Support WBUR
Finally, Medications That May Help People Addicted To Meth
Methamphetamine use and resulting overdose deaths are devastating families in cities and towns across the U.S. In the world of addiction treatment, many specialists say meth is their most formidable challenge. There are no accepted medications that help patients resist the intense cravings.
That starts to change today with the publication of a study through which meth users received a combination of two approved drugs, an antidepressant and naltrexone, which is prescribed for addictions to opioids and alcohol. Among the 403 study participants, nearly 14% of those who took the combo presented mostly drug-free urine samples. It’s a modest percentage but still more than five times greater than participants who received a placebo.
“It’s the first time we have a large trial showing such a clear signal of therapeutic benefit, so it’s a big deal."
Dr. Nora Volkow, NIDA
“It’s the first time we have a large trial showing such a clear signal of therapeutic benefit, so it’s a big deal,” said Dr. Nora Volkow, director of the National Institute on Drug Abuse (NIDA).
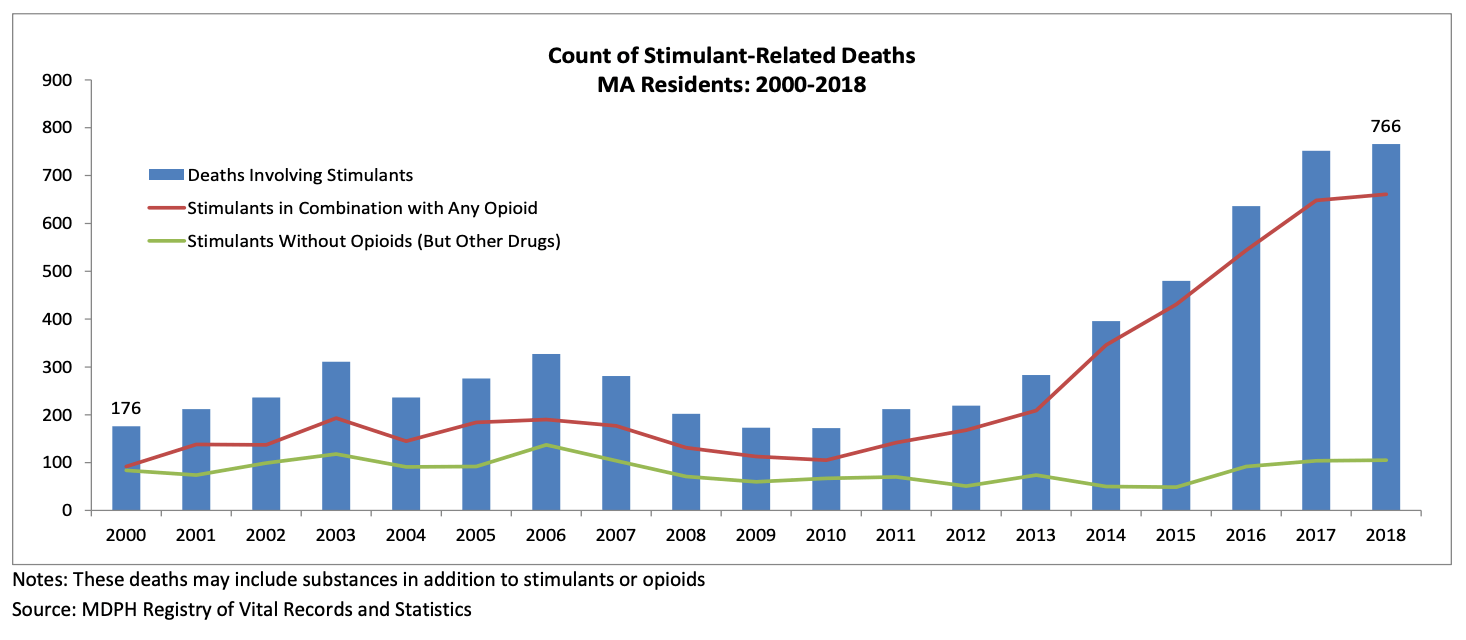
The results are particularly important now, says Volkow, when the latest CDC figures indicate deaths tied to meth use increased 35% in one year. In Massachusetts, where Mike Leslie is in recovery from addictions to several drugs, fatal overdoses involving meth and other psychostimulants have risen more than 400% since 2000. In Boston, where Leslie supervises recovery coaches, he says meth use is rampant.
“To see the state of meth right now and how it continues to rise, there’s no better time to come up with a breakthrough like this,” Leslie said.
But this drug combination might not work for people like Leslie who sometimes used meth in combination with an opioid. Naltrexone, one of the two drugs in this study, blocks opioid receptors. It essentially pushes anyone who’s taken an opioid, including a very low dose medication like buprenorphine, into immediate withdrawal. So Dr. Laura Kehoe says while she’s excited about getting help with meth treatment, she doesn’t expect to begin frequent prescriptions of these two drugs.
“Primarily what we’re seeing is people who are using multiple substances,” said Kehoe, who is medical director at the Massachusetts General Hospital Bridge Clinic. “There’s a huge subset of patients who have chaotic opioid [use] in addition to methamphetamine use who would not be able to use this medication combination.”
Prior research has looked at each of these drugs separately and not found any significant impact on meth use. Lead author, Dr. Madhukar Trivedi says this study didn’t try to assess why bupropion, the generic version of the antidepressant Wellbutrin, and injectable naltrexone, also known by the brand name Vivitrol, worked when used together, but the study does suggest whether or not they did work.
“We wanted to be very crisp about this because unfortunately the risk and public health magnitude of the problem is only increasing,” said Trivedi, a psychiatry professor at the University of Texas Southwestern Medical Center. “The urgency of finding a treatment that works is quite dire.”
Trivedi says the next hurdle will be educating patients and clinicians about this option and trying to ensure that prescriptions for this use of the two approved drugs are reimbursed by insurance companies. Some clinicians say that may not be a significant hurdle because many people who use drugs suffer from and are prescribed an antidepressant and many have a co-occurring addiction for which naltrexone would be appropriate.
“These meds are on formularies and bupropion is generic so access should not be much of a challenge overall,” said Dr. Ken Duckworth, chief medical officer at the National Alliance on Mental Illness, in an email.
Duckworth calls the study compelling. He says the efficacy of this drug combo, that helps 1 of every 9 patients who get it, is comparable to other behavioral health medications. Both Duckworth and Kehoe say they would like to see a larger trial group.
“In terms of changing stigma about people who use methamphetamine, that’s a game changer.”
Justin Alves, BMC's OBAT
Justin Alves, a nurse who has worked with patients addicted to meth since 2013, said he’s impressed that the study was done at all and that participants addicted to meth stayed involved. Alves says the results offer hope that’s been sorely missing for clinicians and for patients with a stimulant use disorder.
“Many providers won’t even see these folks, won’t even do the intake or will exclude them from treatment because they feel like, ‘I have nothing to offer them, why would I see them?’ ” said Alves, who is a nurse educator at Boston Medical Center’s Office-based Addiction Treatment (OBAT) program. “In terms of changing stigma about people who use methamphetamine, that’s a game changer.”
Researchers in this study encouraged counseling but did not require it. Alves expects that adding support systems and behavioral health interventions would boost the success rates for patients. One such intervention, contingency management, provides people who use drugs gift cards for reducing their drug use. Alves says most providers don’t try it because they aren’t reimbursed. Recent legislation in California would require coverage by the state’s Medicaid program.
Drug company Alkermes, with offices in Waltham provided Vivitrol for this study. The company declined comment on the results and the possibility of a new market for its injectable version of naltrexone. Trivedi has consulted for the company in the past but says they had no influence over or input into this research.
Bausch Health, the makers of Wellbutrin, said in a statement that “these independent results appear to show promise for the difficult problem of methamphetamine addiction. Our team will review this data and assess possible paths forward for investigation of WELLBUTRIN XL for this potential indication.”
