Support WBUR
Commentary
Now We See: How The Opioid Crisis Has Laid Bare Deep Flaws In American Medicine
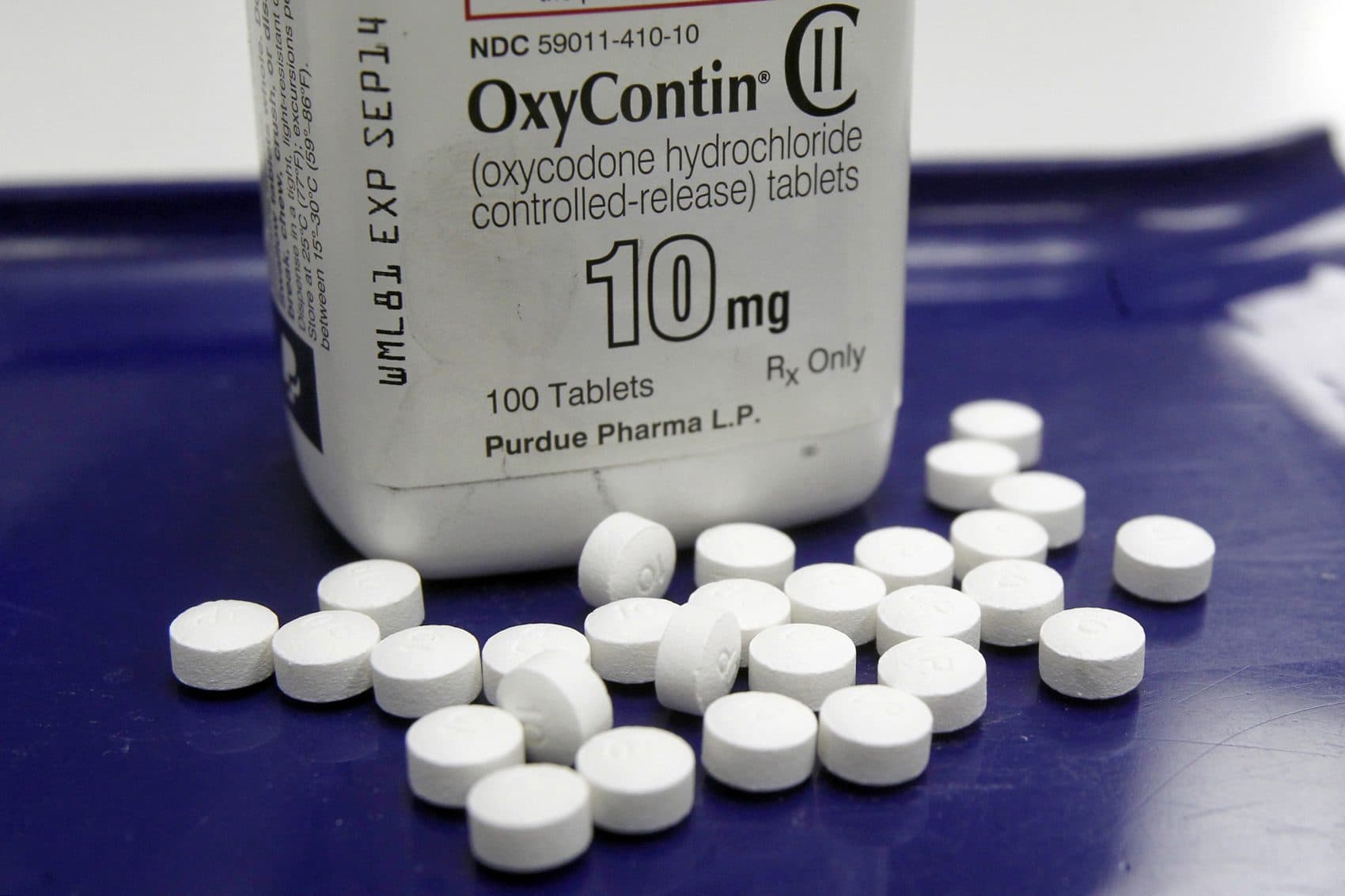
I now know that everything that I was taught about opioids was wrong.
My thinking began to change after meeting a patient I’ll call Danny. A man in his 50s, overweight and over 6 feet tall, he was an imposing physical presence. I could tell he had once been handsome before years of living on the streets; even in his hospital bed, his dark brown hair was impeccably groomed.
Danny had recently left a physical rehab center where he had been given the largest doses of opioids I had ever seen for his chronic back pain. Eventually, he was sent out onto the streets with a week’s prescription and no followup plan. He ran out of pills in a few days.
He walked into our emergency room demanding that we give him opioids. When the ER doctors hesitated, he screamed and threatened them.
This was 2013, two years after the Centers for Disease Control and Prevention had declared that America was in the midst of a prescription drug epidemic. Yet most physicians continued to write prescriptions for opioid medications at record levels.
We had been taught that patients were either in pain or they were drug-seeking addicts -- never both. Patients with chronic pain who started to show addictive behaviors, we were told, were not addicted but “pseudo-addicted,” suffering because we were not giving them enough opioids.
"Pseudoaddiction can be distinguished from true addiction in that the behaviors resolve when pain is effectively treated,” according to a statement in 2001 from the American Pain Society and the American Society of Addiction Medicine. Even illicit drug use was to be seen as a sign that we were not giving enough opioids.
In other words, don’t question your patient’s behavior: Prescribe more pain pills.
The concept of pseudoaddiction, I recently learned, was coined by David Haddox, now a longtime employee of opioid-maker Purdue Pharma and former chairman of the American Pain Society.
Beyond that single 2001 statement, there has never been empirical evidence that pseudoaddiction is a legitimate diagnosis. Yet, in spite of its questionable assumptions, the term was doctrine in pain treatment while I was in medical training, spread throughout the medical community by pharma-sponsored lectures and educational materials.
It was this line of thinking that guided me when I was taking care of Danny. I did not want to give him the opioids. But I worried that I was acting out of bias -- that I didn’t want to give Danny opiates because he was living on the streets, he was unpleasant, and he intimidated me. With all this in my head, and my desire to win Danny’s trust, I decided to give him the medications. My training taught me that it was the right thing to do.
All of us who continued to prescribe these pills closed our eyes to his intensifying addiction.
For the next few days, I walked into Danny’s room every morning to check on his progress. After each dose of opioids, I saw his head drop, his pupils shrink, his breath slow -- early signs of an opioid overdose.
I had followed all the guidelines, but I knew then that I hadn’t given Danny the care he needed. All of us who continued to prescribe these pills closed our eyes to his intensifying addiction. After about a week, I sent Danny back out onto the streets.
Why Didn't We See?
It’s hard to understand now why I couldn’t recognize that Danny was suffering from chronic pain and addiction, or that the two commonly coexisted. It is even more painful to acknowledge that during most of my medical training, the teaching I received was so thoroughly dominated by corporate interests pushing pain prescriptions that we let it blind us to flimsy data and even our own clinical experience.
When some physicians were reluctant to prescribe opioids, hospitals pointed out their importance in increasing patient satisfaction scores. When it was noted that racial minorities received fewer pain pills, hospitals encouraged physicians to prescribe more opioids to everyone in the name of reducing disparities. We accepted teaching from pharmaceutical companies that opioids caused addiction in less than 1 percent of patients with “legitimate” pain, and that they were effective for chronic pain.
While opioids certainly have a role in acute pain, there was never any hard evidence that they were effective or safe for chronic pain conditions. When OxyContin, Purdue’s blockbuster opioid, received FDA approval, the company had conducted no studies on how often longer-term consumers developed an addiction. And studies that were used to justify prescription opioids for chronic pain lasted just six to 12 weeks.
We now know that having a diagnosis isn’t a magical safeguard against the dangers of these drugs. A quarter of those who are prescribed opioids for chronic pain will misuse them, and about one in 10 will develop an opioid addiction. And the first-ever study of opioids for chronic pain to last at least 12 months, published this year in JAMA, found that opioids were less effective than other medications for arthritis and chronic back pain, and had twice as many adverse effects.
Some doctors also believed that they could accept all-expense-paid trips to places like Boca Raton and Scottsdale funded by pharmaceutical companies, free lunches and free samples from pharma reps, follow guidelines written by doctors with multiple conflicts of interest, and still make the right decisions for patients. We ignored — and continue to ignore — research that suggests as little as $20 in food changes doctors’ prescribing practices.
Looking back, it is clear that opioid manufacturers offered an easy answer to the difficult problem of chronic pain, allowing doctors to feel like we had done something to help our patients. As Dr. Anna Lembke, program director for the Stanford University Addiction Medicine Fellowship, said in a talk last year, “There’s tremendous pressure on doctors to palliate pain, to prescribe pills and perform procedures because that’s what pays, and to please patients because patients have become customers. Guess what? Opioids are a pretty good solution to that problem.”
Patients mistakenly think that I can write a prescription to safely wipe all their pain away -- and it’s uncomfortable for me and other doctors to admit that we can’t.
Colleague And Patient Challenges
Now, even when I try to do the right thing by limiting opioids, my efforts are often undermined by other doctors with freer prescription pads.
Recently, I was unable to convince one of my patients of the dangers of opioids. We talked about it over several visits. I knew that she had an anxiety disorder, a huge risk factor for abuse. I knew that she had little social support. I knew that the opioids might provide her short-term relief, but were unlikely to help with her chronic nerve pain, which she would probably live with for the rest of her life.
But even though I talked to her about the risks, she still kept asking for pain pills. One day, I gave in. I gave her a few weeks of pills until her scheduled surgery for chronic pain. After her surgery, I got a note from her surgeon: She had been discharged from the hospital with 30 days of high-dose, round-the-clock opioids with no followup plan. I haven’t seen her since.
Dr. Andrew Chambers, director of addiction psychiatry training at Indiana University School of Medicine in Indianapolis, shares my frustration.
“The biggest cause of relapse in my [opioid-addicted] patients is getting health care from a dentist, a surgeon, a primary care doctor or an ER doctor," he told me. "How do I treat addiction that’s being caused by two other doctors? If I want to, then I need to track them down and convince them what they’re doing is wrong, and I don’t get reimbursed for that."
Moving forward with patients means starting with honesty about our limitations as providers. Lembke says she breaks the truth to patients this way: “There’s a possibility that there’s nothing that modern medicine has that will help your pain, and I’m very sorry about that. But at the very least we can try to not make things worse.” Lembke explains to them that opioids may help in the short-term, but the only safe solution is “to harness your creativity to find how to make your life worth living, even while we may not be able to stop your pain.”
Pills alone aren’t the solution, Lembke tells her patients, and I’ve started telling mine. Medications all have potential side effects whose consequences multiply the longer they’re used. Safer, more effective therapies long term include things like physical therapy, psychotherapy and mindfulness, which, unlike opioids, have all been shown to improve quality of life.
When our goal is primarily palliative care, opioids are an important treatment option, including for frail elderly patients who cannot safely take alternative medications. And for many patients who are on high doses of opioids and have not shown any signs of addiction, it may be safer to continue them, or discontinue at a very slow pace and only with the patient’s buy-in.
For many, however, this option is no longer available, as some physicians refuse to prescribe opioids under any circumstances, or to take on patients on chronic opiate therapy. These patients are left without support as they abruptly discontinue medications they have been taking for years, and may be physically dependent on.
We have failed to come to grips with the scale of destruction we have created ... and the work we have to do to combat this epidemic and prevent future ones.
When patients show signs of an addiction, many physicians opt to simply sever ties with the patient. Few offer treatment. Buprenorphine, a drug used to treat opioid addiction like methadone that also helps prevent overdose, is an important option I’ve seen work in practice. Buprenorphine and methadone reduce mortality for patients with opioid addiction by half. But only 3 percent of doctors are certified buprenorphine providers, and fewer than a quarter of residency programs offer training. How can we interpret these statistics except as a lack of seriousness about addressing a crisis we helped create?
Things have changed since I was an intern. Some physician groups, including the American Medical Association, are eager to tout successes such as decreasing numbers of prescription opioids. These efforts are important, but they are belated to say the least, and woefully anemic. We have failed to come to grips with the scale of destruction we have created, the ways our clinical decision-making was and still is vulnerable to corporate greed, and the work we have to do to combat this epidemic and prevent future ones.
Patients have a right to be angry with us for the way we’ve (mis)treated them with opioids. We need to give each patient the time they need, make changes slowly, and understand that some will not be able to get off of these medications. We need to ask for help from colleagues and demand that our institutions support safe opioid prescribing and addiction treatment.
Every generation of physicians has to work to undo the mistakes of its predecessors. It is the nature of working in a constantly evolving field. But the physician-fueled opioid epidemic is something different: the result of an effective marketing campaign that has killed hundreds of thousands of people.
As a medical community, we continue to play fast and loose with the corrupting influence of money on our clinical decision making. We allow it into our guidelines, our most prestigious societies, our medical education, our patient advocacy groups, our offices and operating rooms.
Important progress has been made. We are exposing fewer patients to these dangerous and largely ineffective drugs. But the fundamental weaknesses in American medicine that led to this crisis remain unchanged: short time with patients; a customer-service mindset that prioritizes satisfaction over good medicine; the largely unchecked influence of money on our providers and health care leaders; and an unwillingness of physicians to diagnose and treat addiction.
The opioid epidemic has laid bare the flaws of American medicine. We should be willing to look at them. Otherwise, this will not be the last epidemic we create.
Elisabeth Poorman is a primary care doctor in Everett, Massachusetts, and a clinical instructor at Harvard Medical School. She is on Twitter at @DrPoorman.