Support WBUR
Commentary
Do High-Deductible Plans Make Even Cancer Care A Luxury Item?
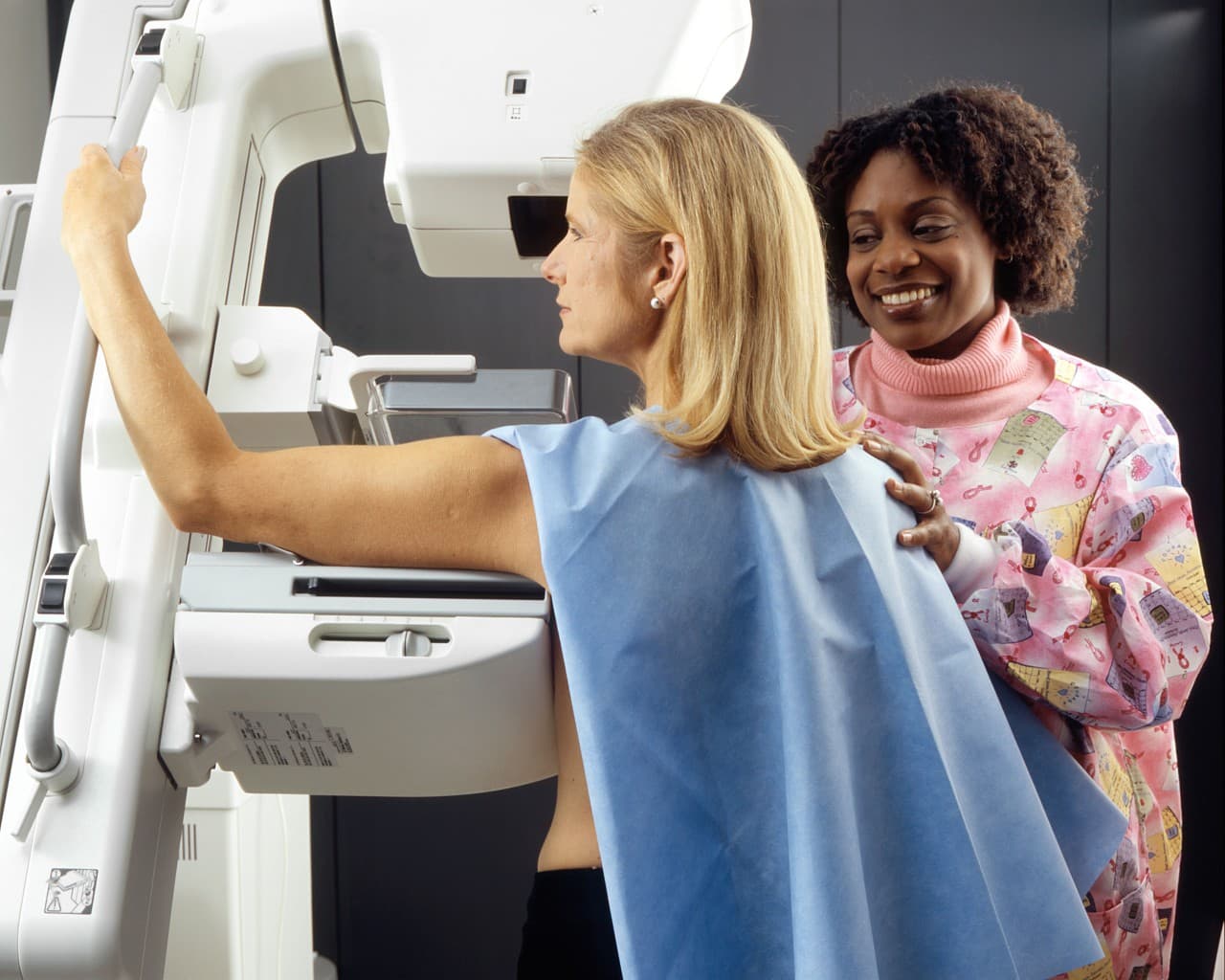
I’ve dedicated much of my career to improving access to health care. I served as one of the founding leaders of the Massachusetts Health Connector, and before that, I was the chief operating officer for the state's Medicaid program.
I’m also a breast cancer survivor. And a high-tech mammogram, followed by timely care, saved my life.
When I went in for my regular screening in the fall of 2016, the high resolution images detected some tiny, suspicious cells that I soon learned was very early-stage breast cancer. After further tests, I underwent a mastectomy and now my chance of survival is 100 percent. But if I had waited a year or even six months for the additional testing and treatment, it could have been a totally different story -- for me, my husband and my children.
That’s why I was so disheartened to read about a recent study that found American women are increasingly deferring tests — and even treatments — for breast cancer because their health insurance plans have such high deductibles.
These results echo other research with similar findings. For example, last year, the CDC's National Center for Health Statistics reported that among privately insured adults aged 18–64, the percentage of those who did not get or delayed medical care due to cost was significantly higher for those with a high-deductible health plan (about 9 percent) than for those with a traditional plan (about 5 percent).
Compounding the problem, high deductible plans are gaining popularity. That same CDC report concluded that the number of Americans age 18 to 64 with a high-deductible plan increased from 26 percent in 2011 to 39 percent in 2016.
What this tells me is that more and more Americans are thinking of their health plans as catastrophic care only. In other words, they’re opting for insurance that only covers them if something “big” happens — and they’re treating tests and other medical procedures like luxury items.
But here’s the problem with that mindset: When people put off getting diagnostic imaging and biopsies or delay treatment because they can’t afford the out-of-pocket expenses, there are very real costs — for them, and for the rest of us, too.
For serious conditions, like breast cancer, even short gaps between diagnosis and treatment can complicate matters. Multiple studies have shown that preventative care leads to better health outcomes and higher quality care. In breast cancer, the earlier the disease is diagnosed and treated, the higher the chances for long-term survival. The American Cancer Society breaks it down as follows:
· Stage 0-1: Close to 100 percent survival rate.
· Stage 2: Relative survival rate of 93 percent.
· Stage 3: Relative survival rate of 72 percent.
· Stage 4: Relative survival rate of 22 percent.
If high-deductible plans continue to gain traction in the marketplace, we will all pay the price. There is no doubt that these plans can be a source of poor medical decisions when more people are forced to make hard decisions about whether some care is worth it.
Granted, striking the balance between health care quality and cost isn’t easy. But if Americans are delaying care that could prevent health emergencies later or improve their quality of life, I think it’s time to take a step back and re-examine how we got here: Why do we tolerate this disconnect between health care access and affordability? Can we do a better job of eliminating financial barriers so people can get the care they need? And have we gone too far in discouraging unnecessary tests, to the point that people are now confused about which tests and treatments they truly need?
For me, it boils down to protecting the Affordable Care Act from further erosion. The ACA not only requires that mammograms be fully covered, it also provides BRCA gene testing and genetic counseling free of charge for those who qualify.
What’s more, the law prevents insurers from denying coverage or charging people more based on pre-existing conditions. Insurers cannot impose annual or lifetime limits on coverage, which is important because breast cancer treatments are costly. And no one should have to choose between food, housing or paying for medical bills so they can live.
Finally, we need to put a lid on out-of-pocket costs, and consider restructuring high deductible plans so that people don’t defer needed care. We also need to insist on coverage of “essential health benefits,” so that your insurance actually covers the conditions you may have, while helping you find, and treat, any new ones that may crop up.
As a cancer survivor, I’ll be forever grateful for early detection and treatment. Almost as importantly, I benefited from having great health insurance -- I had a low deductible, and never once had to give pause to think about how I might pay for an expensive surgery, chemo or radiation bill. It’s hard for me to imagine any woman with breast cancer having to let money drive their decisions about medical care when it is obvious what’s best for their health.
Early, prompt care saved my life. How awful that for many Americans, it is now a “luxury.”
Rosemarie Day is the president of Day Health Strategies, a Somerville-based consulting firm, and has been actively involved in health reform since 2006. She tweets @Rosemarie_Day1.