Support WBUR
What Difference Does It Really Make To Talk About Dying Earlier?
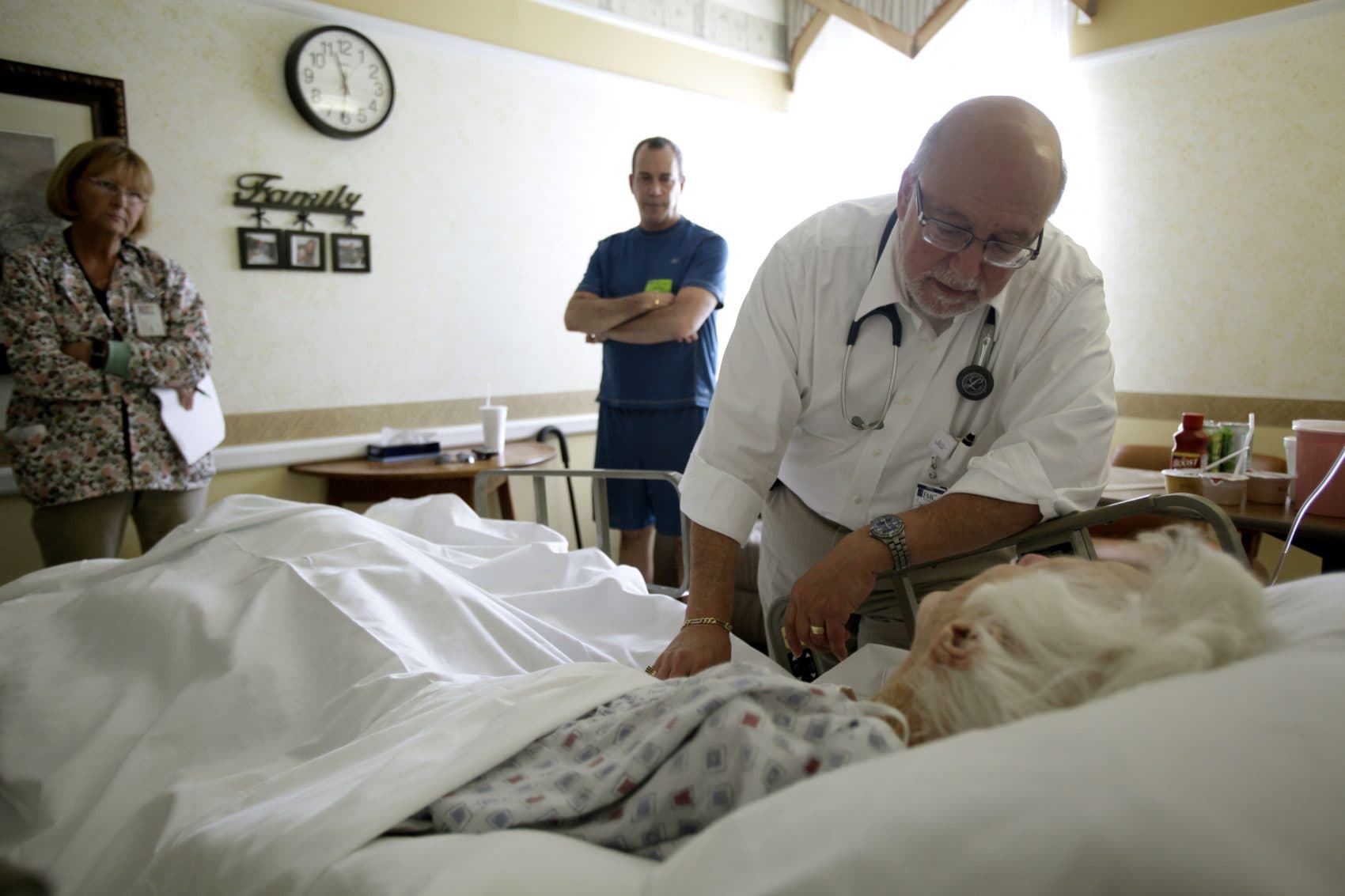
For years now, patients with serious illnesses, their family members and medical staffers have been encouraged to discuss their wishes well before the end of life draws near. It makes sense that such conversations can lead to better deaths — but how much of a difference do these end-of-life talks actually make?
They seem to cut anxiety and depression quite a bit, according to a four-year study that followed 278 Dana-Farber Cancer Institute patients with advanced cancer.
The study enrolled half its subjects in the Serious Illness Care Program developed by Ariadne Labs, the health-care innovation center founded by famed physician-author Atul Gawande, while half got usual care.
Among those in the serious illness program, moderate to severe anxiety was only half as common as among those in the control group, the study found. And that improvement persisted for months.
But when it came to affecting medical treatment — reducing unwanted or unhelpful measures — the study found no significant effects, perhaps because its sample size and the number of deaths were small.
It found no clear improvement on dying more peacefully or getting care tailored to personal goals, and no change in survival time. End-of-life conversations did tend to happen a couple of months earlier, about five months before death.
"It is disappointing that relatively strong improvements in measures of process translated into limited effects on patient outcomes," says a commentary on the study in the journal JAMA Internal Medicine.
Still, it says, oncologists should start end-of life conversations early, "Not because this will necessarily improve outcomes, but because patients want, require, and deserve to know what is coming."
My personal reaction: Having earlier and more end-of-life conversations clearly make sense. But many clinicians have expected them to bring major reductions in futile care. Does this initial lack of apparent medical impact perhaps mean that dying is just so terribly hard that even better conversations can't make much of a dent?
I asked Dr. Susan Block of the Dana-Farber Cancer Institute, who led the creation of the Serious Illness Care Program, and she kindly responded that it was a brave and important question, and that yes, "Dying is incredibly hard."
Then she shared a personal experience:
My husband died three-and-a-half years ago. We had conversations throughout his illness. He was very brave about having the conversations. When he approached the end of his life, I knew exactly what he wanted. And his doctors knew exactly what he wanted. And without that, I think it would have been a much worse set of decisions.
I would have been conflicted. My children would have been conflicted: Should we send him to the ICU? Should we discontinue his ventilatory support? We wouldn't have known that the doctors knew [what he wanted]. We wouldn't have necessarily trusted that they would do it. We felt that we knew, and the doctors knew, there was no conflict, there was no ambivalence, there was no regret.
And I think that is a really extraordinary outcome. And it made the subsequent time, when we were trying to come to terms — as we still are — with my husband's death much easier on all of us.
Conversations beget conversations. Conversations with doctors beget conversations with family members and vice versa. I think it makes a huge difference, and I've observed it over and over clinically, that when the doctor knows, he or she is better able to support the patient and the family. When the patient and the doctor have a conversation, there's more conversation [of] the family with the doctor, and everybody is more on board about the course of the clinical care.
Ariadne Labs says more than 300 medical organizations are using the Serious Illness Conversation Guide, and research on its impact will continue. More details here in Dr. Block's conversation with WBUR's Jack Lepiarz. The transcript has been edited for length and clarity.
The study found there were reductions in anxiety and depression. How long did that last?
The reduction in anxiety lasted for as long as we could measure it, which was half a year. And after that, because people died in the study, the numbers got so tiny that it was really hard to say anything about it. Depression stayed below but it wasn't statistically meaningful.
The two outcomes that we had thought we might see were patients getting more of the care they wanted and being more peaceful at the end of life, and we weren't able to show that. We don't know if that's because it didn't happen, or because our measures are not good enough — our numbers were too small and we weren't able to pick up a signal.
We're actually implementing this study in an ongoing way at several hospitals here in Boston, at hundreds of hospitals across the United States, and also internationally.
What exactly should these early conversations entail? What should patients and doctors be discussing?
We think it's really important for doctors and patients to talk about what's important and meaningful to the patients. What are their goals? And can medical treatments help them achieve those goals? So we ask patients: What do you understand about your illness? How much information do you want about what's likely to be ahead with your illness? What are your goals in living with your illness? What are your fears and worries? How much are you willing to go through to get more time?
Why weren't these conversations happening in the first place?
I think there are a lot of barriers for doctors as well as for patients. Doctors aren't well-trained to have these conversations. They — we — want to protect our patients and don't want to cause harm by having the wrong conversation or saying the wrong thing. We're concerned about whether we're right about the information — for example, about prognosis. And they're painful conversations even when they're conducted by people who are really good at them.
From the patients' point of view, patients are often kind of ambivalent about getting the information. They know what they want, but they're scared of what they're going to hear. They want to protect their family members. They want to protect themselves. So there's a lot of intense anxiety for both the clinician and the patient.
Is there an ideal time to have that conversation? You want to be sure of the prognosis but you also don't want to wait too long.
We think, in a way, it's never too early to start having these conversations. And right now the first conversation for most cancer patients takes place 33 days before death, and by that time, people are wicked sick, and they're usually in the hospital, conversations are with people who don't know them -- with strangers, sometimes in the middle of the night, with an intern who's kind of harried and has to figure out this information.
We think that is definitely the wrong time to start these conversations. So we really try to help them happen with the clinicians who really know them, and to have it when the patients aren't in crisis. If you think about having the conversation, you should probably have the conversation, if you're a clinician.
What can doctors do, what can patients do to ensure these conversations happen and they happen at the appropriate time?
I think for doctors and other clinicians, it's to think: Is this patient getting sicker? Is this patient having more problems with their illness? And if that's the case, then it's a good time to start having a conversation.
For patients, it's being a little bit more proactive and to say, 'You know, I'm worried about what's ahead. I'd like to have a conversation about my illness and what I'm facing here.'
Readers, are you surprised the study didn't find more of a medical effect? Theories? Did this conversation make you reflect on your own experience or that of a family member?
This article was originally published on March 14, 2019.
This segment aired on March 14, 2019.

