Support WBUR
Ask About The Quality Of Your Colonoscopy: It Matters
Someday soon, you'll need a routine medical test, perhaps an ultrasound or a mammogram, and you'll obviously want the best. But the quality of health care tests and procedures can vary a lot depending on the doctor or hospital, and it's not easy for patients to find information about quality.
Still, we're all supposed to be choosing our care more carefully these days. So when I got a scribbled note from my doctor saying that it was time for a colonoscopy, I set out to find the best one in Boston.
I used to think a colonscopy is a colonoscopy, just one of those tests we have to get when we hit middle age. Then I met James Tracey, a gastroenterologist (GI) who does more than a thousand colonoscopies a year. He starts telling me about this running competition he has with other GI docs, one in particular at Hawthorn Medical Associates in North Dartmouth. It's about who has the highest rate for finding polyps in patients during a colonoscopy.
"When he and I walk down the hall, it wouldn't be uncommon for him to mention his percentage just to get me going," Tracey says. "And of course that redoubles my effort that I'm not going to have that edge over me! I'm going to make my numbers as good as his."
Tracey tells me some doctors in his practice find polyps in twice as many patients as others. Hold on, I think, this seems pretty important. I'm getting this not-so-pleasant test to look for adenomas, those polyps that can develop into colon cancer. So I ask Tracey, why is there such a big difference? He reminds me the colon is a five- to six-foot-long tube packed into the abdomen.
"Sixty to 70 percent of the colon you can see clearly, no matter what you do," Tracey explains. "But 30 percent of the colon, you need to work at it. You need to irrigate the colon out if there's any fluid or debris. You need to reexamine an area several times if the anatomy is distorted so the colonoscope cannot clearly see."
My takeaway is that some doctors look more closely for polyps than others. And, of course, patients play a big role here. If we don't follow the prep instructions, such as fasting, and come in for this test with a clean colon, the doctor is not going to have a clear view of potential problems. OK, enough description. So I make a list, based on conversations with doctors, of ways that one colonoscopy can be better than another. I email the list to some large hospitals and physician groups in Greater Boston and ask them how they measure up.
The first doctor who responds says, "You must be kidding," as in, we've never done this before and we're not going to start now.
The next one says, "We'll get back to you," so who knows what means?
A third doctor says, "We'll see what we can do," and another says flat-out,"No."
I look around for other hospitals and physicians groups who've published information about how well they perform colonoscopies. I can't find any public numbers even though doctors tell me they have this information. OK, now I understand the resistance. No one wants to go first, especially when there are no clear quality standards.
But knowing which doctors finds polyps more often than others is important. It can mean the difference between finding an early sign of colon cancer and missing it. And in the end, five of six physician groups I contacted agree, for the first time, they say, to give me information about how well they do on colonoscopies, but only as a group. I can't get individual information for doctors unless I ask them individually.
Still, I have to applaud the groups who share their numbers voluntarily. They're the docs at: Beth Israel Deaconess; Mass General; Harvard Vanguard; Hawthorn, which is affiliated with Steward Health Care; and Digestive Health Associates, whose doctors are part of the physicians group at Tufts Medical Center.
Dr. James Richter, the director of MGH's gastroenterology quality management, says it may be time for GI docs nationwide to begin posting information for patients as well.
"We do think that accountability for performance is something we owe society, but we want to do it in a serious, rather than a superficial, way," Richter says.
Physicians in many specialty groups are ramping up quality measurement tools. Douglas Pleskow, president of the Massachusetts Gastroenterology Association, says private insurers are demanding more of this information and posting it for patients will be a federal requirement soon.
"We are getting ready," Pleskow says. "We do know that this will be mandated, we do know that this is an important part of our practice, and we do know that patients are interested in finding the information as well."
But there is understandable resistance from doctors. They say physicians who take care of sicker patients won't score well, through no fault of their own and they don't know what quality data will be required.
"Most data on quality is too brand new. It just hasn't caught on. It's changing," says Dr. Jose Marcal, who practices in Stoneham at Digestive Health Associates. Marcal says he thinks "things are becoming more open. The concern about sharing data is obviously the concern about malpractice and issues related to that." Marcal, by the way, did share his adenoma detection rate. He finds these polyps in 50 percent of patients — that's a high score.
But the concerns he raises apply to many, many tests and procedures, not just to colonoscopies. Patients have to be more inquisitive.
"It's certainly their right to ask providers about this information," says Dr. Beverly Loudin, the medical director for patient safety at Atrius Health (which includes Harvard Vanguard physicians).
"My hope would be that moving forward we can be completely transparent about all of these things, but I’m not sure when we will get to that point of complete transparency," Loudin says.
For now, if you need a colonoscopy, be sure you ask at least one question: How often does your doctor find adenomas, the polyps that can develop into cancer? That answer is important.
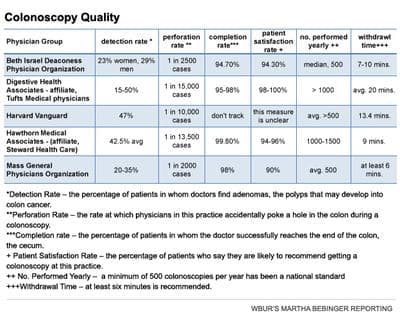
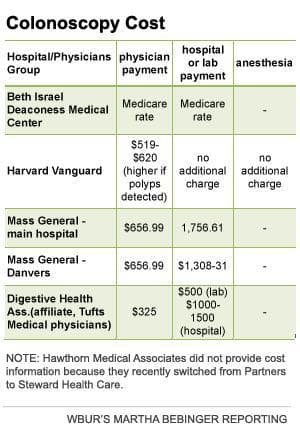
If you really want to find the best "value" colonoscopy, try comparing the quality chart above and the cost chart to the right. Both are rough. The quality information has not been cleaned up or adjusted for the sickness of patients. And on the cost chart, some of the prices you see are based on what my insurer, Blue Cross, would pay, and some aren't. This isn't close to what we patients need to make smart choices, but it's a start.
This program aired on January 10, 2013.
