Support WBUR
Penalties For Hospital Readmissions May Boost Deaths, Study Finds
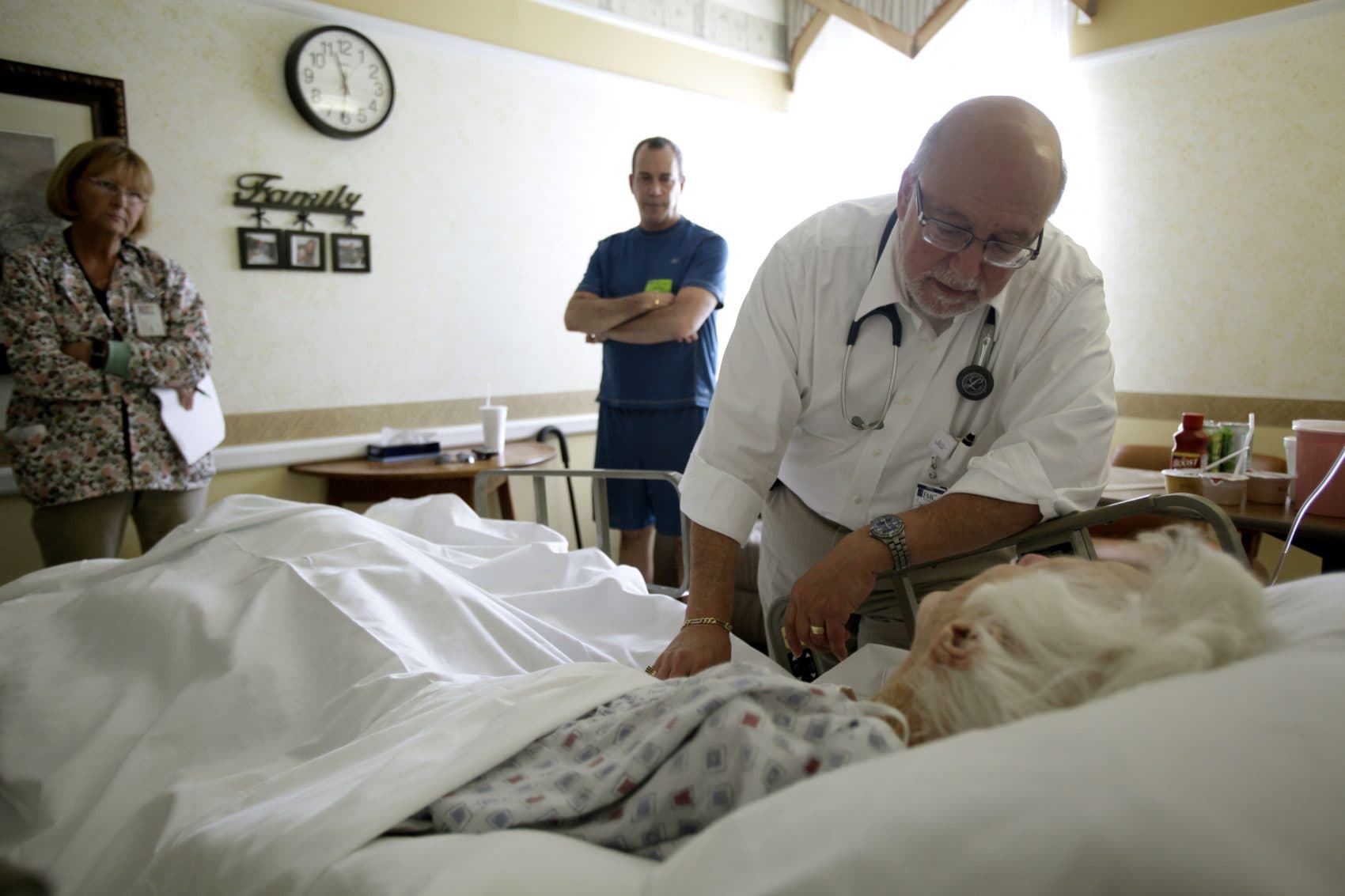
The federal government uses penalties to curb hospital readmissions, but a study in JAMA suggests those incentives may be tied to an increase in mortality rates for patients initially admitted for heart failure and pneumonia.
WBUR’s Martha Bebinger spoke with Dr. Robert Yeh who directs the Smith Center for Outcomes Research in Cardiology at the Beth Israel Deaconess Medical Center. Yeh is one of the study's authors.
Here is a lightly edited transcript of their conversation:
Let’s start at the beginning. What is the Hospital Readmissions Reduction Program?
The Hospital Readmissions Reduction Program was part of the Affordable Care Act, which Congress passed in 2010. The law created financial penalties for hospitals with higher-than-expected readmission rates for patients with pneumonia, heart failure and acute myocardial infarction (heart attack). Under the law, the penalties would be levied based on historical data, meaning the question was how your readmission rates compared the past few years.
The financial penalties didn’t begin until 2012, but in 2010, we all became very aware that hospitals stood to be penalized quite significant sums of money, and most hospitals began to make preparations to reduce readmissions at that time.
Tell me about your study. What did you look at, and what did you find?
We studied approximately 8 million Medicare patients hospitalized between 2005 and 2015, and what we found was that implementation of this policy – the HRRP – coincided with a significant increase in deaths within 30 days of discharge among patients hospitalized for heart failure or pneumonia, but not for those hospitalized for heart attacks.
What do you mean by “significant"?
In paper we refer to statistical significance. It doesn’t look like these rises were due to chance alone. It looks like there was a measurable change in the trajectory of deaths that occurred. We can also look at the magnitude of that effect. It looks like there might have been a little bit more than 10,000 excess deaths that occurred after the implementation of the HRRP. Those deaths were split fairly evenly between heart failure and pneumonia.
What do you think could be behind these findings?
I think there are several possible explanations for the findings. The most concerning would be that the passage of this law and the implementation of this policy created incentives that actually worsened the quality of care we’re delivering at hospitals. There’s certainly some evidence that physicians and clinicians felt some pressure not to admit patients to the hospital, and there might have been patients who had really good indications for being admitted to the hospital who were instead cared for in the emergency room. It’s not always clear that it’s in the best interest of patients to be cared for in these non-inpatient settings.
Another possible explanation is that patients now may actually be sicker than they were historically. And so the rise in mortality reflects that we’re caring for a more debilitated and a more morbid group of patients than we had historically, in a way that we can’t actually measure.
Why might that be the case?
One reason could be that if the threshold for admitting patients to the hospital is now higher, it could be that in order to qualify for admission, you need to have a more severe illness than you did historically.
What should people do with these findings? Do you have any recommendations?
I think that the most important thing that we need to think about at the hospital level, and as physicians, is how we respond to incentives. This really should be first and foremost about patient outcomes including their mortality rate.
Why are health policies that profoundly influence patient care not rigorously studied before their widespread implementation in the same way that we rigorously test new medications or devices?
Dr. Robert Yeh
There’s consideration for extending this law to all hospitalized conditions. For now, from a policy standpoint, we ought to proceed with more caution. HRRP should probably not be expanded to all hospital conditions until we have a better understanding of what is responsible for these trends.
And the findings really highlight a larger issue. Why are health policies that profoundly influence patient care not rigorously studied before their widespread implementation in the same way that we rigorously test new medications or devices? It’s imperative that we understand the potential intended and unintended consequences of our policies before they’re widely disseminated.
Any final thoughts?
In the past, we found that readmissions had declined nationally with implementation of this policy, and we thought that was actually a good thing. People prefer not be in the hospital. Being in the hospital is disruptive to one’s circadian rhythm and you’re exposed to hospital-acquired infections.
There are a lot of good things that come out of not being readmitted to the hospital, but we think the ultimate arbiter for the policy should be mortality.

