Support WBUR
Why Patients May Be Put In Charge Of Their Own Post-Operative Care
A surgical staple remover looks a bit like a handheld hole punch. Not the alligator-mouth contraption used for paper staples.
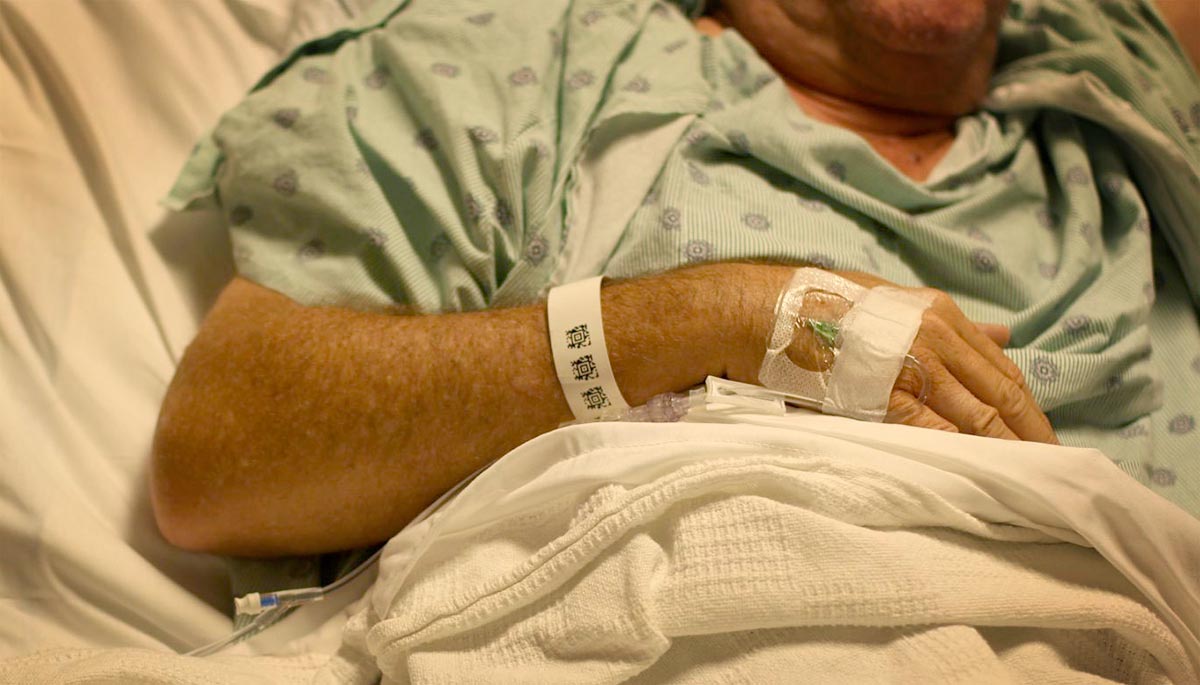
I know this because my father recently had a radical prostatectomy to treat early-stage prostate cancer. Less than 36 hours after his surgery, he was sent home with instructions on how to remove his Foley catheter, and a shrink-wrapped metal contraption to remove his own surgical staples.
This seemed risky to me.
My dad is the type of guy who leaves the instructions in the box, so I was a bit nervous that he might have told his surgical team that he had removed his own staples a bunch of times.
“Are you sure he can just take those things out on his own?” I asked his surgeon.
“Sure,” he said. “Even I can do it.”
Hardy har har.
Johns Hopkins’ James Buchanan Brady Urological Institute is the third-highest-ranked prostate cancer treatment center in the nation, according to U.S. News and World Report, and my father’s surgeon recently won the Huggins Medal for lifetime achievement from the Society of Urologic Oncology. So, the treatment was top notch. Why, then, was my dad put in charge of removing medical equipment from inside his own body?
It turns out my father is on the leading edge of a growing trend for routine surgical patients with no complications and no other complex medical problems: Get out and stay out.
There are multiple reasons, as it turns out. First, and probably most important, it’s cleaner. Anytime you enter a medical care setting you risk picking up an infection. Hospitals, in particular, are lousy with them. The latest CDC-compiled statistics, for 2011, recorded an estimated 722,000 hospital-acquired infections that year, 75,000 of which resulted in death. A reduction in the amount of time spent in a doctor’s office or a hospital reduces exposure to nasty bugs.
Also, it’s cheaper. Another visit to the surgeon to have things removed means another co-pay, another bill to the insurance company and another 15 minutes of a surgeon’s time (surgeons make around $110 an hour). If the wound has healed without infection and the catheter insertion site is pain-free, you can buy a 10cc syringe and a surgical staple remover at Walmart for under $20.
Nowhere, however, in the typed out discharge instruction packet that my father received, did it explicitly say that he should take out his own staples. The catheter removal process was outlined, and he was reminded that he could visit his local general physician if he didn’t feel up to it. His surgeon told him he could safely remove his own staples. His nurses told him he could do it. But the language concerning the staples simply said, “If you know a physician or nurse near your home you can take a staple remover home with you and have them remove the staples on the same day as catheter removal.”
Who decided that my dad could be a proxy physician?
So who decided that my dad could be a proxy physician? I asked Dr. Elliott Haut, vice chair of quality, safety & service in the Department of Surgery at Johns Hopkins, if there was a protocol in place for choosing which patients can take out their own staples. The answer was no.
“A lot of the hospital protocols really only cover the inpatient hospital stay,” he said, in a recent phone interview. “Once patients leave the hospital, there are a lot fewer hard and fast rules and protocols that need to be followed.”
Making health care rules and regulations is a tricky business. A hospital-wide protocol must be backed up with high-quality, evidence-based data, which, Haut says, is hard to come by.
"There’s not a lot in medicine that is 100 percent cut and dry for what you should do in a certain situation,” Haut said. “You can do A or B or C, and all are equally reasonable options."
The science just isn’t there. “Standardization makes life easier,” Haut said, “but it’s hard to push for standardization if there’s not proof that one way is better than the other.”
The lack of evidence-based research isn’t limited to one hospital or even one city. I asked the CDC for their guidelines on post-operative care, to which their statistical arm, the National Center for Health Statistics, replied, “we have no information on guidelines for post-operative care.” They also couldn’t provide reliable data on the percentage of ambulatory (same-day) surgeries compared to inpatient procedures.
Haut says it would be great to gather more data on post-operative care in and out of the hospital, but surgeons don’t have the resources.
“We would love to have more time and energy for research, but right now the push in medicine is clinical work,” Haut said. “The No. 1 priority is to get patients through the door.”
When it comes to postoperative care, large teaching hospitals like Johns Hopkins rely on their surgeons and, Haut says, the multitudes of people on the surgical teams to make assessments as to a patient’s ability to follow instructions. Many of those people are nurses.
“Nurses collect data all the time,” said Charlene Berube, chair of the Undergraduate Nursing Program at Simmons School of Nursing and Health Sciences. “We have an extraordinary ability to gather data, process data, and use data very quickly.”
It was probably the nurses, Berube says, who were evaluating my father’s ability to take care of himself. A pre-surgical appointment involves several forms that are meant to provide a baseline picture of a patient’s abilities. They ask about mobility, medical history and support networks at home. Recovery nurses will often re-ask these questions after surgery.
“I ask the questions directly,” Berube said, in a recent phone interview. “When I ask a patient a question directly, I get intonation, facial expression, pause in thinking. [Nurses] know the prompts to get their story.”
In general, recovery times for surgery have dropped due to advances in anesthetics and pain medications. Berube says nurses no longer have the luxury of time to coach patients with difficulties caring for themselves. They have to make determinations quickly. “We look at cognitive ability, physical activity,” she said. “We sure as heck aren’t going to let them go home until they demonstrate.”
When my father was receiving his discharge tutorial, his nurse carefully explained that she needed to see him empty his catheter bag on his own.
“I’m sure she will be doing it most of the time,” she said, smiling at my mother. “But, just in case…” At the time, it seemed routine, but after talking with Berube, I now know she was collecting data, watching for tremors, problems with motor control, or wincing during movement.
“We process [data] so quickly, it tends to look and feel like intuition,” Berube said. “It isn’t.”
In the future, that data collection could continue, even from the home. John Semple, professor of surgery at the University of Toronto, and a team of surgeons recently tested the efficacy of a mobile app to monitor patients after ambulatory surgeries.
Semple and two other surgeons used an experimental app to monitor symptoms such as nausea, pain control and anxiety. Patients were also asked to take pictures of incision and surgical drain sites.
“We were looking for post-op infections at around five or six days, which is the most common time you would see them,” he said, in a recent phone interview. “We had a couple scenarios where we were able to intervene on what we thought was a developing infection, without having a disaster develop.”
This type of post-surgery data is just starting to be collected. “I think, even 10 to 15 years ago, once you were discharged from the hospital after surgery, nobody really cared what happened to you or where you went,” Semple said. “But now, everybody is very keen on knowing exactly how you’re doing and what the rates of post-op infections are.”
That might be less of a desire, and more of a requirement.
In 2013, in response to a rise in hospital-acquired infections, the U.S. Office of Disease Prevention and Health Promotion issued a National Action Plan to Prevent Health Care-Associated Infections. The plan, along with a section in the Affordable Care Act blocking Medicaid payments for provider-preventable infections, means hospitals lose money if they don't monitor their post-op patients effectively.
Semple says these types of technological advances not only help gather data, but also free up time for surgeons to concentrate on challenging cases.
“Health care is looking at the entire population of patients undergoing certain types of surgery and saying 30 to 40 percent of these patients can go straight home and follow their own instructions so we can focus resources on that 10 percent that really requires it,” he said.
So, my dad was part of the ‘get out and stay out’ cohort. The nurses trusted him to go straight home and follow instructions. I trusted my mother to remind him that staying hydrated involves water, not Fanta.
And nine days after his surgery, they sat together in their familiar bathroom, drained 15 cc’s of saline from his Foley catheter balloon, slid out the tube, and removed 16 surgical staples with what looked like a handheld hole-punch. Case closed.
Alicair Peltonen is a freelance journalist in Boston and part-time administrative assistant at the Harvard School of Public Health. She can be reached on Twitter @AlicairP.