Advertisement
Study: Persistent Yeast Infections Can Trigger Chronic Vaginal Pain
Melissa Farmer, a pain researcher at McGill University, reports in a new paper that persistent yeast infections in mice can lead to chronic vaginal pain, in fact, the same type of pain that human females experience when suffering from a condition known as vulvodynia, chronic pain of the vulva.
Up to 14 million women in the U.S. have vulvodynia at some point in their lives, according to The National Institutes of Health. Characterized by a burning, cutting or raw sensation in response to light touch or intercourse, the condition often goes undiagnosed.
Farmer simulated a vulvodynia-like state in mice by exposing them to a series of three yeast infections. (Specifically, she put the mice to sleep and then pipetted 20 microliters of yeast in saline solution into their vaginal cavities to induce a severe infection.
Later, she treated the mice with oral fluconozole, familiar to any woman who has had a yeast infection.) After the third infection, 6 out 15 mice became hypersensitive to touch, to the point where they jumped from pain.
Farmer's study, published in the journal Science Translational Medicine found that after three rounds of infection and treatment, there were some lasting changes in the mouse's body:
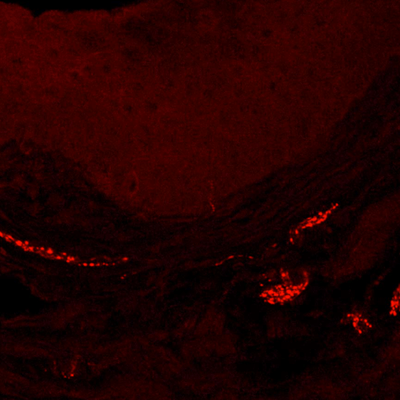
Although the vulvar skin of hypersensitive mice looked normal, a closer inspection revealed that affected mice had more sensory nerve fibers compared with the vulvas of unaffected mic e. The results hint that recurrent yeast infections spurs the production of more nerve fibers in some individuals; and this increase in nerve fibers may be the cause of the chronic pain in some women with vulvodynia.
The researchers conclude:
The hypersensitivity and hyperinnervation were both present at least 3 weeks after the resolution of infection and inflammation. Our data show that infection can cause persistent pain long after its resolution and that recurrent yeast infection replicates important features of human provoked vulvodynia in the mouse.
Farmer, the study's lead author, has been examining the phenomenon of genital pain for some time. In fact, she told me she just completed her Ph.D. on the the sex lives of male and female mice who experience pelvic pain (more on that later). But how, exactly, does she measure vaginal pain in a mouse?
To test hypersensitivity in this experiment, she said: "I used a calibrated, plasic filament — a hairlike fiber — and using different amounts of pressure I gently pressed against the posterior part of the vulva and looked for the presence of a quick reflexive jump. The jump I was looking at was almost involuntary — that's how I determined which mice were in pain."
In the thrice infected mice, Farmer said: "There was a significant reduction in what it took to trigger pain."
Of course, it's important to note that this is a small study in mice, and that not all the mice developed pain after three infections (just like not all women do). Still, Farmer says, the take home message is that women who are prone to yeast infections should probably seek "early, aggressive" treatment.
Personally, I could totally related to these poor, yeast-infected mice. It's kind of what happened to me a few summers ago — a couple of bad yeast infections led to chronic pain, and ultimately a series of posts on pelvic pain during sex and how to treat it. If you don't want to read my whole saga, I'll just tell you this: I had a far better outcome than my afflicted rodent comrades.
This program aired on September 21, 2011. The audio for this program is not available.
