Support WBUR
Brigham Face Transplant Pioneer Reflects On His Patients And The Procedure As He Heads To Yale
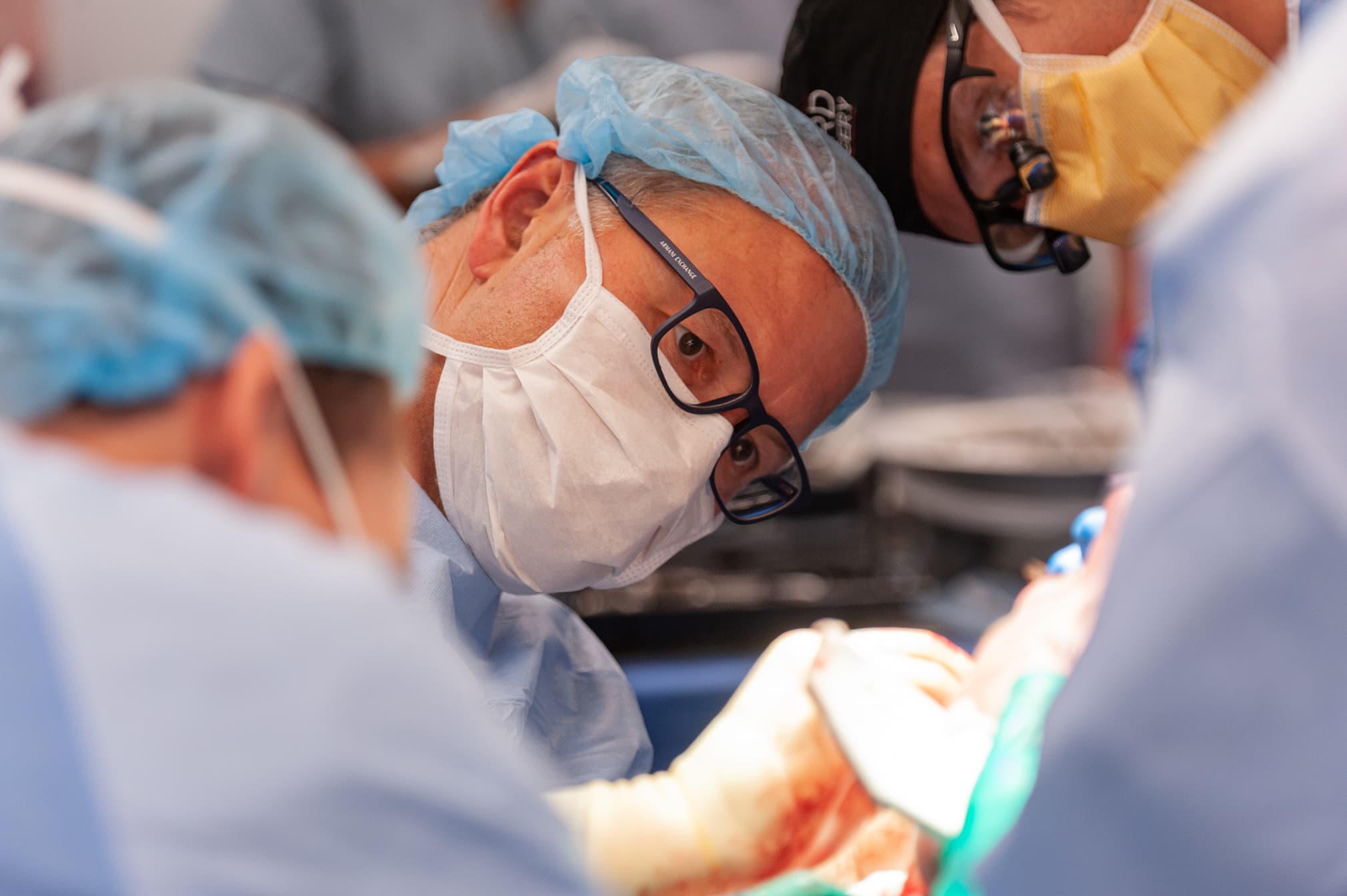
The future of face transplants at Brigham and Women's Hospital is under discussion upon news that the surgeon who pioneered the program there starting more than a decade ago is leaving.
Dr. Bohdan Pomahac, director of plastic surgery transplantation at the Brigham and professor of surgery at Harvard Medical School, has accepted a new position as chief of plastic surgery at Yale. He says he'll remain at the Brigham until the end of May and start at Yale this summer.
A spokesperson for the Brigham issued a statement to WBUR saying the hospital remains committed to caring for its patients who have undergone a face transplant there but understands some of Pomahac's patients will follow him to Yale for their ongoing treatment. The statement goes on to say, "As Dr. Pomahac transitions out of his current role, we are carefully considering the future of the face transplant program at the Brigham."
Pomahac is a national leader in face transplants. He's performed 10 of the 17 procedures that have taken place in the U.S. Brigham and Women's is one of only a handful of hospitals in the country that does the operation. Face transplants have also been performed in several other countries.
WBUR's Jack Lepiarz spoke with Pomahac on All Things Considered about his reflections as he prepares to leave Boston.
Interview Highlights:
Dr. Bohdan Pomahac: Well, it's sort of bittersweet. I started the endeavors more than 10 years ago, and it took quite a bit of time to be able to build it and do all the exciting operations that we did. But I also feel that it's the right time for me to move on, and I'm certainly hopeful that the patients [who've already received face transplants] would continue following up with me and stay my patients for the future.
On whether the face transplant program at the Brigham will continue:
It's possible. To be honest, I don't think there's immediately anyone who could succeed me. But it's not impossible that someone will either join or learn the technique. It's, after all, not that unique anymore. And there are many of my colleagues that are skilled enough that they could certainly, with a little bit of training, pull it off.
On what he was feeling when he led his first full face transplant operation in 2011 (following a partial transplant on another patient in 2009) — the first full face transplant in the U.S.:
Oh, I was nervous beyond belief. It was nerve-wracking. We had also some complicating events related to really acute need [to recover] some of the lifesaving organs from the donor, so it created logistical complications and problems. It was really stressful. But thanks to the team, it really worked out.
The fundamental problem is that it takes about six, sometimes even seven, hours to recover a face from a donor. And that time is actually longer than recovery for all of the other organs together. So we actually have to start first, but with the understanding [that] if there is an acute need for lifesaving organ recovery, we would stop and let the other teams recover — or work together as much as possible.

On what it means to patients' lives for them to receive new faces from donors after suffering disfiguring trauma:
You know, we all take for granted that we have eyelids to protect our eyesight, nose to be able to breathe, lips to be able to communicate, eat and so forth, not drool ... But for the patients that we have selected, all of those things were gone. And even though after the transplant they don't look perfectly normal, they don't function perfectly normally, it is such an exponential improvement compared to what we used to do and what we were able to achieve. The patients have been universally extremely satisfied and happy.
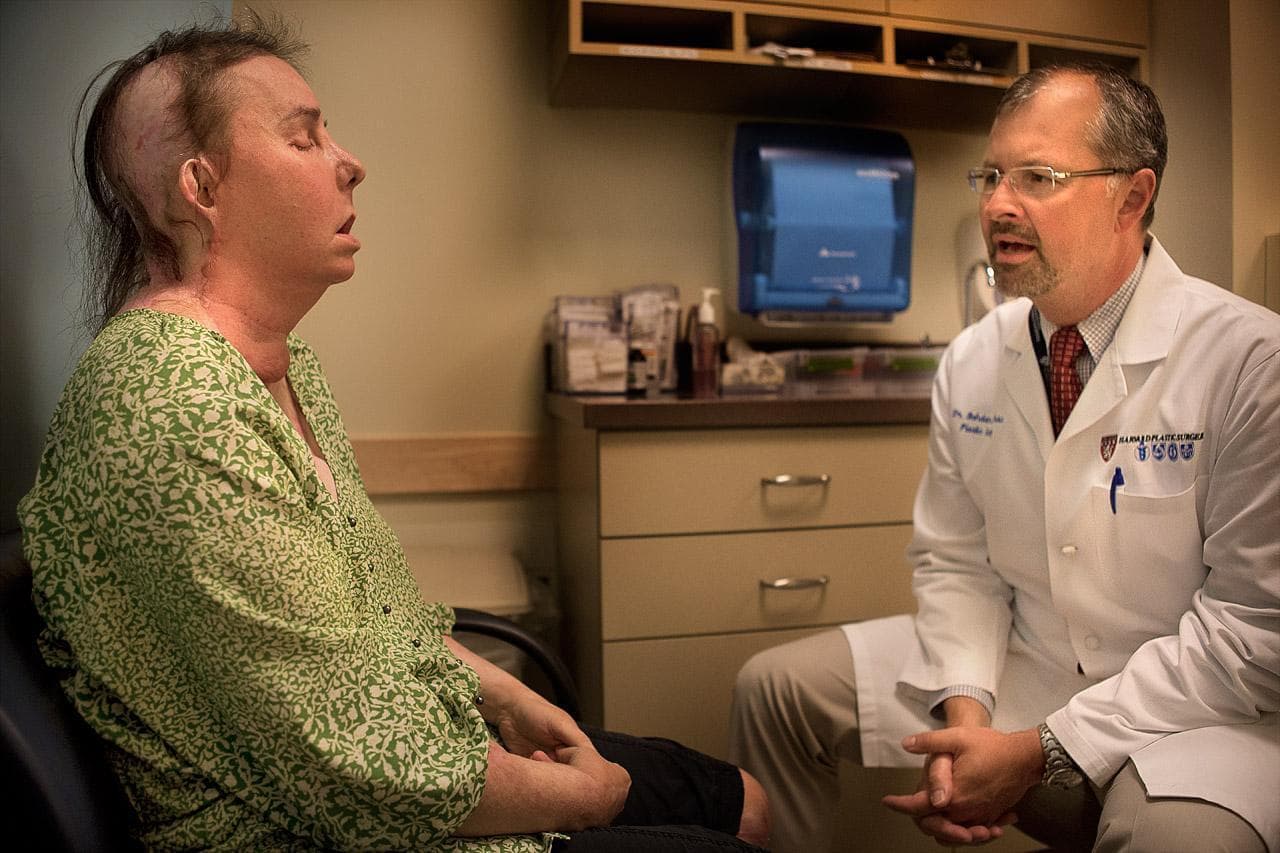
On milestones, including performing the first face transplant on a Black recipient in the U.S., Robert Chelsea, (in 2019) and last year, performing a second face transplant on Carmen Blandin Tarleton because her body was rejecting the first one (which had been transplanted in 2013):
They both are very unique and both very amazing people ... Carmen, as you have mentioned, she was a victim of domestic violence and she has had so many complications because of her complex immune system and ultimately ended up getting — as the first patient in the U.S. — a second transplant. That whole story is just unbelievable to me. And I'm always impressed by her strength, by her attitude, by her ability to move on in situations when I think not many of us would be able to do so and would find that strength and courage.

On advances made in immune response to transplanted faces and the procedure itself:
Without a doubt, immune suppression and the side effects of the medications is the main problem with this. But no question, in the future, if we find a way to minimize immune suppression it would be terrific. We have put together protocols with immunologists and we have had some early successes, minimization of medications. But we're still far from the ideal, which would be either medication without any side effects or no medications at all.
We have learned a lot both from what we have done, but also from our colleagues elsewhere. There have been a lot of nuances and technical aspects that have made the results better and the operation faster and safer.
This segment aired on April 2, 2021.

