Support WBUR
Coronavirus Coverage
‘Second Toll’: Study Finds Heart Disease Deaths Shot Up In Early Pandemic, But Not In Mass.
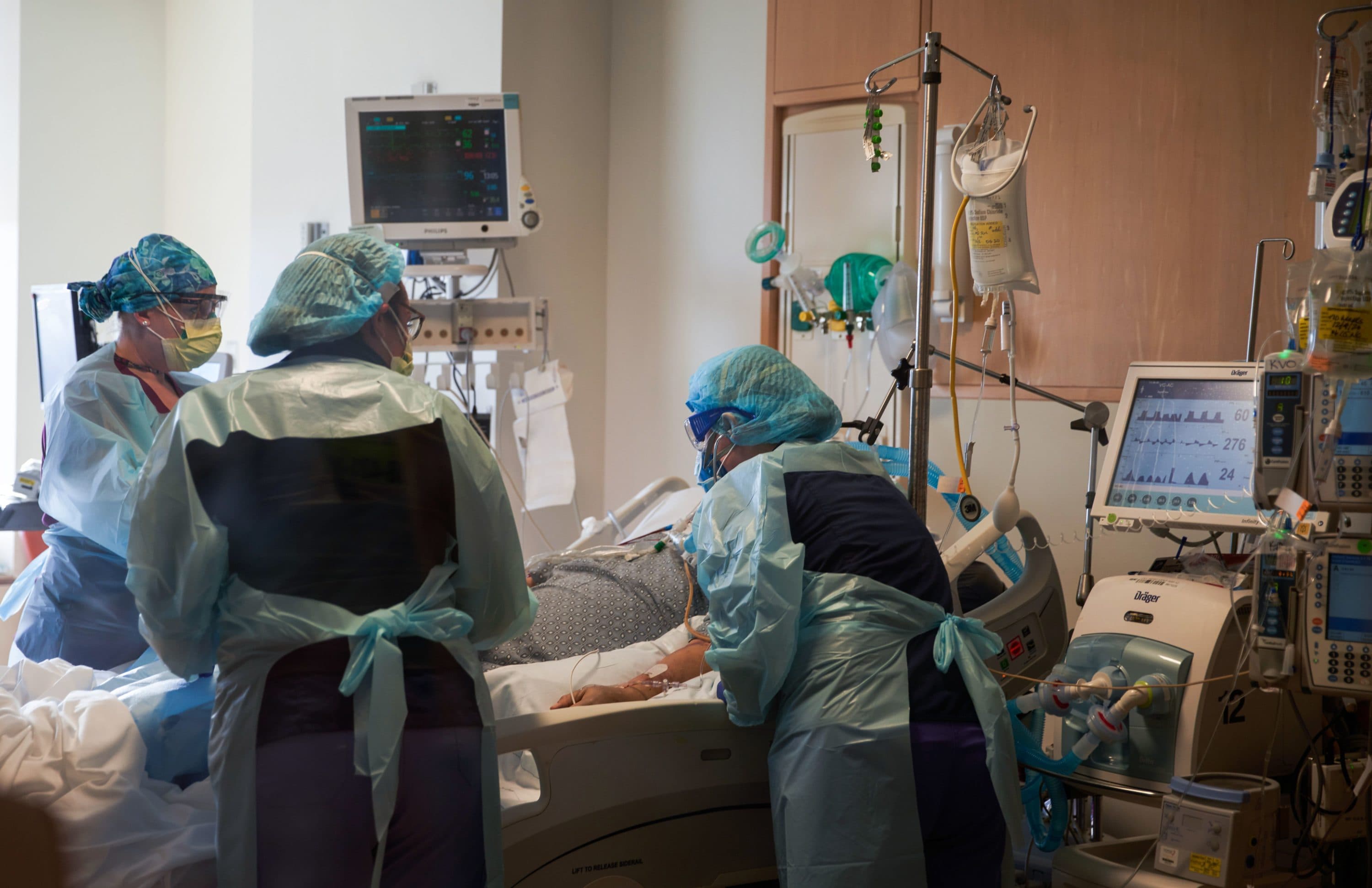
Amid the COVID-19 surge last spring, Massachusetts officials and hospital leaders begged patients not to delay urgent care for other medical issues out of fear of the virus. Delay carried a danger of its own, they warned: a potential “second toll” of pandemic deaths from causes other than COVID.
In some early hot-spots, that second toll was high indeed, according to a new study of tens of thousands of deaths by Beth Israel Deaconess Medical Center researchers .
In New York City this spring, heart disease deaths more than doubled, the study in the Journal of the American College of Cardiology finds. Nationally, heart-related deaths rose by 11% compared to the same three-month period the year before. Deaths from complications of high blood pressure rose 17%.
But Massachusetts and Louisiana were spared.
Why? It’s possible, says lead author Dr. Rishi Wadhera, that though Massachusetts was hit very hard in the spring surge, it fared better because its hospital system did have a bit more time to prepare than, say, New York City’s.
At the same time, he says, Massachusetts patients “who really, really needed care for non-COVID-19 illnesses probably still came in to the hospital, because our public health messaging really consistently encouraged patients with emergent conditions to seek care.”
The findings, he says, seem to highlight how important it is for public health leaders to broadcast the message that hospitals are still safe places to receive care, and that delay — for example, for chest pain that could be a heart attack — is dangerous.
The paper’s numbers on non-COVID heart deaths jibe well with other studies so far, says Dr. Anupam Jena of Harvard and Mass. General Hospital, who was not involved.
“We know from lots of other work that delays in cardiac care can increase mortality,” he says. The stress of the pandemic, including job loss, could also hurt patients: “There’s a lot of good evidence that cardiac conditions like heart attacks do respond to stressful events.”
And if hospitals are stretched too thin, that can affect care, he says, though in large cities and major hospitals, there has generally still been “sufficient bandwidth” to address emergencies.
To the extent medical care, rather than patient hesitation, has led to additional deaths, factors could include the cancellation of outpatient visits as well as delays in prescriptions and diagnostic testing, the paper suggests.
Also, delays in “semi-elective procedures” — for example, replacing a defective heart valve that limits blood flow — could play a role.
The research focused only on non-COVID-19 deaths, but it’s possible that patients had the virus and remained undiagnosed.
The higher death rates tend to correlate with areas that were overwhelmed by outbreaks with astronomical coronavirus rates, says Dr. Jeremy Faust of Brigham and Women's Hospital, who edits the coronavirus newsletter Brief19.
He argues that the main driver of the additional deaths is likely to be deaths that were classified as caused by heart disease but were actually due to COVID.
Dr. Faust accepts the additional deaths calculated in the paper, he says, but believes "mostly it's because of either a direct effect of COVID-19 — a complication in the heart — or that it was basically blamed on heart disease because there's nothing else to blame when a 70-year-old person dies at home. The most common reason for that is cardiovascular disease. So if you don't have any other reason, then that's what you blame it on."
Such mis-classifications would not occur in Massachusetts, Dr. Faust says, because the health care system never became overwhelmed.
Whatever the main drivers of the rise, the message for patients is clear, Dr. Jena says: “If you are having an acute medical problem like chest pain, like shortness of breath, then you’ve got to get medical care immediately.”
Dr. Wadhera offers added reassurance about anti-virus protection in medical settings.
“I think the health care systems, specifically in Massachusetts, are even better prepared than they were early in the pandemic to take care of patients with COVID-19,” he says, “and also to take care of patients with other medical conditions.”
Overall, Dr. Jena says, about 2.8 million Americans normally die each year from all causes. Deaths have already risen by about 10% during the pandemic.
Extrapolating the numbers from studies so far, he says, the pandemic’s “second toll” could involve up to 8,000 additional deaths from heart disease and up to 30,000 additional deaths overall from non-COVID causes. But of course, he says, “the vast majority are going to be from COVID-19.”
Dr. Faust from Brigham and Women's offers additional reassurance: the Massachusetts health care system, despite the current surge and its pause on elective procedures, does not have to turn away any patients with urgent medical issues — for now. That makes controlling the surge all the more urgent, he says.
"We're not there, and I don't want to get there," he says. "So the message is that we still can treat everyone's emergencies, but we don't want to get to a point where that's not the case."

