Support WBUR
More than 20% of women won't get diagnostic breast imaging if deductible is involved, Boston study shows
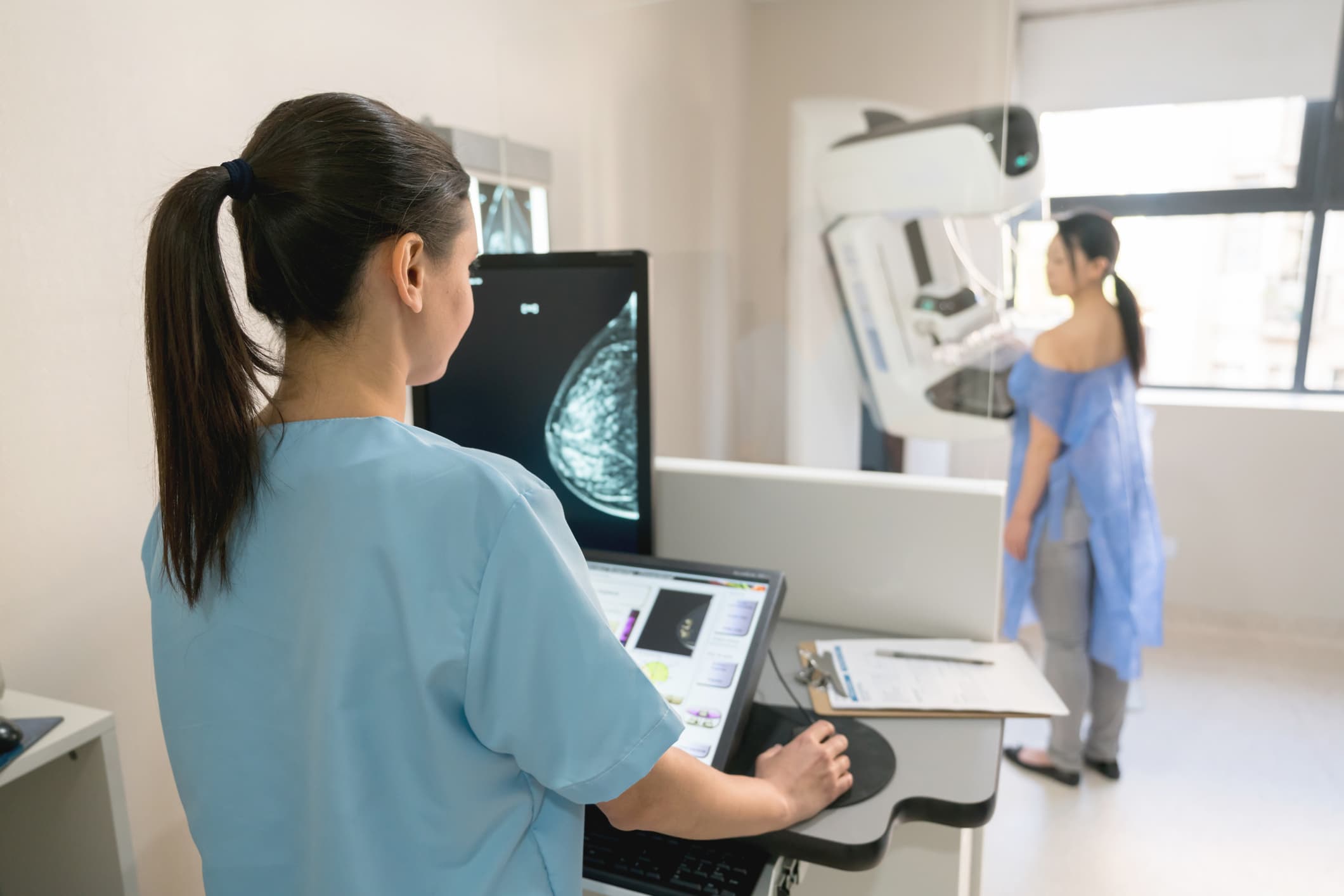
A new study finds 21% of women who get abnormal findings on their mammogram screenings will not get follow-up diagnostics if a deductible is involved.
Nearly 1,000 women with breast imaging appointments were surveyed at Boston Medical Center.
Dr. Priscilla Slanetz, a co-author of the study, said she's concerned at the number of women putting off testing to detect breast cancer early.
"Anecdotally, I have seen patients who have delayed care for financial reasons, but I really was actually a little surprised it's as high as 20%," Slanetz said, "but it probably does explain some of the health care disparities that we're seeing"
Slanetz said thenumbers show the need for insurance mandates that fully pay for follow up diagnostics to protect the health of women.
She estimated that about 10% of women are asked to come back for additional imaging — that's when it becomes a diagnostic test, and is no longer fully covered under most insurance plans.
"We need to have insurance companies cover diagnostic breast imaging at first dollar, meaning that the patients would no longer have any copay or out-of-pocket cost in order to come in and have that diagnostic imaging performed," Slanetz said.
Slanetz said the study was partially aimed at providing data to push forward a pending bill in the Legislature that would mandate that coverage.
She added that BMC has a financial service group that can provide people with ways to overcome financial barriers.
But, she said, "many women are not aware that that even exists, so that's part of the issue as well."
