Support WBUR
Harvard Study Of Skeletons Suggests Much Age-Related Arthritis May Be Preventable
For more than a year, Harvard researcher Ian Wallace scoured the country for skeletons. Thousands of them.
No grave-digging was involved. Wallace unearthed the bones in academic collections that ranged from ancient remains found by archaeologists, to 19th-century bodies never claimed at morgues, to cadavers donated recently to medical schools.
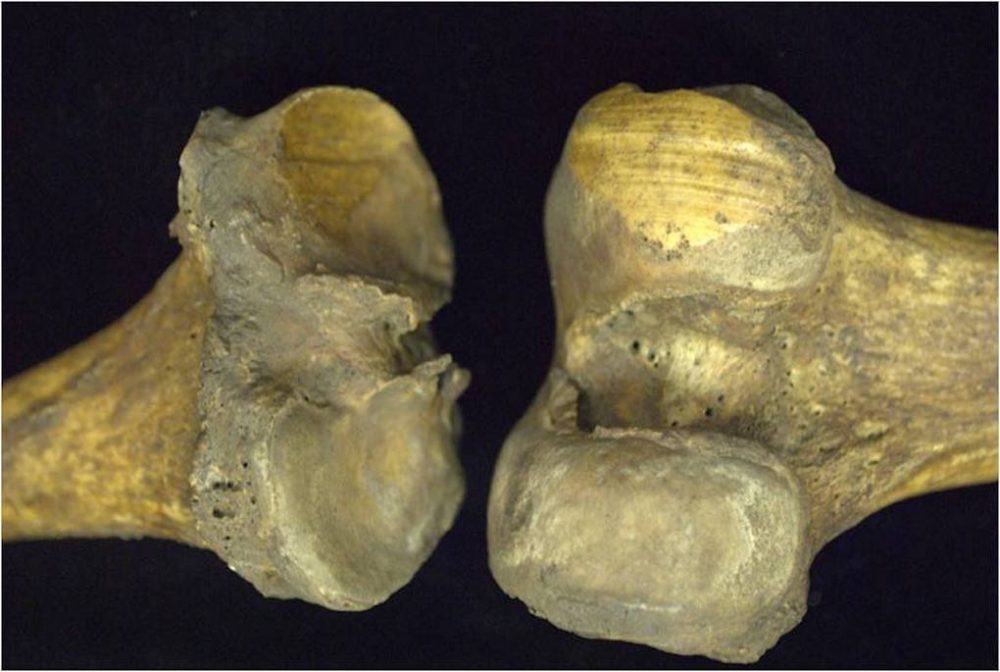
His quest: to gauge the rise of osteoarthritis, the most common form of arthritis, which tends to come with age and affect hips and knees. He checked the knees of more than 2,000 skeletons for a telltale polished look, called eburnation, that means the bones have been rubbing against each other.
The finding: Knee osteoarthritis has doubled in prevalence since the mid-20th century, Wallace and colleagues report in a paper just out in the journal PNAS.
Of course, everyone who pays attention knows that arthritis has been on the rise as Americans live longer and tend to weigh more, imposing heavier loads on aging joints. Initially, Wallace says, doctors responded to the finding that arthritis rates were up dramatically with a resounding ho-hum.
But then came the statistical kicker: Even after the research team adjusted for weight and age, they found the doubling in arthritis rates.
"That's when people's eyes got big and they started scratching their heads," Wallace says. "This is a pretty major revelation for physicians, because it means that tons of cases of this disease that they encounter in the clinic might not be due to the two risk factors that receive by far the most attention — old age and obesity."
And it could be a revelation for anyone who hopes to avoid the aches and pains of arthritis: If our ancestors had far less arthritis than we do — roughly 8 percent of the early skeletons vs. 16 percent of the more recent ones — there's hope that we could figure out what they were doing right.
"The most important message here is that we shouldn't consider arthritis a wear-and-tear disease of age," says Harvard professor Daniel E. Lieberman, senior author of the paper. "Arthritis is a disease that becomes more common as you age, but it's not caused by 'wear and tear'; if anything, it might be caused by the absence of physical activity," so a major way to prevent arthritis could be moving more, not less.
Though still just a hypothesis, physical inactivity is his prime suspect, he says: "It is one of the biggest differences between people who live today and people who lived in the past whose risk of arthritis was much lower" — like many of our grandparents, who tended to sit much less and walk much more than we do.
When Lieberman says wear and tear does not cause arthritis, it still may seem counter-intuitive. After all, joint injuries greatly increase the risk of arthritis, and aging seems so linked to things "wearing out."
But what goes awry in arthritis is looking more complicated than just mechanical overuse, says professor David Felson of Boston University Medical School, a co-author on the paper.
"Joints biologically develop to bear a load, and bear stress across them," he says. "When they aren't able to do it well, they break down. And that's what's going on here — they're somehow not able to withstand the stress that's put across them."
What's making them vulnerable like that is the central question, Felson says. The paper found such a large difference over time that it's likely due to more than one factor, he says, but it's plausible that inactivity is having an effect.
Exercise makes joints more stress-resistant, he says: "Their cartilage gets thicker; the muscles that support and protect the joints get stronger. And joints are hardier when you're active, so the absence of activity isn't necessarily good for our joints."
But is it ever too late for exercise? Say, after arthritis has already hit hard?
"I think probably it can always help," Felson says. "The issue is: When your joint is already far gone, is it a good idea to suddenly engage in physical activity? And the answer is probably no. So it depends on where you are, the stage of disease."
Not to over-promise: Physical activity by no means guarantees arthritis prevention. Felson notes that arthritis has been found in Egyptian mummies; it has also been found in Neanderthals.
But the skeleton findings do point the way toward additional research to pinpoint exactly which factors are at work in the rise of arthritis, and how to counteract them.
"Your probability of having arthritis today is more than double at a given age what your probability of having arthritis was if you had been born before World War II," Lieberman says. "And obviously, genes for arthritis haven't swept the population since World War II. It's something about the way we're living today that's changed. And those are factors that we can shift."
