Support WBUR
Commentary
The Most Important Part Of A Doctor's Job Is Not Her Bedside Manner
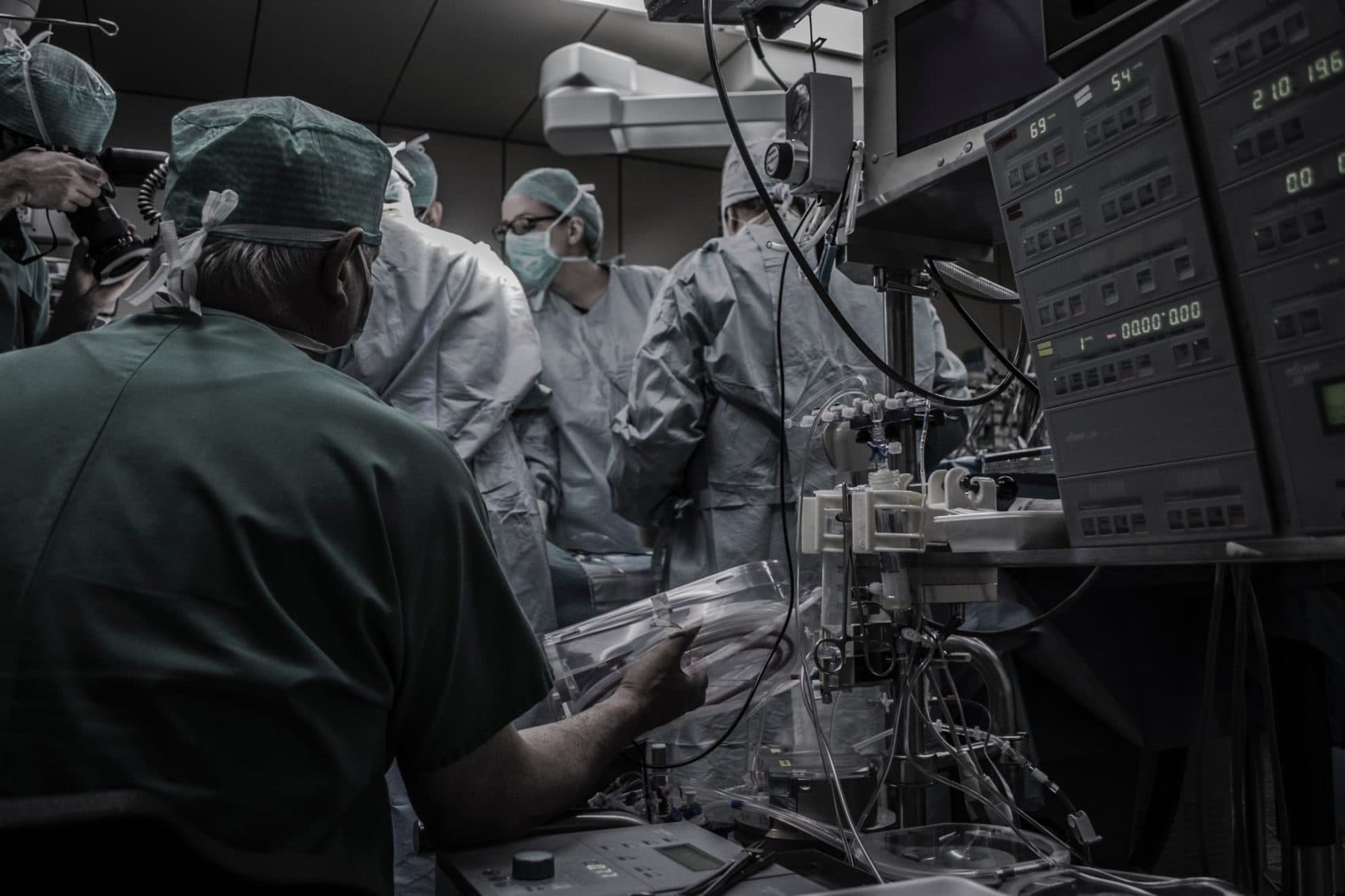
A recent article in Scientific American pondered the role that artificial intelligence may play in medicine, just as it outlined the information-overload many physicians experience. Medicine is both an art and a science. With each technological advance, we risk losing sight of the importance of the personal care that is essential to healing, and it’s clear that the best care comes from a particular alchemy of high-tech medical advances and empathetic care. Balancing the two is time-consuming and challenging, but essential for providing ideal care in the 21st century.
The month I started medical school, a beloved aunt gave me a framed print of "The Doctor" by Sir Luke Fildes, with congratulations and best wishes for my future career. Over my 25 years as a doctor, its meaning to me has changed many times. The doctor in the painting appears wise, compassionate and powerful in juxtaposition to a sick, helpless child and desperate, distraught parents. In the late 19th century, there was little to offer a critically ill child. It was a medical world almost unrecognizable today, with rudimentary and ineffectual hospitals, no antibiotics, no mechanical ventilation and diagnostic tests limited almost exclusively to a physical exam.

Fast forward to 2018, a world of extraordinary medical interventions like pacemakers, dialysis and heart transplants. Or the more common collection of blood tests, IVs, MRIs. Spend much time on a hospital ward or in an ICU, however, and you may despair of the endless testing and interventions while your doctor wrestles with the time she spends entering, synthesizing and evaluating data.
When my infant niece, Kate, was critically ill in the ICU, there were times that the doctors — the best in the world, with the ability to snatch children from death’s jaws — spent most of their time adjusting equipment, scrolling through 40 test results a day, their eyes glued to the bedside computer. But 21 days and almost $300,000 later, Kate was home and on her way to recovery. Which of those tests and tubes were unnecessary? How many of those hours analyzing lab data could have been spent sitting next to our family in quiet contemplation? Maybe some, but with my niece’s life saved, I’ll never ask and I’m not sure I care.
Medicine in the U.S. today is one of sophisticated diagnostic testing and high-tech therapies in hospitals with patient experience directors and an emphasis on shared decision making, concepts unrecognizable when Fildes’ archetypal painting was created.
Empathy is key in the doctor-patient relationship. But do we really long for the days when the doctor sat next to the bed at home? When your family member is critically ill, you want a high-tech hospital with 10 medications and 15 different diagnostic tests, if that’s what will make him well.
If our goal is to improve and save lives, medicine will not become less complicated, nor should it. If we consider our current rate of scientific discovery, it is less likely the doctor will sit at the bedside in silent and impotent contemplation, and more likely he or she will sat in the computer room down the hall.
Empathy is key in the doctor-patient relationship. But do we really long for the days when the doctor sat next to the bed at home?
At a recent medical conference, my colleagues and I heard an update on diabetes medications. The options were overwhelming, even for those of us who had cared for diabetic patients for years: over 25 options, each with its unique benefits, risks, side effects and costs. Yet none of us would wish for the days when injecting insulin was the only way to control this disease — and not a very effective one either. My colleagues and I are grateful for the therapies that allow us to provide better care for our patients, but we also realize that these advances have unintended consequences. On the fast-paced hospital floor, the medical residents and I struggle daily with the appropriate balance of talking at the bedside with the need to expedite the next diagnostic test and interpret the results from the day before.
The onus is on physicians to conduct the challenging symphony that modern medicine has become: the synthesizers of complicated scientific data and the diagnosticians who intuit just which of the 20 blood tests ordered that day hold a clue, and which is a benign incidental finding.
New therapies are miraculous, offering us opportunities to treat illnesses more safely and more easily with fewer side effects. But with the availability of disease-modifying interventions come long medication lists requiring doctors to balance carefully the risks, benefits and patient preferences. Each drug has the potential for disease improvement, but too many, especially in an elderly patient, can lead to the myriad risks of "polypharmacy."
As we long for the times when the doctor sat at the bedside, pondering whether the natural progression of the disease would take a life, let's embrace the fact that when she sits there today, the doctor performs miracles not imagined a 100 years ago, even if it means multiple tests and a computer between her and her patient.
With skill and practice, this scientifically intensive care can be provided with the wisdom, connection and compassion that is also essential.
