Support WBUR
What You Should Know About Using Naloxone
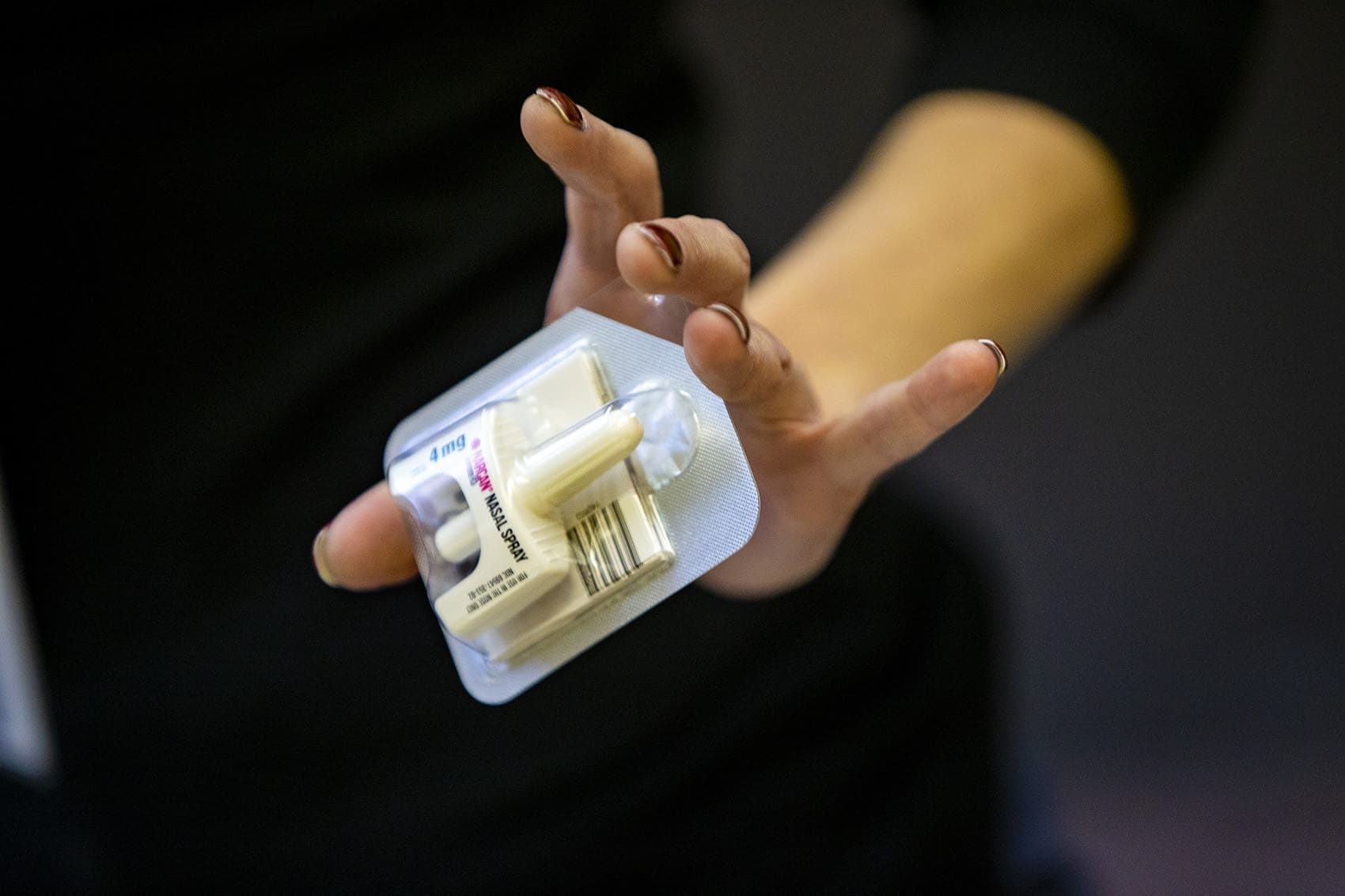
Christmas. A time for gifting sweaters, books, board games, tech gadgets … and the opioid overdose reversal drug Narcan? This happened at my Christmas celebration last month.
The person who gave Narcan didn’t explicitly say, “Merry Christmas! Save a life!” but that was the sentiment. And why not? There are billboards and posters from public health campaigns all over imploring you to get it, and the media is full of stories about people on the brink of death who were revived by it.
“How do I use it?” the recipient asked, turning the white box over in her hands.
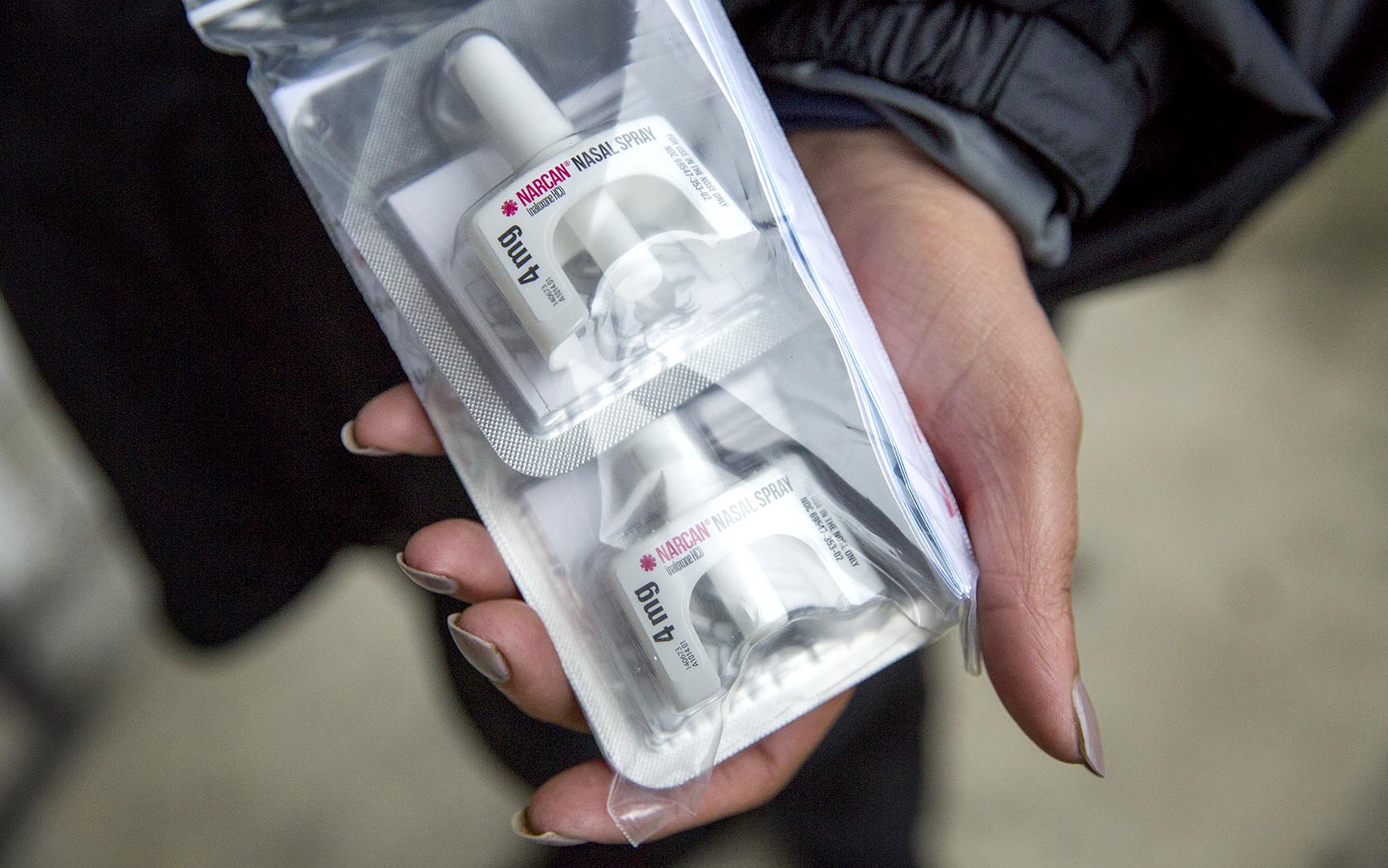
Narcan, the most common brand of the opioid overdose reversal drug naloxone, works by temporarily bonding to the brain’s opioid receptors and blocking the effects of opioid molecules.
It's been around since the 1960s, and was traditionally given intravenously. These days, it can be administered through a simple spray into one nostril.
Approximately 3 million doses of Narcan have been distributed in the U.S. since 2016, according to Adapt Pharma, the company that makes it.
Contrary to what you might have heard, naloxone does require a prescription, but in states like Massachusetts, a standing order makes it available to everyone. This means that you can walk into most major pharmacies and obtain it. (Depending on your health insurance plan, part or all of the cost may be covered.)
OK, so you’ve seen the public health campaigns about naloxone, and maybe you've decided to carry it. Now what?
Opening a package of Narcan and pushing a button to shoot mist up someone’s nose is fairly straightforward. It’s everything else that feels sort of tricky, right?
Should everyone carry naloxone? How long does it take it to work? Can you mess it up? Do people wake up agitated or even violent? And perhaps most importantly, how do you even know if someone is overdosing and needs it?
Who Should Carry Naloxone?
There’s no hard and fast answer to this. According to U.S. Surgeon General Jerome Adams, “for patients currently taking high doses of opioids as prescribed for pain, individuals misusing prescription opioids, individuals using illicit opioids such as heroin or fentanyl, health care practitioners, family and friends of people who have an opioid use disorder, and community members who come into contact with people at risk for opioid overdose, knowing how to use naloxone and keeping it within reach can save a life.”
Given the widespread nature of the opioid epidemic, nearly everyone I spoke with agreed that having more people carry Narcan — or having it publicly available through lock boxes or in First Aid kits — could only help.
How Do I Know If Someone Has Overdosed On Opioids?
A person under the influence of opioids often looks sleepy. Their facial muscles might be slackened, and they might have trouble standing up straight, says Amy Delaney, program manager for the Boston Public Health Commission's harm reduction team, and the leader of a free Narcan training session I attended.
Discerning whether a person has overdosed and needs naloxone isn’t always immediately apparent.
“If I come up on someone and they look very sedated — so chin on the chest, slumped over — it could potentially be an opioid overdose,” she says. “The first thing you’re going to look for is breathing.”
If the person isn’t breathing, or is breathing at an abnormally slow or irregular rate, you have a medical emergency and need to call 911.
Other telltale signs of an opioid overdose include grayish or pale skin, blue lips or fingertips and nail beds, abnormally small pupils, and loss of consciousness or an inability to wake up.
Contrary to popular belief, opioid overdoses aren’t always immediate, Delaney says. A lot of people nod off slowly and don’t cross into the realm of overdose for a half hour or more.
But fentanyl has been a game changer.
“It’s far more potent and lethal than heroin has ever been, and has a very rapid onset, so it can change the way an overdose looks,” she says.
She tells a story about a man who had been clean for "an extensive period of time" and came into the Health Commission building to access further services, but ended up using in the bathroom.
"When he came out of the bathroom, he looked OK. He maintained eye contact with staff — we were like, 'Hey, are you all right?' All of a sudden his whole body seized up," she says, making a gasping noise and scrunching up her body.
"His hands went to claws, and he just dropped."
To Delaney, it was clear that this man had used fentanyl because he had what's called "wooden chest syndrome." When this happens, the muscles in the chest cavity seize up and become rigid.
The man went from "walking and talking to rigid and purple in less than a minute," she says. "It's a lot more traumatic and violent looking than one would expect from an opioid overdose," but you should be aware that this is what you're seeing should you come across it.
I’m Fairly Certain That Someone Has Overdosed On Opioids. What Do I Do Now?
First, ask if they’re OK. If the person doesn’t respond, you could try a gentle shake on the arm. (Again, if the person isn’t breathing, call 911.)
If that doesn’t work, try rubbing your knuckles up and down their sternum. A sternal rub, Delaney explains, is the most painful thing you can do to someone that won’t harm them. If the person still isn’t responding, it may be time for Narcan.
If the person has a pulse, but isn’t breathing regularly — or at all — the best thing you can do after giving Narcan is rescue breathing.
The brain starts to die after a few minutes without oxygen, so rescue breathing “can be the difference between life and death. And brain health,” Delaney says. “We talk a lot about overdose fatalities, but what doesn’t get talked about a lot is all of the kids who are in [traumatic brain injury] homes as a direct result of overdoses.”
If the thought of putting your mouth on a stranger’s mouth makes you uncomfortable, she says you can use fabric, like the bottom of your tee-shirt, as a barrier between your mouth and the other person's mouth.
Is Narcan Really That Easy To Administer? Can I Mess It Up?
The short answer is yes, it’s really that easy to administer, and no, you can’t really mess it up. With the Narcan nasal spray, you don’t have to worry about dosing because all 4 milligrams will be released at once. And unless someone is allergic to naloxone or another component in the spray, it’s essentially harmless.
“I cannot stress enough that the worst thing that happens is you give someone a wet nose,” Delaney says.
It’s worth reiterating that naloxone only works on opioids. If someone has passed out from alcohol, naloxone won’t do anything to help them. Similarly, if someone has mixed an opioid with another drug, naloxone will only reverse the effects of the opioid.
How Long Does It Take To Work?
Because every overdose is different, this question is hard to answer. Generally, the nasal spray takes a three to five minutes to work, experts say, so don’t worry if the person doesn’t respond immediately.
“Nasal naloxone is not the fastest or most effective version of this medication, it’s just the most palatable to the general public,” Delaney says. An intravenous or intramuscular injection of naloxone works a lot faster than the nasal spray because the mist has to pass through the membranes of your nasal cavity before it enters the bloodstream.
This slower absorption can be a good thing. People receiving it aren’t thrust into withdrawal as quickly, and can wake up in a slower, more incremental way.

What If The Person Isn’t Waking Up? Should I Give A Second Dose?
A lot of people worry when someone doesn’t immediately wake up from Narcan, says Jeremy Walsh, paramedic coordinator for the Cambridge Fire Department.
“Our paramedics get on scene sometimes and there will be three or four empty boxes of Narcan on the floor because they just gave them in rapid succession.”
He advises people wait three-to-five minutes before administering a second dose up the other nostril.
“There are a lot of people who give people four or five doses of this very expensive medication. And they do it out of fear. They panic — more is better, get it in — but that’s not the way this medication is supposed to work. It’s supposed to bring people back gently so that they get medical care,” Delaney says.
“If someone is not coming to after several doses, and six to eight minutes, we can assume one, that the person has passed on; two, the drug that they overdosed on may not be an opioid; or three, that the opioid that they got was just so strong that we need more naloxone," Delaney says.
Hopefully by this point, she adds, emergency responders will be on the scene.
Is It True That Some People Wake Up Agitated And Violent?
People wake up in a variety of ways, Delaney says. She’s seen people who start breathing but don’t regain consciousness for a while, while others open their eyes and are verbal or standing in a few minutes.
She knows we may have heard stories about people waking up in the throes of withdrawal and yelling, vomiting or even becoming violent, but says those fears are overblown.
“I can tell you after over a decade of responding, I’ve never had someone be violent. I’ve never had anyone be sick," she says. "What makes people agitated or uncomfortable is if they’ve been given too much of this medication too quickly, or if when they come to, people are yelling in uniforms standing over them."
You shouldn’t expect anyone to thank you for giving them naloxone, she says, but if you create a calm environment, you probably don’t need to worry about a negative reaction.
Walsh, of the fire department, agrees.
“It used to be a common thing where we’d say, ‘Oh yeah, they’re going to wake up and you’re ruining their high, and they’re going to be mad at you.’ Or you send them into withdrawals because you do it too quickly.”
Naloxone that’s administered through an IV too quickly can precipitate withdrawal, which makes people wake up faster and feel sicker, but with the advent of the nasal spray, this hardly ever happens, he says.
(WHYY's Nina Feldman found that some people do get annoyed, so be prepared for that possibility.)
But of more pressing concern is the fact that Narcan starts to wear off after 30 to 90 minutes, Delaney says. This means that a person can slip back into overdose without the proper medical attention.
If someone regains consciousness before emergency responders arrive, you should explain to the person “that they just experienced an overdose, you just administered Narcan, and that the Narcan is going to wear off, so they can’t go off and be alone," she says. People might refuse to wait for first responders, she adds, “but it’s important as bystanders to inform them that they’re at much higher risk if they don’t get medical monitoring.”
Am I Putting Myself Or The Other Person In Legal Jeopardy By Intervening?
The short answer is no.
"Every state has some kind of general good Samaritan law that protects bystanders who render emergency aid in good faith," says Corey Davis, deputy director at the Network for Public Health Law. "We've never heard of anybody anywhere ever being sued for administering naloxone in what they believed to be an overdose emergency."
He adds that you shouldn't feel compelled to intervene in a situation that makes you feel unsafe.
"In the United States, you have no legal responsibility to render aid to anybody," Davis says. "So there's no legal liability if you walk by."
As for the person overdosing, everyone I spoke with said that you shouldn't let fears about the person getting in trouble for drugs stop you from saving a life. Every jurisdiction operates differently, but when I spoke with Jeremy Warnick of the Cambridge Police Department, he said his department's priority is connecting drug users with addiction services.
"They're not going to come out of their overdose and be put into jail, at least here in Cambridge," he said. "We're not going to arrest our way out of this."
Final Takeaway
Almost everyone I spoke with said that while they applaud anyone willing to use naloxone to save a life, no one should do so at the expense of common sense or personal safety.
“You have to go with your gut instinct and what you think is right. If you want to help, you help. But obviously staying in a bad situation may not be the best thing to do,” Walsh of the fire department says. "And if you’re going to give Narcan, you can give it, and you don’t have to stay on scene if you feel like you’re unsafe. Call 911 and get to a safer area."
Bottom line, whether you got Narcan for Christmas or are thinking about getting it, taking a training class offered by the state or your local health department is probably one of the best things you can do to prepare.

