Support WBUR
Study: Fetal Alcohol Syndrome Is Quite Common — And Most Children Aren't Diagnosed
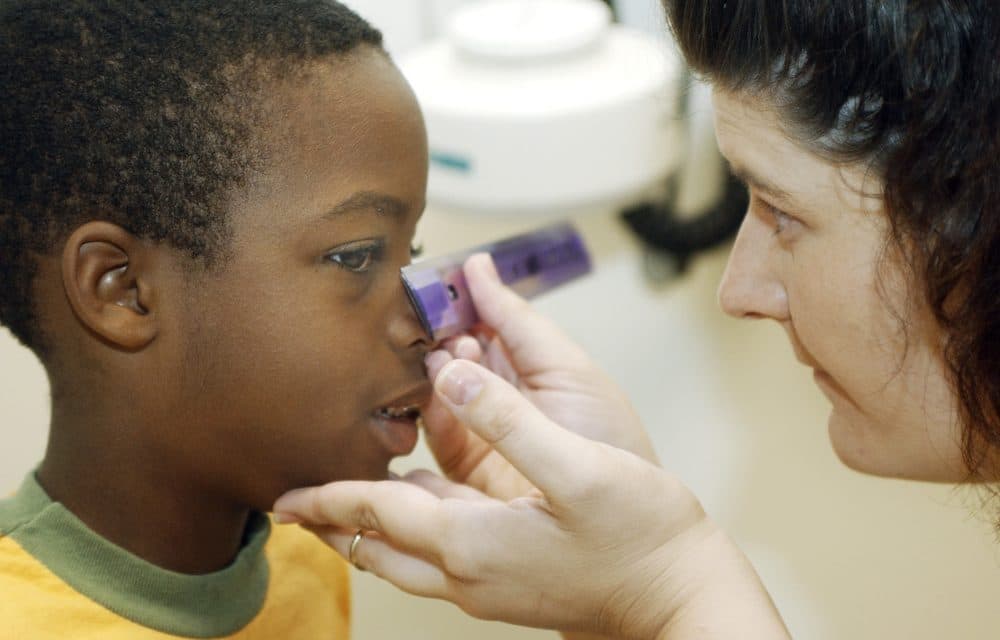
Fetal alcohol syndrome, which can be physically, emotionally and intellectually disabling, is quite common, and most sufferers are not being diagnosed, according to new research.
The study found that 1 to 5 percent of children are afflicted with the disorder -- which makes it far more prevalent than Down syndrome, and equally or more common than autism, though both get substantially more public attention.
“It’s reprehensible that this could be going on this long and nobody bothered to see it,” said Dr. Carl Bell, a Chicago psychiatrist who was not involved in the research, but has been trying to draw attention to the problems of fetal alcohol exposure for years. “Homelessness, drug addiction, violence, suicide, school failure, unemployment, being victimized in childhood. All of those things are connected to this.”
Of the 222 children the researchers found to have fetal alcohol spectrum disorder -- a broader category that includes fetal alcohol syndrome -- only two had been previously diagnosed. So the vast majority of children are being missed by doctors and the social workers, teachers and parents who might seek a diagnosis.
“It’s quite worrisome that this is a problem that really hasn’t had the kind of attention it deserves,” said Dr. Michael Charness, a neurobiologist at Harvard Medical School and Brigham and Women’s Hospital and one of the authors on the new research. “This study I hope will provide a little push to make all of us think harder about how to address it.”
No Safe Levels Of Alcohol During Pregnancy
Roughly half of pregnancies are unplanned and about 30 to 40 percent of women drink regularly, said Christina Chambers, another of the study’s lead researchers, so the damage may already be done by the time a woman realizes that she is pregnant.
Alcohol is known to affect the developing fetus, potentially causing intellectual disabilities, behavioral problems, slowed growth and sometimes seizures. Research — mostly in animals -- has found connections between fetal alcohol exposure and immune problems, metabolic disorders such as diabetes, Alzheimer’s and an increased risk of dying young.
More alcohol is worse than less, of course, but it’s not clear how much alcohol is needed to cause birth defects or whether the precise timing matters, Chambers said.
In studying animals, researchers have never found an amount of alcohol that’s safe to give a pregnant mother.
What is clear is that “the sooner you quit drinking, the better for the baby,” said Chambers, also a professor of pediatrics at the University of California San Diego.
If the mother drinks alcohol very early in pregnancy when the fetus' face is forming — around 17 days after conception, which is before most women know they are pregnant — the child may develop facial features that can be used to diagnose fetal alcohol syndrome: The space between their upper lip and nose is smooth, for instance, rather than grooved; their heads are small for their age; and their eye openings -- the distance between the inner and outer edge of the eyes -- tend to be shorter than normal, said Charness, also chief of staff at the Veterans Affairs Boston Healthcare System.
"The developing brain is affected by alcohol in every trimester of pregnancy."
Dr. Michael Charness
Drinking later in pregnancy causes brain injury, too, Charness said, but without the distinguishing facial features, which is why the condition is now officially called fetal alcohol spectrum disorder.
"The developing brain is affected by alcohol in every trimester of pregnancy," he said.
Why Is It So Often Missed?
The diagnosis is missed in so many children, Charness said, because its effects can be subtle, and because doctors are embarrassed to ask women about their drinking habits during pregnancy.
Those effects can be especially subtle in infancy, not becoming noticeable until the child is a toddler or preschooler, said Kenneth Warren, a study co-author who was head of the National Institute on Alcohol Abuse and Alcoholism when the federally funded study was authorized.
Because it is so often under-reported, the researchers took six years to conduct their study, painstakingly visiting hundreds of first grade classrooms in four communities to look for the condition, rather than waiting for the children to show up in a health clinic.
They talked to children, examined their facial features and behaviors, and interviewed their mothers. The four communities represented a range, from urban San Diego to a Midwestern town in the Rockies to rural Virginia, Warren said. The estimates of fetal alcohol's prevalence are probably conservative, because only about half the families agreed to participate.
Despite the diversity of the four communities, the findings were relatively consistent, Warren said. “It wasn’t like one region stood out,” he said. "Rates in the general population are probably the same or fairly similar across the United States.”
A New Public Health Message
Two years ago, efforts by the Centers for Disease Control and Prevention to limit fetal alcohol exposure backfired when the agency was seen as paternalistically telling all women of childbearing age and not on birth control not to drink.
Now, public health officials have changed their message, focusing on the idea of arming the individual woman with information to protect her fetus, rather than telling her not to drink, Charness said.
Still, there are few medical conditions that have a clearer cause -- or means of prevention.
“If you’re drinking and you’re having sex, using contraceptives will reduce the risk of fetal alcohol exposure. And if you’re trying to get pregnant or might get pregnant, avoiding drinking altogether will prevent fetal alcohol exposure,” Charness said.
But blaming the mother is counter-productive, he said. “A punitive message only increases the stigma and makes it more difficult for people to seek health or change behavior."
Not every woman who drinks during pregnancy will harm their child, Charness noted. “It’s equally important to not panic people who were exposed to alcohol during pregnancy, or mothers who had a drink before they recognized they were pregnant that this is not an automatic consequence.”
Potential Treatments
Diagnosis matters, Chambers said, because early intervention can help children with fetal alcohol syndrome function better.
Bell, the Chicago psychiatrist, said his preliminary research suggests that providing adequate amounts of the nutrient choline in a prenatal vitamin can protect the fetus from the effects of alcohol.
The Institute of Medicine decided in 1998 that prenatal vitamins should include 450 mg of choline. But in a recent study, Bell found that eight brands of the vitamins contained 50 mg or less, and 17 brands had none at all.
Even in adulthood, Bell said, he’s seen a long-term combination of vitamins and minerals, plus social supports, transform people with fetal alcohol, although there are not yet any scientific studies to back up his observations.
In the '70s, alcohol was seen as so harmless during pregnancy that it was often used to slow premature labor.
A Slow, But Growing Understanding
Fetal alcohol syndrome was first identified in 1973, said Warren, who began studying the condition four years later. At the time, he said, alcohol was seen as so harmless during pregnancy that it was often used to slow premature labor.
Women were given an IV drip of alcohol, keeping their blood alcohol levels for days at more than twice what would be considered legal to drive today. “I hope that procedure is not used by anyone in the world anymore,” he said. “Even when it was used, there was no indication that it was any more effective than doing nothing.”
Until recently, researchers focused on the brain deficits that come with fetal alcohol -- ignoring physical problems like heart and kidney defects, Warren said. Most also ignored the fact that children with fetal alcohol syndrome eventually grow into adults with the disorder.
“We’re just beginning to study how all this plays out over a much longer time period,” Charness said.
Demographic Disaster
Bell, a psychiatrist in a hard-scrabble neighborhood of Chicago, said the community where he works has been devastated by fetal alcohol exposure.
He doubts the new study's findings that there were no demographic differences among those affected by fetal alcohol syndrome. The study, published in the Journal of the American Medical Association, found that children from all racial and socioeconomic backgrounds were equally likely to have fetal alcohol disorders. And one 2011 study found that women from high-income households were more likely to binge drink than women with lower incomes -- and thus put their children at higher risk.
But Bell thinks his community is harder hit than others -- and than this new research suggests. In a 2015 examination of 611 children who came to the Jackson Park Hospital's Family Medicine Clinic on Chicago's South Side, roughly 40 percent met the criteria for a fetal alcohol spectrum disorder, Bell said.
Bell describes a recent young patient with fetal alcohol syndrome, who lost control when she couldn’t find her wrist watch. Her temper tantrum wasn’t about being spoiled or rotten, he said, but about needing the watch to compensate for a poor sense of time. But such behavior can often be misunderstood, earning a child punishment instead of help.
Bell said he often sees fetal alcohol in grownups as well. Adults with fetal alcohol may have a bad temper, poor social judgement and terrible math skills, he said. They were often born prematurely and have a heart murmur. They were in special education classes as a child and can’t hold down a job as an adult. They may be violent toward others or at risk of harming themselves.
“It’s all over prison, foster care, special education,” he said. “It’s heart-breaking, that’s what it is.”
