Support WBUR
With Cancer Diagnoses, Better-Off Americans May Get Too Much Attention
It's just common sense: People who are better off get better medical care.
But when it comes to cancer screening — to find hidden malignancies when they're early and curable — a new analysis says conventional wisdom doesn't hold up.
The analysis, in the New England Journal of Medicine, challenges the intuitive notion that well-insured Americans, who are more likely to get screened regularly for cancer, have a lower risk of dying from the disease.
Dr. H. Gilbert Welch and Dr. Elliott Fisher of the Dartmouth Institute for Health Policy and Clinical Practice compared the rates of cancer diagnosis and cancer death between more and less affluent U.S. counties. Specifically, they looked at four types of cancer: melanoma and cancer of the breast, prostate and thyroid.
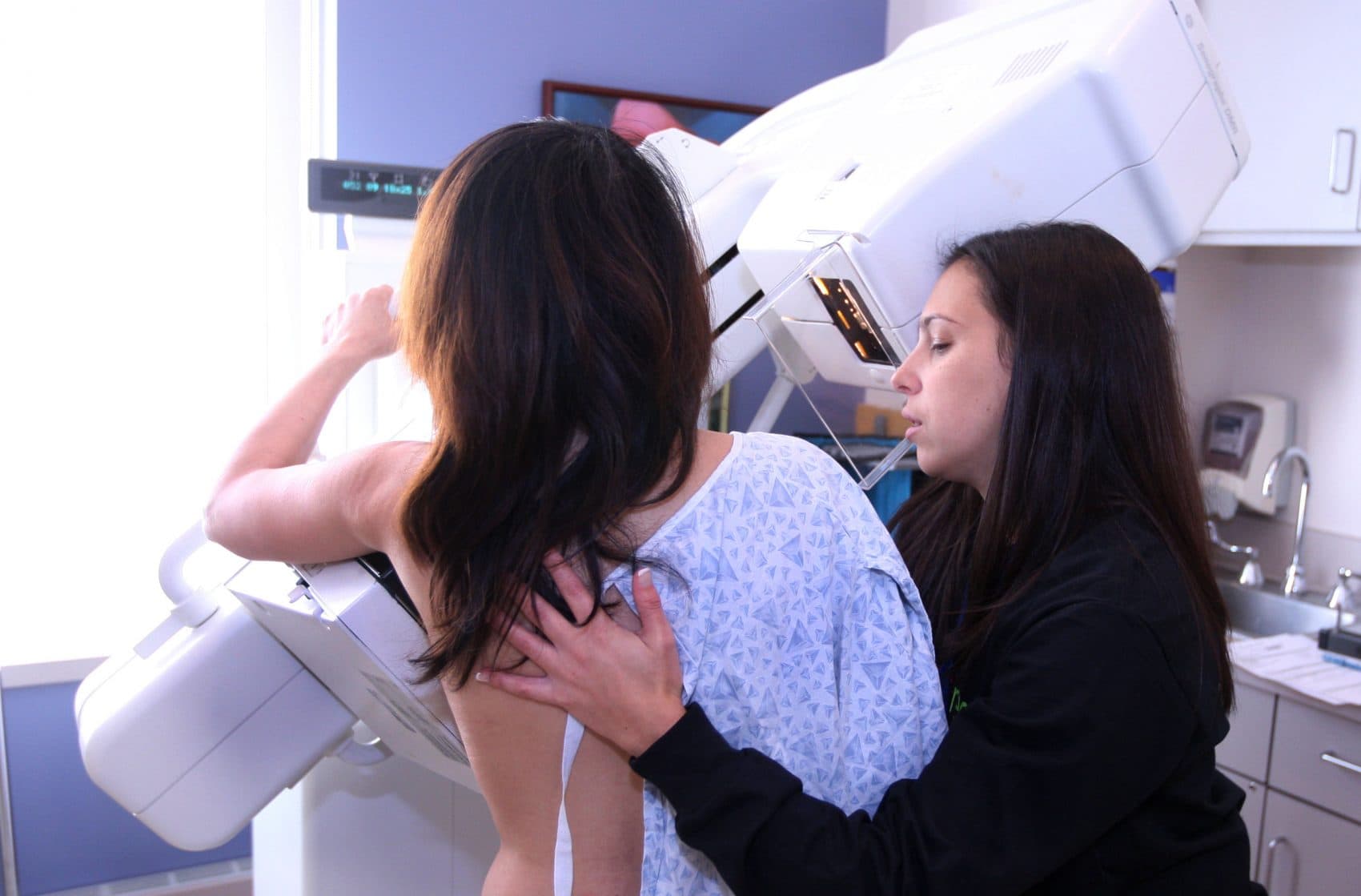
To find these cancers in apparently healthy people, doctors use mammograms for breast cancer, PSA blood tests for prostate cancer, neck exams for thyroid cancer, and regular skin exams to spot suspicious moles.
Death rates for these cancers were nearly identical over 38 years in richer and poorer counties, even though the rate of cancer diagnosis was much higher among the more affluent.
Sure enough, the Dartmouth researchers found, a lot more of these cancers are diagnosed among more affluent Americans. That undoubtedly leads to more surgery, chemotherapy, radiation and newer forms of therapy — exposing them to more treatment side effects as well as costs. But there's no strong evidence they're better off because of it.
Death rates for these cancers were nearly identical over 38 years in richer and poorer counties, even though the rate of cancer diagnosis was much higher among the more affluent.
"There are reasons to wonder whether wealthier people receive too much care," Welch and Fisher write, "whether because of their greater ability to pay for services, their expectations or demands, or more aggressive marketing by the health systems that serve them."
This is the latest of a long series of papers by the Dartmouth researchers on what they call over-utilization of medical care. I asked Welch, author of the 2016 book Less Medicine, More Health, about the new analysis. Our conversation, edited:
Why did you decide to look at how getting diagnosed with one of these cancers is influenced by patients’ income levels?
Well, I've always been interested that the frequency of cancer diagnosis is, in part, a function of how hard you look. So my colleague Dr. Fisher and I wondered whether high-income individuals would be more likely to be diagnosed with this set of four cancers simply because they're seeing doctors more often, they're being tested more often, they're being screened more often.
Why did you choose these four malignancies -- melanoma and cancers of the breast, prostate and thyroid?
These are four cancers where the rate of new cases has increased rather dramatically as we’ve stepped up our efforts to look for them. These four cancers are especially sensitive to the intensity of observation — how hard we look for them.
And what did you find?
The core finding is that high-income Americans experienced a markedly greater increase in their incidence of breast cancer, prostate cancer, thyroid cancer and melanoma [between 1975 and 2013] than low-income Americans. We believe that’s simply the result of more scrutiny. They're being looked at more carefully, so more cancers are being found.
What do you mean by “high income”?
We looked at median income at the county level as measured by the 2000 U.S. Census. The wealthier counties are those whose median income is higher than $75,000 a year in 2000 and the poorer counties are those with a median income of less than $40,000 a year.
So “high-income” in this analysis doesn’t mean wealthy?
No, we're not talking millionaires here, absolutely not. These are people who one would guess have fairly good access to care.
But I gather you didn’t find more cancer deaths as the rates of cancer diagnosis went up?
That's right. You would expect that if this increase in these cancers was real, you'd see increased mortality rates. But in fact, mortality rates are not going up. Instead, they're going down. That largely reflects improved treatments for breast and prostate cancer, which in turn reflects our recognition that many of these cancers are hormonally influenced and can be helped with hormonal therapy and chemotherapy.
And was there any difference in death rates for these four cancers between low- and high-income patients?
No, they're declining in both high- and low-income counties, but somewhat slower in low-income counties. That probably does represent less access to these new treatments [among lower-income people]. That would be our best guess.
By the way, I’m surprised you included melanoma. With the other three, there’s been a lot of debate about whether some cases don’t require treatment. But I thought melanoma is one malignancy that’s always important to catch as early as possible.
Well I think that mantra — that it's always good to catch it early -- has existed for all four cancers, and yet all four of them have experienced rather dramatic swings in their incidence rate based on how hard we look for them. Melanoma is simply another cancer that is sensitive to how often people are going to physicians and how often physicians biopsy skin lesions. I think it's pretty similar to the other three.
So what do you make of these findings?
I think the story’s probably a little different for each of the four cancers. But the commonality is that all of these cancers are subject to the problem of over-diagnosis — that is, the detection of abnormalities that meet the pathologic definition of cancer yet are never destined to bother the patient.
"The conventional wisdom that early detection is always better is not correct."
Dr. H. Gilbert Welch
Many people have trouble with that concept -- that there are many cancers that don’t need to be found and treated, because they won’t grow, or grow so slowly that people will die of something else first. We’ve always been told that it’s always better to find cancer as early as possible. You’re saying that’s not entirely right.
The conventional wisdom that early detection is always better is not correct. And the reason it’s not correct is because whenever we look early we find a lot more cancer than we otherwise expect. So the question is: To what extent should we be looking hard for earlier cancers? If there's one message I could get out, it’s that the best test is not the test that finds the most cancer. That is a recipe for over-diagnosis.
I want to be clear that patients with symptoms who notice a new lump or see a concerning skin lesion should be evaluated by their physician. But the larger question is to what extent people who have no idea that anything is wrong should be looked at incredibly carefully to see if in fact we can find something wrong. So the question is how early to find things. And I'm afraid our drive towards earlier and earlier is leading us to find more and more cancer and treat more and more patients, many of whom don't need to be treated.
Is this true for all cancers, or just the four you think are most likely to be over-diagnosed?
I wouldn’t say other cancers are free of the over-diagnosis problem, it’s just much less common. It’s important for people to know that there's a lot of heterogeneity within cancer in general, whatever organ we're talking about.
It’s been described as the barnyard pen of cancers. There are three animals in the barnyard — the birds, the rabbits and the turtles. And the goal of early detection is to fence these animals in, to catch them early. But you cannot fence in a bird, the bird’s already flown away. And these represent the most aggressive cancers, the fastest-growing cancers, the cancers that have already spread by the time they're detectable.
The rabbits are hopping around and you can catch them if you build enough fences. These represent the more slowly progressive cancers that are potentially helped by early detection.
And then there are the turtles. And you don't need any fences because these are the cancers that aren't going anywhere anyway. These represent abnormalities that meet the pathologic criteria for cancer but do not progress. And the reality is there are just a lot of turtles in thyroid, breast, prostate and melanoma
So if doctors can't yet tell which cancers are birds, rabbits or turtles, more screening and diagnostic testing is not better?
Yeah, you can't test yourself to good health. And in fact it may distract from more important determinants of health — things like good food, regular exercise and finding purpose in life. I think we sort of oversold this idea that you need to come to your physician to be thoroughly investigated to determine whether you're well or not. It actually can be the fastest way to be turned into a patient.
But what’s the “right” amount of cancer screening? What’s the Goldilocks solution, and how is the ordinary patient supposed to find it?
I think there's a growing recognition that the conventional concern about too little medical care needs to be balanced with a concern about too much. Excessive testing can produce real harm. It can lead to treatments that cannot help patients but nonetheless can result in things like medication side effects, surgical complications and occasionally even death.
A lot of physicians totally get this problem, but they're hesitant to raise it to a patient because it is so counter-intuitive. I think just acknowledging that you understand there are tradeoffs here may lead to a much more balanced conversation with your provider.
Your previous studies and statements about over-diagnosis have not always been welcomed by your medical colleagues. Is the argument tipping more your way?
I think the debate is shifting. When I started, the debate was, did over-diagnosis exist or is it a figment of some researchers’ imagination? Now, the debate is, how common is it and is it a problem we ought to deal with?
But there are a lot of forces driving “more is better.” There’s a lot of money on the table. For medical centers [cancer screening] is a great way to produce new patients to treat. So there are very strong forces that tend to promote more testing.
There’s another paper in this week’s New England Journal of Medicine that suggests ways doctors might eventually identify which small breast tumors they have to worry about and treat aggressively, and which they can safely monitor without immediate treatment.
It is a great paper because it provides a sort of biologic mechanism for over-diagnosis. What it’s showing is that small breast cancers tend to have fundamentally different biologic characteristics. They tend to be more indolent. We're beginning to see that in fact the biology of those cancers is different.
There are two questions I want to separate out. One is the question of how hard to look. The second question is once you find something, what you do about it.
The one thing that the over-diagnosis debate has done for the treatment community is: It has made the option of active surveillance — of simply watching things — a more legitimate option.
This segment aired on June 9, 2017.