Support WBUR
Budgeting Care For One Of America's Most Expensive Patients
First in an occasional series
STOUGHTON, Mass. — A small, thin woman, tucked in the corner of her cream-colored couch in Stoughton, is one of the country’s most expensive patients.
"I’ve had MS [multiple sclerosis] since I was 18 years old," says Sue Beder, 65, as she begins to tell her story. "My husband passed away when he was 37, leaving me with two children. It was hard, but my parents were a big help. I've always had a lot of doctors."
Beder recently signed up with an agency that will try to improve her health while working under a budget, sometimes called a global payment. (We'll track Beder's care for her first year in this plan.) As more and more patients are covered by global payments, Beder represents the future of health care in Massachusetts. And, if health care on a budget doesn’t work for high-cost patients such as Sue Beder, it may not make sense for any of us.
'I Always Needed The Ambulance To Get Me Up'
On a hot day last summer, Beder, hunched behind her walker, shuffled to the car of her home health aide. They drove to the Stoughton Fire Department.
"I got cookies for them," Beder says, smiling with delight. "They’ll come any time, they really will, if you need them."
Beder offered the cookies as thanks for the roughly 40 trips firefighters made to her home over the past year. Beder’s emergencies — a few of which sent her to the hospital — started with a seemingly simple problem: She couldn’t get to the kitchen to pour herself a glass of water or get food.
Beder brushes back wavy brown hair as she speaks. Her curled hands move a lot. But those hands, weakened by 47 years of multiple sclerosis, can’t hold a knife to chop food into small pieces she can swallow without choking.
Many days, Beder would not eat until her 93-year-old mother or a home health aide made dinner for her. If she stood up to walk to the kitchen or bathroom, she often wouldn’t make it.
"I’d be standing here trying to walk to the bathroom and I would just fall," she says, describing the days before she signed on with her new agency. "I would call my children, see I have the Lifeline, thank God, and they were getting angry with me." Beder pauses and purses her lips. "They [my sons] wanted me to go someplace, but I’m happy here. This is my home. So, I always needed the ambulance to get me up."
Firefighters responding to Beder's 911 call would check for injuries, pick her up off the bathroom or kitchen or living room floor, clean her up, and place her in a chair where she would go back to waiting for dinner.
Crafting A Minute-By-Minute Plan
"Right away within the first five minutes of meeting Sue I knew that things had to change," says Judy Tremblay, a nurse manager with Senior Whole Health in Cambridge.
Tremblay remembers arriving at the front door of a neat, two-bedroom home last fall. She knocked and called for Beder. "She told me to come in. Her voice was sort of far away." Tremblay discovered Beder in the bathroom, unable to pull up her pants.
Tremblay helped Beder to a comfortable chair and launched an investigation of the home. She looked for scatter rugs, electrical cords, clutter on the floor, passages that were too narrow — anything that might explain why Beder was having frequent falls.
"Is it equipment, is it drug-related, is it dizziness or weakness? Why is she falling? What can we do to stop this?" Tremblay remembers asking herself as she looked around the house and got to know Beder.
Tremblay must figure out why Beder is among the 5 percent of patients whose expenses add up to half of the $2.6 trillion Americans spend every year on health care.
She tells Beder she can hire more help and that Tremblay will make sure the aides can meet Beder's specific needs. Tremblay's nurse creates a minute-by-minute plan for Beder’s care: five minutes a day for grooming, 10 minutes for dressing twice a day, 30 minutes for shower, and on and on.
Tremblay’s mission is to see if spending more money up front — on handrails in the bathroom, better home care, taxi rides to the doctor’s office, and many more services — will help Beder stay healthy and help the government save money on her care.
"We keep people out of hospitals and nursing homes," Tremblay says.
A Global Payments Gamble
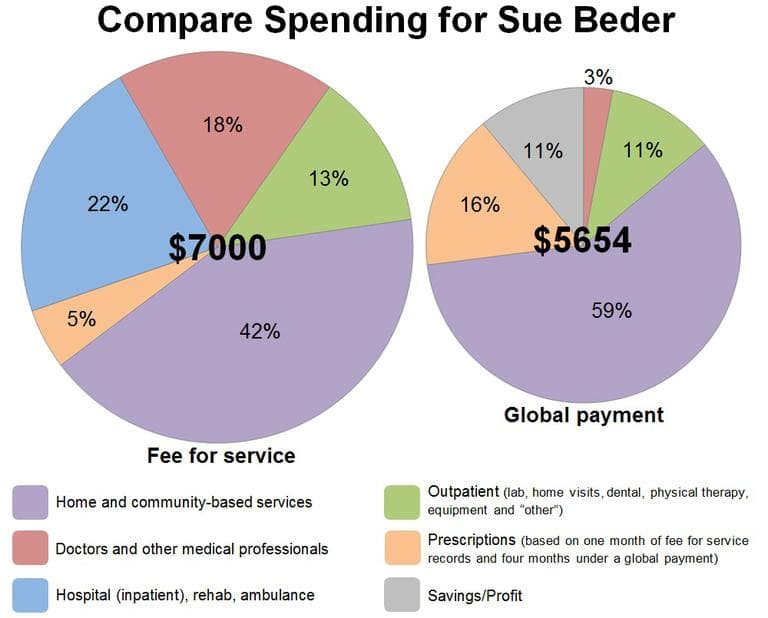
But Tremblay and Senior Whole Health are taking a gamble. They’ll try to provide all of Beder’s care for 20 percent less than what Medicare and Medicaid were spending on Beder before she signed up with the agency. That was roughly $7,000 a month. In return for taking this risk, Senior Whole Health, in an unusual arrangement, gets a lump-sum payment from the two government programs. The agency decides how best to spend money on Beder.
Senior Whole Health is so convinced prevention works that they waive all the co-pays for Beder's medications, pay for her vitamins and lotions, and buy her adult diapers. Tremblay says Beder should not have to choose between lying on wet sheets and a precarious trip to the bathroom.
"We didn’t want her climbing out of bed in the middle of the night," Tremblay says, when "she’d be more at risk for falling."
"It’s incredible," says Beder, who still seems stunned by the arrival of free Depends. "And it’s just saved me. I mean, before I was having so many accidents because they’re so expensive."
If all goes well, Beder will remain happily at home, the government will save money, and Senior Whole Health won’t lose money paying for Beder's care. So far, Beder has cut way back on calls to the Stoughton Fire Department.
"I just wonder if they miss me," Beder says, laughing. "I used to call them a lot. But Jen, my life is better, isn’t it?"
Beder turns to her home health aide, Jen McDonnell, who nods, smiling.
Beder’s 911 calls haven’t stopped altogether. There was one day in January when she called the fire department twice; a sign, perhaps, that keeping her at home, and out of expensive hospitals and nursing homes, will not be easy.
We had help with this story from WBUR's Aayesha Siddiqui and Wilder Fleming.
It was produced, in part, as a project for the California Endowment Health Journalism Fellowships, a program of the University of Southern California’s Annenberg School for Communication & Journalism.
This program aired on April 6, 2012.
