Support WBUR
Commentary
'Just When You Think It's Over, It Comes On Again': My Year With Long-Haul COVID

I can see it. My husband can see it. My friend, who has been running fevers since May, can see it.
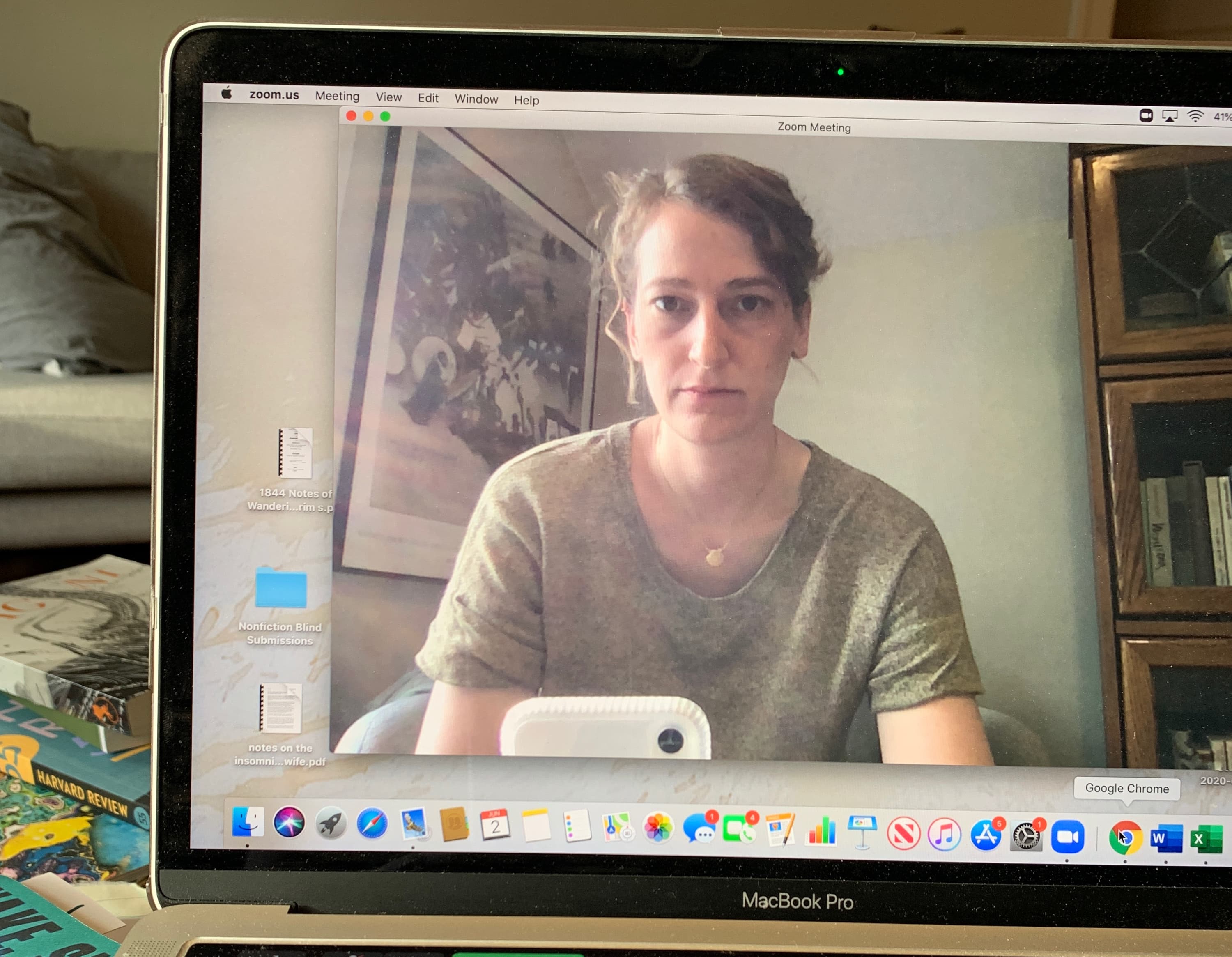
But if I were to hop on a Zoom call with you now, you probably wouldn’t notice. It’s a certain pallor washed across the face, a hollowing out that reveals itself in a delicate but deep crescent crease beneath each eye, shadows a shade of lavender that won’t show in most lighting.
The other day a coworker glimpsed it and texted, after a Zoom meeting, to check in. I’d been having a bad day: the chest compression had returned; a fog flooded my frontal cortex. As I pushed through the workday, my lungs began their telltale ache.
“How did you know?” I asked.
“You looked like you did during those first months,” she replied. “I assumed it was back.”
It had never left. Though by December we’d regained most of our energy, my husband Marc and I still experience symptoms from when we first contracted the coronavirus on a trip to India in March 2020.
At first, the disease was the whisper of a cold that could be brushed away as jet lag, in the days when there were only three reported cases in a country of 1.3 billion. Then, as if awakening with the rest of the Western world to the pandemic’s arrival, it bloomed. Marc and I were both violently ill on our flight back to the States on March 13, the day Trump declared a travel ban. We woke the following morning short of breath.
365 days later, it’s still with us.
A post-viral syndrome is a hellish disruption, even at its most minor manifestation. When the smallest spark continues to smolder, flaring and receding but never going out, over days, weeks and months, it can burn a hole right through you.
Hell is not only in this disease’s acute and fatal forms; it also exists in its small, unquantifiable losses. And in its unendingness. Just when you think it’s over, it comes on again.
Last weekend, after 20 minutes of exercise, Marc was back on the couch with body aches, a fluttering pulse and cheeks flushed with fever. I still feel echoes of the pain that sent me to the emergency room last May, a sharp stab at my lungs, a twinge at my heart. Return to exercise has been slow. I work with a physical therapist who keeps an eye on my heart rate while I pace the revolving floor of a treadmill.
Because our symptoms remain shy to the observing eye — even the X-ray vision of modern medicine can’t detect what is wrong — it took until December to get professional help. My illness couldn’t be seen by science, so the burden of proof was on my shoulders — and I couldn’t stand upright without my chest feeling as if it was caving in.
Many of the pandemic’s losses will not be visible to the outside observer. We may never know the suffering hidden behind the face next to us on a Zoom call.
The cardiologist dismissed my elevated pulse as dehydration and told me to see a psychiatrist. The infectious disease doctor refused to treat without a diagnosis, citing her Hippocratic oath but failing to see the harm she was doing by prescribing anxiety meds for symptoms that were so debilitating, Marc and I purchased a stool because we couldn’t stand at the kitchen sink long enough to wash dishes.
Stories of others with our condition had, by late summer, begun to pick up traction in the media, along with monikers like “long haulers,” a term that originated in support groups meeting by the thousands over Facebook and Slack. Yet the prevalence of a protracted post-viral response to COVID-19, symptoms that linger and flare, remained largely unrecognized until recently.
A year into our lived experience of this illness, our ongoing ailments have been legitimized by the scientific community with a name: Post Acute Sequalae of Sars-CoV2, and a number: 30%. One in three individuals continue to suffer nine months beyond an initial Covid-19 infection.
Without the work of advocacy organizations such as Body Politic — the support group I turned to when denied medical care — we might have waited much longer for this acknowledgment. From the beginning, many with prolonged symptoms stayed quietly at home, hesitant to seek help when there weren’t enough diagnostic tests or hospital beds for those gravely ill.

While the world was in triage, it was hard to complain of a mild case of COVID, even when it went on and on.
Some, I suspect, continue to stay silent because of this seeming endlessness. While the sensations hold an evergreen fascination for those afflicted — like a horror film you can’t look away from — to outsiders, their quotidian presence becomes mundane after a few mentions.
And we are silent because when it was finally OK to seek help, we were turned away. We are afraid of being discounted by the medical professionals we once trusted to help us heal.
Many of the pandemic’s losses will not be visible to the outside observer. We may never know the suffering hidden behind the face next to us on a Zoom call. As our conversations shift to vaccines and re-opening, as we emerge from a state of emergency, my hope is that those left with this lingering, life-altering condition will be seen, and will one day receive care.
Meanwhile, our bodies heal at their own private pace. With the guidance of my physical therapist, I’ve begun to increase my cardio exercise to a fast walk, charging up a slope near my house, keeping an eye on my soaring pulse as I stretch my legs in a silent, rhythmic triumph, filling damaged lungs with the cold, crisp air of late winter — the same season I left for an ill-fated trip one year ago.
