Support WBUR
Coronavirus Coverage
Tackling Vaccine Hesitancy In Massachusetts, One Conversation At A Time
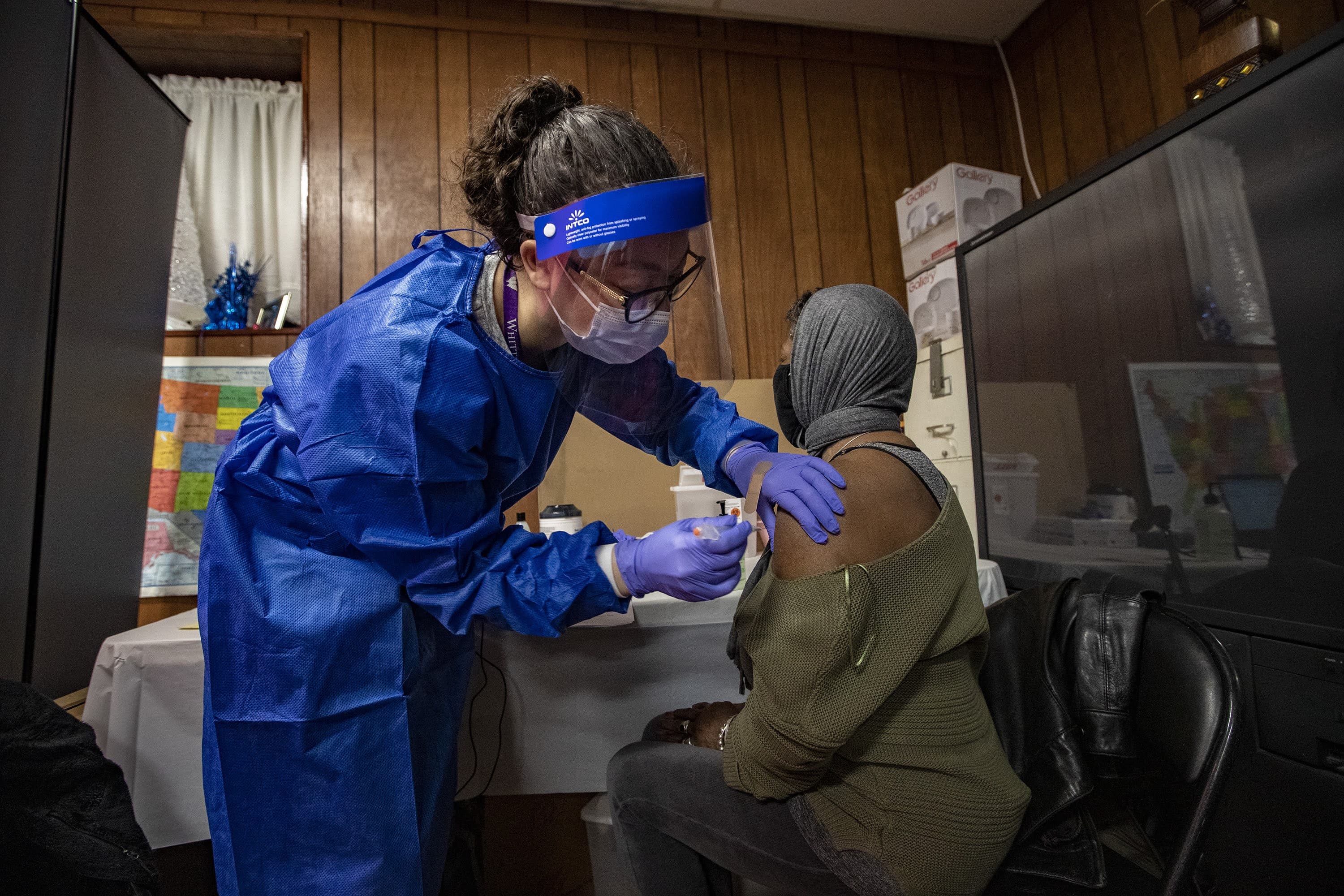
The blue bus stands out on this narrow street running through a neighborhood of subsidized housing in Revere. If you miss the banner announcing “Vaccine Information” or the mounted TV scrolling through vaccine FAQs or the table stocked with masks and hand sanitizer, maybe this announcement will catch your attention.
“Good afternoon neighbors, we are here with the City of Revere and Mass General Brigham distributing the free food boxes.”
As you pick up a box, someone from Massachusetts General Hospital is there to help and strike up a conversation. How are you and your family doing? Have you been touched by COVID? Have you thought about getting the vaccine?
This is vaccine outreach as the state and nation race to stop the spread of the coronavirus and mutations that could trigger another surge, restrictions and more deaths. At least one national poll shows growing interest in the vaccines with Blacks exceeding whites. Thirty-seven percent of Latino respondents still say they don’t plan to get vaccinated.
Massachusetts has funded a vaccine campaign that will focus on 20 communities with the highest rates, but some hospitals, health centers, churches and other groups are already out — looking for residents who are hesitant, and encouraging them to talk about why with people they trust, in places where they are comfortable.
In Revere, a woman in an orange Ford Fiesta pulls up next to the blue Mass General Brigham van. Someone slides a box of produce and dried goods onto her back seat then asks if she has any questions about the vaccines. Nope, she’s on board, just waiting her turn for a shot.
Khadija Sona, who stops to pick up a box of food, says she doesn’t want a COVID vaccine.
“If I have to do it, I will do it to work or go to my country, Morocco,” Sona says, “but I would rather not.”
Sona says she’s heard the vaccine is not healthy. She doesn’t want to elaborate. A nurse steps over to talk about why some people feel sick after getting the vaccine; it’s because their body is building immunity to the coronavirus. Haroon Sidiqi has heard similar concerns about side effects from hesitant co-workers but says he trusts the vaccines.
“We live in the best country on the planet,” he says. “This country will not give something to their own people if it’s not safe enough.”

Dr. Joseph Betancourt, the senior vice president for equity and community health at Mass. General, has been out with the van, talking to residents in Chelsea and Revere.
“We’ve had a lot of conversations with people, and here’s the stereotype breaker,” he says. “In many communities we’ve been in, people are actually very eager to get the vaccine. The questions we’re getting are more about where can I get it, when is my turn.”
Vaccination rates are slightly lower in Revere compared to the state as a whole. As of last week, 9% of Revere residents were fully vaccinated, compared to 12% statewide. Among white residents of Revere, 13% are fully vaccinated. The rate for Black residents is 8% and for Latinx residents it’s 3%.
Betancourt says that lower vaccination rates in some hotspot communities are less about hesitancy and more about the lack of easy access to a vaccine. There are two pharmacies that offer vaccines in Revere. Beth Israel Lahey Health has a clinic for patients in that system, and there’s a public clinic one town over from Revere. But the two closest mass vaccination sites are about a 30 minute drive, much longer via public transportation.
“Until we’ve made vaccine available in communities, made people aware and been able to facilitate scheduling, it’s only until then and we see low numbers that we can say it’s because of vaccine hesitancy,” says Betancourt. “Today quite frankly, vaccine has not been readily available, in easy ways, in hard hit spots across the state.”
Betancourt and other doctors say easy access means more local clinics, where people can walk in without the hassle of online registration, in familiar places. Six Boston churches are testing something like that model this month.
At Pleasant Hill Missionary Baptist Church, Pastor Miniard Culpepper leads a team of volunteers in prayer before opening the door to the basement social hall for a pop-up vaccination clinic run by Whittier Street Health Center.

“The church is in the business of saving people, that’s what we do,” Culpepper says. “We save people, we save lives. Now we’re trying to save lives in a much different way.”
That’s not an easy sell for some parishioners who wonder why they should trust a drug the U.S. government is urging them to take.
“If you look at the history of how the government has treated African Americans,” Culpepper says, “how we were tricked, it’s a challenge to help folks understand that the coronavirus doesn’t discriminate against anybody.”
But a fear of COVID trumps vaccine resistance for Pleasant Hill community members in line today.
“That doesn’t mean I don’t take into account the history of what happens to African-Americans, but I don’t want to die from COVID,” says Nazaleem Smith, a retired teacher who got a walk-up appointment.
Lucille Culpepper-Jones, the pastor’s sister, says she never gets shots, including the flu vaccine. But Culpepper-Jones has had several lung surgeries.
“I would rather take the chance with the vaccine than with COVID,” she says. “And oh yeah,” she’s nervous.
Vaccine outreach and the questions posed by residents will vary. Many younger people are less worried about dying from COVID but still have concerns.
“Does it do anything to your reproductive system?” asks Gabriela Wood during a routine appointment at the Lynn Community Health Center.
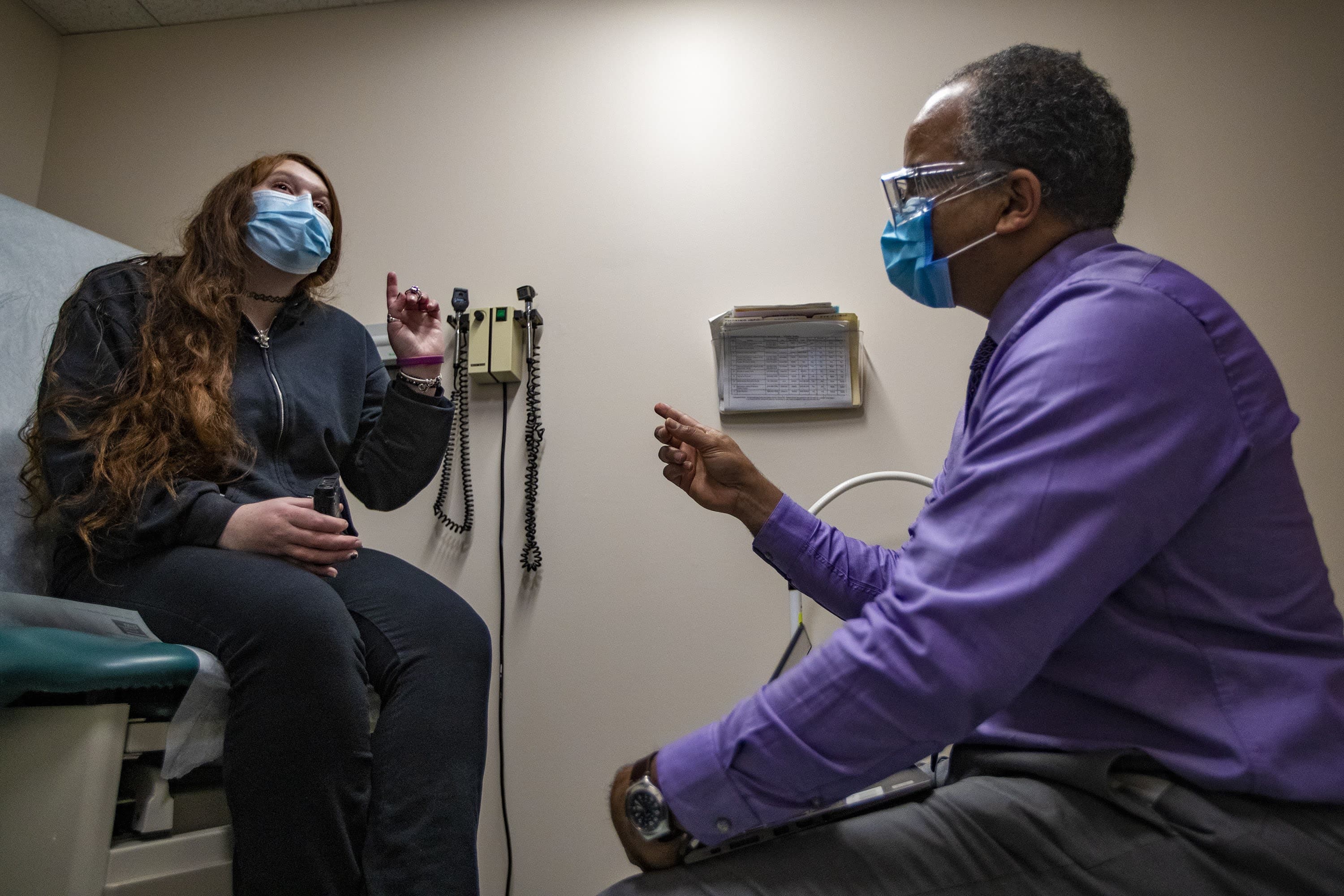
“I’m very comfortable that it’s not going to affect fertility or even a pregnancy, I’m fairly certain that’s not going to happen,” says her physician, Dr. Kiame Mahaniah.
Mahaniah started this appointment with Wood, as he does now with many patients, by asking if she’ll get vaccinated.
“I don’t know, it just scares me,” she says. “There’s so much out there and so much misinformation, it’s hard to know what to believe.”
Mahaniah asks Wood more about why the vaccine is scary, where she gets information and whether her family and friends plan to be vaccinated.
“The thing that really influences people whether or not they’re going to get the vaccine is what their social circle is doing,” he says, after the appointment.
Wood has some skeptical family members. She’s eligible for the vaccine based on some high risk medical conditions but has declined so far.
Mahaniah is having a lot of open-ended discussions with patients about their health and vaccines. He says it’s pretty clear that giving people more data is not persuasive. Instead, he uses a technique known as motivational interviewing as he would with patients who smoke or who are due a screening test they’re avoiding.
“I don’t approach these [conversations] as me being able to provide them with the right information to make the right decision,” Mahaniah says. “I’m really approaching these as, let’s try to create a space in which a conversation can happen where they can evince their doubts, their uncertainties.”

There may be data that’s useful at some point, but the initial conversations are about the patients thoughts, opinions and world views.
“So instead of me being pro-vaccine and the patient being anti-vaccine, it’s really about eliciting the parts in the patient’s own thinking that are pro-vaccine,” Mahaniah says.
It’s a time-consuming process but one that is unfolding in clinics, hospitals, pharmacies, churches and many other sites as we get closer to a time when there will be access to vaccine appointments for a broader swath of the public and rising pressure on people who are still hesitant.
This article was originally published on March 14, 2021.
