Support WBUR
State Will Stop Paying For Some Hospital Re-Admissions
Medicaid is one of the fastest growing parts of the state budget. To tackle rising health care costs, Gov. Deval Patrick's administration plans to stop paying hospitals with high rates of re-admissions when low-income patients return within 30 days.
It could be a man who leaves the hospital with new prescriptions and takes the wrong pill four times a day. Or a woman with depression who skips a critical follow-up appointment after surgery. Perhaps it's a child who goes back to the same activities and has another severe asthma attack. These are all reasons patients return to the hospital shortly after release. They might all be prevented with better instruction inside the hospital, a better hand-off to our doctor outside or more active patient follow-up.
“We are paying for the wrong things," said Dr. Judy Ann Bigby, state secretary for Health and Human Services. Bigby said it’s not just that the state doesn’t want to pay. Repeat hospitalizations carry risk, “either a hospital-acquired infection or some other type of outcome that demonstrates that the quality of care is not as good as it could be, and it’s costly to the system," Bigby said.
Hospital re-admissions may be prevented with better instruction inside the hospital, a better hand-off to our doctor outside or more active patient follow-up.
Bigby’s office is sending hospitals their re-admission scores. Later this year, the state plans to stop paying hospitals where the re-admission rate is higher than the statewide average.
"We want hospitals and other providers to do a better job of coordinating care for people throughout the system," Bigby said. "We recognize that this is not just a hospital problem."
But the burden will be on hospitals and that’s where administrators object. They question the way the state is defining and counting preventable re-admissions and point out that hospitals are working on this issue without state intervention. Medicare and a few private insurance plans are also ending payments for some re-admissions. But Karen Nelson, senior vice president for clinical affairs at the Massachusetts Hospital Association, questions who is really responsible for this problem.
"Re-admissions are a community issue," Nelson said. "Some of the factors that lead to a re-admission are not something the hospital has control of." For example, Nelson said, the hospital can't decide whether "the patient can access their physician to prevent them from going to the emergency department of the hospital."
Ending some payments for re-admissions is expected to save $8 million in the next fiscal year — a drop in the pool of Medicaid dollars. But Bigby said she hopes the change will compel hospitals to make connections with doctors and other partners in the community so that there’s a network of providers paying attention to each patient. Such networks will be part of the state’s move towards global payments, where doctors and hospitals will be financially responsible for any kind of care that a patient needs. Focusing on re-admissions offers a glimpse of how challenging learning to work as a network of caregivers may be.
"Nurses and doctors on the floor are more worried about the sick patient coming to the floor than about the relatively healthy patient who is ready to go home," said Dr. Brian Jack, at Boston Medical Center. Jack refers to a study that found most hospitals spend just six to eight minutes, on average, preparing patients to leave the hospital.
Jack designed a program that starts discharge planning well before the patient leaves.
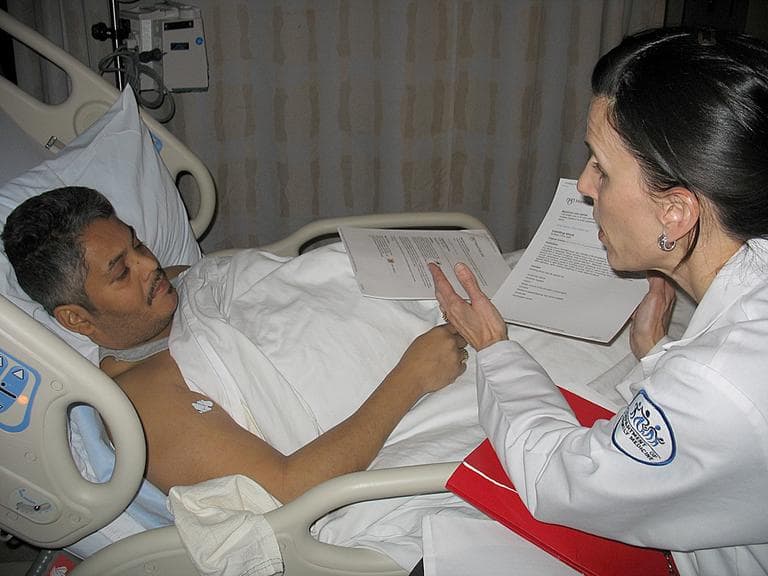
Here’s Kim Visconti, a special discharge nurse, talking to Edgardo LaSanta about a test he just finished taking:
"Depending on what that test shows, they may send you home later today or they may decide to keep you overnight," Visconti said. "Did they tell you what the plan is as of yet?"
It isn’t clear when LaSanta, who has Hepatitis C, will leave. He’s still a bit yellow. But while he waits for the latest test results, Visconti is putting together a list of the medications LaSanta will take, making the follow-up appointments he’ll need, and going over a few new health problems.
"I got a murmur in my heart, they found today," LaSanta tells Visconti.
"So that was something that was new for you as well?" Visconti asked. "Do they think that you’re going to need follow-up with a cardiologist?"
Before he does leave, Visconti will hand LaSanta a booklet with a color-coded daily schedule for his medications and an appointment calendar. She’ll quiz him to see if he understands what the prescriptions are for and when to take them.
Jack said this program cut re-admissions at Boston Medical Center by 30 percent and saves $412 for each patient who does not return within 30 days.
"There are not too many things that improve the quality of care and save money, and this is one of them," Jack said.
Reducing re-admissions has not been in a hospital's best interests under the current way we pay for medical care, because hospitals are paid to fill beds. That's supposed to change as the state moves to paying hospitals a lump sum instead of payments based on how many patients hospitals admit. In the meantime, Boston Medical Center is testing a video version of the discharge nurse.
"It looks like you are going to be leaving the hospital soon, so I brought some information for you," an automated voice said as a black woman in an animated video turns the pages of a booklet.
This is Louise, who takes patients through their detailed discharge plan. Jack said twice as many patients say they prefer Louise to a real nurse. To hear more about why, meet Louise and add your thoughts, go to our CommonHealth blog.
More:
This program aired on February 8, 2011.
