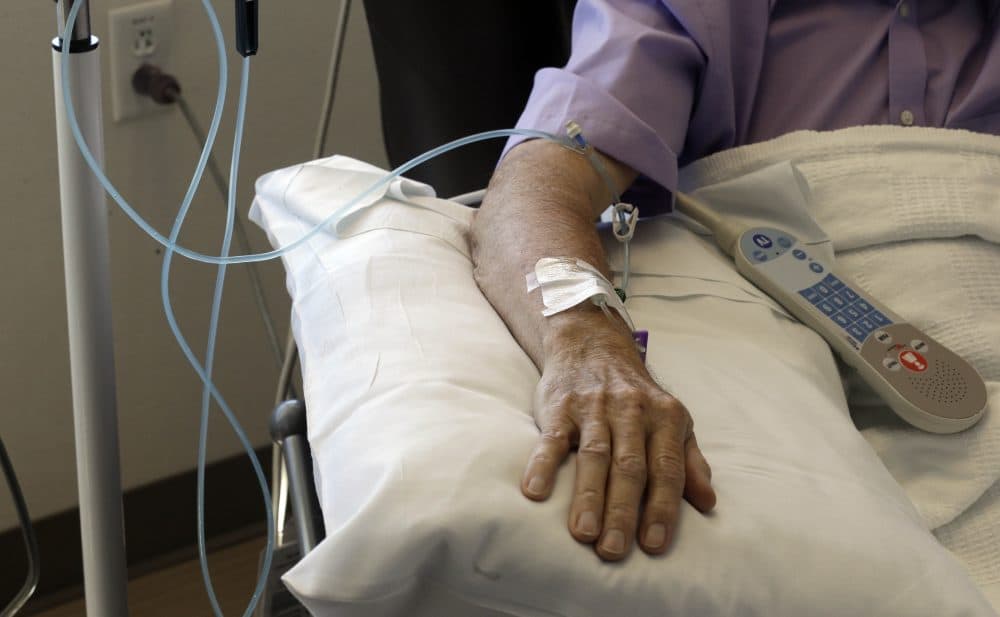
This story is part of our "This Moment In Cancer" series.
Just imagine how it would feel:
Your doctor diagnoses cancer. She says there’s a good chance you can beat it, or keep it under control for a long time. But you can’t afford the thousands of dollars you’d have to pay for treatment that your health insurer won't cover.
That cruel dilemma is cropping up every day among the 1.5 million Americans who will be diagnosed with cancer this year. And it’s getting worse with every new cancer drug that’s approved.
Cancer specialists have a name for it: financial toxicity.
"Just as we monitor the toxicity of drugs -- nausea, vomiting, diarrhea and so on -- there’s an increasing amount of data showing that patients with cancer suffer financial toxicity," says Dr. Daniel Goldstein of Emory University’s Winship Cancer Center.
The latest in a growing body of studies came out Monday in the journal CANCER, drawing on national household surveys of nearly 9,000 cancer survivors and 126,000 people with no cancer history. It reveals that nearly one in three non-elderly cancer patients are not taking their prescribed drug regimens because they can’t afford it.
A new study reveals that nearly one in three non-elderly cancer patients are not taking their prescribed drug regimens because they can’t afford it.
Researchers found that, compared to other patients, those with cancer are more likely to leave prescriptions unfilled or delay filling prescriptions, skip medication doses to save money, ask doctors to prescribe cheaper drugs, or seek out alternatives to the regimens recommended by their oncologists.
The study found that financial toxicity is more common among recently diagnosed cancer patients. This is likely a reflection of the growing cost of cancer drugs, insurance policies that put more cost burden on patients, or both.
The study didn’t measure the consequences of financial toxicity, but its lead author, Ahmedin Jemal of the American Cancer Society, says it’s likely some patients are dying because they don’t get timely or recommended treatments since "some of them are definitely life-saving."
Take adults with a form of leukemia for which there is now a highly effective -- but costly -- drug therapy. Separate research has found that patients who took at least 90 percent of their doses had complete disappearance of the disease. But those who took only three out of four prescribed doses had much poorer responses.
Fatal Bankruptcies
Financial toxicity has other consequences too. Researchers at the Fred Hutchinson Cancer Research Center in Seattle report that cancer patients in Washington State are nearly three times more likely to declare bankruptcy than people without cancer.
Those researchers also found that cancer patients who filed for bankruptcy were 79 percent more likely to die than cancer patients who didn’t. “Severe financial distress requiring bankruptcy protection after cancer diagnosis appears to be a risk factor for mortality,” they wrote in the Journal of Clinical Oncology.
This week’s study found a more pronounced effect among patients with high-deductible health insurance -- those that require an individual to pay the first $1,200 in medical bills, or $2,400 for a family policy. But Jemal notes that many deductibles these days are considerably higher, "$6,000 and even $11,000."
Even after the deductible has been met, "the patient often has to pay 20 percent," Jemal says. "So if a drug costs $100,000, the patient has to pay $20,000. That’s a lot of money. And it doesn’t include the cost of the hospital, surgery or radiation."
The new findings cover the period between 2011 and 2014 -- the first years of the Affordable Care Act. So they indicate that the expansion of health insurance coverage under the ACA has not yet provided an adequate safety net for many cancer patients.
Another clue is that cancer patients over 65, who are universally covered by the more comprehensive Medicare program, do not report forgoing prescription drugs at a higher rate than those without cancer.
Pressure Is Building
All these studies (and more) are fueling a sense of urgency to do something about the skyrocketing cost of cancer care, which is only 5 percent of the nation’s $3.2 trillion health care bill but is increasing faster than any other sector.
"We have to have policy reform to create a safety net for non-elderly cancer patients," Jemal says. "I’m not sure whether it has to be part of Medicare. I’m just an epidemiologist. I’m just saying there has to be something similar to Medicare."
But expansion of Medicare to cover under-65 cancer patients does not seem to be in the cards as Congress and the Trump administration struggle to reform the Affordable Care Act.
Meanwhile, cancer specialists are beginning to discuss among themselves how doctors and patients might prevent, or at least mitigate, financial toxicity.
“We may be forced to prioritize the use of expensive interventions, depriving some potential candidates of access to approved medications or procedures,” warned Massachusetts General Hospital specialists in The Oncologist Express way back in 2013, when the situation was less dire.
Rationing A 'Touchy Subject'
That means, in other words, explicit rationing -- deciding who gets the best shot at costly curative or significantly life-extending care.
And that’s “a touchy subject,” as researchers recently put it in The Oncologist — with some understatement. They note that the National Institute of Medicine, the American Society of Clinical Oncology and others have recommended “that patients be clearly informed of costs as part of delivering high-quality cancer care.”
That doesn’t happen most of the time, studies indicate, and there are formidable barriers to making those discussions routine. At the top of the list: cancer specialists usually don’t know how much the treatments they prescribe will cost a given patient, they don’t know how to find out, they don’t have time to find out, and many don’t believe that cost should play a role in treatment decisions. The scant research available suggests that many patients think so too.
Nonetheless, stopgap proposals are popping up on how “financial toxicity” might be reduced, pending longer-term solutions on controlling and spreading the costs of cancer treatment.
Will Hope Become Unaffordable?
Here are five strategies offered by Scott Ramsey and Veena Sankaran, the University of Washington researchers who participated in the bankruptcy studies mentioned earlier:
- Reduce or eliminate cost-sharing for the most effective cancer treatments -- that is, the amount that patients must pay out of their own pockets.
- Discourage costly cancer treatments that don’t extend life very much and make the cost more transparent so doctors and patients can make explicit tradeoffs -- between a cheaper but equally effective regimen, or between an expensive treatment that offers limited benefit and a cheaper one that may forgo the possibility of a few weeks or months of additional life.
- Eliminate tests and treatments that don’t make a difference, such as PET and bone scans for early-stage breast and prostate cancers.
- Make patients’ “financial health” a routine part of cancer care planning so patients have timely access to sources of assistance -- such as manufacturers’ underutilized drug discount and free-drug programs.
- Provide financial counseling as part of cancer care, taking into account not merely the cost of medical treatments but patients’ ability to continue working, pay for transportation to care centers, and juggle complicated medical bills.
None of these stopgap measures will be simple or quick to implement. But the alternative seems to be a growing number of cancer patients who can’t afford whatever hope U.S. medicine may offer.