Support WBUR
Troubled Compounding Pharmacy 'Clean' Room Not Clean, Inspectors Say
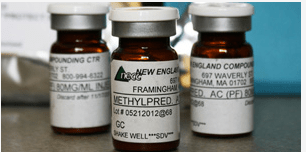
State investigators have found numerous health and safety problems at the Framingham pharmacy allegedly tied to 23 meningitis deaths, but still don't know how fungus got into steroid vials.
Inspectors with the Department of Public Health say they found black particles in vials of steroid returned to New England Compounding Center...the steroid that has caused 23 deaths and made 304 patients in 16 states sick.
The "clean room" where the steroids were produced did not meet basic standards including untested sterilizing equipment, dirty floor entrance mats and protective hoods that weren't cleaned.
Governor Deval Patrick, speaking at a news conference today, extended condolences to all those affected by this outbreak. He says the state will begin unannounced visits of the other 25 pharmacies that mix drugs in Massachusetts and require more specific reporting.
The state's preliminary report is here.
Here are the governor's remarks:
Again, good afternoon. Immediately following the meningitis outbreak at the end of September, our Department of Public Health took decisive steps to isolate and remove the contaminated substances. The Board of Pharmacy, under the direction of DPH, shut down operations at New England Compounding Center and its sister operations, suspended the pharmacist licenses of company leaders, and secured a nationwide recall of the products.
We worked with health care professionals and boards of public health to notify patients who received NECC products. We reminded the Commonwealth's 25 other compounding pharmacies that make sterile injectable medications that state rules require them to have a patient-specific prescription in hand for each treatment they produce, and to follow nationally-accepted pharmacy standards.
And from day one, we have partnered with the CDC, the Center for Disease Control, and the FDA, the Food and Drug Administration, in an ongoing investigation into NECC and its sister operations. I want to this afternoon have Dr. Biondolillo, Director of the Bureau of Health Care Safety and Quality, to brief you on the preliminary findings of that investigation and to update you on our ongoing work with our federal partners. And then I want to advise you of some further action steps we will take.
[Dr. Biondolillo speaks]
[Governor Patrick returns]
Thank you, Doctor. Our joint investigation with the FDA continues. You should also know, if you don't already, that a federal criminal investigation has been launched. Meanwhile, I want to announce that the Board of Pharmacy has voted permanently to revoke NECC's license to operate in Massachusetts, as well as the licenses of the company's three principal pharmacists. Those whose laboratory practices caused this outbreak should never practice pharmacy or manufacture in Massachusetts again.This incident I think also casts a spotlight on a broader issue, as well - the fact that, over the years and for a variety of reasons, some pharmacies have transformed from your neighborhood drug store into large-scale manufacturers that sell products across state lines. Normally, interstate commerce is a matter of federal oversight, but for various reasons there has been little of that over the years. Congressman Ed Markey has aptly called this a “regulatory black hole.” Thankfully, the Congressman is leading the charge to close this gap and we look forward to working with him and his colleagues in the Congress to strengthen FDA's oversight to reflect this new reality.
It's also clear that our own rules here in Massachusetts governing compounding pharmacies have not kept pace with an industry that's changing rapidly. Though consistent with — and in some cases more stringent than — those in effect in other states, it's time, in my view, to update our practices. Accordingly, I have directed the Board of Pharmacy as follows:
First, the Pharmacy Board will immediately start periodic unannounced inspections of compounding pharmacies that prepare sterile injectable medications such as those directly linked to the outbreak. These pharmacies will be inspected at least annually, and more frequently in the case of a substantiated complaint. We will also strengthen the penalties for noncompliance.
Second, we will require compounding pharmacies in Massachusetts to submit annual reports of production, volume and distribution of medications. This reporting will allow us to better identify large-scale operations acting more as a manufacturer, which requires federal licensure and additional scrutiny.
Third, we will require compounding pharmacies to report to the Board all interactions with federal regulatory authorities so that we, here, at the state level have a full picture in each case of what's going on.
And finally, we will form a special commission to examine best practices in other states and potential changes at the federal level, and to advise us on what changes we should make in state law through legislation to further assure the public's safety. I intend to invite industry and regulatory experts, consumer advocates, and designated Legislators to participate as well. The Commission will make recommendations to me by the end of the calendar year.
On behalf of the entire Commonwealth, I want to extend condolences to those who have lost loved ones and encouragement to those trying to recover. No one should live in fear that medicine is unsafe. In these times of constantly questioning the role of government, surely we can all agree that protecting the public's health and safety is paramount. We will make these and any other changes necessary, at the state and, I believe, at federal level as well, to assure that that duty is carried out.
Dr. Biondolillo and I are happy to take any questions you may have.
And here are Dr. Madeleine Biondolillo's remarks:
Good afternoon. Thank you Governor Patrick, for your clear vision in calling on state and federal leaders to develop effective long-term solutions to the regulatory gaps that have been highlighted by these tragic events.
Since September 25th, DPH staff have worked around the clock to conduct a comprehensive investigation of the New England Compounding Center. On October 1st, we were joined by investigators from the U.S. Food and Drug Administration, and we have collaborated with them on all aspects of the investigation since that time.
The investigation of NECC has many components, and is ongoing. DPH investigators have obtained substantial evidence, reviewed Standard Operating Procedures, NECC’s practices and records. Investigators also conducted interviews with NECC staff, and made observational findings while they were physically inspecting the facility.
Our investigators documented several health and safety deficiencies related to the practice of pharmacy at NECC.
Investigators demonstrated that compounded medications ready for distribution were not labeled with patient-specific identifiers, as is required under Massachusetts licensing regulations. With this violation, NECC was operating beyond the scope of their compounding license, instead acting as a manufacturer.
NECC staff also failed to conduct a review of patient-specific medication history and drug utilization reviews.
As has been previously described, there are three suspect lots of the steroid, methylprednisolone acetate, that have been implicated in the majority of infections. DPH investigators documented that on 13 occasions, NECC staff shipped orders from the suspect lots BEFORE receiving their own test results confirming that those lots were sterile. Medication was shipped as long as 11 days before results were received.
Investigators also found that processes for sterilizing medication at NECC was not done in conformance with accepted, standards. Examination of NECC records indicated a failure of the facility to sterilize products for even the minimum amount of time necessary to ensure sterility. NECC also did not conduct proper validation of the equipment used to sterilize product, for example, failing to test their autoclaves on a regular basis to ensure proper function.
On October 2, visible black particulate matter was seen in several sealed vials of methylprednisolone acetate that had been recalled from providers and returned to NECC. That matter was later confirmed by the FDA to be fungal contaminant linked to the outbreak.
In addition to these violations of regulations and patient safety, a variety of other findings showed NECC’s lack of maintaining basic accepted standards of pharmacy operations. Powder hoods in the sterile compounding areas, a physical barrier designed to protect pharmacists from inadvertently inhaling substances while they are being prepared, were not thoroughly cleaned and residual powders were seen.
Mats used to wipe dirt, dust, and other possible contaminants off of shoes before entering sterile areas were visibly dirty, soiled with assorted debris.
And a leaking boiler was located next to the clean room, which created an environment in which contaminations could have occurred.
Again, these results are preliminary and are not intended to and do not seek to conclusively identify the root cause of this outbreak.
DPH’s collaborative investigation with the FDA is comprehensive and will continue until investigators have all information needed to determine the root causes and what further action should be taken. This investigation also extends to NECC’s business practices and the environmental conditions surrounding the business, including the presence of a nearby recycling center that shares ownership with NECC. The DPH and the FDA are also actively investigating NECC’s sister companies, Ameridose and Alaunus Pharmaceuticals. As Governor Patrick described, findings from these investigations will also be used to inform needed federal actions to address regulatory gaps within the quickly evolving compounding industry.
This program aired on October 23, 2012. The audio for this program is not available.