Support WBUR
Harsh Reception For Supervised Drug Injection In Boston
If the first public hearing is any indication, Boston supporters of rooms where drug users would inject under medical supervision have a long road ahead of them.
Passions ran high before the hearing on bringing supervised injection facilities, or SIFs, to Boston even began Monday.

A redhead named Whitney, standing outside the Boston City Council chambers, described a crushing spinal injury that introduced her to morphine 30 years ago. Now, with fentanyl in most bags sold on the street, Whitney says she’s overdosed 11 times since January. If Boston had a supervised injection facility, Whitney says she’d use it.
"It’s horrible, I don’t want to die, but I’m in pain," said Whitney, her voice shaking. "So I have to go into a port-a-potty and shoot up 'cause I have nowhere safe to go, and I overdose? It’s so sad, it’s not right."
Inside the chamber, a panel of supporters urged council members to back opening a SIF in Boston.
"SIFs save lives," said Dr. Gabriel Wishik, an addiction specialist at the Boston Health Care for the Homeless Program. "We desperately need this option in Boston."
Wishik ticked off a list of reasons:
- SIFs reduce overdose deaths. Wishik cited a study that found deaths decreased 35 percent in Vancouver within 500 meters of a SIF there as compared to 9 percent in the city as a whole. No one has died inside the Vancouver clinic. (Critics say the 35 percent analysis is flawed because it doesn't include all relevant deaths. The study authors defend their methodology here.)
- SIFs increase referrals to treatment. Insite, the Vancouver clinic, says clients are 30 percent more likely to engage in treatment than are drug users outside the SIF. (But data for 2015 shows a much lower rate, and SIF opponents point out that few Insite clients complete treatment.)
- SIFs do not encourage drug use.
- SIFs have a neutral, if not positive, impact, on the surrounding community.
- Drug users want access to SIFs.
Boston City Councilor Frank Baker, one of two councilors who called the hearing, listened to four other doctors and public health specialists outline the benefits of SIFs.
"I’m still not convinced by your testimony, like not even close, that it will be helpful," Baker said, mentioning the low rates of referral to treatment in 2015. If the city did allow SIFs, Baker said, there should be a limit on the number of days — perhaps between three and seven — for each drug user. After that, they'd have to go into detox.
"I think it might be the wrong path to make it easier for users," he said. "It’s almost like, it should be more difficult to use."
Doctors on the panel said the cap might not make sense because addiction is a chronic disease.
Aubri Esters, an active drug user, broke into the debate. Esters says she spends hours every day in the section of Baker’s district known as "Methadone Mile."
"It’s already an injection facility," Esters said. "People are already injecting publicly all over the place. We all know that. It’s just not supervised. There’s no one making sure folks aren’t dying."
Councilor Michael Flaherty said he's disturbed by the idea of doctors or nurses supervising illegal drug use.
"So we’re going to watch them inject, snort or whatever?" Flaherty asked. "And then we’re going to sit by and wait to see whether we have to jump in and render assistance? I think that is absolutely asinine."
"It’s already an injection facility. People are already injecting publicly all over the place. We all know that. It’s just not supervised."
Aubri Esters
Flaherty says what the state needs is more treatment on demand. He says supervised injection rooms send the message to children and young adults that opioid use is a normal part of medical care.
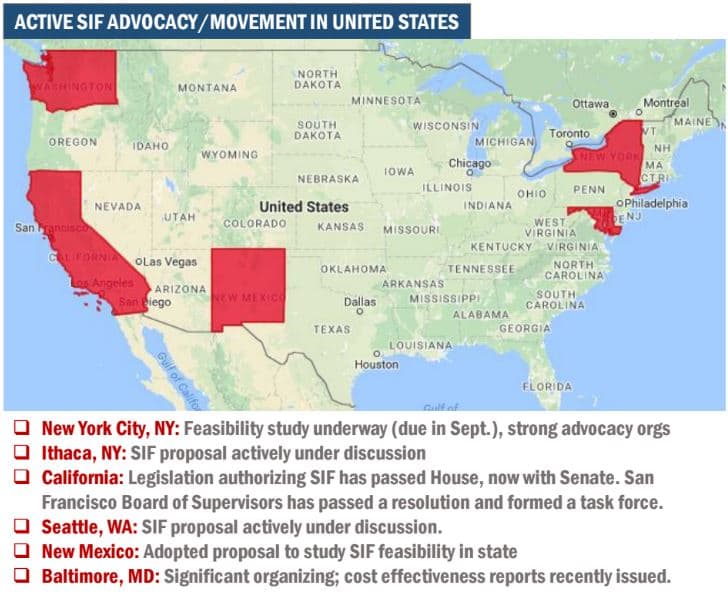
There are no SIFs in the U.S., but interest is growing.
Massachusetts Medical Society (MMS) issued a report in April that endorsed SIF pilots. But doctors were criticized several times during the city council hearing for taking that position.
"The Massachusetts Medical Society should be ashamed of themselves," said Sue Sullivan, executive director of the Newmarket Business Association, whose 235 members say they are overrun by drug use near the South Bay shopping center. The medical society "should be ashamed of themselves because we have the best minds in the world here, and this is the best they can come up with? You’ve got to be kidding."
MMS President Dr. Henry Dorkin responded to Sullivan’s comments after the hearing.
"I don’t think doctors are ashamed of themselves for savings lives," Dorkin said, "and I don’t think doctors would be ashamed of themselves for taking a look at all possible options in order to save lives."
The MMS backs creation of a statewide task force that would review the evidence on supervised injection facilities. It would conduct a Massachusetts version of cost studies that have found SIFs save money with fewer deaths and less transmission of HIV and Hepatitis C. The state Senate has approved launch of the task force; the House has not.
This segment aired on June 20, 2017.
