Support WBUR
Losing to Lyme
Many Seek Care At Boston 'Tick-Borne Impairment' Clinic That Tries To Avoid Taking Sides On Lyme
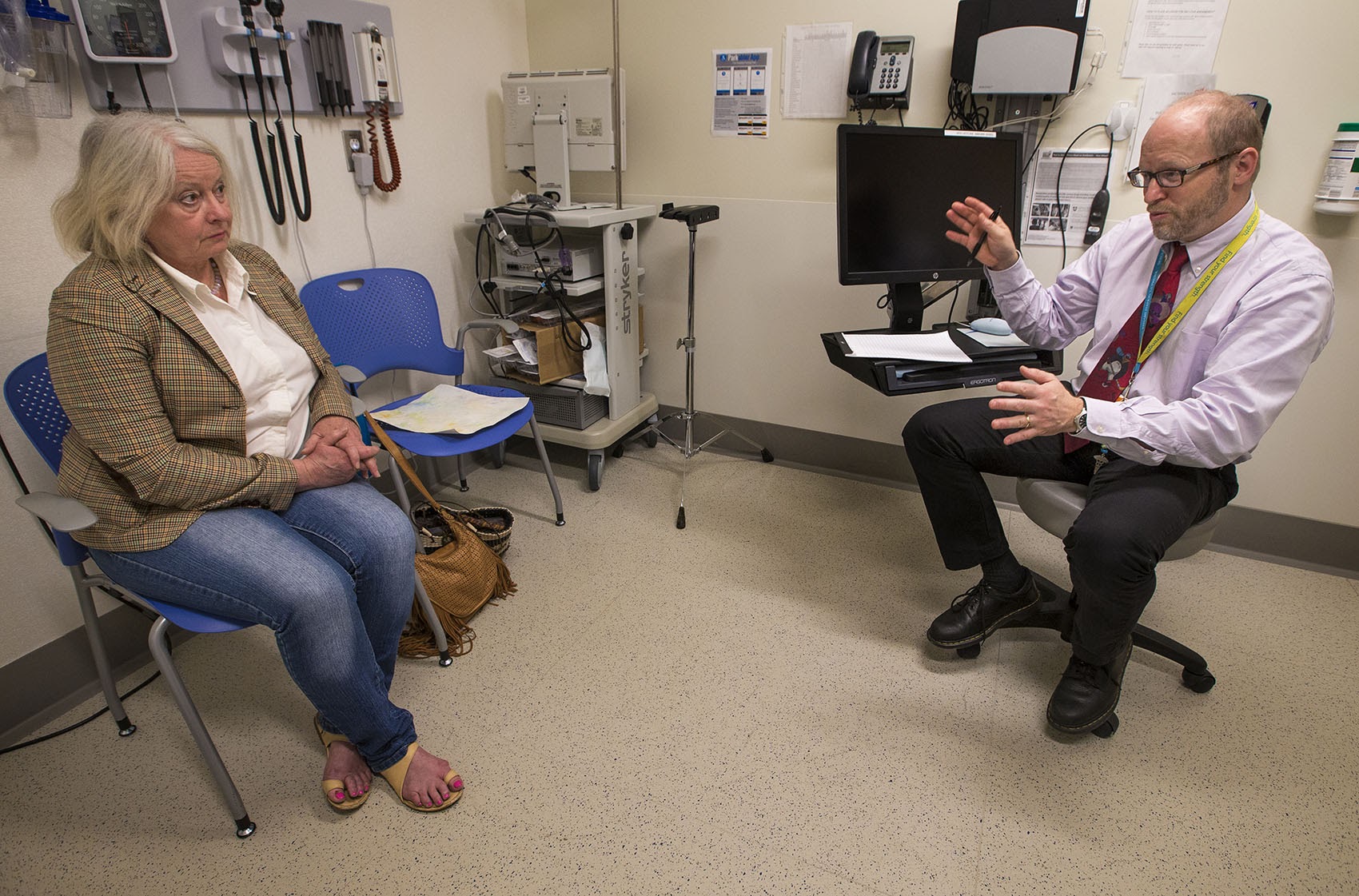
Dancing was Jean Marie Hart’s first love. “Dance was everything for me in my life," says the 62-year-old from Hull. "That’s how I identified myself.”
But now, “I see myself as a stick figure," she says. "Very two-dimensional. Because I have a lot of pain.”
First bitten by a tick as a newlywed on Nantucket in the late 1980s, Hart has been struggling ever since with bouts of joint pain, and cognitive difficulties like brain fog and word searching. She sought help from countless doctors over 17 years until, in 2005, she was diagnosed with Lyme disease by a positive blood test.
The diagnosis did not solve her problems. Despite trying a number of homeopathic therapies and extended antibiotic treatments, Hart still suffered repeated relapses of her symptoms.
So last year, she turned to the Dean Center for Tick Borne Illness. Based at the Spaulding Rehabilitation Hospital in Boston, the Dean Center sees patients who complain of long-term symptoms linked to Lyme disease as needing rehabilitation, much as patients with concussions do.
Instead of focusing on the most contentious Lyme disease questions -- diagnostic labels, long-term antibiotics -- physicians at the Dean Center sidestep the controversy and focus on treating patients’ symptoms.
“Because when people present with impairment, we certainly feel like we should be doing something about it,” says Dr. David Crandell, the clinic’s co-director, who favors the term “tick-borne impairment” to describe what afflicts its patients.
A Yearlong Waiting List
So when Hart came to the clinic, Crandell listened to her for 90 minutes, sorting through reams of old medical files and blood tests, and referring her to various specialists. Among her treatments: speech and language therapy, aqua therapy, a coping skills group, and one-on-one psychological counseling. Most are covered by her insurance; the counseling is free.
Hart had to wait five months to see Dr. Crandell, but she says it was worth it.
“He really understood what patients with Lyme disease go through and how we suffer,” she says. “That was such a breakthrough for me, because it’s so hard to find a doctor that understands this disease.”
Hart is among the 650 patients who have been treated by Crandell and clinic co-director Dr. Nevena Zubcevik in the two years since the Dean Center opened. Patient demand for care there remains overwhelming, to the point that in recent months, the waitlist reached a year long.
Currently, the clinic has stopped putting patients on the waitlist; it hopes to expand clinical services for more appointments next year.
As it expands, the clinic will face the high demand for care and also a challenge unique to Lyme disease: Can it maintain a neutral position in possibly the most contentious field in medicine?
The Lyme Wars
The Lyme Wars is the common term for the rancorous debate over Lyme disease.
On one hand, I’ve heard frustrated physicians express their disbelief in “chronic Lyme,” and concern that patients are being taken advantage of by doctors seeking to make money by over-diagnosing Lyme and offering expensive treatments like long-term antibiotics.
On the other, I’ve heard from suffering patients who felt their symptoms were dismissed by many previous doctors as “all in your head,” yet they desperately seek a diagnosis and treatment to help them get back to normal.
In my training and now in practice, I’ve seen controversies in medicine, but nothing else quite like this. The Lyme Wars have led to distrust, dividing lines and code words like LLMD — “Lyme-literate MD,” often shorthand for physicians willing to deviate from guidelines on the prescription of long-term antibiotics — if you’re on one side, and IDSA — Infectious Disease Society of America -- guidelines if you’re on the other.
The heat of the conflict has alienated patients from the medical system, and physicians from patients suffering with symptoms like fatigue or brain fog that don’t lend themselves to a clear, easy diagnosis.
Adding to the controversy, there are no official numbers on how many people are affected; the distrust runs so deep that no official study has been done. While an estimated 40,000 to 50,000 people get Lyme yearly in Massachusetts and over 300,000 nationwide, we only have estimates that suggest anywhere from a “small percentage” to 40 percent can end up with chronic symptoms.
Amid all this controversy, every Lyme clinic faces one particularly thorny question: whether doctors should prescribe long-term antibiotics.
The IDSA, the leading national group of infectious disease specialists, issued guidelines in 2006 saying antibiotic treatment should stop at four weeks, max. The smaller International Lyme and Associated Diseases Society developed different guidelines suggesting longer treatment with antibiotics is sometimes necessary.
But the long-term antibiotics question has been looked at in high-quality, randomized studies with placebo controls, says Dr. Paul Auwaerter, a Johns Hopkins professor and president-elect of the Infectious Disease Society of America.
“And in these prospective studies, it's been determined that there really isn't a significant or durable benefit to additional antibiotics,” he says.
As a result, the American Academy of Pediatrics, American College of Neurology, American College of Rheumatology and the Infectious Disease Society of America all recommend against long-term treatment with oral or intravenous antibiotics for post-treatment Lyme disease syndrome. So do equivalent physician societies from Switzerland, the United Kingdom, France, Canada and the European CDC.
Against that backdrop, the Dean Center does not currently prescribe antibiotics — except, Dr. Crandell says, in rare, clear-cut cases of acute Lyme disease.
Crandell says that policy is the clinic’s attempt to steer clear of the swirling antibiotics debate. “We tried to position ourselves not on either side, but on the side of the patient and caring," he says.
"We tried to position ourselves not on either side [of the Lyme Wars], but on the side of the patient and caring."
Dr. David Crandell
The Dean Center does, however, tell potential new patients in an email that, “We work together with your current Lyme/Tick Borne Illness Literate doctor,” and provides a list of Lyme-literate MDs to help patients find a clinician.
And the Dean Center's Dr. Zubcevik is an invited speaker at an annual International Lyme and Associated Diseases Society conference this fall. So even as the center tries to walk a fine line in the Lyme debates, truly neutral ground is hard to find.
Hart, the patient from Hull, who would like to include antibiotics as part of her treatment, has not yet found a doctor to prescribe them. She currently has insurance through MassHealth, the state's Medicaid program, and no physicians that take her insurance are willing to prescribe antibiotics for her condition, she says.
To see an out-of-network doctor who would prescribe long-term antibiotics, “it’s out-of-pocket expense, you know, $850 to $1,200 just to walk through the door,” she says.
Do Alternative Treatments Work?
Other Lyme treatments also spark some debate, though far from "Lyme Wars" level.
The Dean Center often refers patients to specialists for well-accepted rehabilitation techniques, like Hart’s physical therapy or aqua therapy. But they also refer for complementary and alternative therapies, like acupuncture, yoga or reiki, which are not as widely accepted by the medical community because little research backs their use in Lyme patients.
For example, one study examined over 30 alternative therapies that are marketed to treat people with Lyme disease, and stated: “The efficacy of these unconventional treatments for Lyme disease is not supported by scientific evidence, and in many cases they are potentially harmful.”
Auwaerter, the Johns Hopkins professor and one of the authors on the study, says, “There really is not anything other than practice experience and hypotheses as to whether [alternative treatments] might help.”
On the other hand, that “practice experience” can mean a major difference in helping a patient manage a chronic, debilitating condition. Many patients at the Dean Center, including Hart, find them very helpful, they tell the staff.

'It's A Very Isolating Disease'
All Dean Center patients are also offered mental health support. In the five months that Hart waited to see Dr. Crandell, the center started her with a coping skills group, run by Kerry Lang, its mental health counselor.
“I’m a Lyme sufferer myself so they know that I get it,” Lang says. “What I really try to do is build a sense of community. I think that gives patients a sense of empowerment, but also just the validation.”
Such support was precisely the goal of benefactors Brandi and Chris Dean, whose gift — they have declined to make the size of the sum public — made the Dean Center possible.
Brandi Dean herself was diagnosed with Lyme in 2011, after multiple doctors dismissed her symptoms as anxiety due to caring for two young children. As part of the donation from the Deans, mental health counseling at the center is free.
“I met a few people who were struggling, who lacked the support system that I had," Brandi Dean says. Some died by suicide. “So it was important to me to have someone available as a mental health counselor.”
Hart felt a similar sense of abandonment, and difficulty convincing doctors there was a problem. “It’s a very isolating disease, because you don’t look sick,” she says. “It’s an invisible disease.”
Things have gone so well lately, Hart says, that she started her own Lyme support group that meets once a month in Hingham.
The Rehab Approach
The Deans chose Spaulding because of its experience providing long-term care for patients with debilitating, chronic illnesses of all types.
“We thought, because of their open mindedness and compassion, that they would be more willing to take on our patients,” Brandi Dean says. “It takes a team of people with an understanding of the debilitating effects of Lyme disease.”
And it's a team whose approach centers on rehabilitation: techniques and therapies to help patients regain function and learn to cope with chronic illness.
Before leading the clinic, Dr. Crandell specialized in amputee rehabilitation, receiving a public service award for his work with victims of the Boston Marathon bombing. But “whether it’s my area of expertise or not, as a full service physical medicine and rehab physician, it’s in our bandwidth,” Crandell says, referring to his and Dr. Zubcevik’s specialty.
Most other academic centers that focus on post-treatment Lyme disease syndrome are run by internists specializing in infectious disease, like clinics at Brown University or Johns Hopkins.
Often, the focus is on determining if a diagnosis of Lyme is correct, and if additional antibiotics are needed. At Columbia, a neuropsychiatrist runs the specialized Lyme clinic.
Dr. John Aucott, director of the Lyme Disease Research Center at Johns Hopkins, says rehab physicians have a special advantage: “They have significant experience treating the symptoms and focusing on function, as well as lots of experience with cognitive symptoms and fatigue,” he says. “It’s very complementary to what an internist does."
Medically Familiar Symptoms
Patients come to the Dean clinic with many diagnostic labels -- “chronic Lyme” or “post-treatment Lyme disease syndrome,” among others.
(Lexical note: Diagnostic labels in this realm are contentious. The term “chronic Lyme” does not have a clear definition, meaning different things to different people. The CDC uses “post-treatment Lyme disease syndrome” but this has very strict diagnostic criteria.)
Dr. Crandell’s preferred term, “tick-borne impairment,” or TBI, is a play on words: In medicine, TBI is better known as the initials for “traumatic brain injury.”
Crandell says the term is not meant to suggest his patients have brain trauma; rather, it’s a reminder that many of their symptoms are medically familiar, and amenable to treatments familiar to rehab doctors who routinely treat brain injury.
"For Lyme, we’re where we were for concussion 20 years ago."
Dr. Nevena Zubcevik
At first, some of the Spaulding therapists worried they didn’t know how to treat Dean Center patients. Dr. Crandell disagreed.
“You know how to take care of people with brain injury, you know how to treat people who have had severe deconditioning and fatigue, right?” he recalls explaining. “The label, the designation of tick-borne illness is just the entry point to a rehabilitation care system that actually could help.”
Dr. Zubcevik compares tick-borne impairment to concussion 20 years ago, when persistent post-trauma symptoms were little understood. In time, “post-concussive syndrome” came to be described in medical journals, and efforts could begin to prevent it.
“Now, every kid who is riding a bike is wearing a helmet,” she says. “For Lyme, we’re where we were for concussion 20 years ago: it’s misunderstood by the medical community, the pathophysiology, the mechanism of illness is not quite understood.
“We don’t have the same movement for prevention,” she adds. “Every little kid should be putting on insect repellent. Alongside their helmet, there should be insect repellent. But that is awareness that we lack.”
It’s too late for Jean Marie Hart to prevent her impairment, but she says with the Dean Center’s help, she’s feeling much better. She recently signed up for an aqua dance class, and even took a foxtrot class.
“I like to say now, because of my experience with the Dean Center, that it’s invisible but I’m not alone,” Hart says. “It’s been incredibly helpful to bring me back… to a more three-dimensional being.”
Correction: An earlier version of this post mistakenly gave the wrong first name to Dr. John Aucott. The post has been updated. We regret the error.
This article was originally published on August 25, 2017.