Support WBUR
'Impossible Lawsuit': Families Find Few Options To Sue Long-Term Care Over COVID Deaths

Part one of two stories. Read part two here.
Suzanna Smith’s mother was supposed to spend a few weeks at a rehab facility in Fitchburg to recover from surgery, but she never came home.
“She went in for back surgery, and she died from COVID. It’s still so surreal to me,” Smith said. Her mother, Masae Hodges, was 73 when she died last year.
Hodges is one of more than 6,000 residents of nursing homes and other long-term care facilities in Massachusetts who have died of COVID-19, roughly one third of all COVID deaths in the state. But for grieving relatives like Smith, there are few legal options if they believe these facilities should have done more to protect their loved ones during the pandemic.
According to Smith, her family didn’t know that the facility, Fitchburg Healthcare, had been experiencing COVID cases when Hodges was transferred by the hospital. After she arrived, they struggled to get information about how she was doing.
“There were days where we were not getting any calls, and we would be calling the facility, and sometimes the phone would ring and ring and ring," Smith recalled. "One day I called and left the phone ringing for 20 minutes straight. Finally someone picked up the phone.”
The Massachusetts Department of Public Health, not staff from the facility, notified Smith's family that her mother had contracted COVID. Smith remembers that a state employee called her father to report the test results.
“And that was a real surprise to my father because the nursing home never, ever communicated that they were testing my mother, one. And two, that they had COVID patients,” Smith said.
She and her father were furious. They couldn’t visit her mother because of COVID safety regulations, and her health quickly worsened.
"... The nursing home never, ever communicated that they were testing my mother, one. And two, that they had COVID patients."
Suzanna Smith
Hodges was sent to a nearby emergency room five days after the positive test. Smith spoke by phone with the doctor who cared for her mother there.
“They were saying that her lips were bleeding, she was severely dehydrated," Smith said. "The doctor from Leominster Hospital speculated that she had been dehydrated for several days.”
Hospital officials said they cannot confirm any details about Hodges' condition, citing patient privacy laws. Fitchburg Healthcare also said it can’t comment on a former resident but provided a written statement to WBUR.
“The safety of our residents and employees is of the utmost importance and is always at the center of all decisions we make,” the facility wrote, adding that the state began auditing nursing homes’ infection control procedures during the pandemic. “Fitchburg Healthcare received two on-site audits and in both cases received a perfect score.”
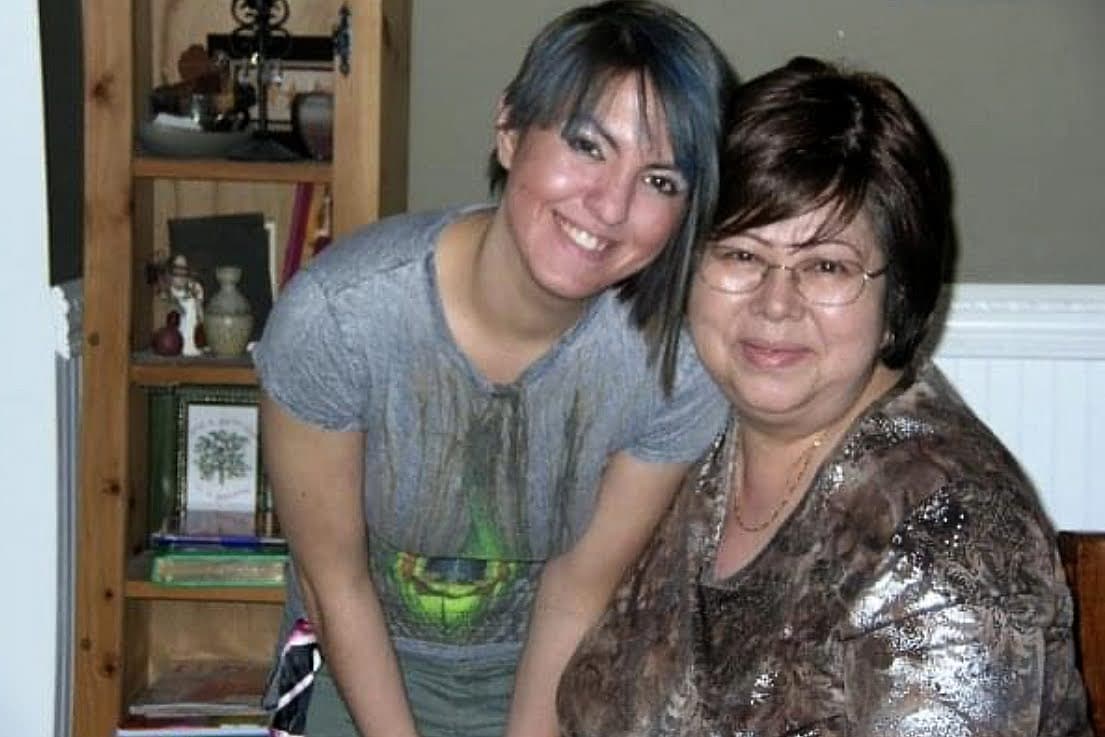
Saying Goodbye
Hodges was born in Japan, where she met Smith’s father. She was known in the family to be strict and blunt but also funny. She was an artist who loved painting portraits in traditional and modern Japanese styles.
On May 5, 2020, the family had to say their goodbyes on FaceTime.
“It’s a very traumatizing experience to watch your mother with the way that she was with the ventilator in her mouth, unable to speak,” Smith recalled, fighting back tears. “But she could hear us because you could see her crying, so she knew we were there. And I don't know what those tears were for. I don't know if she was in pain or if she wanted us to let her go.”
Smith would like to sue Fitchburg Healthcare over her mother’s death, but so far she has not found an attorney willing to help her.
“We are hearing that it would be an impossible lawsuit to take on,” Smith said.
The main hurdle is emergency state and federal laws designed to give long-term care facilities, hospitals and other health care providers broad immunity from legal actions related to their care during the pandemic.
The Push To Protect Health Care Providers
The Massachusetts legislation to protect health care facilities and their employees from lawsuits was introduced by Gov. Charlie Baker in April, 2020, at the beginning of the state’s first COVID wave.
“I cannot overstate the urgency of enacting this legislation,” Baker wrote to lawmakers as they weighed the measure. “We need to ensure that the fear of liability will not prevent the Commonwealth and its medical institutions from acting decisively to deliver the kind of medical response we need during the pandemic.”
State Sen. Cindy Friedman, a Democrat from Middlesex County, vice-chairs the committee that vetted the bill.
“This was a complete and utter crisis [and] I will say our health care system really rose to the occasion, but they needed the support,” Friedman said. “And they knew what they needed, and that’s what they were asking for, and that’s what we gave them. And I feel absolutely confident that this was the right thing to do.”
With little debate, the bill was signed into law nine days after it was introduced. The protections were retroactive to the governor’s declaration of a state of emergency on March 10, and they ended when it was lifted more than a year later, in mid-June, 2021.

Those lobbying for the bill included the Massachusetts Hospital Association, insurance companies and nursing homes.
“Like other health care providers at the onset of the outbreak, long-term care facilities faced unprecedented shortages of, and access to, COVID-19 testing, vital personal protection equipment and funding to secure staffing,” wrote Tara Gregorio, president of the Massachusetts Senior Care Association, which represents many long-term care facilities, in an email to WBUR. “In addition, state and federal guidance from public health officials was constantly evolving and changing as regulators learned more about the virus.”
Massachusetts is far from the only state that rushed to pass COVID protections for health care providers. Nearly 30 other states have similar laws on the books, and a federal measure also provides some immunity from liability.
These measures set a high bar for lawsuits on behalf of families who believe long-term care operators should be held accountable for COVID outbreaks and deaths in their facilities. In Massachusetts, the emergency state law requires plaintiffs to meet a standard known as “gross negligence.”
“If you hear something and you go, ‘OMG, I can’t even believe that could happen,’ that is probably a situation where there was gross negligence,” explained Kathy Cook, an attorney who litigates malpractice cases in Massachusetts.
Closing The Courtroom Doors
Cook’s firm has taken on just one medical malpractice case during the period covered by the immunity law, and she says it was not related to COVID. She believes her office is not alone.
“There is a general feeling among the bar that does these types of cases that they are going to have to look really, really bad for us to even take a look at them, to even consider them,” Cook said.
Other factors beyond the immunity laws can discourage attorneys from taking such cases. One is a general lack of evidence because COVID restrictions kept visitors out of health care facilities for many weeks. Another is the concern that jurors will be more sympathetic to caregivers, who were on the frontlines of the crisis.
"If nursing homes believe that they have a legitimate defense ... in a way that reasonable people would say, ‘It’s not their fault,’ let them tell that to a jury. Let them tell that to a judge.”
Mike Festa
Because it’s so difficult to bring cases, some legal scholars are now raising questions about the wisdom of COVID immunity measures.
“Passing these immunity laws is not justified one way or another by an emergency,” said Lawrence Gostin, professor of global health law at Georgetown University.
Gostin argues there is no research or other evidence to show that immunity from liability laws benefit public health. The real issues in an emergency, he says, are problems like surge capacity in hospitals, availability of medical equipment and the need for new and innovative therapies.
"These are the critical aspects of dealing with COVID,” he said.
Long-term care facilities can still be held accountable criminally. Right now, there are at least two ongoing investigations in Massachusetts involving facilities in Holyoke and Littleton.
But patient advocates say families need more options. Mike Festa, state director of AARP, thinks closing the courtroom doors during the pandemic was a mistake.
“If nursing homes believe that they have a legitimate defense to the fact that when this happened they were caught short in a way that reasonable people would say, ‘It’s not their fault,’ let them tell that to a jury. Let them tell that to a judge,” Festa said.
It’s the opportunity Suzanna Smith’s family is hoping for. She knows she can’t bring her mother back, but she wants to make sure the next patient receives better care.
“Money is meaningless, I have enough money. I don’t care about that,” Smith said. “I want accountability.
"Nobody is immune from aging, and I want to be at a facility that’s caring for me, that has empathy for the patients, that provides quality care, that provides basic essentials such as water and food. I don't even know if that was provided or not.”
This segment aired on August 19, 2021.