Support WBUR
Concerns Rise About Possible Complications From Steroid Injections For Hip And Knee Arthritis
As an assistant dean at the Boston University School of Medicine, Maria Ober sees a lot of the studies by the school's researchers before they're published in scientific journals. One that crossed her desk last week caused her personal worry: For the last decade or so, she's been getting steroid shots in the problem knee that has pained her ever since a high school tennis injury.
"I just didn't like reading the fact that it might not be doing me any good at all," she says.
The shots do help lessen the pain for a while, she says. But she was "distressed to think about the long-term consequences for my short-term alleviation of pain. Is this really something that I should be doing?"
More than 30 million Americans have osteoarthritis, a chronic condition of the joints that affects mainly older people. Many patients seek relief from the pain it causes by getting injections of steroids into their hips and knees.
Now, a new study out of BU School of Medicine is raising concerns about possible long-term complications from those injections. Its headline asks a troubling question about them: "Perhaps Not As Safe As We Thought?"
The paper's senior author, BU School of Medicine professor Ali Guermazi, says it looked at 459 injections in the hips and knees during 2018, "and we found that the complication rate is around 8%. And that's probably underestimating the real number."
Eight percent may not sound like a lot, but it's more than you'd expect for a procedure that doctors widely consider safe. Guermazi says when he was learning about it 30 or so years ago, the message to patients was that it might not help them, but at least "it would not harm you."
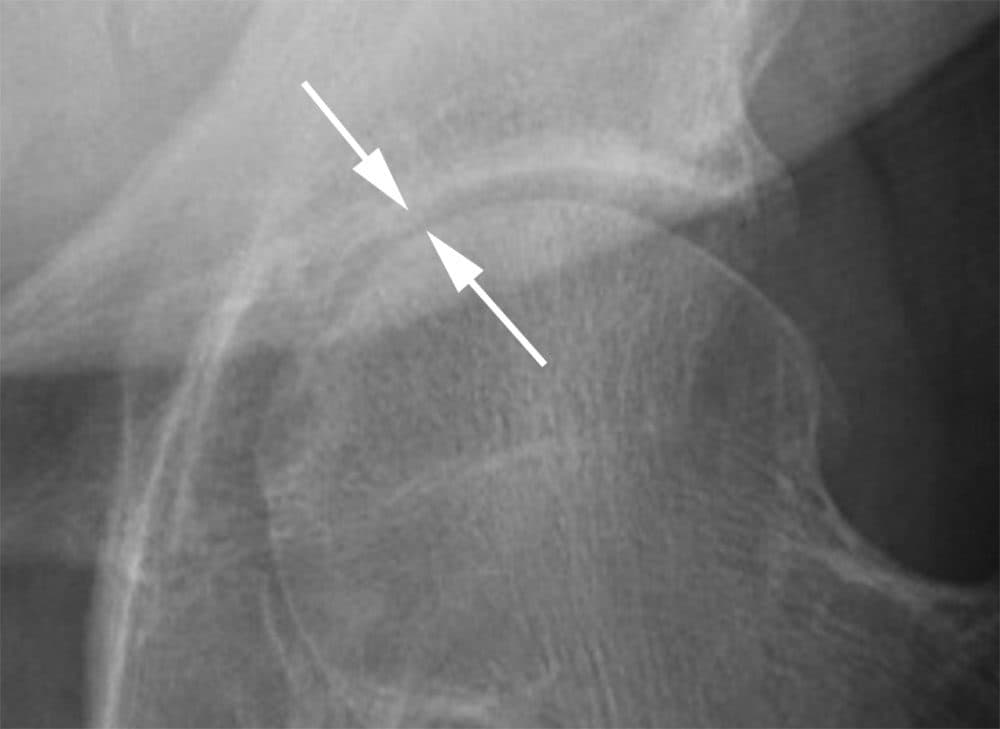
The paper includes MRI images of some major complications, including joint degeneration that progressed very rapidly, fractures and bone loss. Guermazi emphasizes that these findings do not prove that steroids cause the complications.
"What I'm saying here," he says, is "be careful. There is a problem," and "we need more evidence. So that's why we argued in our conclusion that we need more studies."
There have been very few good studies on the long-term effects of steroid injections, says Dr. Richard Kijowski, a professor of radiology at the University of Wisconsin who wrote an editorial published alongside the new study.
"So right now, our physicians have no qualms about either injecting into the joint, in order to treat osteoarthritis, or injecting in other areas of the body," he says.
The injections have become so common that a 2016 study found that more than one-third of Medicare patients newly diagnosed with knee arthritis got steroid injections for it.
Dr. Kijowski says many patients do get relief for weeks or months. But he also cites a small but growing body of evidence that steroids may accelerate arthritis.
"I don't suggest that we should completely frown on this," he says. "I just think that the radiologists, including myself, should basically at least tell the patient that there may be some adverse risk. It may lead to more rapidly progressive destruction of your joint, leading to end-stage osteoarthritis."
If the concerns about possible complications from steroid injections are correct, that is.
Dr. Jeffrey Katz, a professor of medicine and orthopedic surgery at Harvard and Brigham and Women's Hospital, says he does not believe that "people should regard this report as something that should cause terribly much worry."
The new study was not designed to show whether steroid injections caused the complications, he points out, only to alert the field to that possibility. And evidence on the possible link is fairly new and still developing.
"So for clinicians and patients who've been doing injections for several years probably it's worth it to pause and say, 'Do we want to discuss what we think are the benefits and the risks of this again?'"
The paper suggests that there could be sub-groups of patients at particular risk, including those whose severe pain can't be explained by what can be seen on an X-ray. And there could be various explanations for the complications. For example, Dr. Kijowski says, pain relief itself can lead to problems.
"These patients feel so good that they go out and really overload their joints," he says. "That can be a problem as well, because they're structurally weak."
Ober from the BU School of Medicine will be watching what the field says about the potential risks of steroid injections.
"I'm definitely going to have a conversation with my doctor," she says. "I'm curious to know what orthopedic surgeons' reaction to this paper is."
If she's any indication, the paper may already be spurring some of the doctor-patient discussion its authors hoped it would.
This segment aired on October 17, 2019.
