Support WBUR
Commentary
As doctors, we like to 'know.' COVID took that away

I saw them through the plate glass window as I came out of the stairwell and into the lobby. The mother stood on the sidewalk, wearing a stiff round mask that dug into the flesh of her cheeks. The baby nestled in a wrap across her chest. They were my first patients with COVID-19, and I crossed the lobby as naturally as possible in my new protective gear to welcome them.
“I was dressed exactly like that when I got COVID,” she said, looking me up and down. “It isn’t enough.”
For a moment I was glad my expression was covered. Then I reminded myself of the reasons she was mistaken. These were the days, after all, when my doctoring still rested on deep wells of certainty — the days before COVID took that away.
I had donned my PPE for the first time that morning, reciting the steps as I covered my body parts one by one. Then I had walked, fully cloaked, through the length of our building to escort them in. Families in the waiting area, the security guard at his desk, a couple coming out of the stairwell — they all looked at me with wide eyes, full of fear. It was March 2020 and I may as well have been carrying a sign announcing COVID IS HERE.
In the previous weeks, my colleagues and I had scrambled to dismantle and reconfigure the pediatric practice we had built over 22 years. We erased our schedules, rearranged exam rooms and set up isolation areas. We turned to our most trusted health care agencies for guidance, but they seemed equally harried. The moment the Centers for Disease Control suggested we wear bandanas if we ran out of masks was the moment I understood: We were on our own.
These were the days, after all, when my doctoring still rested on deep wells of certainty -- the days before COVID took that away.
It wasn’t the fear that undid me most. Fear is a thing I have faced before. What was new and ominous and far more unsettling was caring for others with so much uncertainty.
On our way to the office, the mother explained she was a nurse at a nearby hospital and had tested positive a week or so earlier. Now her son was having symptoms. Her chest rose and fell in labored breaths, and my mind cleared in the particular way it does when focused on what I can do for another person. I showed her to the exam room and supported her elbow as she settled into a chair. Then I shut the door behind us, to keep COVID in.
The visit proceeded with a tension I came to know well in the coming weeks. I wrestled with occupying the role of caretaker — same voice, same posture, same listening and guiding — but without the foundation of knowledge I had always relied on. I offered what guidance I could, always adding the caveat, “Of course, there’s so much we don’t yet understand.”
As physicians, we’re accustomed to embracing what we do not know and researching the best way forward. But when COVID arrived, the data was scant and conflicting. No amount of digging yielded answers we could comfortably rest on. While experts debated the definition of exposure, which symptoms merited testing and whether the virus lived on surfaces or in air, we stepped in and out of exam rooms, determined to provide the best possible care with the information we had. Or at least, to do no harm.
In our new reality, the “what ifs” hung in the air. Unanswerable. Haunting.
We canceled well visits and told parents to keep sick children home, because the care that normally defined our work was deemed no longer essential. But wasn’t it? We worried the care we delayed — immunizations and dental treatment and developmental therapies — might have long-term implications we could never take back. We feared the limp we evaluated by video screen might be cancer or the bellyache could be appendicitis.
Physicians are trained to rest our practice on tried and true evidence. In our new reality, the “what ifs” hung in the air. Unanswerable. Haunting.
There can be magic in the exam room, a connection that fills the space. It starts with a provider who combines wisdom with empathy and results in a patient who feels truly cared for. Reaching this doctoring place has been the source of my greatest strength and pride. Living it is my nourishment. Losing it made my blood run cold.
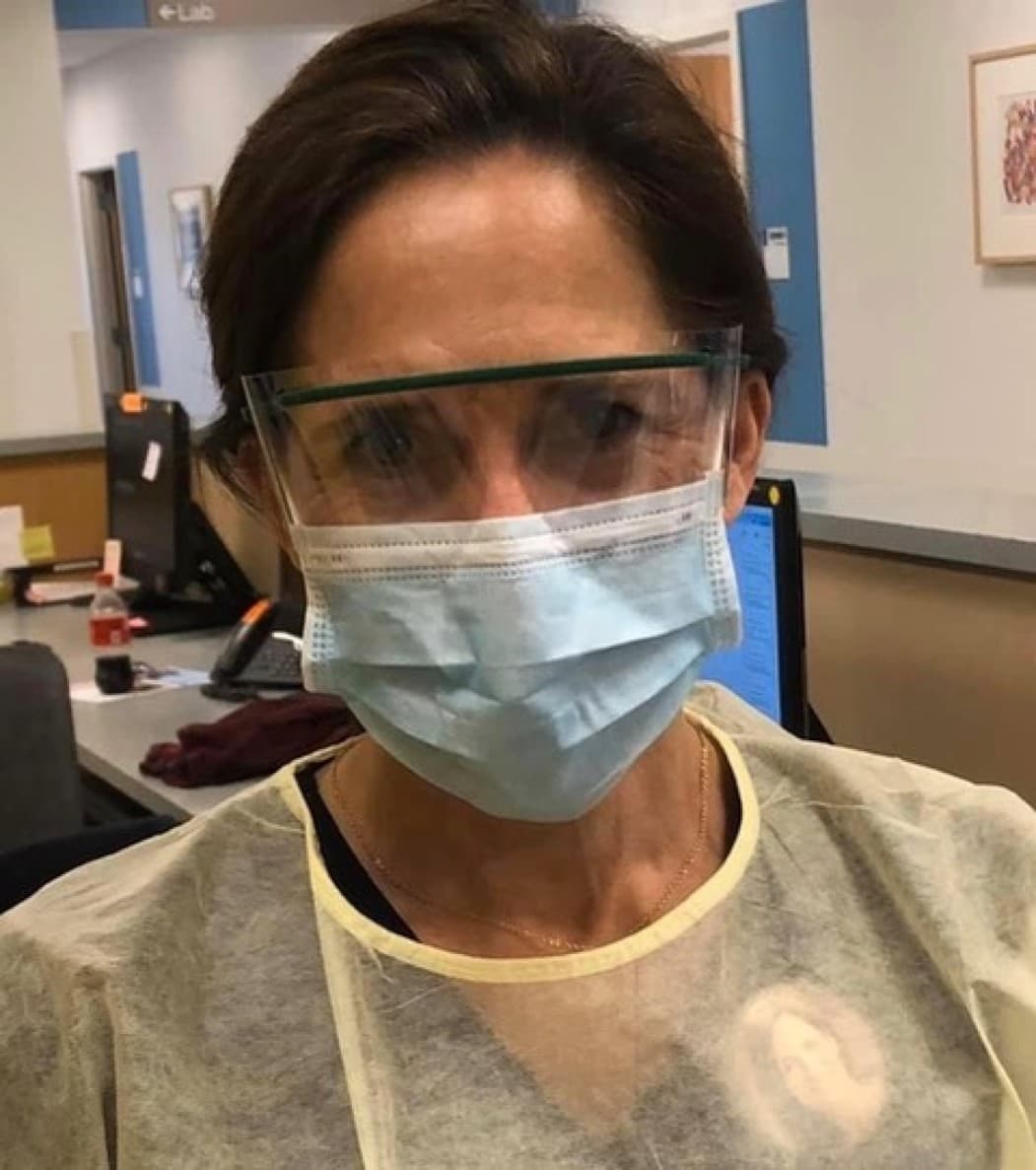
As COVID set in, I had all of the empathy but nothing that felt like wisdom.
The solution, I knew, would be in learning. I poured over research from around the world and compared notes with infectious disease colleagues and public health friends. As the science grew and expert opinions began to converge, not every scenario was a new puzzle with no apparent answers. We were finding our way.
It helped, too, that as time went on I began to feel safer. If I could remove children’s masks and peer in their throats, if I could thread swabs up their noses while they coughed on my goggles and mask — if I could do this without getting sick, it must mean I could trust my understanding and counsel others with clarity.
I stepped more firmly than ever into my purpose. Because I had fought for it, and because the need was so great. For nine months I stood tall in that doctoring place, doctoring COVID.
Then one night an ache crept into my back and thighs, and my pulse began to quicken. I had the virus and I had it good. Over the next 10 days, I felt gradually liquefied.
It wasn’t the weakness that sobered me most. It wasn’t my oxygen drifting lower or my temperature climbing higher. It wasn’t even the one time I showered, with the hope I could rally, and realizing I couldn’t. Couldn’t breathe that thick air, couldn’t stop coughing.
It was the feeling I had failed. Getting COVID was like falling off a pedestal I had built stone by stone. For others, when COVID acted unexpectedly, I was able to say “This virus works in mysterious ways.” But not for myself.
If COVID-19 was the earthquake, these new unknowns are aftershocks.
The disbelief as the fever set in. The shock of being so terribly ill. The guilt that I had sickened the ones I love most in the world.
I sickened. Them.
My husband. My daughter (my light, my baby, the whole of my heart). A friend in crisis I had traveled to visit. I lay in a heap as they all fell ill. Unable to fathom the truth of it all, that I was the cause.
When I returned to work, all I could sense was COVID, waiting to descend on my patients and colleagues in ways we couldn’t know.
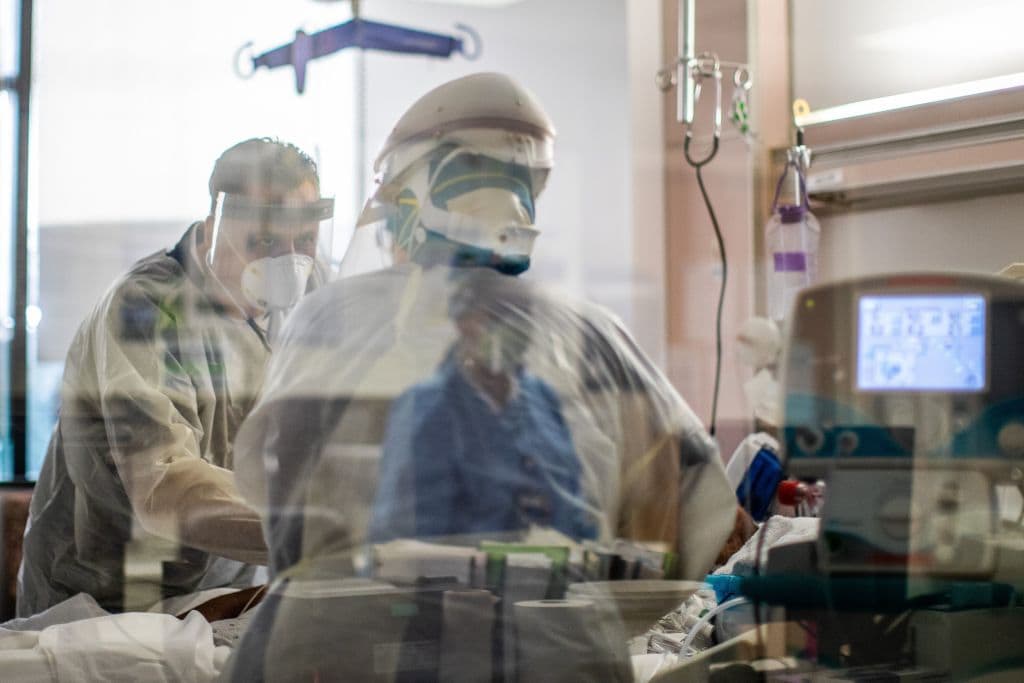
Ten months have passed since I got sick, and I’m far more myself. It took some time for the ground to feel steady under my feet. But now delta is raging just as schools have opened. Immunity may or not be waning. Questions abound. We’re guiding patients as best as we can, while we wait for the science to catch up. If COVID-19 was the earthquake, these new unknowns are aftershocks.
When they started I thought, I can’t. I thought about leaving for mountains and lakes and faraway places.
But it turns out, I can. The baby in his swaddle is now a teetering toddler and his mother is well. I still say to my patients, “There’s so much we don’t understand,” except it no longer feels like I’m wrestling. Because this time, I’m allowing uncertainty in. It’s a different sort of doctoring, this place where the ground keeps on trembling. But it’s still my place.
It turns out that even without so much knowing, there’s plenty of care we can give.
Identifying details have been changed to protect patient privacy.
