Support WBUR
Coronavirus Coverage
Pace Of Coronavirus Vaccination Lags Supply In Mass.
So far in Massachusetts, the pace of vaccinating residents against COVID-19 is way behind supplies of coronavirus vaccines. The latest update Monday from Gov. Charlie Baker shows about 40% of the doses delivered to Massachusetts have been injected and, state data released last week shows, 92% have gone to hospital staff. There’s a similar lag in vaccine distribution happening in other states.
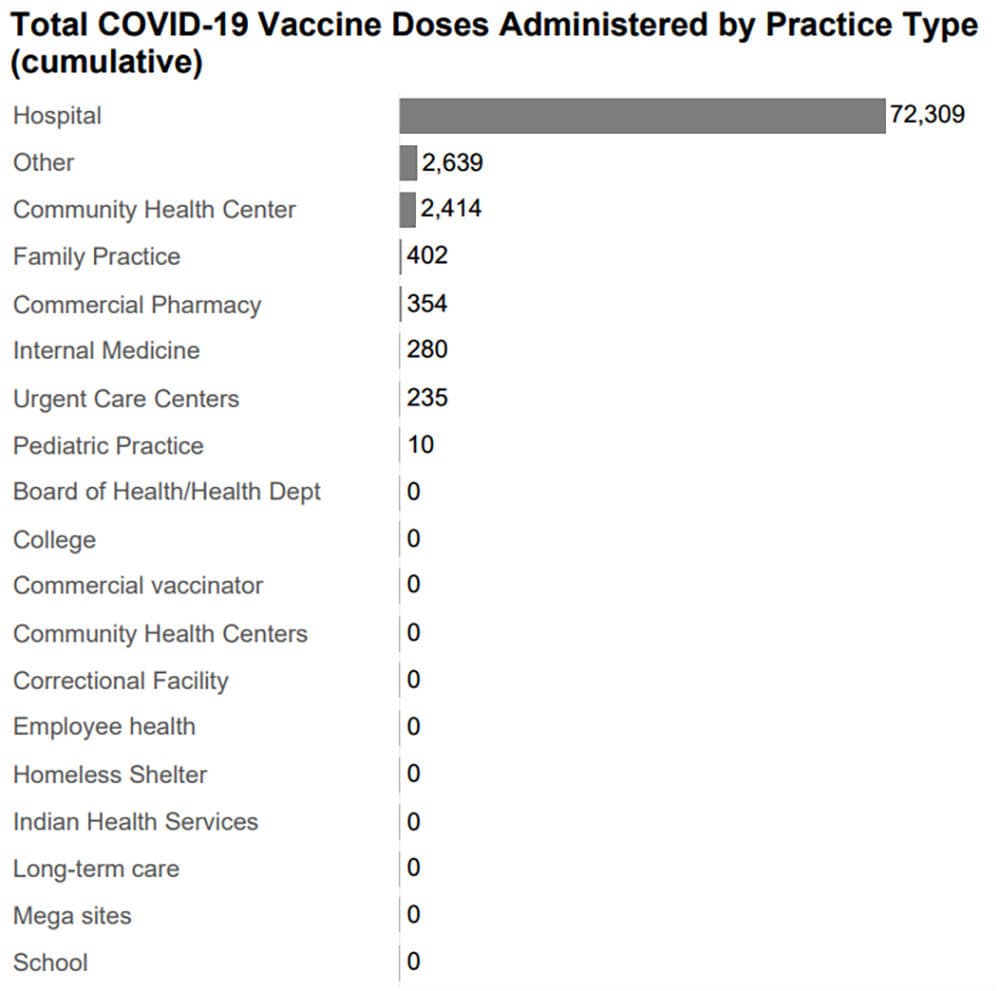
Gov. Baker has cautioned that vaccination numbers reported by the state could be up to four days behind because there are delays in updating the state’s vaccine registry. There appear to be some longer reporting gaps. The current dashboard shows no vaccines delivered to nursing homes even though vaccinations began in those facilities on Dec. 28.
State health officials have not yet responded to WBUR’s questions about the rate of the vaccine rollout so far.
Numbers aside, there are some consistent reasons vaccinations are off to a slow start for the first two priority groups, front-line health care workers and the staff and residents of long-term care facilities.
- The December holidays reduced vaccine clinic hours over the last two weeks of the month. Some facilities offered vaccines on weekends, others did not.
- Hospitals, community health centers and nursing homes all have eligible employees who don’t want the vaccine at all or don’t want it right away. There’s a wide range, with some facilities reporting fewer than 10% of staff are hesitant and others saying that about 63% have declined.
- Facilities may have received more than they need for the first dose. Some are holding on to extra vials in case more employees come forward, or in case it’s time to deliver the second dose of Pfizer or Moderna’s vaccine before more supplies have arrived.
- Delivering the vaccines takes longer — in some cases much longer — than other vaccines. Some clinics have delivery of a flu vaccine down to 2.5 minutes per person. Coronavirus delivery times started at 30 minutes or more, depending on how much paperwork was completed online, in advance, and how many questions each recipient asked. Some clinics have cut the time, including 15 minutes of observation after injection, to 20 minutes. But at nursing homes, it’s taking longer to vaccinate residents who can’t leave their rooms, for example.
Dr. Asif Merchant, a geriatric medicine specialist, says there just aren’t enough vaccinators trained and mobilized for even the early stages of this mammoth project.
“That’s caused much more of a delay than I would have anticipated,” said Merchant, who is the medical director at four nursing homes near Boston. “I think when it comes to the general public, that’s going to be even more of a problem.”
It’s a problem that could lead to wasted doses. Late last week, one pharmacy chain thawed more of the Pfizer vaccine than could be used at several nursing homes. The vaccine is only good for five days after it comes out of the deep freeze, so pharmacists gave several hundred doses to Beth Israel Lahey Health, where a hospital spokeswoman says they were glad to receive them.
The nation’s top infectious disease expert, Dr. Anthony Fauci, said on Sunday that the pace of the vaccine roll-out is increasing and could get back on track in the coming weeks. But there’s also concern that vaccine distribution will become more, not less, difficult and complicated as more vaccines are authorized for emergency use and vaccinators try to reach a broader swath of people including vulnerable groups: home-bound residents, people who don’t have stable housing, patients battling addiction and other chronic diseases.
Although Massachusetts’ vaccination rate trails supply, the state is proceeding with its plan to vaccinate the next priority groups. Some first responders are scheduled to receive their initial shot of the Moderna vaccine on Jan. 11. Vaccinations inside prisons, homeless shelters, addiction treatment facilities and group homes could begin the following week, depending on supply of the vaccine and of people to deliver the shots.
Tufts Medical Center is training medical students to help administer vaccines. Elizabeth Hale, the director of clinical services at Lowell Community Health Center, says she’s creating partnerships with the city’s health department and school nurses as the coronavirus campaign expands. But she and Dr. Merchant are both looking for more regional, state and national leadership.
“Let’s do some more planning. How can we do this faster?” Hale asks. “Get us all together, get us collaborating. Let’s use what we learned from contact tracing and testing and apply that to vaccinating.”
