Advertisement
CommonHealth: Charlie Gard Case Prompts Tricky Ethical Questions
Resume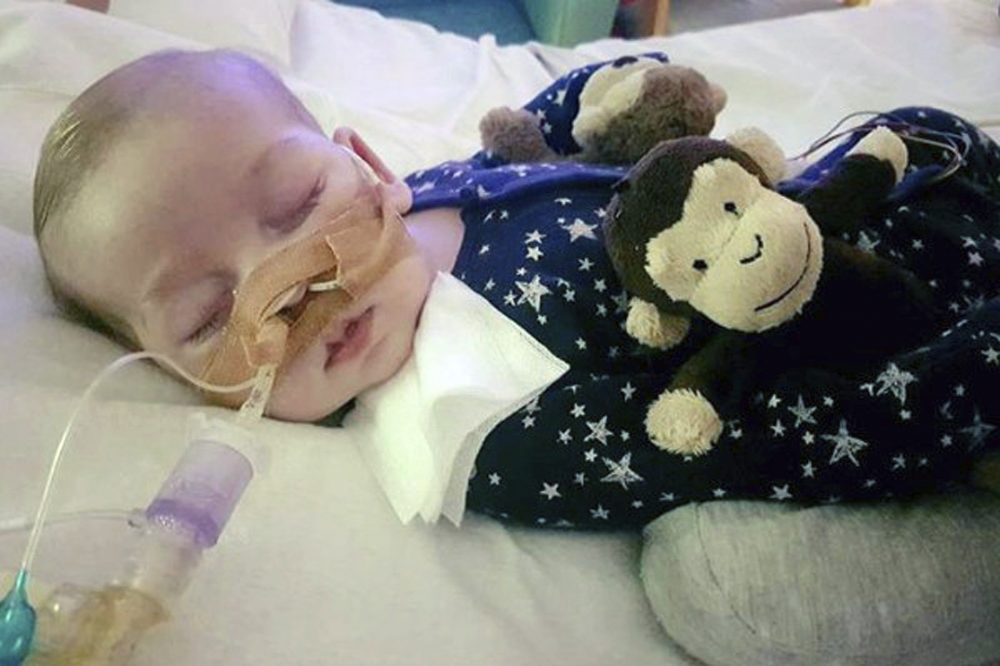
For months, the parents of Charlie Gard, the critically ill baby from the United Kingdom, fought a legal battle to get possible experimental treatment for their son in the United States. Last week, after they were told that experimental treatment was no longer an option, Chris Gard and Connie Yates ended that battle. Charlie was taken off life support and on Friday, just short of his first birthday, he died.
"As Charlie’s devoted and loving parents, we’ve decided that it is no longer in Charlie's best interest to pursue treatment and we will let our son go and be with the angels," said Chris Gard.
Guests
Carey Goldberg, host of WBUR's CommonHealth blog, which tweets @commonhealth.
Robert Truog, Director of the Harvard Center for Bioethics and Frances Glessner Lee Professor of Legal Medicine, Professor of Anaesthesia.
Interview Highlights With Dr. Robert Truog
On the principles of the right-to-try laws movement
"I have to say I think the right-to-try movement is pretty misguided. Ninety percent of new drugs that come on the market never make it past the first round of testing. Many turn out to be harmful. I think that the oversights that we have, of putting new drugs through a careful process of clinical trials, is actually a very smart thing. Trying to circumvent that through right-to-try laws actually does more harm than good."
On how having the financial resources for a treatment shouldn't always mean care can or should be given
"The kind of care that Charlie required can only be provided through tertiary care ... the kind of medical centers that exist only in a limited number of places in the world. The intensive care unit where I work -- we are always full. I think we have a responsible to make sure that we are using our services for children that can most benefit from what we’re doing.
When we don’t have beds in the ICU, it means that children who are waiting for surgeries that are not absolute emergencies have to wait longer. So, just the fact that somebody could pay for that bed is not the end of the story. We need to think about the other families, the other children, that need those resources and what’s the best way to use them."
Nobody could actually pay to create an additional bed in the intensive care unit. It simply doesn’t exist, it’s not part of the building. It’s one of the constraints that we work on. Truly every single day, those beds are completely full. We are having to turn people away, delay their surgeries because we don’t have the resources. It’s not just a question of money. It’s what is physically available and the responsibility of... the doctors and nurses who take care of these patients. We have the responsibility to make sure they work for everyone's benefit."
On the support the family has received from Pope Francis and President Trump
"[Pope Francis] and President Trump were responding as all of us would -- that our heart goes out to families like this. The loss of a child is the worst thing that can happen in anyone's life and that natural response is there for all of us, not just for them.
But, then we need to think it through a little more and think about all of the children that are really sick in the world and how do we fairly treat all of them in the best way possible. That’s where the decisions get more complicated."
This article was originally published on July 31, 2017.
This segment aired on July 31, 2017.