Support WBUR
When You Think It Might Be Lyme Disease
Note: At the bottom of this post are a general guide to early Lyme Disease treatment and five pieces of official advice.
All that week, I was agitated, unquiet. I felt like the nun in "Madeline", the children's book: "In the middle of the night, Miss Clavell turned on her light and said, 'Something is not right!'"
Tully, my 6-year-old son, had been bitten by a tick over Memorial Day weekend, but we didn't find the loathsome thing until two days later, engorged and dug in on the milky-smooth skin just above his navel.
That discovery led to a quandary that many thousands of us who venture outside in Lyme-infested regions from Massachusetts to parts of the mid-Atlantic, Midwest and northern California may face: If you think it's Lyme Disease but you're not sure, do you err on the side of antibiotics? When is that appropriate? What if it's not appropriate but you still want to do it?
Here's our recent saga, and though evidence of resurgent tick populations remains no more than anecdotal at this point, it’s the kind of story likely to arise more often this year than last. The recent wet weather is just dandy for the deer ticks that carry Lyme Disease.
Lyme Disease tends to peak twice during warm weather, Massachusetts state public health veterinarian Dr. Catherine Brown said: from late May through June and possibly into July, as the tiny, hard-to-spot young "nymph" ticks sneak onto us; and from August into September, as the bigger adult ticks attack.
[module align="right" width="half" type="pull-quote"]
Dr. Jonathan Edlow: 'It’s important for patients and parents and physicians to recognize that Lyme Disease can present with just a fever and no rash.'
[/module]
Last year's hot weather appeared to keep ticks in check, but she expects this year to be back to typical levels, which average 4,000 reports statewide of Lyme Disease and a great many other cases that go unreported.
When we found Tully's tick, I called our pediatrician's office, knowing that the 48 hours it had been on him was enough time to transmit Lyme Disease. But the nurse said just to wait and see if he developed any symptoms.
A few days later, he did: low-grade fever, occasional nausea and on-and-off headaches that lasted a full week. And the illness had an odd pattern that I called "malarial": instead of simply getting better, he was up and down, improving but with occasional brief morning episodes of chills or headache.
I brought him in to be checked when his fever first spiked, hoping he could just start on antibiotics, as he did a couple of years ago when he had Lyme Disease then. But the doctor said the red area around the tick bite did not resemble the classic "bullseye" rash — a ring of red around a clear middle — so we should continue to wait and see.
We waited, but nothing became clearer except that when you mention the possibility of Lyme Disease to people, you get horror stories back. A man on Cape Cod whose face is now half-paralyzed. A girl who contracted it at 6 and has had brain problems ever since. Joint pain. Generalized pain. Recurrent fevers.
Never in my nearly ten years of parenting have I been this kind of mother, but in my growing alarm, I verged on calling the doctor to demand, "Just put my son on the [deleted] antibiotics!"
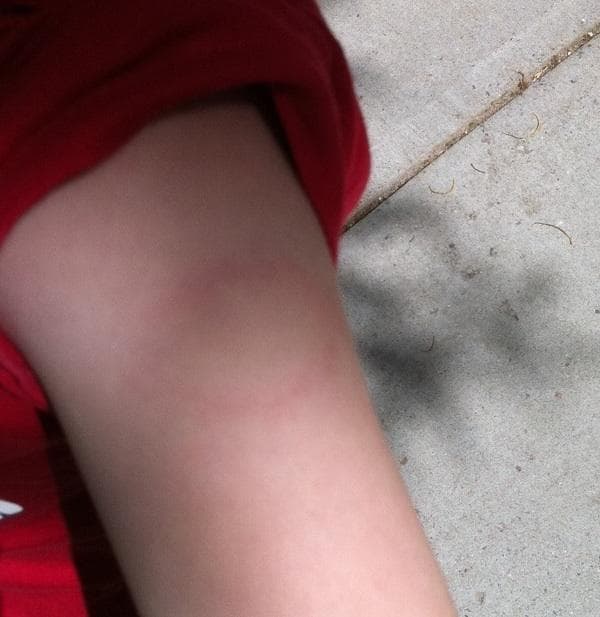
I was saved by the bullseye. On Sunday, I was pulling off Tully's shirt and saw the ring-like mark above on his arm. I took that photo and sent it to the doctor on call, and he said instantly, "That's Lyme Disease," and phoned in the prescription for antibiotics.
But the question lingers for me: Why, when the disease is so notoriously tricky to identify, and the possible consequences of missing the diagnosis so devastating, would you not want to err on the side of antibiotics? Why not prescribe them if there's even a modicum of doubt?
I asked the state's Dr. Catherine Brown. It’s a complicated issue, she said, and she’s always very careful to respect the authority of a treating physician. That said, we tend to “fall back on national guidelines that have been put together by panels of experts. And if you read those guidelines, what happened with your son actually follows those guidelines exactly.”
[module align="right" width="half" type="pull-quote"]
My late-night wonderings: What if the doctors had continued to refuse to prescribe Tully antibiotics, even though I knew in my maternal bones he had Lyme Disease?
[/module]
In adults, she said, if you’re in an area where Lyme Disease is considered endemic — like Massachusetts — and you know the tick has been on you at least 24 hours, there are recommendations to consider a single dose of preventive antibiotics, to stop Lyme Disease from developing. But there are no such recommendations for children.
Why not? “I think it has to do with the preponderance of antibiotics that children are faced with,” she said, “and there is increasing recognition of the harm that overprescribing antibiotics can cause — not just on an individual level but on a population level.”
I get that. I’m well aware of concerns that overuse of antibiotics is leading to strains of resistant “super-bugs.” I’ve never asked for antibiotics for usual winter coughs and flu. But the remote public threat of super-bugs paled next to the more immediate threat of my son with neurological impairment from untreated Lyme Disease. So much for good citizenship.
Catherine adjusted my attitude with some more facts. Even where Lyme Disease is endemic, she said, the number of ticks actually infected is small, and even if attached for long enough, they might not transmit the disease.
From a public health standpoint, she said, mine was actually a happy story: We found the tick. We knew what to watch for. The doctor waited for confirmation and then treated. “In many ways, this is really what we want people to do, is to be aware,” she said.
“The target message is: Not only should you be aware if you find a tick on you. If you spend time outdoors and you develop flu-like symptoms over the summer, you probably should call your physician and ask about it.” There should be “a high index of suspicion.”
There are tests for Lyme Disease, but they cannot return meaningful results until at least two or three weeks after the tick bite, and even then have to be used only as part of a total picture that includes symptoms.
Our pediatrician had been planning to test Tully, but I still can't see this as a happy story. My late-night wonderings: What if the doctors had continued to refuse to prescribe Tully antibiotics, even though I knew in my maternal bones he had Lyme Disease? I asked Catherine: Is it ever appropriate to push for antibiotics?
If people are concerned about the treatment they’re getting, she said, “I suggest they seek a second opinion or, if it’s about Lyme Disease, they can go to an Infectious Disease specialist. It’s really important that you’re comfortable with the medical care you’re receiving.”
It’s a little late, but I did just seek a second opinion. I spoke to Dr. Jonathan Edlow, vice chair of emergency medicine at Beth Israel Deaconess Medical Center. He’s the author of “Bull’s Eye: Unraveling the Medical Mystery of Lyme Disease,” and most recently, “The Deadly Dinner Party,” a collection of true medical detective stories.
He walked me through the decision points in Tully’s case in a highly instructive way, but first, my bottom line: It is worth seeking a second opinion. Because unlike our pediatrician, he would have treated Tully with antibiotics on the basis of the prolonged tick bite and the odd summer fever, even without a classic bullseye rash.
First of all, he said, yes, if an adult is bitten by a tick in New England and the tick has been attached for at least 24 hours, most doctors will give a single dose of antibiotics to prevent Lyme Disease.
That has been shown to work in adults, but no studies of single-dose prevention have been published on children. Studies in children have shown that ten days of antibiotics works, he added, so one practical compromise he often uses is to give a child three days of preventive antibiotics.
So Jonathan would have considered a three-day preventive dose of antibiotics for Tully when we found the tick. Now to the next decision point, when the fever appeared.
“It’s important for patients and parents and physicians to recognize that Lyme Disease can present with just a fever and no rash,” he said. “So my position, if you had seen me on that day — ‘My child’s been bitten by a tick, he now has a fever’ — if I looked at him and saw no ear infection, no strep throat, and the lungs were clear, I would have treated him for Lyme Disease.”
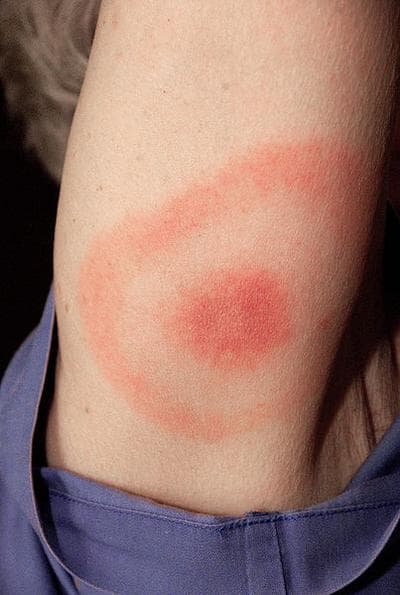
Also, he said, if Tully had a rash but not a classic bullseye, “I still would have treated him for Lyme Disease, because only — and this is an important figure — only 40 percent” of Lyme Disease rashes “have that classic central clearing, that target bullseye appearance, and just having a big red rash with no central clearing is more common.”
By the time Tully’s bullseye rash finally appeared, Jonathan said, “a medical student could make that diagnosis.”
So, I asked, was our pediatrician just being conservative? Arguably, Jonathan replied, his own willingness to set a lower bar for antibiotic treatment is the more conservative course.
True, he said, the overuse of antibiotics is a huge problem because of cost, because of allergic reactions and side effects, and because of resistant bacteria. But that said, the antibiotics used for Lyme Disease — mainly amoxicillin and doxycyline — “are relatively old-school, inexpensive and very unlikely to have a major effect on the global antibiotic resistance patterns. And in addition to that, the earlier you treat anything, the easier it is to treat.”
It comes down to common sense, Jonathan said. What’s the downside of treating a child with ten days of antibiotics? “It’s not that big of a deal.” But of course you wouldn’t want to lower your bar too far, and start giving antibiotics to any children who have non-specific symptoms such as headaches and no history of a tick bite. “Then you’d be treating thousands for no reason.”
His bottom line: “In my opinion, someone who has a definite tick bite and an illness with a fever, in tick season and tick geography, with no other clear-cut explanation like ‘I have a horrible sore throat and pus on my tonsils’ — I don’t think I’m that out there by saying that person needs to be treated as if they have Lyme disease.’ (And there are other potentially dangerous tick-borne illnesses to be aware of as well, babesiosis and anaplasmosis -- see this recent New York Times report and watch out particularly in coastal Rhode Island.)
So is there a rule of thumb, I asked, for when to push for antibiotics? No, Jonathan replied, each case is different. Perhaps “the best rule of thumb is to find a doctor who will give you the time and look you in the eye and explain what their thinking is and listen to what you’re saying. And ultimately you just have to come up with a decision with that doctor on what’s the best move.”
Lyme Disease Guides
UpToDate, an authoritative source for medical staffers that also offers wonderfully readable information for patients, has an excellent guide to early Lyme Disease treatments here. Among others, it cites these sources: The American Lyme Disease Foundation FAQ and the CDC Lyme Disease Home Page, which includes a helpful FAQ and the official treatment guidelines it endorses.
And here is Dr. Catherine Brown’s advice:
1.Before you go outside, remember that tick-borne illness in Massachusetts is a significant issue, so do what you can to protect yourself.
2.If you find a tick on you, remove it carefully using a fine, needle-nosed tweezers. Grab the tick close to the skin and pull it out with steady pressure, without twisting.
3.Go online and find pictures of ticks and figure out if it’s a deer tick, the type that carries Lyme Disease.
4.Monitor how you’re feeling. Watch for the bullseye rash but also for fever, headache, sore muscles, achy joints. If you were bitten by a deer tick and develop symptoms, you have to call your doctor at that point.
5. Lyme Disease is by orders of magnitude the most common tick-borne disease in Massachusetts. But two other illnesses are carried by the same tick: babesiosis and anaplasmosis. Those case number only around 100 a year, but they are much more serious, and tend to affect older populations.
This program aired on July 1, 2011. The audio for this program is not available.
