Support WBUR
Commentary
Dental Sedation Kills 4-Year-Old Who Might Have Been Saved By A Toothbrush
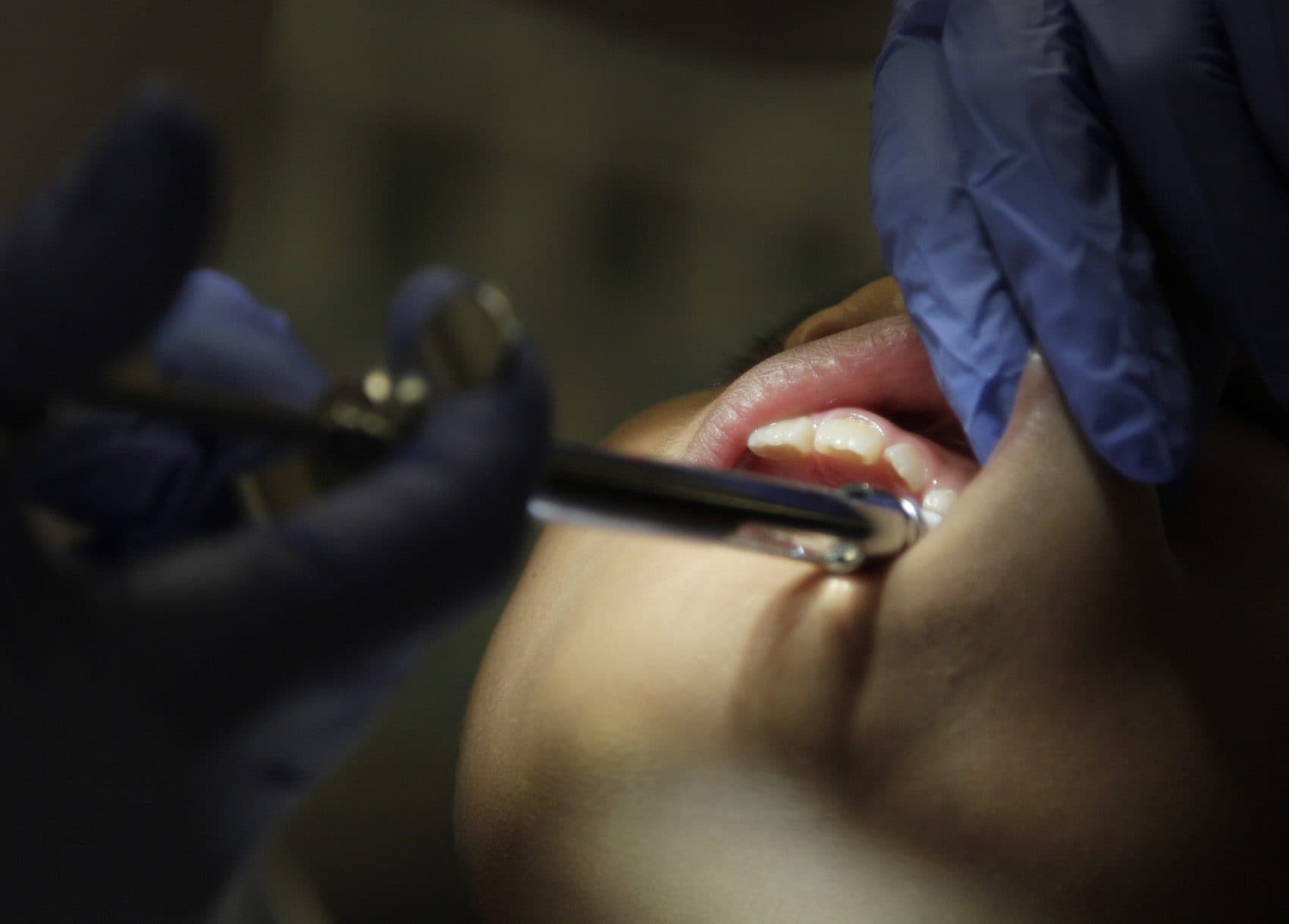
The 4-year-old boy died at the dentist’s office.
He had been brought in for treatment of the painful decay of his front teeth. Because he had “behavioral issues,” and the surgery would be painful, the dentist gave him a sedative, Versed, and nitrous oxide. When he still couldn’t tolerate the surgery, he was given more Versed.
The procedure done, the dentist left the child in recovery with a dental assistant. When he returned with the boy's mother, the child was turning blue from lack of oxygen. Rescue efforts failed, and the boy was dead upon arrival at the hospital.
This case is described in broad outline this week in the journal Pediatrics, under a headline that asks a question: “Death after pediatric dental anesthesia. An avoidable tragedy?”
The answer is a resounding yes. The authors couldn’t be more clear: “Children should never, ever die during sedation for a dental procedure.”
But this isn’t an isolated case, although there is no tracking to give us specific numbers.
Experts specifically recommend against surgery for childhood tooth decay, but it is often performed anyway. And extensive baby-teeth cavities demanding intervention, known medically as "early childhood caries" or ECC, are the most common chronic childhood disease in the United States.
But here’s the topper: Though the disease is easily prevented by basic dental care, half of American children never see a dentist.
So from an ethical point of view, this isn’t just a problem of anesthesia in the wrong hands and the wrong setting; it’s a failure of social concern for children.
It should come as no surprise that money has a part to play in the sad story of early childhood caries. So does managed care, and dentistry’s second-class citizenship in American health care.
The American Academy of Pediatric Dentistry calls caries an epidemic and emphasizes prevention when possible, and nonsurgical interventions to stop the decay. They include painting teeth with silver diamine fluoride, a safe and painless drug available since 2015 that can stop the decay, the Pediatrics article notes.
In spite of this, the pediatric dentist performed surgery in this case — and in a dental office, not a hospital operating room.
Money may have played a role. “Some insurance companies now will not pre-approve operating room [treatment] unless there has been a failed attempt in the dental chair,” says Dr. Marc Ackerman, director of orthodontics and a fellow member of the ethics advisory committee at Boston Children’s Hospital.
The insurer is essentially saying, "First do harm.” This either compromises a dentist’s ability to serve a child’s best interests, or makes the dentist somehow game the system to get the patient into an OR.
Around the country, sedating a child for dental work happens up to 250,000 times a year, often with opioids, but even other medications can cause serious problems including death, the Pediatrics paper notes.
Conscious sedation in a pediatric dentist’s office is most common on the West Coast, Ackerman says, and much less common in the Northeast than in other areas.
Surgery and deep sedation used to be considered worth the risk when tooth decay in childhood was thought to cause subsequent decay in permanent teeth. But that was “vastly overstated,” according to the Pediatrics authors.
The article describes the boy's case as a failure to ensure quality and safety, and to minimize risk in choosing a treatment. Treating caries shouldn’t require surgery. At Boston Children’s, Dr. Man Wai Ng developed an early childhood caries protocol that is becoming the standard of care nationally, according to Ackerman. It includes more frequent office visits to reinforce oral hygiene and diet, while prescribing application of topical fluoride at home to arrest decay.
Even better is preventing caries in the first place. The broader indictment from this tragic case in Pediatrics is that it represents “a societal failure to develop programs to prevent that disease,” the authors write.
Yet, according to the pediatric dental academy, half of American children have never been to the dentist. Dental care is commonly seen as less important than medical care — note its absence from health insurance policies — and that is especially true for people on the tough side of U.S. health care disparities.
American health care is a ZIP Code lottery. Maybe it always was, but it’s backsliding now — with Congress letting both the Children’s Health Insurance Program and federal funding for community health lapse in September.
And make no mistake: Dental health is health. Tooth decay in children can affect speech, sleep, learning, relationships and quality of life right into adulthood.
The 4-year-old boy who died wasn’t otherwise identified in the Pediatrics article, which feels incomplete without his mother's perspective. And yet the chances are good that he was a child of color. Hispanics are especially hard hit by early childhood caries, though the disease seems to practice equal opportunity in low-income families.
Which is to say that early childhood caries is an infectious disease caused by poor health practices in the home, and by social neglect. A toothbrush and floss should not be symbols of privilege.
The solution? More serious attention to social determinants of health, including dental health. In ethical terms, this is an issue of fairness and justice.
But justice is just one of the foundational principles of ethics that have been butchered in this perfect storm of ethical blindness. A dentist who was apparently ignorant of professional guidelines could not get true informed consent from the mother. The likely benefit to the patient, given the other options and the overstated effects on adult teeth, falls down as an argument. And the potential for harm should have been as obvious that day as it is in retrospect.
Ultimately, the specialists who wrote this piece were aiming at their professional colleagues, to spread word of the standard of care. But it holds a broader message for all of us.
Real health equity would require a radical alteration of social conscience and political will. But perhaps the preventable death of a child may serve as added impetus.
