Support WBUR
Commentary
Medical Ethics: In The Charlie Gard Case, Listen To The Nurses
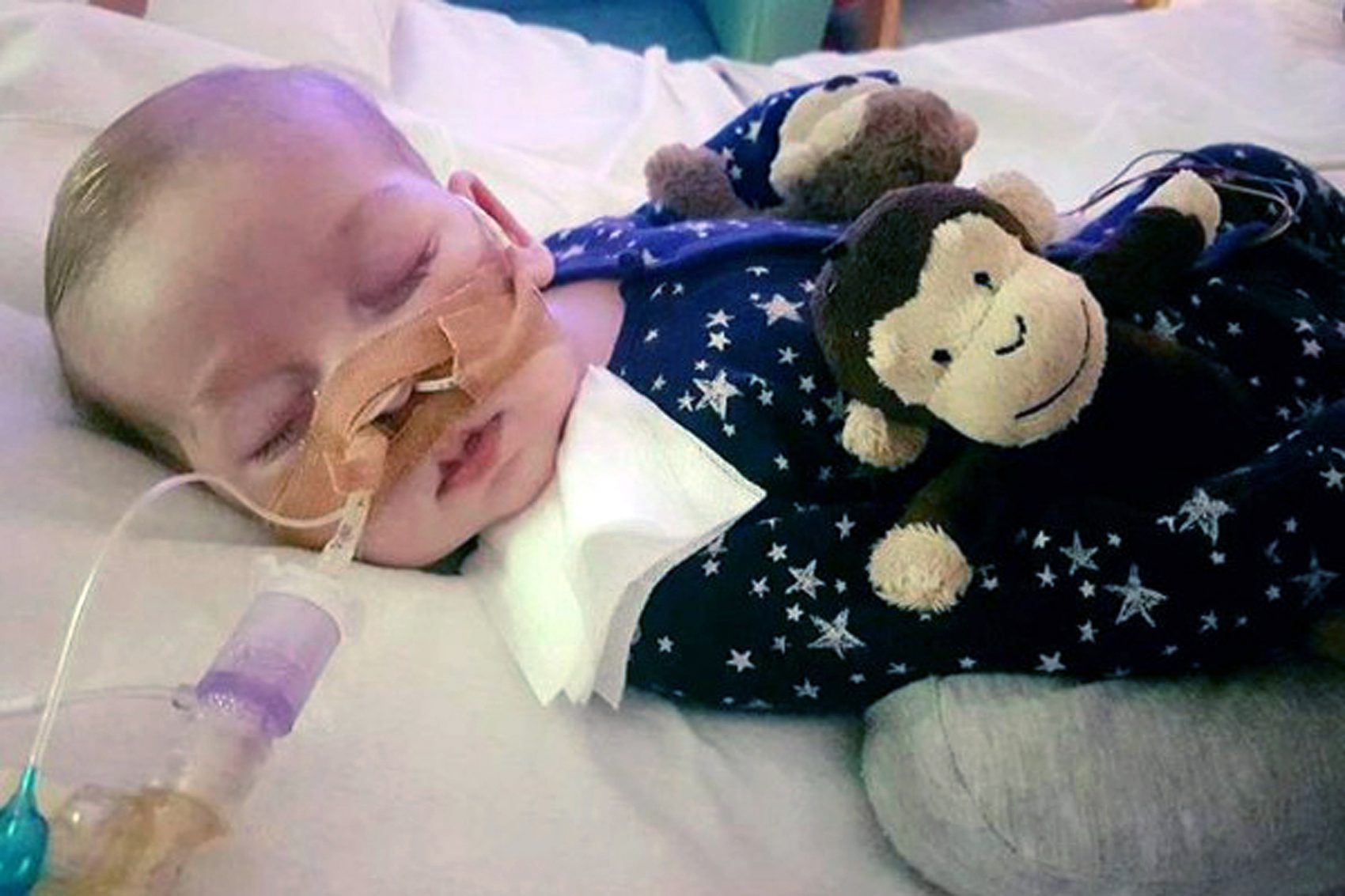
Updated 7/29 with Charlie Gard's death.
The tragic spectacle of the legal battle over Charlie Gard, the 11-month-old British baby whose genetic disease inflicted catastrophic and irreversible brain damage, has drawn to a close. Charlie's parents, told that a possible experimental treatment in the U.S. is no longer an option, stopped fighting his hospital's move to withdraw life support, and he has died in hospice care.
Still, so many aspects of the Charlie Gard case continue to trouble me. The American neurologist’s almost meaningless assessment of the chances that an experimental treatment might help Charlie. Profiteering in the guise of medical heroism — the neurologist's reported stake in the treatment he proposed. The very idea that treatments ought to be based on what patients can afford. The blurring of patient and research subject, in that the treatment proposed for Charlie lacks basic scientific evidence.
And meanwhile, the ongoing attempt to take Medicaid from American kids who aren’t Charlie Gard.
But perhaps most troubling of all for me is the abuse of the nurses and other medical staff caring for Charlie, who lived nearly his all his days on life support and mechanical ventilation.
Every day, they balanced benefit, harm and Charlie’s best interest in a very real, literally hands-on way. What they got in return: hostile messages and even death threats.
I admit to this bias: The life of my friend’s son was counted in months. Call him Nick. Everything was done to save him, and nothing was enough. Desperate interventions went on too long, and years later, my friend’s loss carries the additional burden of a retrospective awareness that Nick’s continued suffering was a parental choice with the best intentions — but not in his best interests.
After his death, my friend also learned this: Nurses had “opted out” of his care. One nurse stuck with them right to the end, then quit.
The pope, President Trump and the bioethicists who came out in opposition to letting Charlie die against his parents' wishes had never been at his bedside in the pediatric intensive care ward of Great Ormond Street Hospital. None of them has a firsthand perception of his suffering, or lack of it. They haven’t changed his dressing, suctioned his airway, searched for signs of pain, joy… any sign of human experience, really. None work on an ICU where needy new patients are turned away because no bed is available.
Months ago, medical staff determined that further interventions on Charlie were doing more harm than good. To a nurse, what does that mean? Repeatedly performing interventions on a child with no apparent benefit, and possible harm, is disheartening.
“I don’t believe you can measure another’s suffering,’’ a longtime pediatric ICU nurse told me in a recent email. “I’m not sure I even know what true suffering looks like because it’s different for each person. And then there are the beholders, who have a different idea about what suffering is. The problem is that nurses are taught, and it’s drilled into us (since Florence Nightingale), that our main goal is to relieve suffering, not cause it or participate or propagate or augment it.”
There are multiple “Charlie Gards” on her ward right now, she said — not with the same diagnosis, but with irreversible brain damage, little or no chance of sustained improvement, and an impossible choice ahead.
One of Charlie’s bedside nurses testified in the initial court hearing to determine whether the hospital could remove him from life support against his parents’ wishes.
As quoted by the judge:
Ms H …. described how, since December 2016, she has spent over two hundred hours in Charlie’s bed space often with his parents present. She said that she has not seen evidence of Charlie responding to his parents. She had not seen him grasp his mother’s fingers nor had she seen him touch or grasp (Ms H’s) fingers. She said that it was impossible to tell if Charlie is awake or asleep. She said that is is impossible to know whether Charlie suffers pain, pleasure or comfort.
Doctors, parents and occasionally judges get to make decisions about care of a child. But the consequences of those decisions are directly, and literally, felt by patients and nurses.
Charlie’s ongoing care was said not to be a resource issue. But I think a precious resource is at stake: nurses. A disheartened nursing staff is a serious problem for all of us. And as new treatments and potential cures emerge, parental decisions about when to allow life to end will only increase.
“That very spot,” the pediatric ICU nurse said in her email to me, “is where nurses now have the most moral distress.”
A most essential kind of patient advocacy is at stake. The chairman of Great Ormond Street Hospital, Mary MacLeod, said in a statement that the staff has been subjected to shocking hostility and death threats. "Thousands of abusive messages have been sent to doctors and nurses whose life's work is to care for sick children," MacLeod said.
That team ultimately met with Charlie’s parents, to determine how and when life support would be withdrawn, all in agreement that this was now in his best interest.
The essential argument of those who backed Charlie Gard's parents is this: In assessing Charlie’s best interests, life is better than death, unless and until the parents say enough. Ethically or morally, there may be no tougher argument to counter.
But in the discussions of Charlie's life, I would accord special consideration to the people who see it up close, who physically sustain it: his nurses. And to the senders of those hostile messages and their supporters on social media, I'd say: If you haven’t changed Charlie Gard’s dressing or taken his pulse, if you were at a safe distance, perhaps the best thing to do would have been to leave the doctors and nurses of Great Ormond Street Hospital alone.
