Support WBUR
The Case For Sending Drug Users Home From The Hospital With Open IV Lines

Two mornings a week, Arthur Jackson clears space on half of his cream-colored sofa and waits for a knock at his front door. He leaves a few rolls of tape and some gauze.
“This is Brenda’s desk,” Jackson says with a chuckle.
Brenda Mastricola, Jackson’s visiting nurse, takes his blood pressure and changes the bandages on Jackson’s right foot. His big toe was amputated in November. An infection, osteomyelitis, destroyed the bone.
Jackson is on penicillin to stop the infection. He came home from the hospital wearing a small pump. It delivers a steady dose of penicillin via a PICC line, a sort of flexible IV, inserted into Jackson’s chest.
“This all looks good,” Mastricola tells Jackson as she checks to make sure the line is clean and in place. “You don’t need me.”
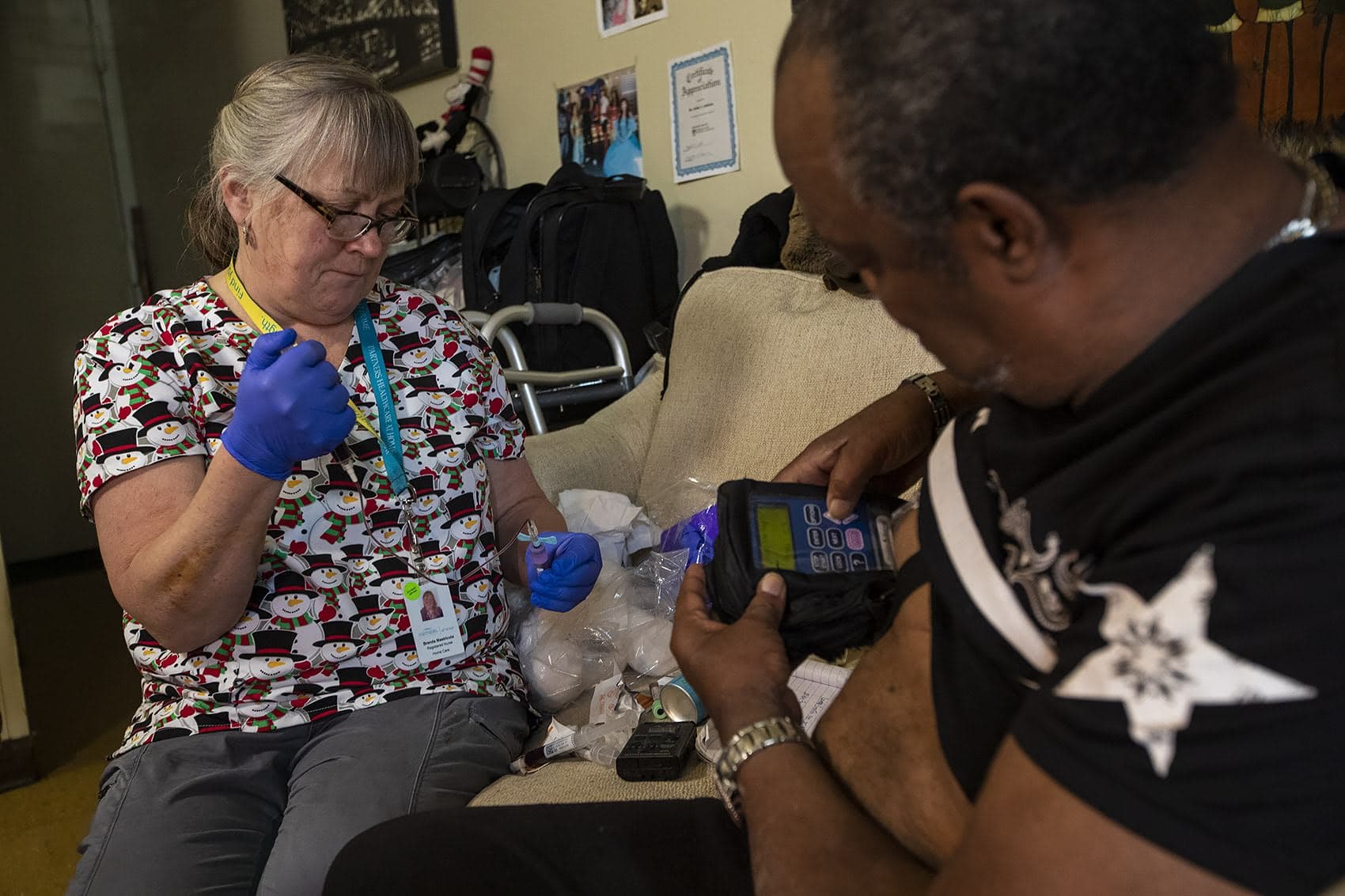
Finishing IV antibiotic treatment at home has become standard protocol for patients like Jackson with a serious bacterial infection. Except that Jackson, who is 69, was addicted to heroin for 40 years. Sending someone with a history of injection drug use home with an open line into a major vein is just not done in the U.S., except at a handful of hospitals. Brigham and Women’s is now one of them.
Mapping A Path To Safe At-Home Treatment
A small team of Brigham doctors and nurses started planning this very unusual option shortly after opening a walk-in clinic for patients seeking treatment for a substance use disorder. Dr. Christin Price, the Bridge Clinic’s program administrative director, says virtually every patient who injects drugs develops some kind of infection. It’s difficult to avoid injecting bacteria into the bloodstream.
“Every time someone uses injection drugs they’re putting themselves at risk for a very complicated infection,” Price says.
A study out of North Carolina found a 12-fold increase in endocarditis, a heart infection, within one decade. But treatment options for patients with a history of drug use are limited. Some skilled nursing facilities, home care agencies and antibiotic infusion companies won’t work with these patients once they’re released from a hospital. And Price says some of her patients aren’t willing to remain in a medical setting for weeks on end, just to finish a round of IV antibiotics.
“They kind of get stir crazy. You can imagine it’s almost like being held captive for six weeks, especially when you’re feeling fine now because the infection is clearing,” Price says. “A huge problem is that some of them can’t last and so they leave before the six weeks are over.”

Patients who don't complete their course of antibiotics could end up with a repeat infection and another trip to the hospital.
Doctors and nurses affiliated with the Bridge clinic wondered if there wasn’t a way to send patients with a history of drug use home — safely. They mapped three requirements. First, patients would have to be on an addiction treatment medication, or be willing to start one. Second, patients would have to check in weekly at the Bridge clinic. And third, patients would need to have stable housing shared with a sober friend or loved one.
Price and colleagues began months of discussions with heart, bone and joint specialists, surgeons and nurses who would need to buy-in, so their patients could participate.
“A lot of people did sort of look aghast,” Price says. “It was just their policy that people with a history of injection drug use would not go home.”
When Dr. Daniel Solomon encountered those looks, he says he’d remind colleagues “that the alternatives aren’t that good either.” Solomon says holding patients is hard on both them and providers. And if patients want to use drugs they’ll find a way to do it in a hospital bed.
In the spring of 2018, Price and Solomon and others enrolled a few patients, then a few more, admittedly cherry-picking those who wanted to be in treatment and who had a sober, stable home.
‘I’m Not Going Back’
Arthur Jackson says there shouldn’t have been any question that he met the first and second requirements. He’d been on methadone for 10 years, used heroin again, then switched to Suboxone, a version of buprenorphine that he’s been taking for two years. In fact, Jackson says he was insulted when one of the doctors presented the home treatment option to him but said she was worried the PICC line might entice him to inject heroin.
“Stop right there,” Jackson recalls telling the nurse. “When it comes to my recovery, I'm serious because I’ve done so much to lick this thing.”
Not that Jackson didn’t consider it.
“First thing I thought was, ‘Oh, I could “inject heroin in here easily,’ ”Jackson says. “But I dismissed that thought because I’m not going back.”
Back to winters on the streets and living from one heroin fix to the next. Other Bridge patients scoff at the PICC line concerns.
“Everyone makes such a big deal about this PICC line,” says Stephen Connolly, 36, who went home with the open port last year to treat endocarditis. “If I want to get high, I know how to do it. I’m not going to mess around with a PICC.”

Connolly says he came to the Brigham focused on his heart, ignoring his other disease: addiction. Connolly says he was surprised when every doctor he saw, even his cardiologist, wanted to talk about addiction.
“I’m like, ‘listen dude, my heart’s falling apart here, so let’s hold up with the drug talk,' ” Connolly recalls. He assured the cardiologist he had his addiction under control.
“Obviously I didn’t, but my mind tells me that. It’s just crazy.”
Connolly finished his antibiotic treatment with family in Abington. Jackson is back at his studio apartment in Roxbury. He lives alone, but persuaded doctors he’d be better off there so he could visit his 93-year-old mother daily, feed his cat and tank of tropical fish and attend his regular Narcotics Anonymous meetings.
“I guess the best way to put it is, I have a life and I need to get back to it,” he says.
“I’m like, ‘listen dude, my heart’s falling apart here, so let’s hold up with the drug talk.”
Stephen Connolly
Brigham doctors say the housing requirement eliminates many patients. A few hospitals are testing ways to continue treatment for patients who don’t have a stable home. In Portland, Oregon, a medical center tried providing IV antibiotics inside addiction treatment programs. A hospital in Kentucky combines addiction treatment, counseling and outpatient IV antibiotics. In Vancouver, the national health program funds small apartments, staffed 24 hours a day with a nurse, where patients can stay while they complete antibiotic treatment.
“People who use drugs deserve the same standard of care,” says Dr. Christy Sutherland, medical director at the Portland Hotel Society in Vancouver. “We can’t change what we offer as clinicians to give people subpar treatment with the excuse that they are IV drug users.”
There are other ways for patients to continue antibiotics outside a medical facility: pills taken several times a day and weekly infusions for some, not all, infections. The standard line in medicine is that these aren’t viable options for active drug users, especially if they don’t have a home. Recent research shows homeless patients with HIV or Hep C do take their meds; there are no robust studies on homeless patients treating bacterial infections.
Dr. Joshua Barocas, an infectious disease physician at Boston Medical Center, says he understands why doctors don’t want to take risks when treating endocarditis and other serious conditions. A home-based antibiotic treatment program can be tricky to manage and administer, even more so if a patient is struggling with a substance use disorder.
“There are some people that can and should be treated in the hospital for their infections,” Barocas says. But “when we’re talking about people who inject drugs, we need to work past the long-held beliefs of the medical community and figure out what’s best for the patient and what’s going to improve their outcomes, not what we feel the most comfortable with.”
Promising Early Signs
Jackson is one of 40 patients with a history of drug use the Brigham has discharged to complete IV antibiotic treatment at home. The Brigham is paying particular attention to 21 patients within that group who are active drug users. So far, these men and women have finished their antibiotic treatment via a PICC line with no complications. One had to be readmitted because he had trouble administering the antibiotics. Price says there were three relapses, but no one used the PICC line.
“I think we’ve shown through this pilot that it is safe and feasible, for certain patients,” she says.
And, says Price, this pilot is cutting health care costs. Together the 21 high-risk patients spent 571 days at home rather than in a hospital or rehab facility, saving roughly $865,000, based on estimates of $1,500 per hospital day. That doesn’t include the cost of home care visits.
Medical ethics experts say cutting costs is fine, but the main question is whether sending patients who’ve injected drugs home with an open line into a major vein will do more good than harm.
“The key here is rather than relying on emotional arguments or knee-jerk reactions, I think it’s really critical that we use an evidence based approach to making sure that we’re treating these patients appropriately,” says Dr. Sarah Hull, a cardiologist at Yale School of Medicine who writes on medical ethics.
But with only a handful of hospitals in the U.S. discharging patients who’ve injected drugs with a PICC line, the research is limited. Brigham doctors plan to publish their initial results. They reviewed 10 studies from the U.S. and three other countries while launching this project and concluded that completing IV antibiotics “may be as safe and effective” for patients who inject drugs as for those who don’t.
A more recent study out of Kentucky supports using outpatient IV antibiotic treatment for patients with a history of drug injecting, as long as those patients are on medication to treat their addiction.
Massachusetts General Hospital offers home-based IV antibiotics as an option to some patients with a history of drug use. Two years ago, MGH published a comparison of such patients who’d gone home with a PICC line and those who went to a skilled nursing facility. The home-based treatment patients had fewer readmissions, relapses and complications.
Many drug users describe being hospitalized with a life-threatening infection or needing open heart surgery (related to endocarditis) as their wake-up call, the event that led them to treatment. Doctors and nurses agree but say too many hospitals and skilled nursing facilities don’t offer addiction treatment medications or connect patients to programs that do. Dr. Sarah Wakeman, the medical director of Mass General’s substance use disorder initiative, says nurses and physicians have an important opportunity to connect with patients and discuss addiction treatment while they are hospitalized with a serious infection.
“And yet, the system is built to do the opposite with siloed care. There aren’t really integrated programs where someone would get their medical and addiction therapy in the same place,” she says. “We need some innovation here to better meet the needs of patients.”
This segment aired on January 8, 2020.
