Support WBUR
Now Mandated To Offer Meds For Opioid Addiction In The ER, Mass. Hospitals Get 'How-To' Guidelines
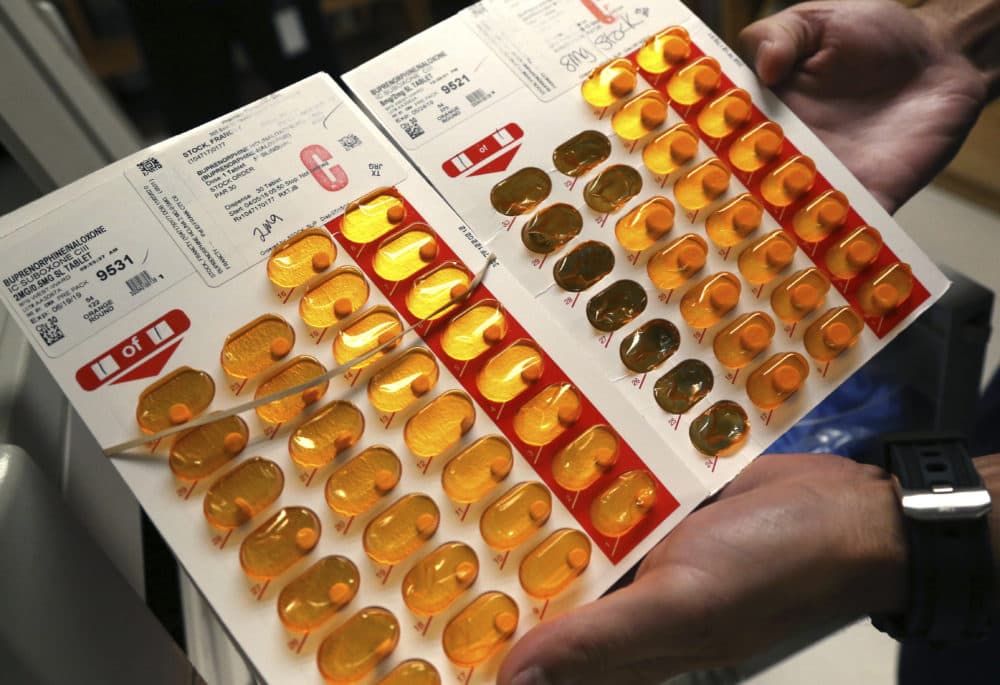
A hospital emergency room is the common place a drug user connects with health care: after an overdose, to treat an infection or deal with an injury. But the vast majority of ERs don't treat the underlying problem: drug addiction. Instead, patients typically leave with a slip of paper and a few names and numbers of programs where they might get help.
In Massachusetts, that is no longer allowed.
A 2018 state law requires roughly 80 hospitals and satellite emergency rooms to offer patients addicted to opioids a medication to help treat their disease. A handful do. For most, this is a new frontier.
For starters, most hospitals don't have enough or any emergency department physicians, nurses and physicians licensed to prescribe buprenorphine, often sold as Suboxone, a drug that curbs cravings for stronger opioids.
Now the Massachusetts Health and Hospital Association (MHA) is out with guidelines that explain how staff can obtain permission to prescribe buprenorphine; how to screen patients who might benefit from the drug; when to begin the first dose; and ways to get patients up to three days' worth of the drug.
"We're facing an opioid crisis of proportions we've never seen before and EDs and hospitals are on the front lines of that," said Leigh Youmans, MHA’s senior manager of behavioral health and health care policy. "This is a critical moment that we can really get people into treatment and help them get back to their lives."
The expectation is that patients will get a prescription for more buprenorphine at their follow-up appointment outside the hospital. But many hospitals do not have addiction clinics or a network of primary care providers trained to manage patients on buprenorphine. The guidelines suggest these hospitals partner with nearby community health centers or existing addiction treatment programs, including methadone clinics, which the MHA says may soon expand to include buprenorphine and naltrexone, a drug that blocks opioid receptors.
But making sure patients have a place to continue treatment that begins in an ER is the biggest challenge ahead, especially for small or rural hospitals, says Dr. Ali Raja, who chaired the MHA guideline working group.
"This is going to take hospitals. This is going to take communities. This is going to take towns to set up outpatient treatment facilities for patients who we initiate in the emergency department," said Raja, vice chair of the Department of Emergency Medicine at Massachusetts General Hospital.
Raja says the main lesson he's learned after almost a year of initiating medication-assisted treatment at Mass General is the need for a seamless connection to outpatient care. Raja remembers patients who couldn't make it from the ER to an outpatient clinic within the hospital. Now he or a colleague take patients right into the clinic waiting room.
"That outpatient connection is so tenuous that if we don't make it as easy as possible for our patients, they may never connect," Raja said.
Some hospitals have hired or plan to hire recovery coaches to supervise the transition from the ER. Their responsibilities include ensuring patients take their next dose of buprenorphine, or helping them get to the first few follow-up appointments and begin counseling.
For decades, many doctors and hospitals avoided addiction treatment. Patients entered programs outside mainstream medicine.
"The divide still exists to a certain extent, but it's narrowed considerably over the past 10 years. This is an opportunity to further bridge that divide," said Vic DiGravio, president and CEO of the Association for Behavioral Healthcare, which represents mental health and addiction providers. He offered input on the MHA guidelines.
DiGravio says the guidelines reinforce the science: that addiction can be treated.
"There's still a mindset out there that addiction is a moral failure, that people really don't want to get better," said DiGravio. "Unfortunately that stigma is not just in the general population but in parts of the medical community as well. So the hospital association saying this something we can do and are excited to do, that sends a really clear message.
It's also clear from the guidelines that there will be hitches. Hospitals without an in-house pharmacy will have to ensure local pharmacies can fill short-term prescriptions for buprenorphine. Some ERs may need to rely on providers available via telemedicine to write the prescription. And, there is no billing code yet for initiating medication-assisted treatment in a hospital emergency room.
The MHA says it is not aware of any other states that require offering medication-assisted treatment to patients treated in an emergency room.
The MHA reviewed guidelines in use or being tested by individuals hospitals in Colorado, New Haven, Buffalo, Rhode Island and an eight-hospital pilot project in California. Going forward, Massachusetts hospitals will have to show compliance with the requirement to renew their state license.
