Support WBUR
One Man's Sedation-Free Colonoscopy (And Why You Should Try It Too)
Guest Contributor
I’m one of an elite group of American patients. Only about one percent of us undergo colonoscopy without sedation. The big secret: it doesn’t have to be painful. And it’s probably safer than with sedation.
Like most Americans, I was ignorant of all of this until about a month ago. In my imagination, a sedation-free colonoscopy would have been painful indeed, the device snaking up my GI tract, pushing against my insides as it resisted the twists and turns. Then my best friend, Greg, who has made several suggestions that have resulted in distinct improvements in my life, suggested forgoing the drugs, as he had recently done.
It made sense. I could drive myself to and from the hospital, and I’d be able to work when I got home.
Greg had also told me that there’s a correlation of anesthesia with loss of memory later in life. Some googling revealed that this may be true in some cases. But despite that uncertainty, that made the unmedicated colonoscopy far more compelling.
It helped to learn that Dr. Douglas Horst, who would be doing the colonoscopy, did a number of them unsedated, and even more, that he called me to discuss it, putting my mind even more at ease. (He gets top grades on several different doctor evaluation websites.)
And overall, the discomfort was minimal, hitting maybe 3-max out of 10 on the pain-meter for seconds at a time here and there, and otherwise never going beyond 2 out of 10, comparable, perhaps, to a very mild cramp. I’d much rather have another colonoscopy than an upset stomach.
The Prep: Dystopian Poison
Far worse than the colonoscopy was the “prep.”
And the really bad part of the prep was the drinking of the laxative. At 7pm the night before the colonoscopy, and again at 4:30 in the morning, I had to drink 15 ounces — two cups — of the supposedly lemon-lime flavored magnesium citrate. The prep sheet from Beth Israel Deaconess Medical Center in Boston recommended putting it in the icebox prior to use, to blunt the taste, which they suggested because chemical reactions, including those involved in taste, proceed more slowly at lower temperatures. I went one better. I stuck the bottles in the freezer for the last 45 minutes. But even with ice beginning to form in the bottles, the taste was still strong and dreadful. The drink combined the wonderful fizziness of soda — the elixir of the summertime American childhood — with a cloyingly sweetened base metallic taste. There are plenty of bad-tasting medicines, but that juxtaposition of good memories with sweetness gone sickly made this stuff seem like a post-apocalypse dystopian poison.
During the 7pm episode, it took me an hour and a half to down the two cups’ worth, washing each bit down with some ginger ale in a largely vain attempt to banish the dystopian aftertaste. During the 4:30 am episode, I tried chugging it down more quickly, but it still took 40 minutes.
The magnesium citrate had to be followed with at least three normal-sized cups (24 ounces) of clear liquid, to maintain hydration in the face of the saline onslaught. The prep sheet warned that failure to do so could endanger your kidneys — just one more thing to go wrong if you failed to follow the directions in the middle of the night.
Ironically, my biggest fear—the fear that had kept me from getting the colonoscopy for the first nine years after I turned 50, was the vision I’d had of being a prisoner in the bathroom while my guts violently wrung themselves out for hours on end. Yet, the diarrhea, which began after about an hour of drinking the gag soda, was not the least bit gut-wrenching, and not particularly copious — thanks probably to the day of fasting. During the hour and a half or so that it continued, it quickly became liquid, and gradually became clear (your results may vary). While I’d set out magazines and books on the little table, as well as a radio, figuring I wasn’t going to leave the bathroom for a couple of hours, I found I was able to move around the house with impunity.
The Procedure: Up Mine
After a few more hours of sleep, I got up, and drove the 35 minutes or so in mild traffic from Lexington into Beth Israel, arriving around 9:30. I’d been afraid I might need to go to the bathroom on the way in, but the diarrhea was over.
At 10:45, Nurse Tina DiMonda rolled me into the procedure room. She installed an IV — just in case — and asked me to lie on my left side. Then, Drs. Douglas Horst and Byron Vaughn began feeding the colonoscope inside my plumbing.
In our society, and perhaps generally among our species, the rear end carries a lot of baggage, as is obvious from the various epithets and other expressions that have the word, “ass” in them. This is not helpful in the medical theater. But between my own blasé attitude, and the docs’ and Nurse DiMonda’s excellent bedside manner, during these proceedings the anal orifice became a mere porthole into the gastrointestinal plumbing. Mine might have been exposed, but it was totally safe, and I soon forgot about it, despite the fact that it was propped open, mildly uncomfortably, by the colonoscope.

Dr. Horst immediately launched into some jokes, and soon I felt as if I’d gone to a bar with some friends. Of course, there were some major differences, such as the spectacular view on the screen of the pinkish tunnel with the skinny ridges encircling the passageway, looking the way one might imagine a hallway down the inside of a segmented worm. What is the evolutionary reason for the ridges, I wondered. Dr. Horst said he didn’t know of one, but he’d come up with a theory if I could write it up and make him famous.
Soon, a small clump of tiny white things appeared, adhering to the inside of my colon. “Did you take a capsule?” Dr. Horst asked. “Niacin.”
Now we were approaching the first of four sharp bends in my colon, and I could feel my insides being stretched. Although the discomfort may have reached a mere 3 out of 10 on the pain-meter, it’s always more unnerving when you can’t see the source.
Now we were approaching the first of four sharp bends in my colon, and I could feel my insides being stretched. Although the discomfort may have reached a mere 3 out of 10 on the pain-meter, it’s always more unnerving when you can’t see the source, even if you know what it is.
I began making noises like those that Tigger had made when the Pooh Corner gang, trying to figure out what Tiggers eat, had tried thistle on him. Tigger, undoubtedly discombobulated by the thorny stuff sliding down his insides, had said, “Warawarawarawarawara.” A.A. Milne had his onomatopoeia down pat; and the docs knew what I was talking
about, and slowed down, maneuvering carefully around turn #1, mitigating my discomfort. Then we were off on another
straightaway.
A Bend In The Road
A later sharp bend in the colon occurs where the plumbing approaches the surface of the stomach from the vertical, and then turns 90 degrees to run parallel to that surface. Tina put her hands flat on my belly, pressing gently, a maneuver which prevented that unsettling stretching within, the docs rounded the bend, and we were off on another straightaway.
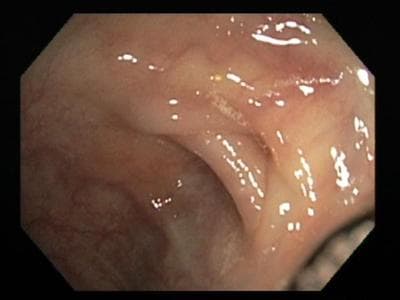
The rest of the half hour long spelunking expedition was uneventful, with occasional unsettling, mildly uncomfortable moments, particularly at the sharp bends, and at one point, a mild burning sensation in my anus, which turned out to be insufficient lubrication, a problem which was quickly remedied. As for the inner terrain, the cleansing had been so successful that even in the upper reaches, almost nothing was visible except for the shimmering surface of my colon, which was devoid of even tiny polyps. (Healthy colons are thus, even on 90 year olds, because the epithelium gets replaced about every three weeks, said Dr. Horst.)
Congratulations All Around
At the end (oops!), the docs and Nurse DiMonda congratulated me for how well I had tolerated the proceedings. Then we talked about the factors that influence an unsedated patient’s experience. It’s partly the doctor’s skill in guiding the colonoscope in a sensitive manner, said Dr. Horst (a skill which a doctor who has done few or no unsedated colonoscopies is unlikely to have). And it’s partly the patient’s pain tolerance. Some doctor-patient combos have great success, and others fail miserably, according to blog comments on the subject.

Another factor is patient expectations. I’m not particularly pain tolerant. But Greg had primed me not to expect pain. And studies show that expectations have a profound influence on pain, or lack thereof.
Moreover, I’d had my own prior experience with an analogous, though not identical procedure. In ‘98, I’d undergone a “colonic irrigation,” a sort of a new age cleansing to which all sorts of interesting claims were attached, for an article I wrote in an alternative medicine journal. There was plenty of internal pressure as my colon filled with water, and at the time I described myself as feeling bloated, as if I had mild to moderate indigestion — not what you would call a daunting experience.
It’s worth noting that the extra care that must go into an unsedated colonoscopy to avoid hurting the patient probably makes complications, such as a tear in the colon, less likely. But “since complications are rare, it would be hard to assess,” says Dr. Horst.
Not For Everyone
Interestingly, most institutions don’t even offer unsedated colonoscopies, although some will provide them if asked. Even when I came in for mine, everyone I came into contact with beforehand — a couple of nurses, the receptionist — was surprised when I told them I wasn’t getting sedation. (Probably not unlike the experience of some pregnant women who decide to forego drugs during labor and face skeptical hospital staffers.)
Dr. Horst says he performs about two to five percent of colonoscopies without sedation, “higher than the general rate because I have a small reputation for success at that.”
“Of those who start [a colonoscopy] without [sedation], probably 80 percent finish without, which reflects a self selection process — return patients who did it without meds before, and patients interested in and therefore pre committed to doing it,” says Dr. Horst. “Many years ago, I did a study. I offered unsedated scopes to all my patients. 200 patients later, 120 accepted the concept, but 50 percent of those who tried decided to take meds during the test.”
Still, Dr. Horst’s figures, and the fact that in Europe very roughly half of all colonoscopies are unsedated, suggest that far more people would be happy to forgo sedation. For doctors, the unsedated procedure is slightly slower, and more difficult. And for the hospital, and/or the insurer, it’s in the hundreds of dollars less expensive.
Although I had looked forward to a full afternoon of hard work after the colonoscopy, I conked out soon after I arrived home, and had someone not called me an hour later, I think I would have slept all afternoon. It’s not surprising. I’d spent two and a half hours on prep in the middle of the night, and the stress of quaffing the magnesium citrate had undoubtedly further drained me. Nonetheless, when I have to get my next colonoscopy, 10 years from now, I’ll definitely opt out of sedation.
David C. Holzman writes from Lexington, Mass., on science, medicine, energy, environment, and cars. He is Journal Highlights editor for the American Society for Microbiology and won a Plain Language/Clear Communication Award in 2011 from the National Institutes of Health.
This program aired on February 1, 2013. The audio for this program is not available.