Support WBUR
Mental health emergencies rise with heat for all ages, study finds
Hospital emergency rooms may see more patients with depression, anxiety and substance use disorder as summer temperatures rise.
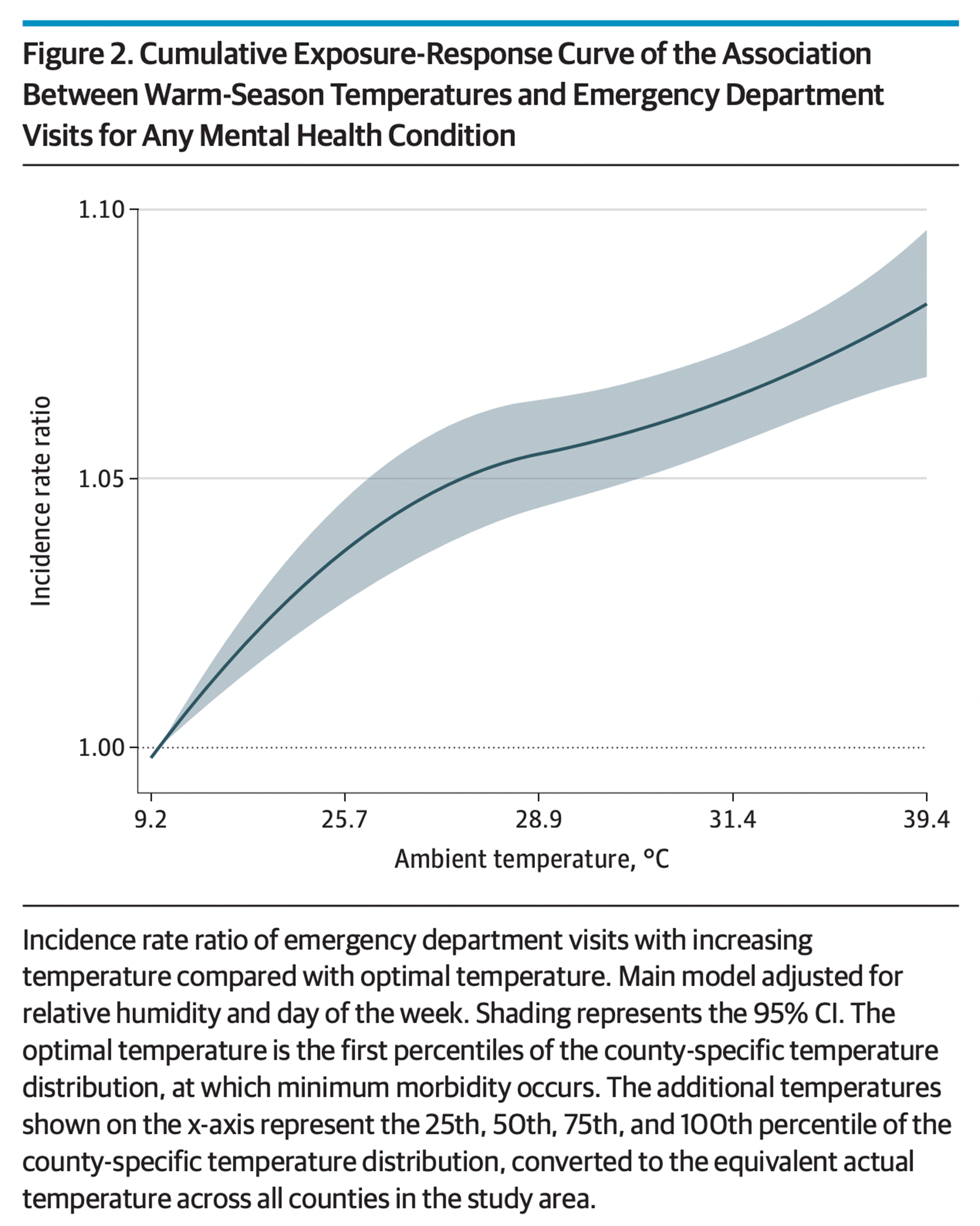
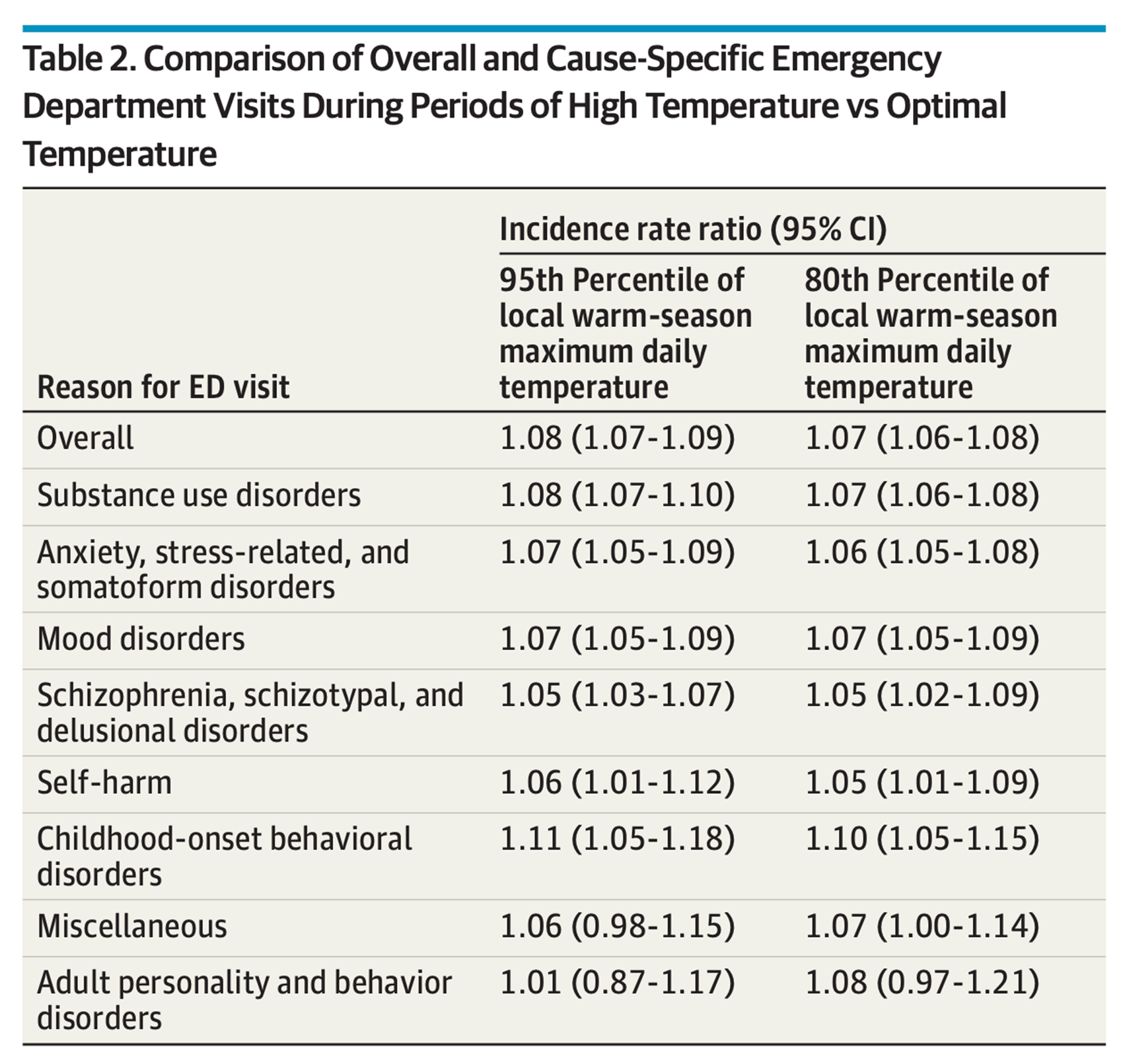
A study in the medical journal JAMA Psychiatry shows a modest but steady increase in behavioral health insurance claims throughout the U.S. aligned with warming days. On peak summer days, the researchers find 5-10% more ER visits for mental health emergencies than in cooler spring months.
It’s a pattern researchers at the Boston University School of Public Health say will become more pronounced as more areas experience prolonged, extreme heat.
“What we’ve been able to show is that climate change is not a theoretical future problem to be dealt with,” says the study’s lead author, Amruta Nori-Sarma. ”It’s something that is impacting our health and impacting our communities today.”
The findings are based on 3.5 million insurance claims filed from 2010 to 2019, which were provided by OptumLabs Data Warehouse. The highest rates of increase are in northern states. Nori-Sarma says that is probably because residents of these states are less likely to have air conditioning.
The association between heat and mental health or substance use emergencies is similar for all age groups, the findings show. The study is one of several that point to heat as a health risk for children as well as older adults and those with chronic conditions.
Some emergency room physicians are not convinced. Dr. Kathleen Kerrigan, president of the Massachusetts College of Emergency Physicians, says she’s not aware of any increase in mental health visits during hot weather.
Dr. Hamad Husainy, speaking for the American College of Emergency Physicians, agrees. Husainy says if there are more behavioral health insurance claims in the summer, it may be because mental health problems are more public during warmer months than in the winter when people tend to isolate at home. But Husainy says the research could open new ways of thinking about emergency room visits.
“The data may debunk some of our innate opinions about what drives volume [in emergency rooms],” says Husainy. “And it will make me ask more about my own patients.”
Dr. Lise Van Susteren says there are clear physiological reasons heat could send more patients with mental health issues to an ER. Heat, for example, can trigger a release of stress hormones.
“The substances that jack your system up into a fight or flight mode go up when exposed to heat,” says Van Susteren, a psychiatrist and author who studies the impacts of climate change on mental health..
For patients managing an addiction, Van Susteren says heat can increase the urge to self-medicate with drugs or alcohol.
“That’s how people try to turn the temperature down,” she says.
Van Susteren adds people living with mental illness also may have poor judgment and self-regulation, sometimes as a side effect of medications, especially those that block perspiration. So doctors may need to adjust those meds and take extra steps to make sure patients can spend hot days in a cool place.
Nori-Sarma, the lead researcher, says she hopes the study will encourage patients and clinicians to recognize they may need more support during the hottest days of summer. That could mean more counseling, guidance about finding air-conditioned spaces or education about when rising temperatures can trigger problems.
“This speaks to the need to identify patients who may be particularly susceptible,” Nori-Sarma says, “to avoid those emergency department visits which are very costly both from an individual perspective and also from the perspective of our health care system.”
