Support WBUR
She Lost Her Husband To COVID. His Death Could Help Other Families Sue Nursing Homes
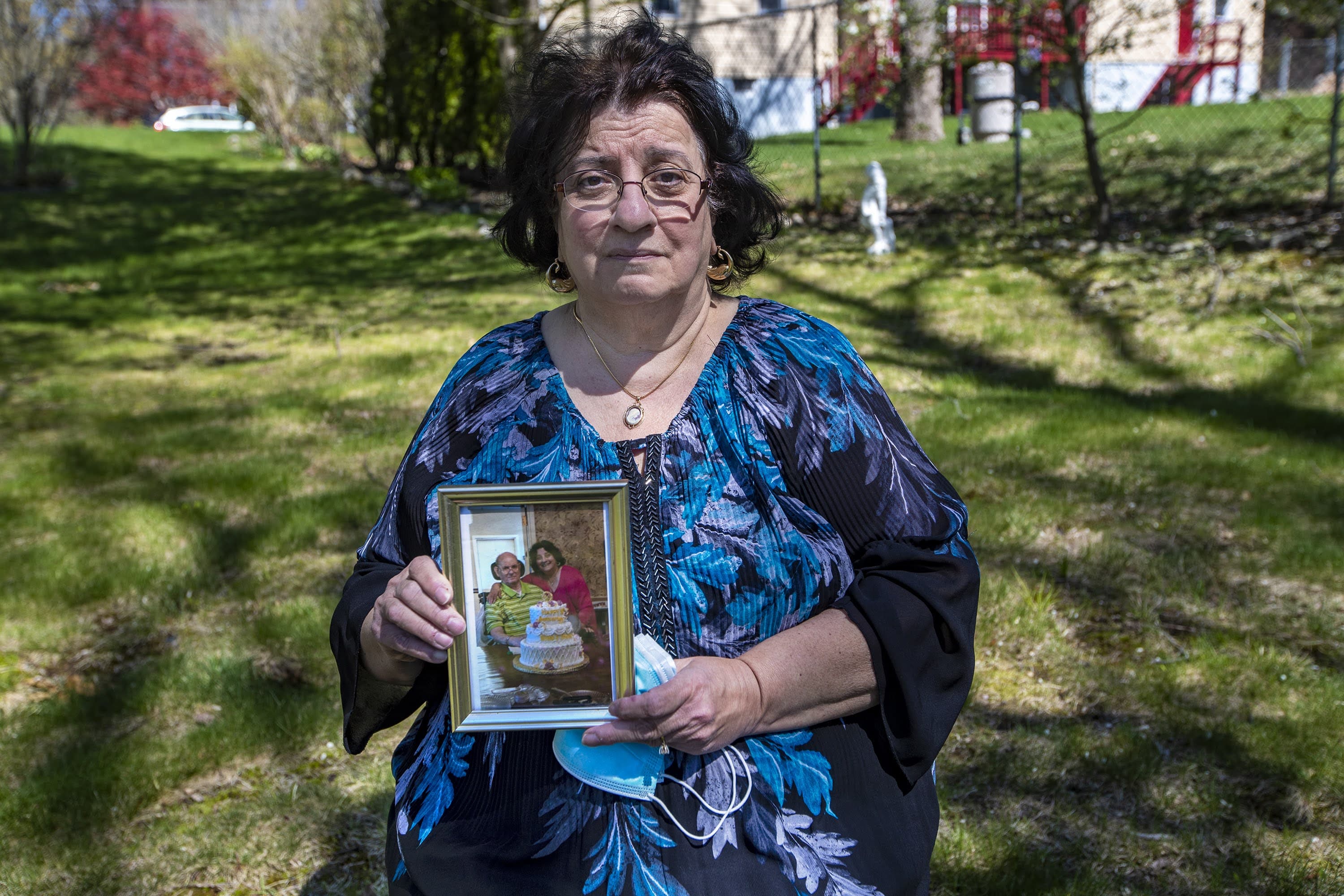
Part two of two stories. Read part one here.
David Hoey is known as the guy to call if you have a problem with a nursing home in Massachusetts. So, as you might imagine, his law office has been busy over the past year.
“Why did my mother get COVID? Why were there 36 deaths in that nursing home? Why weren’t we told?” said Hoey, listing off some of the questions he’s received. “Why wasn’t I allowed to visit my loved one?”
Hoey got so many of these calls, he had to hire more staffers just to manage the phones. So far, he estimates he’s heard from more than 500 people.
The volume of calls doesn’t surprise him. There were problems at some facilities before COVID hit, he says, and the pandemic just showed their deadly consequences.
“Infection control issues, policies, proper staffing, allocation of money, resources, supplies,” from Hoey's perspective, if all these things had been addressed, COVID would not have devastated so many nursing home residents.

But Hoey has to tell the families calling his office that there’s little he can do because of emergency state and federal laws that protect health care providers from most lawsuits during the height of the pandemic.
The laws were intended to ensure that health care providers could act quickly in an emergency without fear of being sued. The measure passed by Massachusetts lawmakers made it so health care workers and facilities — including nursing homes and other long-term care facilities — were immune from nearly all lawsuits over their care during the COVID-19 emergency.
There are few exceptions, unless the provider engaged in what’s known as “gross negligence,” recklessness, or intent to harm or discriminate.
“Gross negligence is exactly what that word is — gross. It is a heightened level of negligence," Hoey explained. "That’s pretty much ignoring somebody, all their needs, shift after shift, hour after hour, day after day, neglecting somebody to death.”
Gross negligence is exactly what that word is — gross. It is a heightened level of negligence. That’s pretty much ignoring somebody, all their needs, shift after shift, hour after hour, day after day, neglecting somebody to death."
David Hoey
It's a standard, Hoey adds, that is very hard to prove. Hoey wants to test the limits of these liability protections, and he’s exploring one particular case that could help him do it.
His client, Stella Kazantzas, lost her husband, Nick Kazantzas, after he contracted COVID at Life Care Center of Nashoba Valley, in Littleton. Nick was among the first long-term care residents in Massachusetts to become ill and die of COVID-19.
On March 29, 2020, Nick was sent from Life Care Center’s facility to the local emergency room and put on a ventilator. But the treatment wasn’t working.
“The nurse said, ‘He’s intubated for two hours, he’s not responding, it would be cruel to keep it going,’ ” his wife Stella remembered, tears welling up in her eyes. “I said, ‘Can’t you try a little longer? Maybe he will respond.’ ”

Because of COVID restrictions, she couldn’t be with her husband in his last moments. Instead, she said goodbye over the phone.
“And I told him I loved him and that his daughter loved him. And I told him in Greek that he was ... a strong warrior,” Stella said through tears. “And they told me that when I spoke to him, that he opened his eyes, and he passed.”
That was March 30, 2020. Nick Kazantzas was 83.
Life Care Center of Nashoba Valley, where he contracted COVID-19, is owned by Life Care Centers of America, which bills itself as the largest privately owned long-term elder care company in the U.S. Its facility in Washington had the country’s first major COVID outbreak at the beginning of 2020.
During the outbreak, more than 100 people tested positive for the coronavirus, and nearly 40 people died.
After what happened at that facility, Hoey argues that long-term care providers across the country should have leaped into action to protect their residents from the coronavirus. Instead, he alleges they didn't do enough.
“So there was at least a good 20-30 day window where other nursing homes, particularly the national providers, were on notice that there was a problem,” he said. “And then boom, it hit Massachusetts like wildfire.”
The virus spread to thousands of people in long-term care facilities in Massachusetts, including Nick, who was supposed to go home after a rehab stint at Life Care Center of Nashoba Valley. He was there following a major spinal cord injury, but his family was still expecting him to recover enough to come home.
“I always felt we were playing ‘beat the clock,’ trying to get him better just enough to get him home, and it didn’t happen,” said his wife, Stella. “And it didn’t happen because the people at the top weren’t doing their job. That’s it, in a nutshell. They were not doing their job. They weren’t protecting the patients, they weren’t protecting their staff.”
Stella and Hoey sent the facility a letter of complaint in January, the first step toward filing a civil lawsuit over her husband’s death. In it, they allege, among other things, that the facility didn’t do enough to provide protective gear like masks or take enough precautions to stop COVID.
"I always felt we were playing ‘beat the clock,’ trying to get him better just enough to get him home, and it didn’t happen. And it didn’t happen because the people at the top weren’t doing their job."
Stella Kazantzas
In its letter of response, the facility denies that it caused her husband’s death. The response says Stella’s claims have no merit, and asserts that Nick died of a bladder infection, not COVID, even though his death certificate lists COVID as the primary cause of death and makes no mention of a bladder infection.
The facility also points out that it is protected from legal action by state and federal law.
Life Care Center of Nashoba Valley declined to speak with WBUR for this story.
“While this case is pending, we will continue to focus on providing quality and compassionate care to our residents,” the facility wrote in an emailed response to WBUR’s inquiry.
During the outbreak at its Littleton facility, dozens of staff and residents contracted the coronavirus, and nearly 20 people died of COVID. Life Care Center of Nashoba Valley is currently under investigation by the Massachusetts Attorney General’s Office.
Attorney General Maura Healey declined to discuss the investigation but said in a statement that her office is working to determine whether legal action is warranted.
“We owe it to the families who lost loved ones under these tragic circumstances to determine what went wrong,” Healey wrote.
Many other skilled nursing facilities also experienced coronavirus cases and, in some cases, severe outbreaks. Roughly one of every three COVID-19 deaths in Massachusetts occurred at long-term care facilities, killing 6,196 residents by April 2021, according to state data.
Infections and deaths at long-term care facilities declined after the state began an aggressive vaccination campaign at the end of last year.
The Massachusetts Senior Care Association represents nearly 400 of the state’s nursing, rehabilitation and other long-term care facilities. The group’s attorney, Mark Reagan, stresses that there wasn’t enough testing and protective equipment available in the early days of the pandemic, and guidance about how to halt the spread of the virus was still evolving.
“As good as you could be under those circumstances there really was not much of an opportunity to protect the facility, the staff, other residents and the like from the introduction of the virus,” he said. “So without those tools there was an extreme vulnerability that was presented to the sector.”
Reagan argues that’s part of the reason the legal protections for these facilities make sense. The immunity, he points out, doesn’t last forever. The emergency law passed by the state covers a limited period of time that ended when the state of emergency lifted on June 15.
But advocates for residents of long-term care allege there were long-standing problems at many facilities that increased the likelihood that COVID would spread. According to federal data, nearly 40% of nursing homes in Massachusetts were cited for at least one infection prevention and control violation from 2013 to 2017.
This has worried Arlene Germain, co-founder of Massachusetts Advocates for Nursing Home Reform, for years. In addition to infection control issues, she says lack of staffing has also been a significant problem.
“Not a lot has changed,” she said. “When I first got into advocacy 21 years ago, we were talking about staffing, the need for more staff. If you don’t have enough help, no matter how hard they work, if there aren’t enough of them, they can’t give the kind of care we all would want.”
Advocates and lawyers like Hoey fear little will change if the legal system doesn’t hold long-term care facilities accountable for their actions during the pandemic.
For his client Stella Kazantzas, the reasons to pursue a lawsuit are more personal.
“I think people deserve justice. People’s lives are important,” Kazantzas said.
If she is able to move forward with her lawsuit against Life Care Center of Nashoba Valley, it could open a pathway for other families looking to seek justice.
“My husband wanted to come home. That was his dream. And he would ask me, ‘You think I’ll come home?’ And I said, ‘You definitely will come home,’ ” she said. “He should have had a better chance.”
This segment aired on August 20, 2021.