Support WBUR
There’s still time to contain the monkeypox outbreak, doctors say
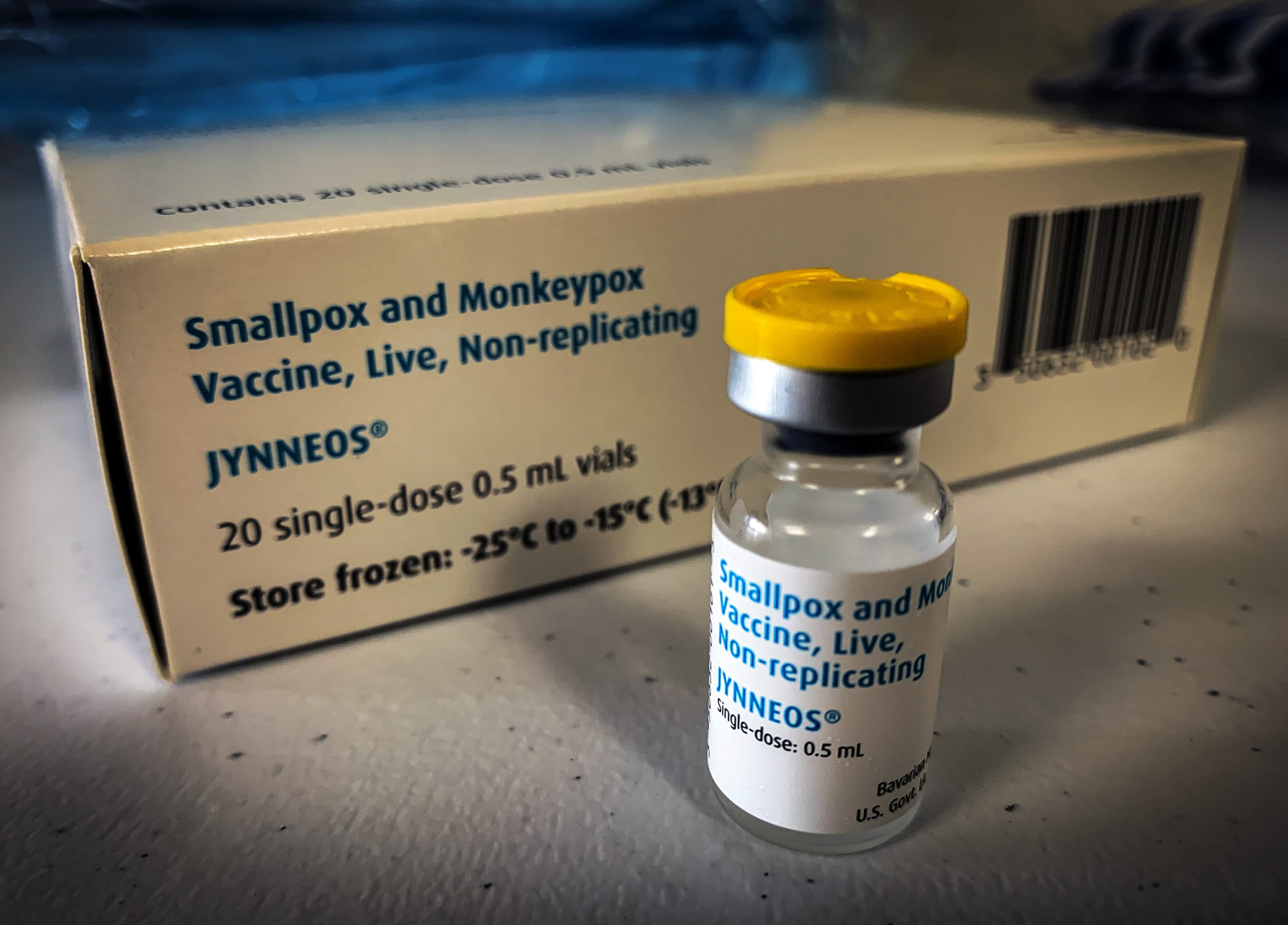
Massachusetts health care providers say they’re hopeful that a new strategy to combat monkeypox will help meet the soaring demand for vaccines and contain the disease outbreak, even as cases continue to rise.
Massachusetts health officials on Wednesday adopted a new federal policy to use smaller doses to vaccinate people at risk of getting sick with monkeypox.
The new strategy allows health care providers to use one-fifth the typical vaccine dose, stretching the country’s limited vaccine supply.
“I think it will be significant,” said Dr. Gabriela Andujar Vazquez, infectious disease physician and associate hospital epidemiologist at Tufts Medical Center. “It basically multiplies by five our current stockpile. I think it will change and hopefully curb the spread of the disease.”
The smaller vaccine doses need to be administered intradermally, meaning between the layers of the skin, instead of subcutaneously, or beneath the skin.
“It does change the standard operating procedure, but it's not something that is necessarily new to health care workers," Andujar Vazquez said. "We just have to make sure that everyone's up to speed with how to do it.”
A group of 14 clinics across Massachusetts are offering vaccinations to people at risk of developing monkeypox — and demand has been high. At Fenway Health, a health care provider known for serving the LGBTQ community, as many as 600 people a day have been calling in search of vaccine, according to Dr. Brian Bakofen, Fenway’s interim medical director
Boston Medical Center recently had a waitlist of 800 people seeking monkeypox shots.
“We've been inundated with requests for vaccines,” said Dr. Cassandra Pierre, infectious disease physician and associate hospital epidemiologist at BMC.
Containing the outbreak, Pierre said, will require more vaccinations, as well as targeted outreach to people at risk and better data collection to monitor the spread of the disease.
So far, health care providers are mostly responding to demand for vaccine and haven't started reaching out to individuals who may be at risk but face barriers to coming into clinics to get vaccinated.
“I am hopeful that we will be able to curtail this, maybe in the next few months to a year,” Pierre said. “But there are a lot of gaps. We have a lot of blind spots.”
The monkeypox outbreak has echoes of the early days of COVID: an unexpected disease spreading quickly, public health agencies unprepared, people scrambling to find vaccines. But experts say there are many important differences between the two outbreaks.
Monkeypox is not a new disease. Doctors have seen it before, and vaccines, though in short supply, already exist.
Monkeypox doesn't appear to spread easily through the air like COVID. Scientists are studying how often it's transmitted through respiratory particles, but so far, it seems to be spreading mostly through direct contact with the skin or bedding or clothing of an infected person.
The virus is not sexually transmitted, but in recent cases, it appears to be spreading during intimate contact, including sex.
“It's not like with COVID, where everyone is at risk,” Andujar Vazquez said. “With monkeypox, the spread is really direct contact with infectious rash and scabs and body fluid. And it's intimate skin-to-skin direct contact."
Monkeypox can cause a painful or itchy rash and flu-like symptoms. But treatment and recovery usually happen at home.
The Centers for Disease Control and Prevention have counted nearly 12,000 cases of monkeypox across the country, including more than 200 in Massachusetts. Black and Hispanic people account for more than half of U.S. cases, according to the CDC.
Deaths have been exceedingly rare worldwide, and none have been reported in the U.S.
COVID, by comparison, has been far more deadly, especially before vaccines and treatments were widely available.
COVID has infected people of all ages, in schools, workplaces and nursing homes. But the vast majority of monkeypox cases have been among men who have sex with men.
“We’re not seeing a rapid spread outside of that population, which is a good sign,” said Dr. Andrew Jorgensen, chief medical officer at Outer Cape Health Services.
The experience in Provincetown, where Jorgensen sees patients, suggests controlling the outbreak is still possible in certain communities. Case numbers in Provincetown are on the decline, which may be a sign that vaccination efforts are working.
“Most of the local population at risk has been vaccinated,” Jorgensen said.
“I don't think this is going to transition to an epidemic or an endemic disease,” he said, “but as I've learned from COVID, you can always be surprised.”
This article was originally published on August 17, 2022.
