Support WBUR
Commentary
If You Get Critically Ill With COVID-19, How Far Should Doctors Go To Keep You Alive?
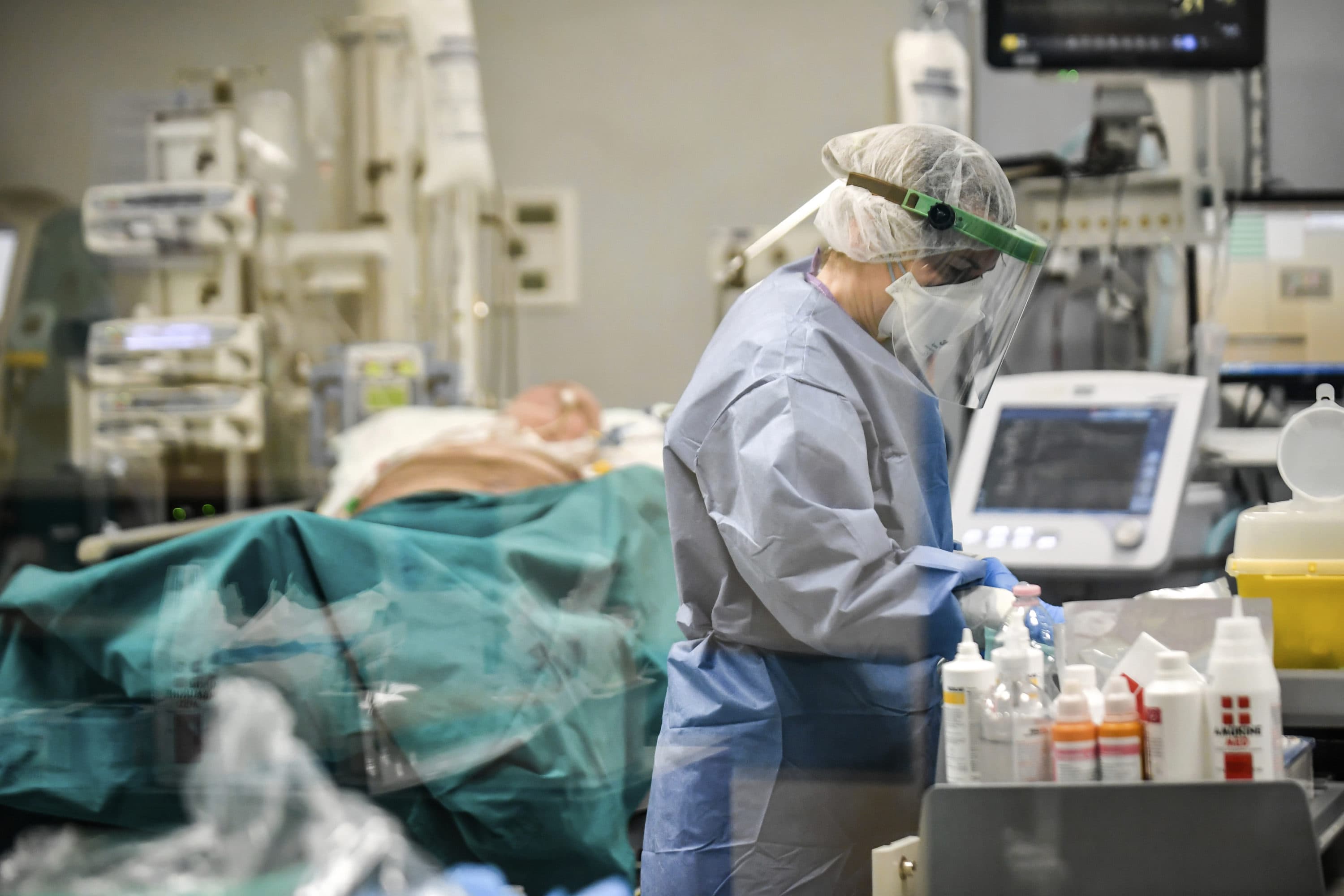
As physicians, we are familiar with the difficult decisions that our patients and their families have to make when faced with critical illness. The urgency of these decisions is even more amplified by the unprecedented and rapidly evolving COVID-19 pandemic.
We fear that many of our patients may end up being hospitalized and confronted with challenging questions — like if they would like to be kept alive on a ventilator, or to have cardiopulmonary resuscitation (CPR) done — and have not had conversations about this in advance.
In light of this, we believe it is time to begin a national dialogue on the role of advance care planning as it relates to COVID-19.
“Advance care planning” is a term used to describe the process by which doctors and their patients can ensure that medical interventions performed in response to critical illness or end-of-life are consistent with a patient’s values and preferences. The term “code status” is used more specifically to detail if a patient would want to undergo CPR and/or intubation (being put on a ventilator) should their heart stop or lungs fail.
We are trained to ask patients about their code status when we encounter them in the hospital. However, many patients may have difficulty comprehending these discussions during episodes of acute illness. And if a patient’s wishes had not been made clear previously, alternative decision-makers may naturally struggle with reconciling what they want for their loved one with what the patient would have conveyed if they had been able. Further, when physicians cannot clearly determine a patient’s code status, we often default to “full code,” or perform all measures necessary to sustain life.
While this may seem like a good default, there are reasons that it may not be.
The prognosis for in-hospital CPR tends to be poor, with only an estimated 15% surviving to hospital discharge. For many patients, being kept alive on machines with little hope of survival is not a way they would want to die.
We expect that during the COVID19 pandemic, physicians will be pushed to intubate and perform CPR on patients who would not want these interventions done. Not only will this cause personal harm to the patient (broken ribs are common, for instance), but it will also risk high-level exposure to those who are involved, potentially putting numerous doctors and nurses in isolation for multiple days or weeks.
Per early estimates from the Chinese CDC, 5 to 15% of those infected with COVID-19 will have severe to critical symptoms possibly requiring management in intensive care units (ICUs). In early reports from the United States CDC, similar results have been reported, the majority of them between 60 to 80 years of age (although certainly some in younger age groups as well). Moreover, those who are elderly with co-morbidities who do end up requiring ventilator support have very high mortality rates. In one recent Lancet study, 31 out of 32 critically ill COVID-19 patients on ventilators ended up dying. In another paper in JAMA last week, 11 out of 21 had died, and a remaining eight were on ventilators in critical condition.
These trends are concerning and should cause all of us to take notice. As a medical community, we must use this moment to focus on understanding people’s end-of-life goals now. If we do it right, we can make sure everyone ends up receiving the care that is most in line with their wishes if they end up in such a position. We see this as an opportunity to avoid unnecessary harm, respect the end-of-life wishes of our patients, and ensure that only people that truly understand and want to be treated in an ICU or on a ventilator end up there.
Evidence suggests that advance care planning decreases rates of undesired hospitalization and in-hospital death. However, in the United States, only about a third of people have done some form of advance care planning.
Here are the steps you can take to make your medical preferences clear:
- Designate your next-of-kin as your Durable Power of Attorney for Health Care or Health Care Proxy.
- Create a Living Will that includes clear language on medical preferences.
- Discuss advance care planning with your physician and complete a Physician Orders for Life-Sustaining Treatment (POLST) form (or similar, depending on your state).
Physicians and hospitals can be proactive in this process as well, by doing the following:
- Reach out to high-risk patients who they feel would especially benefit from advanced care planning.
- Deploy palliative care consultation services to high-risk COVID-19 patients in emergency rooms or early in a hospital admission.
- Discuss and document code status for all patients diagnosed with COVID-19.
Advance care planning need not be mistaken for over-reaction or fatalism, and it is certainly not a call to ration care. It is simply the act of taking steps to ensure that we all have the time and space to consider tough decisions before we are critically ill.
Many, if not all of us, will have some connection to COVID-19, whether personally or through loved ones. Thinking about advance care planning right now may actually save you, your family, and your doctors from having to struggle with more challenging questions later on.
Abraar Karan MD, MPH, DTM&H (@AbraarKaran) is an internal medicine physician at Brigham and Women’s Hospital and is working on population-level COVID19 response in Massachusetts.
Evan Shannon MD, MPH (@eshantang) is a hospitalist and hospital medicine research fellow at Brigham and Women’s Hospital.