Support WBUR
Opinion: In Simulation Era, Your Doc's First Try At A Procedure Should Not Be On You
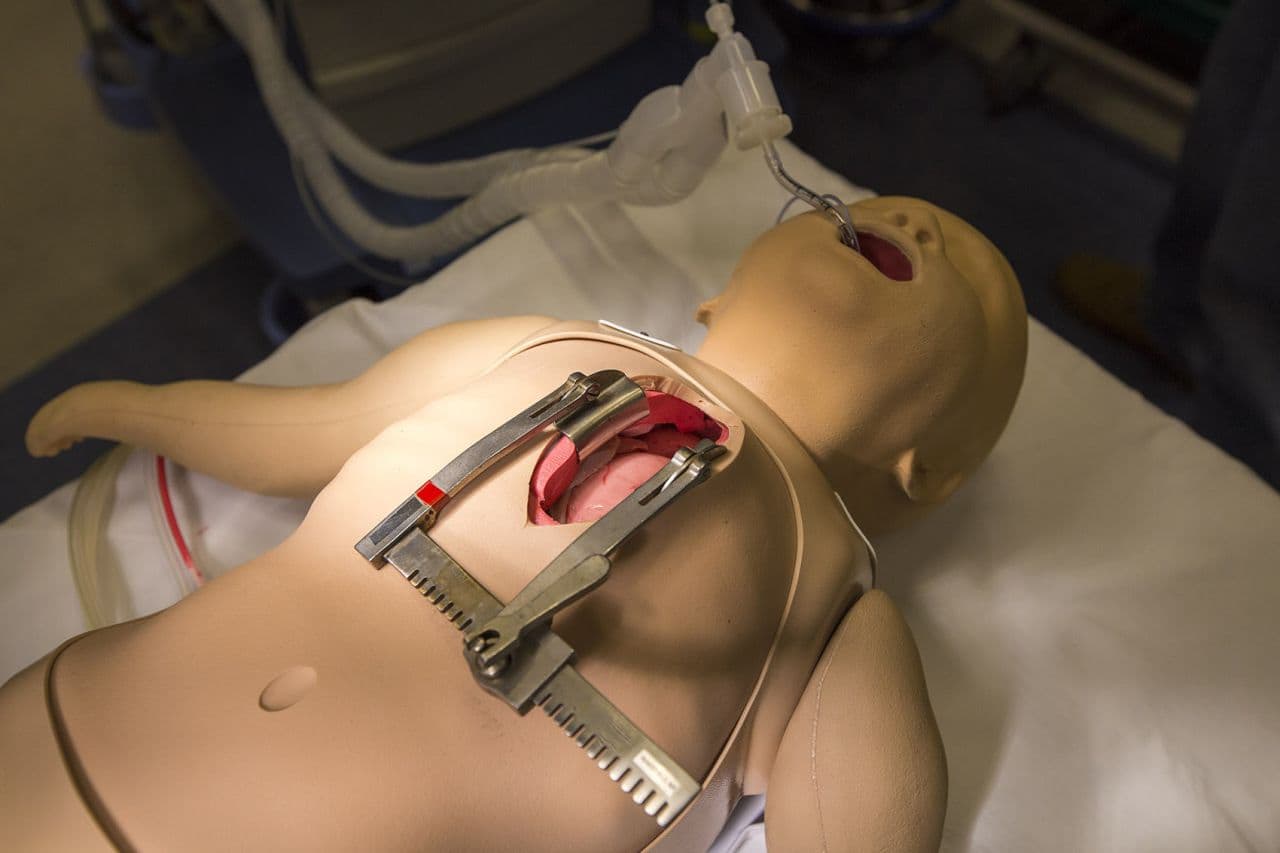
Most doctors never forget the paralyzing terror of their first invasive procedure.
Dr. Charles Pozner, of Boston's Brigham and Women’s Hospital, recalls the first time he placed a central line, which involves sticking an eight-inch-long needle into a patient's jugular vein to place an intravenous line. He had never even seen it done before, but a chief resident offered him the opportunity after a long day working together.
“When I was a medical student, the last thing you wanted to say when someone offered a procedure to you was ‘no.’ You wanted to learn, to be part of the team,” Pozner told me. The chief resident walked him through it without mishap, but “it was an unsafe thing for the patient, and an unsafe thing for me, because I was potentially harming the patient,” he said.
Twenty years later, in 2013, I went through a similar process. I watched a colleague place a central line during my first week as an intern. A couple of days later, I placed my first one, as my senior resident supervised. Thankfully, everything went fine. But that doesn’t mean I’m comfortable with the idea of wielding eight-inch-long needles after only watching someone do a procedure once.
“See one, do one, teach one” is the ancient medical adage for this: that after doctors in training have seen one procedure or operation, they’re qualified to do the next one. It has been the model for teaching physicians for generations.
But in the age of robotic surgery and simulation medicine, is this concept really acceptable anymore?
The short answer is no. Clearly, doctors in training should practice on computers and simulated patients, not real ones. Particularly when, according to a study out this week, medical errors are the No. 3 cause of death nationwide.
The longer answer is more complicated. No one openly defends the concept in medical journals — in fact, experts talk about “see one, practice many, do one.” But the "see one, do one, teach one" culture still persists in hospitals around the country, and it remains routine for physicians in training to practice their first procedure on real patients. (As a patient, what can you do about it? See the tips below.)
"Would you fly on an airplane if they say, ‘We’ll drop the price of our tickets but our pilots will opt out of flight simulation?'"
Dr. Antonio Gargiulo
But that is changing, as more hospitals and medical schools invest in high-tech simulation centers like the $12 million center unveiled by Boston Children's Hospital this week.
Dr. Pozner, who is medical director of the Brigham's STRATUS Center for Medical Simulation, says that in time, medical simulation will mean the death of "see one, do one, teach one."
The Pilot Analogy
Consider pilots. Chesley “Sully” Sullenberger, the pilot who remarkably landed his plane on the Hudson River, is often mentioned in the medical literature on simulation, as are his hundreds of hours practicing simulated emergencies. If Dr. Atul Gawande famously brought the pilot’s checklist to surgery, simulation proponents think more pilot-style simulation should be brought to medicine.
"It's called procedural memory,” Dr. Pozner said.
And studies show that simulation works in medicine. One small study trained doctors in robotic surgery, showing that they could reach expert level proficiency by the time they operated on their first real patient.
“The main advantage of this tool is you can get technically perfect before you even touch a patient,” said Dr. Antonio Gargiulo, medical director of the Center for Robotic Surgery at Brigham and Women’s Hospital.
Another landmark study found that doctors using simulation to practice common procedures led to significant reductions in infections in intensive care units.
For certain procedures, it is difficult to get hands-on training without simulation.
Dr. Gargiulo, also an assistant professor in obstetrics and gynecology, points to the example of vaginal hysterectomies — removing a woman’s uterus through the vagina rather than through her abdomen. Because of the mechanics of the procedure, it is difficult for more than one surgeon to see what is going on at any given time.
Without simulation, “the learning curve for training is steep and dangerous,” Dr. Gargiulo said.
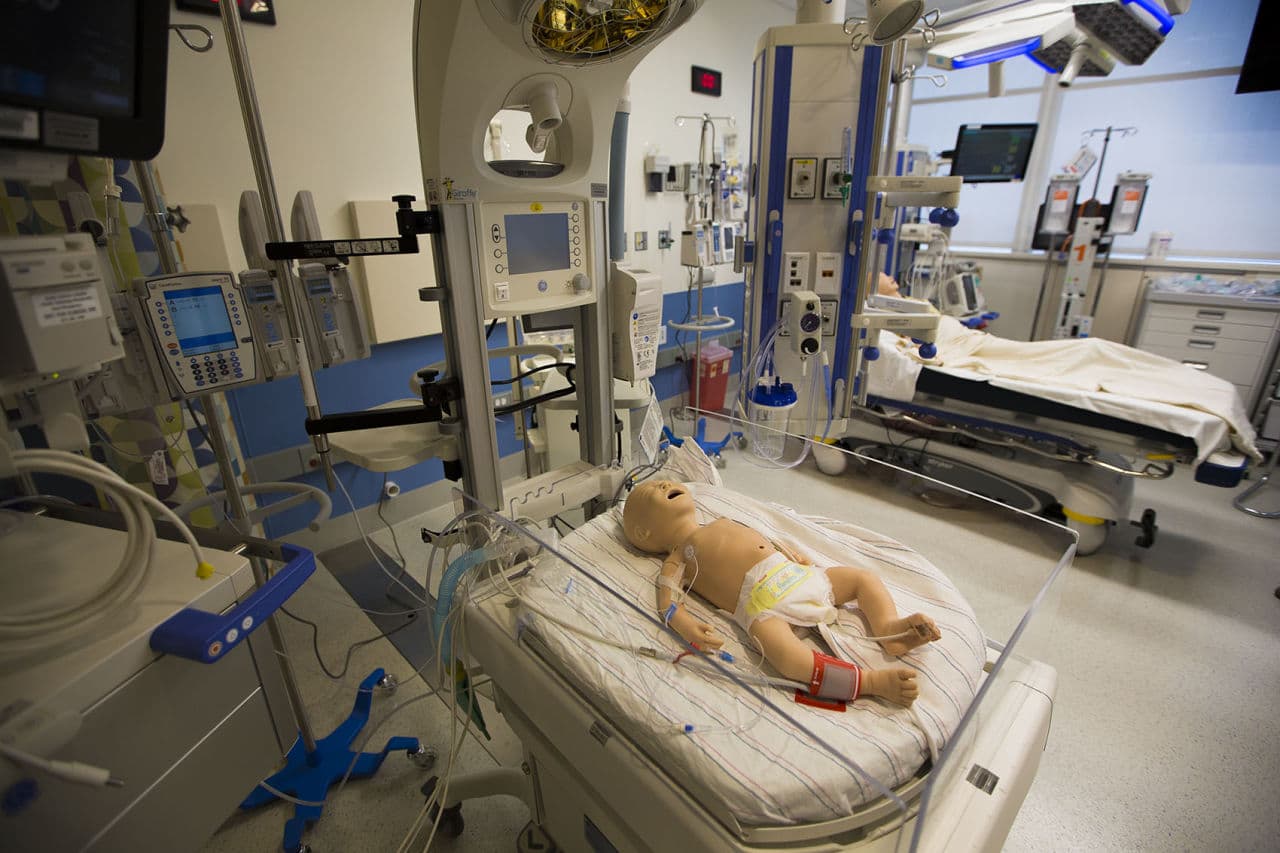
Simulation cannot universally replace experience. Procedures for ear, nose and throat doctors, as well as heart and brain surgery, do not have great simulation equivalents at this point. Plus, while it may offer a good approximation, “simulation is always imperfect,” Dr. Pozner told me.
Still, ideally, the goal is for doctors to observe procedures, then practice the skills in a simulation environment, and finally master them once we practice on patients. It’s a far cry from “see one, do one, teach one.” So why hasn’t this revolution already taken place?
Obstacle No. 1: Money
First, medical simulation is expensive, and it's the bigger, richer institutions that can best afford high-tech simulators. Nearly half of the medical schools and about a quarter of teaching hospitals with simulation centers have annual budgets greater than $500,000 for them, according to a 2011 American Association of Medical Colleges survey.
Not that cost should prevent hospitals from striving for more safety. As Dr. Gargiulo put it, “Would you fly on an airplane if they say, ‘We’ll drop the price of our tickets but our pilots will opt out of flight simulation?’ I wouldn’t fly them anymore.”
But that is the reality, though there are also cheaper, lower-tech simulations.
For my patients’ and my own sake, I wanted to be better prepared for the next central line I placed. The hospital I work in has a mannequin for practicing central lines, costing only a few thousand dollars. I practiced about 10 more times to become more familiar with the equipment and technique before I put in central line No. 2.
Cost may be the largest barrier but it’s not the only one. Simply creating a simulation center won’t compel doctors to use it, and there’s no requirement for doctors to use simulation to keep their skills up to date — unlike pilots who must do simulations to keep their licenses current.
So simulation centers are trying to become easy and convenient to use. UMass Medical School has all its simulation environments under one roof in a 24,000-square-foot facility. Doctors from various departments in the medical school can come to practice their skills.
“The biggest room in the simulation center is the room for improvement,” quipped Dr. Michele Pugnaire, the executive director of UMass’s simulation center.
Skewed Financial Incentives
Another barrier: skewed financial incentives. Hospitals should do what’s best for the patient, right? But insurance companies and Medicare used to pay the extra costs if a patient had complications from a procedure. Until recently, hospitals had little financial incentive — aside from the risk of lawsuits — to invest in minimizing complication rates from procedures, either through simulation centers or other initiatives.
That’s now changing as so-called Accountable Care Organizations are flipping financial risk, making hospitals, well, accountable for complications that might extend a patient’s stay.
Of course, hospitals aren’t trying to infect patients or cause complications — that would be a national scandal — but they don’t always have an incentive to put in place expensive measures to prevent those infections or complications, as detailed in this Vox article on central line infections.
"If you can’t do it in a simulated setting, then you probably can’t do it on a patient."
Dr. Michele Pugnaire
Accountable care organizations work differently, putting hospitals on the hook for preventable complications like certain types of infections. And these days, hospitals are investing more to help prevent complications, and it's paying off. Recently released data showed a 17 percent drop in the rate of hospital-acquired infections in four years, citing such payment reforms as one of the drivers.
Plus, some malpractice insurances are offering discounts in specialties like anesthesia and obstetrics for showing competency in certain simulated environments. These incentives push hospitals to invest in getting their physicians proficient at these procedures through simulation, and push the doctors to do these trainings.
“Not to say if you can do a procedure in a simulated environment, that you can do it in people,” Dr. Pugnaire, also a professor of family medicine at UMass, told me. ”But if you can’t do it in a simulated setting then you probably can’t do it on a patient.”
Still, there are cultural barriers to replacing the “see one, do one, teach one” mentality.
Some physicians have the mentality of: ‘I’m a good surgeon and this is how I trained,therefore this must be the right way to train,’ or, ‘That’s the way we’ve done it all along,’” said Dr. Pozner. It’s a cultural mindset that is slow to change, despite the evidence.
One final obstacle: Unlike tragedies in the airline business, which make front page news and force politicians to act, patients tend to suffer through bad outcomes from procedures in obscurity. And this silence isn’t just a tragedy for the patients. It also fails to raise awareness so patients can start demanding safer procedures.
What You Can Do
That’s where you come in. I asked Drs. Pugnaire, Pozner and Gargiulo for a few commonsense questions you can ask your doctors to make sure they’re not practicing on you.
The goal isn’t to have an antagonistic relationship with your doctor, asking accusingly, “Have you ever done this before?” As in any doctor-patient relationship, being comfortable and open with your doctor is key, and ideally, you'd feel your own honesty and openness reciprocated.
You may want to begin by asking which procedure or method of surgery has the least complications. Some phrases you might consider using are:
•“What is the current standard of care for this procedure?”
•“Are minimally invasive options available?”
•“What are your current skills in this procedure?”
•“Have you practiced this procedure recently?”
•“Are you current in this procedure?”
If the doctor says they’ve never done the procedure before, don’t panic. Listen to their other experience before deciding. And don’t forget, politely asking their help in arranging a second opinion is always acceptable.
"We will never be able to completely end having trainees caring for or performing procedures on patients during their training," Dr. Pozner said. "But patients need to know there's a buffer between the first time performing a procedure on a real patient and the first time that they ever performed the procedure."
Readers, reactions? Have you ever had the feeling you were functioning as a medical training tool?
Dr. David Scales, M.D., Ph.D. is a third year resident in internal medicine at Cambridge Health Alliance.