Support WBUR
A Face-Lift In Boston, A New Jaw In Rwanda: One Surgeon's Global Perspective
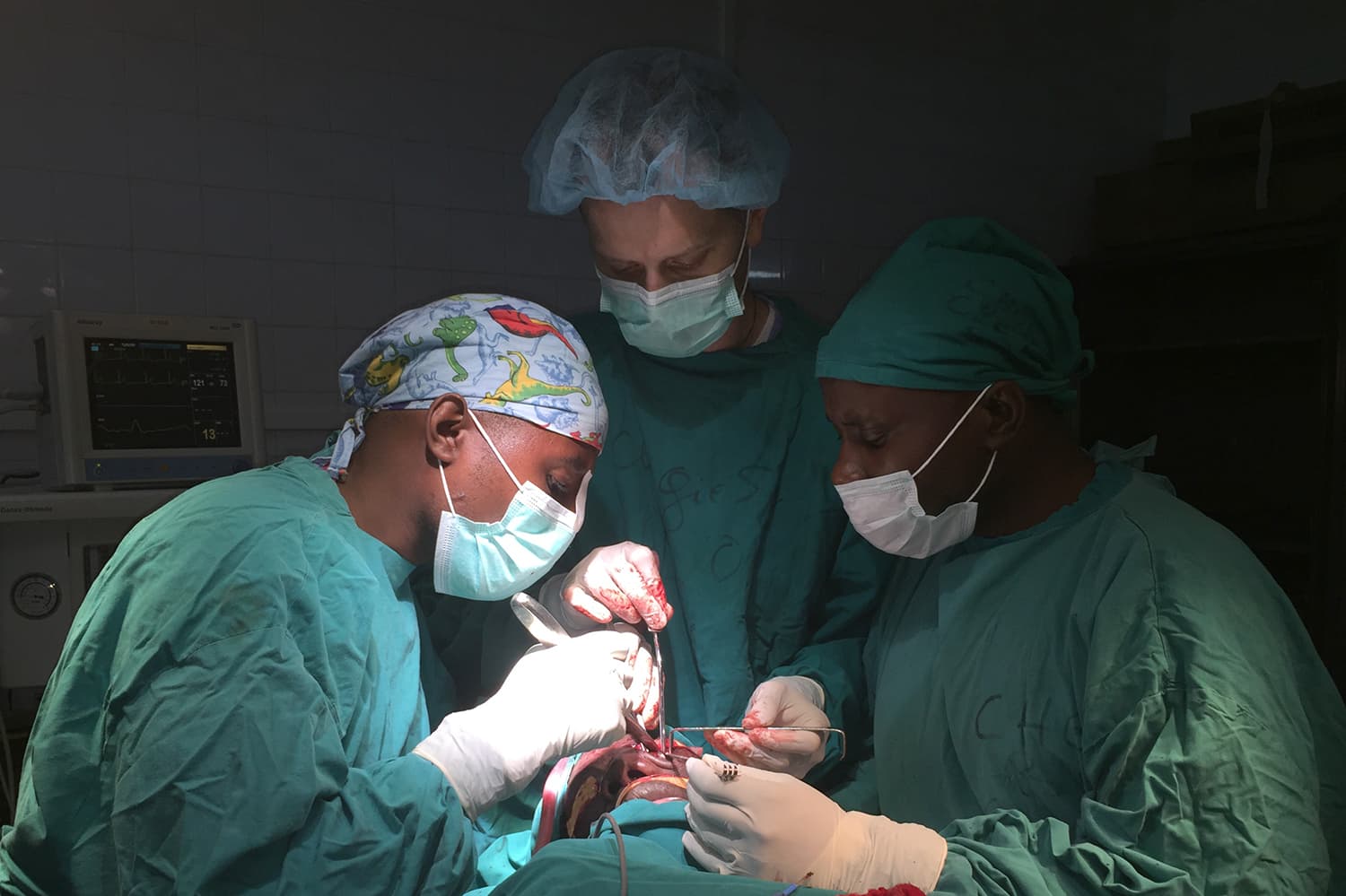
At Rwanda’s Kanombe Hospital in February, I removed a grapefruit-sized tumor from the jawbone of a 21-year-old man. Then, harvesting the non-weight-bearing fibula bone from the young man's leg, I used it to create a new jaw.
That day, after 12 hours of surgery on different patients, all with facial injuries, I received a text message from a Rwandan surgical resident about a patient at the local teaching hospital on the other side of the city of Kigali.
Agnes, a 14-year-old student, had been traveling to her first day of secondary school, catching a ride on a tractor trailer heading through the mountains of Rwanda. The truck lost its brakes and, in order to save her life, she jumped from the moving vehicle at a high speed. Sadly, everyone else in the vehicle died, and although Agnes survived, most of her face had peeled away from her skull. It had been a week since, and her injuries had yet to be treated properly. Agnes was now at the central university hospital in need of urgent attention due to an overwhelming infection.
That night, with a few instruments and by the light of a camping headlight, I worked with Rwandan residents to clear the infection and repair Agnes’ face. We picked Sorghum grains, which the truck was carrying, out of the deepest portions of her eye, and slowly, meticulously -- over the course of five hours -- we put her face back together with the suture we had.
Agnes returned to the operating room twice more over the next few months, and with time, she recovered. Had she not had surgery that night, she would have died.
One Facial Trauma Surgeon For The Whole Country
Rwanda is a country of 11 million people with just one Rwandan surgeon trained to perform facial trauma repair. This is woefully inadequate to address the burden of disease in Rwanda, and this picture is not uncommon for much of the developing world. Nearly one-third (between 28 and 32 percent) of the global burden of disease is surgical in nature. Surgery cannot continue to be neglected within the realm of global health.
At my home institution of Massachusetts Eye and Ear, I work as a facial plastic and reconstructive surgeon, where we produce five new specialists every year through a residency program of Harvard Medical School. For nine months of the year, I run a primarily cosmetic and reconstructive practice at Mass. Eye and Ear, where the most common cosmetic procedures I perform include face lifts, eyelid surgery, nose jobs and facial reconstructive procedures on both adults and children.
For the other three months of the year, I operate and teach in Africa. This began seven years ago in Zimbabwe, where I was operating on children with cleft lips and palates, and where I met my wife, Jessica, who was a volunteer journalist. Now, with our two daughters, we relocate to Rwanda temporarily each year and I operate on patients and teach surgery to Rwandans.
Facial trauma repair includes fractures of the jaw, cheekbone, orbital bones, nose and forehead — and sometimes, it involves all of the above in what is called a “pan-face fracture.” Surgery involves exposing the bones through small, hidden incisions in the mouth, around the eye, hairline or natural skin creases, and then returning the bone fragments to their original position and fixating them in the correct position.
Hammers And Chisels
While the surgical principles remain the same in Rwanda, creativity is required as many tools are lacking. In Boston I use titanium plates and screws to fixate bones, but in Rwanda I often use simple wire, as was used in the United States 50 years ago. Electricity is not always reliable and we often operate with camping headlights, using hand drills or instruments for other parts of the body. It forces ingenuity — morphing universal surgical principles with “make-do” improvisation.
To replace small dental rubber bands we cut a tubed catheter. Drills are pieced together with new battery sources from other instruments. Bones that have healed in an incorrect position are re-fractured with hammers and chisels instead of electric saws.
Facial trauma is one such problem that, if repaired in a timely fashion, can reintegrate someone back into his or her daily life in a short time. Without treatment, however, people can be left with lifelong disability, deformity or even death.
Souzana is an example. She's a 74-year-old woman who, after a fracture of her forehead bone went unrepaired one year ago, arrived at my Rwandan clinic with a golf ball-sized infection that had eaten through her forehead bone and was on the way to the brain. An extensive surgery cleared the infection, but this could have been prevented at the time.
The Rwandan surgical residents are highly motivated to learn, extremely smart and have a large backlog of very challenging patients. All they require is training. Teaching surgery to local doctors is an intervention with high leverage. The surgeries I am training Rwandan doctors to perform not only help patients like Agnes, but also help the future cases the surgeons will surely see during their lifetime.
A Machete Wound
During my recent stay in Rwanda, the Rwandan residents and I used hand fracture tools to fix 6-year-old Kelvine’s jaw, which was crushed by a cow. Out of necessity, wires were used to piece back together Thomas’ entire face, crushed in a motorcycle accident. Borrowed plates from orthopedics were used in a non-conventional way to repair Melanie’s jaw, fractured by a machete wound inflicted by her husband when he found out she was HIV positive.
My experience in Rwanda has stretched my creative thinking to solve a patient’s problem, whether that is cosmetic or reconstructive. The work in Rwanda, although all volunteer, is the highest “paying” work I have ever done, and the practice in Boston supports this unique arrangement.
Through the help of a Human Resources for Health Grant, the first fellowship to train a Rwandan in facial trauma surgery has begun. Over the next three years, the program will produce the first fellowship-trained facial trauma surgeon in Rwanda. The graduating surgeon will be in a position to train other Rwandans as well, to take care of patients like Agnes.
Agnes On The Mend
Before leaving Kigali, I stopped by to see Agnes one last time, finding her among the 50 patients crowded into the open hospital ward. Outside on the lawn, family members slept or dried their laundry in the sun and whispered “Muzungo” (foreigner) as I passed by. Agnes smiled when she saw me, and although the right side of her face has survived, it is paralyzed, so the smile is only half there. I let her know that I will be back in a year to do further surgeries on her paralyzed face. In the meantime, she promised to heal and will return to school.
My family and I made the long and familiar trip back to Logan Airport, landing on a Sunday and settling back into our Boston life. On Monday morning, I began my facial cosmetic clinic, discussing a face lift and brow lift with a patient interested in a more youthful appearance.
Later that week, I received text messages from Rwanda showing me cases performed successfully after my departure. With each message, I’m filled with pride for my colleagues there in Rwanda, who will be performing that surgery on patients for the next 30 years, and who will be teaching it for the rest of their careers. While patients and doctors come and go, the surgery will live on.
David Shaye, M.D., is a facial plastic and reconstructive surgeon at Massachusetts Eye and Ear and an instructor at Harvard Medical School.