Support WBUR
Universal Flu Shots: Why Did It Take So Long?
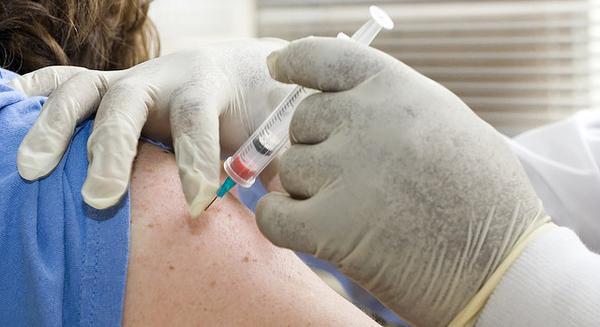
I began with the question, "Why?"
Why, given all we’ve long known about the dangers of flu, is it only now that health authorities have begun to recommend that everyone get vaccinated every year? What took so long, when people were dying along the way?
I gathered pieces of the puzzle in a series of posts (here, here, here and here) and the whole answer has taken shape in my mind now as a story with a beginning, middle and end.
It cannot bring back Nathan Alden Robinson of Newton, the golden 15-year-old son of my oldest friend, who died of flu complicated by pneumonia in 2008. But it may galvanize a few more of us to bare our shoulders for the needle this fall.

Because the moral of the story is: It took so long to get to this point because health authorities were very, very cautious about moving to this “universal recommendation." But medical history was heading this way inexorably. And now that we're here, we may have an unprecedented chance to beat back flu and its usual death toll of more than 30,000 a year-- if we take advantage of it. There's no excuse anymore. Vaccine is all over the place, in department stores, drive-throughs and schools: About one-third of American adults will get our shots outside of our doctors' offices this year, NPR reports today.
Back to my search: I spoke to a CDC spokesman; an international expert; a doctor in the trenches; a man I think of as “Dr. Vaccine” for his fierce, informed advocacy. Still, I felt mystified. Then I found a treasure trove in Dr. L. J. Tan.
As director of medicine and public health for the American Medical Association, he has been an "ex-officio" member of the federal vaccine-recommendation panel for more than a decade, so he serves — unofficially — as part of the group’s institutional memory.
He shared recent flu vaccine history with me, and this wisdom: For the flu vaccine recommendations to change, the panel needed evidence. But to start looking for evidence, something had to "trigger the thought."
[An aside: flu needed a "trigger" like this, but for most vaccines, it's simpler, Dr. Tan noted: there's an unmet medical need. It leads a vaccine maker to develop a new vaccine. And then health authorities consider whether to recommend it.]
So what was the trigger with flu? There was a bad outbreak of a new strain in 2003. Texas and Colorado were particularly hit, and dozens of children died. Before then, public health authorities did not gather data on children's flu deaths. Now, Dr. Tan said, it was clear some pediatric flu recommendation was needed. The data-gathering began, and in the winter of 2004-5, the CDC recommended that all children under 2 be immunized against flu every year.
Flu “has always had a U-shaped mortality,” Dr. Tan said. “The youngest and the oldest tended to die. So that was the easiest recommendation to make.”
But it made no sense to stop there. Among the next-oldest cohort of children, some deaths were also reported, and significant hospital stays. Still, it took time to wrap them in under the recommendation. There were concerns about whether vaccine-makers could keep up, Dr. Tan said. And the science base had to be “incredibly strong — strong enough to stand up to external scrutiny.”
External scrutiny? Might he be referring to the anti-vaccine camp? The multi-dose flu vaccine is one of the last to contain thimerosal, the preservative that some autism activists have long argued could be implicated in autism, despite all the data to the contrary.
Dr. Tan declined to specify, but this is where my mind went: We’re all victims of history. Children with autism could be victims of some environmental or genetic glitches that seem to be on the rise. As their parents struggled to understand autism’s causes and to protect other children, they may have instilled such extra caution in vaccine regulators that it slowed down the adoption of recommendations on vaccines. So fewer children were vaccinated against flu, and more children likely fell sick than would have otherwise.
If the recommendations had moved just a bit faster, might Nathan still be alive? His parents are the best I know, and if they had been told that a vaccine was recommended, they would have gotten him one. So Nathan, victim of a medical rarity, was also a victim of history. Not that it helps to know that.
By 2007, the CDC issued an “encouragement” for all children to be vaccinated against flu. In the fall of 2008, a few months after Nathan died, it came out with the full recommendation that all children be vaccinated against flu. Part of that decision stemmed from the need to simplify, Dr. Tan and others say. Doctors were facing longer and longer lists of the many high-risk categories of children who should be vaccinated, and the vaccination rates were not rising as fast as they should have.
Previous research had shown that sometimes the only way to bridge a gap in vaccine coverage is to switch to a blanket, age-based strategy, when there’s the science to back it, said Dr. Susan Lett. Dr. Lett is the medical director of the immunization program at the Massachusetts Department of Public Health, and has been a member of the federal vaccine panel for the last four years.
Also, she said, “the other thing we know from seasonal flu and H1N1 — and you know personally — is that even people without any risk factors get flu, no matter who they are. Someone who’s perfectly heathy can get it and could have complications and a tragic outcome.”
Yes, I know.
Was part of the hold-up, I asked, some sort of public health calculation of lives versus cost? Did somebody figure that only about 100 children were dying from flu each year, and vaccinating the whole population was a huge undertaking, so it somehow didn’t “cost out”?
I dreaded this answer, but both Dr. Lett and Dr. Tan reassured me. There was no bean-counter who blocked the vaccines, they said. Cost-effectiveness analyses had been done, Dr. Tan said, as they always are, but “cost-effectiveness was never a primary factor with influenza because the vaccine is only ten bucks”-- almost $12, to be exact. And, Dr. Lett pointed out, copious data show that the price of flu is high across the board: from disease and death to absenteeism from school and work. Flu also leads to increased antibiotic use in children, a costly concern.
As Dr. Lett sees it, what happened was “kind of like a paradigm shift that people needed to wrap their brains around — that serious influenza disease was occurring in all age groups, not just babies, toddlers, the elderly and those with high-risk medical conditions.”
Surveillance improved; improved tests became available — the tools and the systems got better. And here, too, history played a role, she said: “A lot of this, I have to say, was probably a side effect of everybody getting ready to be able to prepare for a possible pandemic,” or bioterrorism attack in the heightened vigilance after 9/11.
By last year, of course, children were supposed to get two vaccines: one for H1N1 and the other for “seasonal” flu. And all adults were supposed to get H1N1 vaccines. (In fact, only about 59% of the population is now immune to H1N1 either through a vaccine or a bout of it last year, Dr. Tan said.) This year, everyone is supposed to get just one vaccine, which includes both H1N1 and two other strains.
Last year, I was thrilled by the effects I saw H1N1 having on people’s attitudes. Suddenly, everyone was as scared of flu as I was, and hand-washing went Olympic. And this year, I just assumed that it was H1N1 that pushed us over the edge to a full universal recommendation. But Dr. Lett noted that in fact, if not for H1N1 and the complicated need to manage two vaccines in a single season, the country might well have switched over to universal seasonal flu vaccines last year.
Ah, well. This year, we can get the shots earlier than ever — like, now. On a federal government Webcast last week, Dr. Howard Koh, a top health official, said: “The major message this year is this new universal recommendation we’re promoting. Last year we learned that everybody’s at risk, that everybody is vulnerable, so a new recommendation that’s very important for this season is that everyone six months and older should get the flu shot as soon as it’s available in their community.”
Speaking at Nathan's memorial service, a teacher recalled a classic classroom moment: Nathan was standing nearby when a girl came up and began to hug him for no obvious reason, as girls often did. He met the teacher’s eyes with a helpless, humorous look, as if to say, “Don’t ask me!”
Everybody is vulnerable. To find a shot venue near you, go to flu.gov. It's as easy as typing in your zip code. The flu vaccine, Dr. Tan said, "should not be a vaccine of convenience but rather a vaccine of need."

This program aired on October 4, 2010. The audio for this program is not available.


