Support WBUR
Most Residential Addiction Treatment Programs Don’t Offer Live-Saving Medication
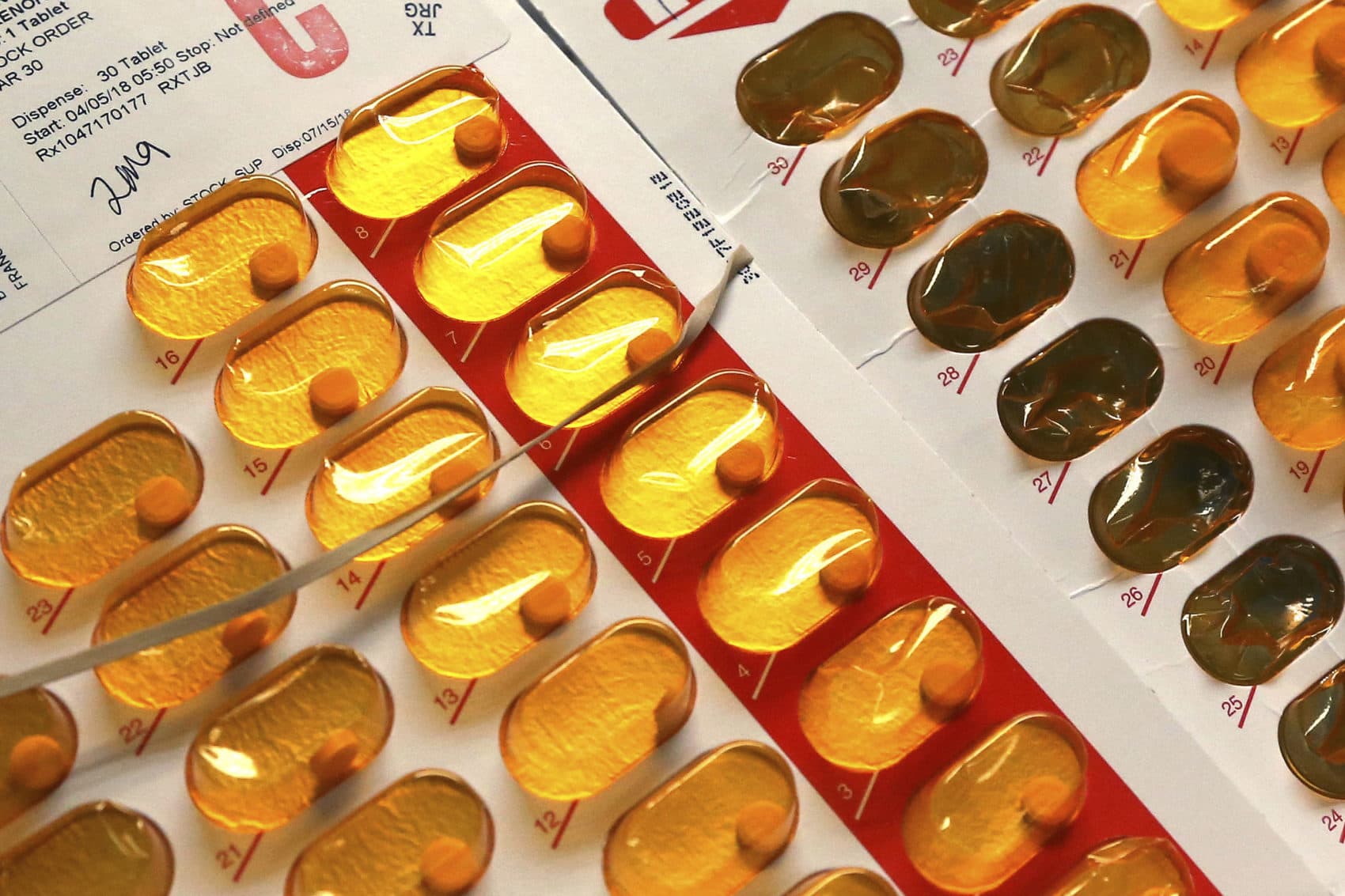
Patients seeking treatment for an opioid addiction have limited access to a life-saving medication, buprenorphine, in residential treatment facilities across the U.S. Research published in JAMA finds that 29% of 368 programs contacted offer the drug that helps reduce cravings for heroin or fentanyl. Another 21% of the treatment centers contacted discouraged its use.
The results build on previous research that shows most programs that patients check in to for days, weeks or months at a time do not offer any of the FDA-approved medications to treat an opioid use disorder. That’s despite the growing body of work that concludes buprenorphine reduces the risk of relapse, overdose and death.
The study used a “secret shopper” approach. Callers posing as 27-year-old uninsured heroin users reached out to both private and government-run facilities.
The researchers, based at Harvard, Johns Hopkins and Yale University, say the results raise concerns about the quality of care patients can expect to find at residential treatment programs. Lead author, Dr. Michael Barnett, says prescribing buprenorphine should be a basic component of addiction treatment.
“That’s a very low bar to pass and still most facilities aren’t meeting it,” says Barnett, an assistant professor of health policy and management at Harvard’s Chan School of Public Health.
The limited use of buprenorphine, whose brand names include Suboxone, Subutex and Sublocade, highlights a long-standing controversy. Many people who’ve been addicted to drugs or alcohol say abstaining from all such substances is the only way to fully recover. They argue that using buprenorphine, a less potent opioid, is substituting one drug for another.
Barnett says that’s more of a philosophy than a position based on clinical results.
“As a physician, I’ve seen how medications like buprenorphine can let my patients with an addiction really lead normal lives,” he said. “It’s a medication just like anything else we use to treat an illness, whether we use an antidepressant for someone who has depression or insulin for someone who has diabetes.”
Annie Peters, director of research and education with the National Association of Addiction Treatment Providers, says she was sad but not surprised to read the study results. She’s heard from people in recovery who feel strongly that others can not make the emotional, lifestyle and spiritual changes while they are under the influence of a drug.
“But spiritual and emotional change is fully compatible with use of a medication that helps you not crave and not overdose,” says Peters.
Peters adds that counseling and group therapy must be packaged with a prescription for buprenorphine.
The NAATP promotes abstinence but Peters said it’s time to redefine what means.
“Abstinence is abstaining from the chemicals that are killing you, the ones that cause you to lose your family and your job and your self-esteem and your mental health,” she says. “If you can abstain from those and take the medications that will be helpful in getting those things back, that’s what needs to change.”
Here’s another reason some addiction treatment providers are opposed to buprenorphine; they argue it is resold and misused on the streets. But Peters points out that’s true for many prescribed medications including antidepressants and drugs that relieve anxiety.
Peters says one remedy here is more education about the benefits of buprenorphine. She and Barnett agree that providers would change quickly if the agencies that license treatment programs started requiring buprenorphine as an option, or if insurers stopped paying facilities that don’t offer it.
