Support WBUR
Worms And Germs: Their Absence May Explain Ills From Allergies To Asthma
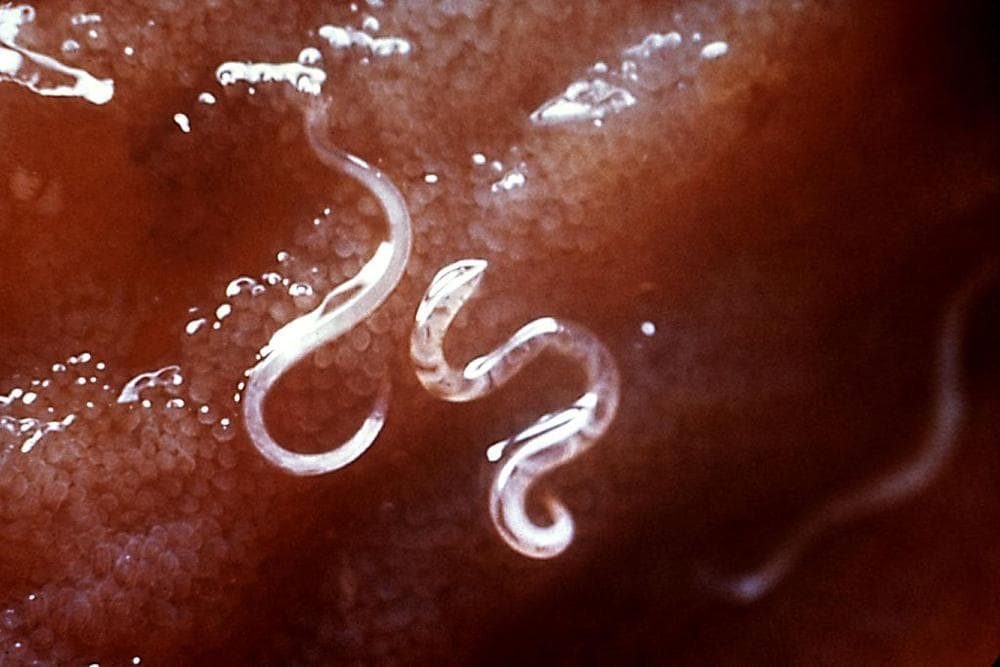
First he hooked me with the hookworms. Who knew there was a whole underground network of people who, in hopes of curing allergies or Crohns disease, go to great lengths — such as stomping about in outhouse offal — to get themselves infected with nasty parasites?
Then he arrested me with the alopecia. I’d glanced at the author photo on the jacket, and something looked a bit off: He wasn’t just completely bald, he also lacked eyebrows and eyelashes. On page 2, he explained that he had alopecia universalis, an auto-immune disease that left virtually no hair on his entire body.

But what kept me reading all through vacation — and really, I’d rather not spend my leisure time with whipworms and “orofecal” bacteria — is that in his new book, An Epidemic Of Absence, author Moises Velasquez-Manoff turned my head around. Ah, the pleasing sound of mental gears grinding as the paradigm shifts!
To me, as a mother and as a health reporter who has written too many sad stories of infection, germs and parasites have ever been the enemy. But now they suddenly looked more like old friends, who could help us more than hurt us — as Velasquez-Manoff sought to test when he went to Tijuana to get infected with his own colony of hookworms.
The book is subtitled “A new way of understanding allergies and autoimmune diseases,” but my summary subtitle would be “A new ‘Theory of Everything‘ about the diseases that now plague modern humans, particularly children: Allergies, asthma, autism, obesity, and more.”
You may have heard of the Hygiene Hypothesis, the theory that allergies are rising so dramatically because modern society is too clean, and our under-challenged immune systems tend to over-react. Velasquez-Manoff takes it many steps further. He argues that without the parasites and bacteria that we co-evolved with for millennia, our immune systems become poorly regulated — in particular, unable to tamp down inappropriate inflammation. And chronic inflammation is linked not just to allergies and asthma but to obesity, cancer, depression — possibly even autism, as he wrote in the New York Times last week. (There's also an excerpt and a Q&A in Wired this month.)
“An Epidemic Of Absence” is a first-class job of science-writing. It takes studies and turns them into riveting stories, moving from the how to the why or the correlation to the causation. But to fully appreciate them, you need to read the book. For now, let’s be ruthless pragmatists: If you accept this theory — and I guarantee that you will by page 300 — what do you do about it?
[module align="left" width="half" type="pull-quote"]'We don't need to be fastidious. Routine hygiene is okay; excessive hygiene may be detrimental.'[/module]
The author asks that very question on page 303, but then gets a bit futuristic, imagining farm gardens inside high-rises and doctors who genotype pregnant women and adjust their microbe population accordingly. He mentions that he’s the father of a young daughter, and that he would never purposely infect her with hookworms as he did himself — but if he knew that it was a sure preventive treatment, and that she was destined for Crohn’s disease and horrible allergies, he might think differently. I wanted to press him about how — if at all — his work translates into health decisions now, in his own family’s life. But first, a word from a scientist.
One of the heroes in "An Epidemic of Absence" is Dr. Joel Weinstock, chief of gastroenterology/hepatology at Tufts Medical Center and a leading researcher on using worms to treat inflammatory diseases.

(He's currently enrolling patients for a major trial using pig whipworms — which die off automatically after two months — in Crohns disease. Earlier studies have found the worms to be safe, he said, and initial results look promising. Later this fall, he said, whipworm studies will begin on ulcerative colitis, and within a few months, on psoriasis and Type 1 diabetes. Contact: 617-636-4593.)
I asked for his practical advice, and took away two main lessons: We must be patient and wait for more solid science. And for the meanwhile, his opinion, which he emphasized is not backed up by data, is "We don't need to be fastidious." (Music to my ears! That's an adjective never once applied to me in my entire life.)
How does that translate?
"It’s okay to have pets in the house. Kids don’t have to wash their hands every time they touch something. If food falls on the floor you don’t have to worry if someone picks it up and puts it in their mouth. Playing in the mud around the house is safe. Everyday, routine exposures to things around us may be helpful. And there’s already data suggesting that if you have multiple animals in the house, you're less likely to get immune-mediated disease.
So routine hygiene is okay; excessive hygiene beyond what is necessary could be detrimental. What is excessive is hard to define, but you see mothers who wipe their kids constantly...People build houses with a separate bathroom for every bedroom. This is a matter of hygiene carried to the X degree. I would say that's not necessary and it could be detrimental, because we know that children raised in households of one bathroom are less likely to get these diseases...
You want kids to interact, you want them to get dirty, touch their animals and let their animals touch them. When you think about it, dogs lick their butts and then lick you, so you're being exposed to the flora of the animal. It's the truth."
Yes, yes, I said, I know it's the truth. I just don't like to think about it. But maybe I should...And now, my conversation with author Moises Velasquez-Manoff, distilled and edited:
You wanted to begin with a major “Do not try this at home” warning: You really don’t recommend that people with allergies or auto-immune disease follow your example and get themselves infected with hookworms from the black market, even though it did help your eczema and your sinuses.
MVM: I don’t recommend that people do what I did. I worry about that. I don’t recommend it for a lot of reasons. I had some severe symptoms. I also saw some benefits. But most importantly, this approach has not yet been shown to work scientifically. You need to have science show that it works, and give us something safe.
I feel like my experiment proved all the different arguments about hookworm true. Did it have a cost? Yes, it was very painful. Did it also change how our immune system works? Yes, it can, it does. In the underground, I interviewed people who did apparently send their diseases into remission, and that’s amazing, and I was able to confirm it. But I also spoke with some people for whom it didn’t work out so well. This isn’t unexpected. If it were a real drug, there will be people who respond well and people who don’t respond. But we have no idea what the ratio is at this point, or if it’s better than placebo. This is not how you conduct science at all.
I think this weird thing may be happening where the underground movement may push the science along just because so many doctors are getting news of it and getting familiar with the literature, and these diseases — like Inflammatory Bowel Disease — are often extremely difficult to treat. So if you can get rid of the parasites easily, then you might ask, what is there to lose? You put it in, and if it doesn’t work, you get rid of it with a quick dose of drugs and it’s gone.
But the flipside is, you’re playing with very important switches in the immune system. What if the treatment worsens some aspects of your condition? Only real trials can tell us what the cost-to-benefit ratio is, who might benefit, and who might not. And another warning. This isn’t in the book because it hadn’t happened yet. I tried to get rid of my worm treatment a month or two ago, and it seemed like my colony was resistant to the treatment, mebendazole. I say ‘seemed’ because I’m not sure, but I still had symptoms afterward. But such resistance is well documented in the literature. I switched to another, more expensive drug, albendazole, and that seems to have forced them out. Again, this is very speculative, but it’s yet another thing for people to think about for people plunging into the hookworm underground.
So now to the “news you can use.” With the initial huge caveat that the science on these particular things may not be nailed down, but we’re living right now, and want to act on reasonable assumptions.
First, I ranked what I was willing to do for my child, and there’s a cost-benefit ratio to each thing. You start with the things you know have little to no cost, but which the science suggests may benefit.
Probiotics
You want to start really early, ideally when the mother is pregnant, and use probiotics of some sort. None of it has been tested in a way that shows it works, but they have a lot of potential benefits and few costs I could see. I had my wife on probiotics when she was pregnant. I wanted to get this regulatory signal going early; the earlier you can direct immune development, the better. There’s very little evidence this works, except for a few European trials that haven’t been replicated. And probiotics given to mothers have been shown in limited studies to change the cytokine profile of breast milk in a way that may be protective against allergies. But I figure – and I may be wrong – that there are few potential costs. So we just used some generic probiotics — a bunch of lactobacilli and bifidobactera.
Caution: There's some potential risk with my prenatal probiotics approach. Scientists are finding that maternal immune equilibrium is very important for fetal health. So to the degree that probiotics upset this equilibrium, they may be counterproductive. That's why actual research is so important. Although current probiotics are usually billed as anti-inflammatory, very few studies have tested them in this capacity. I could, for example, be causing exactly what I want to prevent. So more science is necessary before people take this idea and run with it.
My wife also took flaxseed for the Omega-3s, which fight inflammation.
Daycare
Next is that all the studies show that kids who go to daycare early have less allergies and asthma later — and also less type 1 diabetes in some studies. So our kid is in daycare. That wasn’t intentional. It just happened. Nobody has shown why daycare protects, but it’s probably the sharing of fecal bacteria – the microbial diversity — so the kid gets a nice robust internal ecosystem going early.
And the other thing I talked about in the book a little was Epstein-Barr virus, which, in studies coming from Sweden, locked down the immune system if you got it early. If you get it early, you don’t even have any symptoms. Again, I would wait for an answer from the science on Epstein-Barr, but it may partly explain the daycare effect – that children are getting the virus early, and it changes their immune system in a way that protects against allergies.
And here I thought I was helping my kids by keeping them home when they were little!
[module align="right" width="half" type="pull-quote"]We didn’t even use diaper wipes. It’s so important for the skin barrier to be intact.[/module]
Well, there is some risk to daycare. There are some common cold viruses that if you get them young, they predict asthma later. But no one’s really sure if they cause or if the people who get asthma later have some defect in their defenses to begin with, and they tend to get sicker with the viruses earlier.
Diaper creams
And I would assume you made sure your daughter got no diaper cream, given your section on how skin exposure before oral exposure may lead to allergies?
We didn’t even use diaper wipes. It’s so important for the skin barrier to be intact. You don’t want an irritant. Water is fine, it gets the stuff off.
It’s an interesting issue, the whole skin thing. Ten years ago, the recommendations were to put off eating allergenic foods like peanuts if you have allergies in the family. Now they backtracked and say it’s okay. And my guess is they’re going to say you should start eating them earlier so you develop oral tolerance before skin exposure, which may lead to allergies. We’ll see what the studies under way looking at this say – whether earlier exposure is better or not. But that’s the direction they’re pointing right now.
[module align="left" width="half" type="pull-quote"]I’m not sure that dirt will really help you. It’s very particular microbes that help humans. [/module]
With my kid, I had her eating peanuts and sesame, which I’m allergic to, from a very young age. I would hesitate to recommend that to other people because it hasn’t been proven to work or to protect against food allergies. But it just doesn’t make any sense that kids are suddenly getting allergic from food they’ve always been eating. Unless either our immune system has changed, or the way we’re exposed to the food has changed. As I point out in the book, there’s evidence that both are true.
Dirt and germs
And should we just generally relax about dirt and germs on kids?
Getting the flu is not a good thing. It’s not going to help you. You still want to avoid that. But in terms of dirt, I think everyone needs to relax a little. It’s okay to get dirty. That said, I know some scientists say to let your kids play in the dirt. They say that because it’s a safe recommdation to make. But I’m not sure that dirt will really help you. It’s very particular microbes that help humans, and they don’t necessarily live in any old dirt. If I go to Central Park right now and let my one-and-a-half-year-old play in a mud puddle, it’s probably not going to hurt my kid. But all the research coming out of central Europe suggests that farmers who work with animals, and especially certain animals, like dairy cows, are protected, not necessarily farmers who grow just the crops. That’s a very specific community of microbes.
So dirt may not hurt, but it also won’t get to the heart of the issue, which is that there are certain very specific microbes we need to be exposed to early and chronically. That said, Graham Rook at University College London makes a good case for saprophytes, innocuous bacteria that live in soil and break down organic material. But it’s also important to recognize that we were probably exposed to these microbes by drinking water in the past. That’s direct and chronic contact with our mucous membranes. Very different than playing in the dirt once a week in Central Park.
Farm summers
So maybe we should send our kids to Vermont farms for the summers?
That’s a good question but it may be counter-productive. When studies looked at urban children who went to farms occasionally, they were actually more allergic. You need to have these exposures from a very young age, ideally from before birth, and they need to be chronic.
Antibiotics
How about antibiotics? Do we need to be even more wary of them?
The idea is not to say ‘No antibiotics ever.’ The idea is to talk with your doctor when they prescribe antibiotics and ask, ‘Is there something else? Can we hold off?’ Doctors worry about resistance and try not to over-prescribe them as well. They have their own concerns these days.
Another angle is possibly preventing infections by modulating the immune system with probiotics, so you take antibiotics less — a proactive approach where you’re slightly activating the immune system in a way that protects you. The current generation of probiotics do have some ability to prevent other bad bugs from showing up, simply by occupying the niche. Which brings me to the third possibility: Whenever you take antibiotics, you might want to add probiotics to fill that niche of the good bacteria you’re killing off, so something bad doesn’t move in. In a very fundamental way, it’s ecosystem engineering.
Diet
How about diet?
That’s something else with high benefit and low cost. If you’re eating a varied diet full of plants and whole grains, we’ve always known that’s good for you, and the science on the microbiota now illuminates why it’s good for you: It may modulate the microbiota, your microbe population. So eat a varied, complex, natural diet. Diversity of the microbiota is good. You want to foster that diversity. And McDonald’s does not do that.
I wonder if I should still wash my produce, or could the dirt help?
You want to wash your fruits and vegetables. If you eat organic they shouldn’t have any pesticides and I think washing with water is fine — the microflora will still be there. It’s an unexplored question that I’m sure will be explored more, that fruits and vegetables may have natural microflora that is good for us. They even transmit DNA to our own microflora. The microbes don’t stay in your gut, in other words – they educate your native microbes.
I mentioned one study in the book on the Japanese microbiota. It turns out to have this ability to break down seaweed that the comparison microbiota didn’t have. But the scientists didn’t think that the Japanese were colonized by seaweed bacteria. Instead, they thought that bacteria living on seaweed had transmitted DNA to native microbes in the human gut. It’s fascinating because it gets at this idea, which has become quite fashionable, of localization: It suggests that our internal microbes can acquire information from external microbes in the environment if people are eating the food grown around them — like from the ocean.
Raw milk
You’re adding reasons to go to the farmer’s market. You also sometimes sound surprisingly friendly towards the raw milk camp...
Some people swear by it but there is potential risk of nasty life-threatening infection. Listen to the scientists. They’re saying, ‘Don’t drink the raw milk.’ Even though a lot of people do, but the people who drink raw milk are generally people who know their cows.
Also, if you grow up drinking raw milk, the evidence suggests your immune system is different, it’s slightly activated, you have a better defense against whatever might be in the milk. At this point, the scientists working on this don’t even think it’s the microbes in the milk that protect — though this question is unresolved. They think it’s proteins and other substances in the milk that maybe get broken down in the boiling. If you can figure out what they are, maybe you can just preserve them. One scientist told me that pasteurization is ancient technology and there are other ways to sterilize where you can preserve the constituents of the milk. That’s in the works.
Readers, have I forgotten anything? Please post your questions in the comments below.
This program aired on September 7, 2012. The audio for this program is not available.
